Introduction
Biopolymer injections for esthetic purposes is a public health problem; although its usage dates back from more than a century, its demand has steadily increased in the last decade.1 A wide variety of complications are associated with this procedure, which can be innocuous or even life-threatening; presenting from immediately to years later, locally or systemically, with mechanical, inflammatory or autoimmune characteristics.2 In our country there are a lot of oil preparations with and without biopolymers or silicone used for esthetic purposes in different body areas, such as face, hands, breasts, gluteus and thighs. Unfortunately, these procedures are in many times performed by non-health care professionals.3 The pharmacological effects of these substances are largely unknown, although it has been reported that these can migrate to other organs as emboli, causing a secondary inflammatory or ischemic process.4 We report a case of a patient who presented long-standing symptoms, but only consulted after the onset of an acute lower limb arterial thrombosis that could have been fatal without a rapid intervention.
Case report
A 63-year-old mestizo woman, with a history of biopolymer injection in hands and thighs and augmentation mammoplasty fifteen years ago was admitted to the emergency department because of thigh pain. The patient reported chronic fatigue and myalgia predominantly in the lower limbs in recent years. One month before admission, she reportedly had a progressive bilateral medial thigh pain associated with tumefaction, erythema and changes in skin color; she also presented paresthesia, dysesthesia and bilateral weakness of lower extremities. Then, four days before consulting, her pain became unbearable, with reddish and purplish skin color in the distal third of her right leg that limited its mobility. She reported absence of fever, thoracic pain or dyspnea; she reported being an active smoker and taking no medications. Her medical history was unremarkable.
On examination, the patient was alert and fully oriented. She was pale and appeared ill. The temperature was 36 °C, the blood pressure 125/72 mmHg, the pulse 64 beats per minute, the respiratory rate 17 breaths per minute, and the oxygen saturation 98% while she was breathing ambient air, and the weight 46 kg. The heart and lung sounds were normal. Medial surface of her right thigh was warm, with tenderness, mild induration and associated erythema (Fig. 1A), while distal portion of the same extremity was cold and had associated erythema and diminished sensitivity; her popliteal and dorsalis pedis pulses of the same limb were absent and capillary refill time was 4-5 s. Her left leg was cold; both soles of her feet had violaceous discoloration, which was more pronounced in the right foot (Fig. 1B). The remainder of the examination was normal.
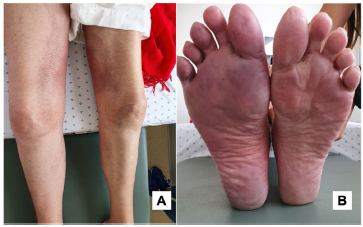
Fig. 1 Lesions of the lower limbs. Panel A. Medial surface of the right thigh: warm, tenderness, mild induration and associated erythema. Panel B. Left leg: her left leg was cold; both soles of her feet had violaceous discoloration, which was more pronounced in the right foot.
A critical limb ischemia was suspected, a CT angiography was performed; it showed thrombosis of the right femoral artery since its origin, thrombosis of the right popliteal artery and of the distal segment of the posterior tibial artery. Anterior tibial and distal peroneal artery of the same limb had adequate blood flow provided by collateral circulation. Additionally, deep and superficial venous thrombosis with extension into the ipsilateral iliac vessels was observed, as well as partial thrombosis of the left popliteus artery with extension into the tibioperoneal trunk. Laboratory tests revealed a normal hemogram, ESR 10 mm/h (reference range 0-30 mm/h), C-reactive protein 3.64 (reference range 0-1 mg/dL), prothrombin time 11.8 s, partial thromboplastin time 51.6 s, international normalized ratio 1.02. Likewise, IgM and IgG anticardiolipin antibodies (aCL) were negative, as were IgM and Ig Anti-Beta-2-Glycoproten I antibodies, antinuclear antibodies (ANAs), extractable nuclear antigen antibodies (ENAs), and anti-neutrophil cytoplasmic antibodies (ANCAs). Complement levels were normal (C3 levels 122.13 mg/dL, C4 levels 42 mg/dL). No other laboratory parameters were obtained.
A femoral and popliteal embolectomy was performed, in which severe soft tissue fibrosis and encapsulated bodies were observed. She received enoxaparin 50 mg bid and low dose oral glucocorticoid (prednisone 5 mg QD) by considering biopolymers as possible triggers of this inflammatory/autoimmune phenomenon. The patient had favorable evolution. A timeline of the clinical findings and evolution is shown in Fig. 2. Unfortunately, the patient did not attend the respective follow-up in subsequent controls. Thus, its clinical and laboratory evolution is unknown.
