Introduction
Elderly older than 65 years, when admitted to hospital, present a higher risk of compromising functionality during hospital stay and after hospital discharge 1. An acute disease or an exacerbated chronic disease, changes produced by aging, and the negative aspects occurring during the hospitalization of an elderly patient precipitate the loss of functional ability 2. Factors such as reduction of mobility, polypharmacy, inadequate architectural conditions, malnutrition, hospital routines and physical restraints contribute to developing this diagnosis 3,4. As a consequence, functional dependence leads to a higher risk of hospital readmissions, admission to geriatric homes and increase of mortality 5,6.
Hospital functional impairment (HFI) is defined as the loss of the ability to perform at least one basic activity of daily life (BADL) (eating, bathing or showering, using the toilet, dressing, sphincter continence, getting out of bed or of a chair, walking, and climbing stairs) at the moment of hospital discharge, concerning the baseline (considered as two weeks before the onset of the acute disease), corresponding in the Barthel Index to the decline of 10 % of scoring related to the population basal functionality level, or the loss of ten points in the scale 7-9.
Lendínez and cols. reported that functional impairment reaches a proportion of 32.2% in elderly older than 65 years, and it grows up to 63.3% in elderly older than 85 years 10. In Spain, the reported HFI ranges between 35 and 70% in patients older than 60 years; patients older than 70 years showed impairment in some BADL by 46%, while in people older than 90 years this figure reaches 88% 9. In Colombia, there are no studies characterizing HFI in elderly population admitted in elderly care units, given the hospital conditions and the lack of care units that would document this impairment.
The objective of this study is to determine prevalence of hospital functional impairment, and the associated factors, in patients older than 65 years hospitalized in the San Ignacio University Hospital in the period between December 1st 2015 and December 31st 2017, and the associated factors.
Materials and Methods
Adescriptive cross-sectional study of a hospital cohort, between December 1st 2015 and 31st 2017 was carried out, reviewing the medical records. This review included the records of elderly persons older than 65 years, hospitalized in the geriatric service of the San Ignacio University Hospital, who were admitted for medical pathology. They underwent functional measurement using the Barthel scale for documenting baseline (two weeks prior to hospital admission) and discharge from hospital. Patients hospitalized for psychiatric and chirurgical pathologies, with uncomplete information in the database, as well as patients who died during the hospital stay, those who have requested a voluntary discharge against medical advice during hospitalization, or those who were referred to another institution were excluded.
Data obtained from the medical records review were fed into a database built according to the considered variables. Dependent variable was HFI, as independent variables sociodemographic characteristics were included: age, as continuous variable; gender (male, female); polypharmacy, considered in dichotomous form, defined as consumption of five or more medications; comorbidities, identified as a continuous variable according to their identification at hospitalization; readmission, measured as a dichotomous variable if the patient had or had not been readmitted; social risk, defined at the admission, whether an adequate support network for the patient was or was not identified; hospital complication, determined as a dichotomous variable according to whether there was a complication or not; malnutrition at admission, defined using a mini nutritional assessment (MNA) as in risk of malnutrition or in malnutrition; delirium, at admission, defined as the existence of at least two out of four criteria of the Confusion Assessment Method (CAM); dementia, indicated as the presence of dementia as clinical diagnosis; duration of hospital stay (DHS), considered according to the number of days, as a continuous variable; and mobility during the stay.
The sample size was calculated based on the proportion formula, obtaining a required minimum sample size of 566 patients of lower risk (around 0.1), which corresponded to a population of low and medium risk. The required sample size for population of high risk (risk of circa 0.3) was 242 patients.
A descriptive analysis was performed with information of the variables of interest using measures of central tendency and dispersion. Additionally, mean and interquartile range were used, according to criteria of normal and not normal distribution. Categorical variables were expressed in frequency tables.
In the bivariate analysis, significance level or p value (p = <0.05) was implemented. Regarding association measures, the Chi-squared test was implemented for the dichotomous variables; and for the continuous variables the Mann-Whitney U test, for establishing whether there were statistically significant differences. Finally, regarding the logistic regressions, a binary model and a multiple model were used adjusted by the confusion variables. In the latter model, age and gender were considered confusion variables. Odds ratio (OR) obtained, together with trust intervals of 95% (CI of 95%), were reported. Analysis was conducted with the Stata 14 program (statistical software package for descriptive analysis).
The study is considered to pose no risk in the terms of Resolution 8430 of Colombian law. The protocol was approved by the Research and Ethics Committee of the SIUH and the Xaverian University.
