Introduction
Adipose tissue is one of the main energy reserves of the human body and contributes to various physiological functions, including the transport and storage of fat-soluble vitamins, as well as structural, endocrine, and immunological roles [1]. However, excessive energy intake, regardless of macronutrient source, combined with sedentary behavior leads to increased fat accumulation, negatively impacting body weight and overall health [2].
These risk factors are increasingly common in the pediatric population. The most recent National Survey of the Nutritional Situation in Colombia (ENSIN) 2015, showed that in school-age children (5-12 years) fried food consumption predominated in 92.5% and fast-food consumption in 57.9%. In addition, 24.4% were overweight, 67.6% spent excessive time in front of screens, and only 31.1% participated in active play [3]. Consequently, the risk of multiple morbidities in adulthood increases as well as the risk of metabolic alterations, such as vitamin D deficiency. Low vitamin D serum levels have been reported in obese people compared to those with normal weight [4] and have been the subject of study in recent years.
Vitamin D is a fat-soluble vitamin, considered by some experts as a hormone that plays an important role in bone health. It also has effects on other cells and tissues that have been denominated as "extra skeletal actions of vitamin D" [5]. Observational studies have consistently demonstrated a negative correlation between serum levels of 25-hydroxyvitamin D (25(OH)D) and 1,25-dihydroxyvitamin D3 (1,25(OH)₂D₃), the bioactive form of vitamin D, and measures of body mass index (BMI), subcutaneous fat mass, and visceral fat mass. Several hypotheses have been proposed to explain the mechanisms linking obesity to low serum 25(OH) D levels. Among these, growing evidence supports the adipose tissue sequestration hypothesis. Research has shown that a high-fat diet increases the expression of Cyp2r1 in adipose tissue, promoting the active uptake of vitamin D₃ and its subsequent conversion to 25(OH)D for storage within lipid droplets [6].
Additionally, other mechanisms, such as volumetric dilution and obesity-related metabolic alterations, have also been proposed as contributing factors to lower vitamin D bioavailability in individuals with higher adiposity [7]. Up to 80%-90% of vitamin D levels depend on direct sunlight exposure and 10%-20% depend on dietary intake [8]. Therefore, low sun exposure and a poor-quality diet can lead to a deficiency or insufficiency of vitamin D. Additionally, factors such as lifestyle, ethnicity, and genetic polymorphisms influence the risk of hypovitaminosis [9]. Vitamin D deficiency is highly prevalent worldwide [10]. Even children living in subtropical climates are at risk of vitamin D deficiency according to recent studies in Brazil [11], Costa Rica [12,13], and Chile [14], as well as in pediatric clinical practice across Latin America [15]. In Colombia, ENSIN-2015 showed a vitamin D deficiency of 20.4% (95% CI 18.4 to 22.6) and insufficiency of 45.2% (95% CI 43.0 to 47.5) nationwide. In Santander, this prevalence was higher than the national average for both deficiency (25.6%; 95% CI 20.2 to 31.9) and insufficiency (47.7%; 95% CI 43.3 to 52.2) [16].
Despite these figures, few studies in Colombia have evaluated the relationship between vitamin D status and adiposity using direct measures of body composition in children. Furthermore, although this study includes cardiometabolic variables such as cholesterol and glucose, these have not been previously explored in relation to vitamin D status in this population.
Given the high prevalence of vitamin D deficiency in Colombian children and adolescents-particularly in the Santander region-despite living in a tropical environment, it is important to explore additional factors that may influence vitamin D status. One such factor is adiposity. We hypothesize that children and adolescents with higher body fat percentages will have lower serum vitamin D levels. Therefore, the aim of this study is to evaluate the relationship between vitamin D levels and body fat percentage in children and adolescents in Bucaramanga, Colombia.
Method
Study design
This is an observational, cross-sectional survey nested on a population-based cohort [SIMBA] [17].
Population and sample
A total of 494 participants aged 10 to <18 years were surveyed. This population corresponded to children and adolescents re-contacted from the baseline sample of the cohort study (n=1282). The sampling method was non-probabilistic by convenience. The statistical power of the sample size (n=494) was between 70% and 75 % (Z1-β = 0.5417), which corresponds to the application of a bilateral test (Z1-α/2) [18].
Eligibility criteria
Exclusion criteria
Medical diagnosis of diabetes mellitus, clinically manifest endocrinopathies, acute or chronic infectious liver disease, and kidney disease.
Children or adolescents under treatment with steroids or hormones (except levothyroxine) up to one month before blood sampling.
Current supplementation with vitamin D (any presentation).
Study variables
The dependent variable corresponded to the serum levels of vitamin D. A serum analysis of 25-hydroxyvitamin D [25(OH)D] was measured using microparticle immunochemiluminescence assay (MICA), with the following cut-off points: deficiency (≤20 ng/mL); insufficiency (21-29 ng/mL); sufficiency (≥30 ng/mL) [19].