Discussion
In 2011 Shoenfeld proposed that siliconosis, macrophagic myofasciitis syndrome (MMF), gulf war syndrome (GWS) and post-vaccination phenomena that share clinical and pathogenic resemblances were included under a common syndrome entitled the "Autoimmune (Auto-inflammatory) Syndrome Induced by Adjuvants" (ASIA).2 Autoimmune/autoinflammatory syndrome induced by adjuvants (ASIA syndrome) groups non-specific disorders characterized by dysregulations in the immune system following exposure to an adjuvant. Amongst systemic clinical manifestations of ASIA syndrome, the most common are arthralgia, chronic fatigue, fever and lymphadenopathy; the median time described between exposure to adjuvants and the onset of clinical symptoms ranges from 1 week to 5 years.5
Shoenfeld et al. created several major and minor criteria in the diagnosis of the ASIA syndrome. Some of the major criteria were defined as exposure to an external stimuli (infection, vaccine, silicone, adjuvant) prior to clinical manifestations; typical clinical manifestations like myalgia, arthralgia or arthritis; chronic fatigue; neurological manifestations; cognitive impairment; improvement by removal of inciting agent and biopsy of involved organs. Minor criteria range from the presence of autoantibodies or antibodies against the suspected adjuvant to evolvement of an autoimmune disease.1 In a Colombian cohort of 190 patients with ASIA syndrome, the most frequent symptoms were: myalgia (92.1%), arthralgia (77.9%), asthenia and adynamia (77.9%) and neurological findings (55.8%).6
Our patient fulfilled three of the major criteria proposed by Shoenfeld2: exposure to an external stimulus (silicone, adjuvant) prior to clinical manifestations, myalgia, and chronic fatigue.
Adjuvants are substances that enhance antigen-specific immune responses, such as aluminum hydroxide, mineral oils, and silicone gel5; patients are usually exposed to adjuvants in the scenario of implanted foreign bodies for esthetic purposes, activating antigen presenting cells and promoting antibody production. Pachón et al. reported the frequency of adjuvants related to ASIA syndrome in their study group; they found that polydimethylsiloxane was the most prevalent (90%), followed by polymethylmethacrylate (6.8%) and paraffin (2.1%).6 T lymphocytes recognize these substances and orchestrate an inflammatory reaction at the injection site, with the consequent development of granulomas. Mobilization of adjuvants into other tissues produce other local or systemic manifestations, including edema, erythema, fistulas and organ failure. However, to our knowledge, there are no reports of arterial thrombosis related to biopolymer injection.
These compounds lead to tissue alterations and injuries. A study that analyze 500 cases from the ASIA syndrome international registry found that 13.8% of patients already had another prior autoimmune disorder before the exposure to foreign materials; additionally, autoimmune susceptibility given by a family history of autoimmune condition was documented in 34.5% of cases.5 Despite our patient had no prior personal or family history of autoimmune disorders it is fundamental to highlight the importance of addressing these questions during the patient's evaluation.
In general terms, acute ischemia of a limb can be caused by arterial trauma or acute arterial obstruction ; the latter as consequence of embolism or arterial thrombosis. In our patient, acute ischemia was secondary to arterial obstruction related to biopolymer migration; this substance probably acted as a foreign body and triggered an inflammatory reaction with a subsequent state of hypercoagulability (as evidenced with concomitant deep vein thrombosis), fibrosis and nodule formation.
Clot removal allowed perfusion of the affected extremity. Nevertheless, considering the presence of subcutaneous nodules and systemic manifestations (such as chronic fatigue and myalgias), and anticoagulation with low-molecular-weight heparin; we administered low-dose oral glucocorticoids and hydroxychloroquine for immunomodulation.5 Some researchers have proposed that patients with ASIA syndrome should be treated with a multidisciplinary management that involves pain control, evaluation by rheumatology, physiotherapy, psychiatry, and palliative care if necessary to guarantee an adequate follow-up to prevent functional and psychological sequelae.7
The use of biopolymers for cosmetic purposes is increasing, with a diverse range of associated complications, many of which can be life-threatening. Patients should be asked about minor procedures and history of autoimmune or autoinflammatory disease if ASIA syndrome is suspected.