Results
From December 1st 2015 until December 31st 2017, information was gathered of 1055 older adults, with a mean age of 85.58 years old (IRQ 9), percentage of participation of women reached 56.68%; the mean Barthel index prior to admission was 59.97. Out of the total studied population, 124 (11.75%) had been readmitted; 822 (72.91%) had a diagnosis of dementia; 797 (75.54%) presented malnutrition; 469 (44.45%) were admitted with delirium; polypharmacy was present in 36.11% of the studied patients, and 892 (84.54%) were at social risk. Additionally, the average number of comorbidities was 4.8. It was found that 434 persons (41.14%) presented hospital functional impairment (HFI). Patients' demographic data are shown in table 1.
Table 1 Characteristics of patients hospitalized at the SIUH in the geriatric service
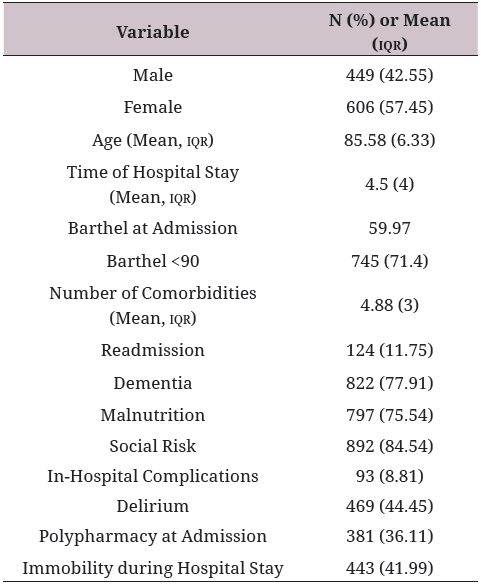
IQR = Interquartile Range
n = 1055
Data of the bivariate analysis is summarized in table 2, where the analysis is divided into two groups: patients with HFI and those who did not present HFI. Population presenting HFI was predominantly female (54.14%); mean age was 87 years (IQR 8, p = 0.071). At admission, 42.97% showed Barthel scores of 20 points (IQR 50, p = 0.00), with poorest scores regarding those who did not present functional impairment. 52.79% with DFH presented dementia, versus 47.2% who showed no impairment (p = 0.046); 54.6% presented delirium compared with 45.4% not presenting HFI (p = 0.00). As for the presence of malnutrition, findings showed that, of the patients with HFI, the number of individuals suffering malnutrition at admission was higher than those in the group with no HFI (439 = 55.1% v. 358 = 44.9%, p = <0.000).
Table 2 Bivariate analysis of individuals with HFI V. individuals with no HFI
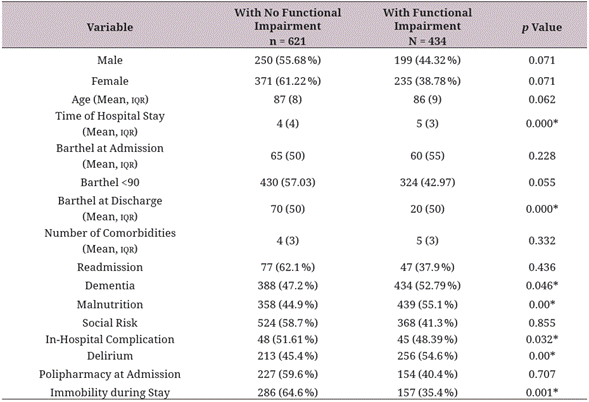
* p = <0.05; IQR = Interquartile Range
For dichotomous variables the chi-square test was implemented, and for the continuous variables the Mann Whitney U Test. n = 1055
In terms of social risk, in the HFI group 368 patients had a poor support network; while 524 patients of the group with no HFI showed this condition (41.3% and 58.7%; p = 0.855, respectively). Regarding time of hospital stay, a mean of five days stay (IQR 3) was established in individuals with HFI, while those with no HFI had a mean stay of four days (IQR 4; p = <0.004). On the other hand, findings showed that 45 patients with HFI presented some complication, while 48 patients with no HFI showed in-hospital complications (51.61% v. 48.39%; p = 0.032).
The logistic regression binary model found a statistically significant relation between HFI and age [OR 0.97, CI95% (0.95-0.999), p = 0.021]; male gender [OR 1.25, CI95% (0.98-1.60), p = 0.071]; time of hospital stay greater than seven days [OR 1.08, CI95% (1.05-1.18), p = 0.0001]; malnutrition [OR 1.96, CI95% (1.4-2.66), p = 0.0001]; dementia [OR 1.30, CI95% (1.004-1.68), p = 0.046]; in-hospital complication [OR 1.59, CI95% (1.03-2.43), p = 0.033]; delirium [OR 2.75, CI95% (2.13-3.54), p = 0.0001]; and immobility during the stay [OR 1.50, CI95% (1.17-1.93), p = 0.0001].