The main independent variable was the body fat percentage (BF%), determined through the Slaughter equation [20], with the tricipital and subscapular skinfold thickness to determine the percentage of fat mass with a cut-off point for alteration of > 26% (see Supplementary Material-S1).
Two examiners, a nurse, and a physician performed the skinfold measurements. The two examiners received training from a nutritionist in the appropriate technique for the procedure of taking these two skin folds and how to standardize the measurements. Each examiner made two measurements of each skin fold for each participant in the same hours according to the scheduled appointment. The values of each skin fold were blinded among the examiners. The triceps skinfold (PTC) and subscapular skinfold (PSE) were measured with a Harpenden® calibrator and with a standard technique [21].
Other independent variables that were considered were: sex, age, socioeconomic status, weight, height, body mass index (BMI), waist circumference, hip circumference, waist-to-hip ratio, waist to height ratio.
In addition, the relationship between vitamin D levels and the following cardiometabolic risk factors was explored:
Impaired fasting glucose: ≥100 mg/dL, Diabetes: ≥126 mg/dL [22].
HOMA-IR: obtained from a mathematical model using the following formula ((FI*FG)/22.5), where FI represents fasting insulin levels in UL/L and FG fasting glucose levels.
Dyslipidemia: *Alteration in triglyceride levels: 10-19 years: ≥130 mg/dL. *Alteration in total cholesterol levels: ≥ 200 mg/dL. *Alteration in HDL cholesterol levels: < 40 mg/dL. *Alteration in LDL cholesterol levels: ≥ 130 mg/dL [23].
Data collection
This process was carried out over 16 months. The participants visited a health institution specializing in cardiovascular diseases. During this visit, information related to sociodemographic, anthropometric, and blood sampling variables was collected, along with a complete clinical evaluation. Data collection was carried out by doctors and nurses previously trained in standardized techniques for this purpose. The procedures for collecting all variables have been described in detail elsewhere [17].
Data quality
The data were double-entered into Excel (Microsoft Corp., Redmond, Wash.). Comparisons were performed using Epi-Info 2000. Discrepancies were corrected by cross-checking with the original physical formats.
Statistical Analysis
Initially a descriptive analysis was conducted. The categorical variables were presented as proportions and the continuous ones as medians and interquartile ranges, according to the distribution they presented. The Mann Whitney’s U-test was used to establish differences by sex. The relationship between the dependent and independent variables was evaluated through binomial regression models with their respective goodness-of-fit tests. In the multivariate models, the variables that obtained a p = 0.05 in the bivariate analysis were maintained. All p values were evaluated using two-tailed test, with statistical significance set at p = 0.05. All analyses were performed in Stata, version 14.0 (College Station, TX: Stata Corporation).
Ethical Approval
The study was conducted according to the guidelines of the Declaration of Helsinki, and the Ethics Committee of Fundación Cardiovascular de Colombia reviewed and approved the present study (Record No. 478 of July 9, 2019) Asociación entre el estado de la Vitamina D, el exceso de peso y alteración del perfil lipídico en adolescentes y adultos jóvenes colombianos: desafíos y oportunidades en la evaluación temprana del riesgo cardiovascular. Written informed consent was obtained from parents or legal representatives for participants under the age of 18. All underage participants were asked for verbal assent and minors under the age of 14 for written assent. Adult participants gave their informed written consent directly.
Results
General characteristics
494 participants were evaluated (38.5% of baseline cohort sample) of which 48.5% (n=240) were male and 51.4% (n=254) were female. The median age was 16.6 years (see Table 1). Regarding cardiometabolic risk factors, statistically significant differences were found by sex in anthropometric variables such as waist circumference, and hip circumference, as well as the waist-to-hip ratio, waist-to-height ratio, and the two skinfold thickness measures evaluated. When analyzing the biochemical variables, differences by sex were found in HDL cholesterol (mg/dL), fasting glucose (mg/dL), and fasting insulin (µU/mL) (see Table 1).
Table 1 Sociodemographic, anthropometric, and biochemical characteristics by sex of children and adolescents. Bucaramanga, Colombia.