As it can be observed in Table 3, in the multivariate analysis all variables were adjusted by age and sex, resulting in a statistically significant association of HFI and time of hospital stay lower than seven days [OR 1.88, CI95% (1.41-2.49), p = 0.0001]; malnutrition [OR 1.59, CI95% (1.16-2.19), p = 0.0001], and delirium [OR 2.38, CI95% (1.83-3.10), p = 0.001].
Discussion
Changes in functionality of patients at the time of hospitalization follow complex trajectories and, as a consequence, severe secondary complications arise 11-15. The present study showed that, of the 1055 patients included in the analysis, 434 persons presented HFI, corresponding to 41.14%, a similar figure to those produced by studies performed in elderly population, with prevalence figures between 30%> and 67 % (1264% women, 24% nonwhite 12-17.
Comparatively, Mañas and cols. conducted a study entitled "Deterioro de la capacidad funcional en pacientes ancianos egresados de un servicio de medicina interna" ("Impairment of Functional Ability in Elderly Patients Admitted in a Service of Internal Medicine") in a Colombian population and reported that the functional loss percentage obtained of the sample was 17.3%, although the results are not comparable, since the included population, the design and the methodology were different 17. In contrast, the study of Cares and cols., performed in Chile, with population of similar characteristics and variables, found that 72% of population presented loss of some functional ability during hospital stay 18.
Predictors of hospital functional decline have been described before in patients at high HFI, associated with a higher burden of disease in terms of large hospital outcomes 19,20. A bivariate analysis was performed comparing patients with HFI and those not presenting this condition. Loss of one or more basic activities of daily life during hospitalization occurred predominantly in the population with longer hospitalization time; this may largely be due to hospital dynamics and to the severity of the index disease. Additionally, the impact of malnutrition considerably increases morbimortality and time of hospital stay 11. In the assessed population, it was documented that malnutrition was prevalent both in those who developed HFI, and in those who did not, with a prevalence of 55.1% and 44.9%, respectively.
44.45 % of the included patients presented delirium at admission, where a significatively higher proportion of them was present in those with HFI, in relation to patients who did not decline functionally (55.1% v. 44.9%), this fact is connected to dementia prevalence in the studied population (77.91%). Likewise, the average number of diseases in both patients groups reached 4.88; the comorbidity mean difference was not statistically significant. Polypharmacy was present in a higher proportion of patients with no HFI versus those with HFI (59.6% v. 40.4%), a trend also evidenced in immobility during hospital stay; it was more prevalent in the population that did not develop HFI (64.6 % v. 35.4 %), a finding that contrasts with the study of De Saint Hubert and cols., "Factores de riesgo que predicen un deterioro funcional posterior en pacientes ancianos hospitalizados" ("Risk Factors that Predict a Ulterior Functional Decline in Elderly Patients"), in which one of the main risk factors for HFI was the low mobility in hospital stay 19.
Age is a continuously mentioned factor among factors related to development of HFI, in our study we found that the population that presented most frequently functional decline was population older than 80 years, explained by aging changes, pluripathology, high frequency of dementia, and polypharmacy 21,22.
Regarding the logistic regression, we found that, in the raw analysis, with statistically significant differences, there was a greater association of HFI to age; male gender, with an OR of 1.25; and time of hospital stay greater than seven days, with an OR of 1.08. Malnutrition increased the HFI by 1.9 times, as well as hospital complications with OR of 1.59; and delirium, with an OR of 2.75. In line with the results, multiple studies have concluded that the common predictors for developing HFI include age, delirium, extended hospital stay, and other cognitive deficits 21. Additionally, in the logistic regression, with variables adjusted by gender and age, statistical significance was found in the appearance of HFI by a time of hospital stay greater than seven days, with an OR of 1.88; malnutrition, with an OR of 1.9; and delirium, with an OR of .38.
These findings are significant in the context of the Colombian elderly population, since the performed analyses had not been considered before in geriatric care units in Colombia 17,23. With this in mind, it is necessary to early identify these conditions in patients, with the purpose of carrying out preventive actions that contribute to reduce the functional decline in our patients.
In the study, a direct measure of cognitive, functional and nutritional factors was performed with standardized measures with the best validity 2,9,17. Inclusion and exclusion criteria were clearly defined, thus reducing the risk of statistical bias. Relevant confounding factors identified by reviewing previous studies were considered, as well as a multivariate adjustment with the purpose of determining factors associated with developing HFI 24; for this reason, further studies are required for assessing interventions proposed for preventing HFI in our population in order to determine which interventions were effective.
Limitations of this study were connected with the fact that performing the assessment of the patient's baseline conditions was carried out in the emergency room. For this reason, it is possible that baseline information that consider the early functionality decline associated with acute disease was collected, however, this method could be consistent with previous studies of patients admitted in emergency departments. There were no direct comorbidity measures as possible confounding factors.