| Characteristics | Total n=494 | Males (n=240) | Females (n=254) | p-value |
|---|---|---|---|---|
| Sociodemographic variables | ||||
| Age in years, median [IQR] | 16.6 [3.0] | 16.6 [2.9] | 16.5 [3.2] | 0.469 |
| Socioeconomic status, n (%) | ||||
| Low | 296 (59.9) | 140 (58.3) | 156 (61.4) | 0.714 |
| Medium | 193 (39.0) | 97 (40.4) | 96 (37.8) | |
| High | 5 (1.0) | 3 (1.2) | 2 (0.79) | |
| Anthropometric variables, median [IQR] | ||||
| Height (cm) | 163.0 [12.9] | 169.9 [8.6] | 158.5 [7.5] | <0.001 |
| Weight (kg) | 56.8 [17.8] | 60.4 [17.1] | 53.1 [14.2] | <0.001 |
| Under 18 years of age [IQR] | n=360 | n=175 | n=185 | |
| Height for age Z score | 0.25 [1.5] | 0.39 [1.4] | 0.08 [1.6] | 0.4696 |
| Over 18 years of age [IQR] | n=134 | n=65 | n=69 | |
| IMC (kg/m2) | 23.2 [6.2] | 22.9 [8.2] | 23.3 [5.9] | 0.6942 |
| Waist circumference (cm) | 74.8 [12.1] | 75.7 [13.2] | 73.7 [11.1] | 0.003 |
| Hip circumference (cm) | 92 [12.35] | 91.2 [13.0] | 93.3 [11.0] | 0.007 |
| Waist-to-hip ratio | 0.81 [0.11] | 0.83 [0.09] | 0.79 [0.11] | <0.001 |
| Waist-to-height ratio | 0.45 [0.07] | 0.44 [0.07] | 0.46 (0.07) | <0.001 |
| Tricipital skinfold thickness (mm) | 15.5 [9.7] | 11 [8.0] | 18.5 [7.0] | <0.001 |
| Subscapular skinfold thickness (mm) | 12.6 [7.0] | 11.1 [6.0] | 14 [7.0] | <0.001 |
| BF% by Slaughter | 25.3 [9.9] | 20.1 [11.1] | 28.8 [5.9] | <0.001 |
| Biochemical variables, median [IQR] | ||||
| Vitamin D levels (ng/mL) | 27.3 [10.5] | 26.4 [10.2] | 28 [10.9] | 0.2008 |
| Total cholesterol (mg/dL) | 156.6 [36.3] | 155.4 [34.5] | 158.1 [37.8] | 0.074 |
| LDL cholesterol (mg/dL) | 94.0 [26.6] | 89.2 [32.0] | 93.8 [32.0] | 0.215 |
| HDL cholesterol (mg/dL) | 47.7 [15.1.0] | 44.4 [14.6] | 50.5 [14.9] | <0.001 |
| Triglycerides (mg/dL) | 79.1 [49.5] | 81 [52.6] | 78.1 [45.0] | 0.223 |
| Fasting glucose (mg/dL) | 91.3 [6.7] | 93 [9.0] | 89.2 [8.4] | <0.001 |
| Fasting insulin (µU/mL) | 9.8 [6.1] | 8.7 [6.3] | 10.7 [5.6] | <0.001 |
| HOMA (UI/mL) | 2.0 [1.5] | 2.1 [1.6] | 2.0 [1.4] | 0.679 |
Note. IQR: Interquartile range; BMI: Body Mass Index.
BF% and vitamin D prevalence
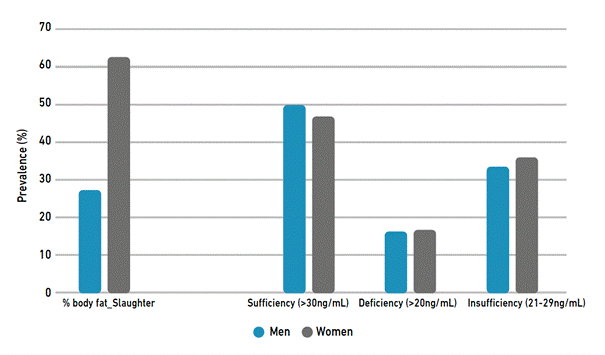
BF%: 45.5% of the population presented a high BF% calculated by Slaughter (> 26%), with a higher prevalence in women 62.6%, versus 27.5% in men, making this difference statistically significant (<0.001) (see Table 2).
Table 2 Vitamin D status and body fat percentage prevalence by sex.
| Variables | Both sexes n (%) | Males n (%) | Females n (%) | p-value |
|---|---|---|---|---|
| BF% by Slaughter > 26% | 225 (45.5) | 66 (27.5) | 159 (62.6) | <0.001 |
| Vitamin D | ||||
| Deficiency (≤20 ng/mL) | 240 (48.5) | 120 (50.4) | 119 (46.8) | 0.722 |
| Insufficiency (21-29 ng/mL) | 82 (16.6) | 39 (16.2) | 43 (16.9) | |
| Sufficiency (≥30 ng/mL) | 172 (34.8) | 80 (33.6) | 92 (36.2) | |
Note. BF%: Body Fat percentage.
Vitamin D: 48.5% of the participants evidenced deficiency, 16.6% insufficiency and 34.8% showed sufficient levels. No statistically significant difference (<0.722) was found by sex. (see Table 2 and Figure 1)
Relationship between BF% and vitamin D levels
In the adjusted model, a statistically significant relationship was found between vitamin D insufficiency and elevated total cholesterol levels (RP = 1.99; 95% CI: 1.04-3.81). This suggests that participants with insufficient vitamin D levels were nearly twice as likely to present with high total cholesterol compared to those with sufficient levels. No statistically significant relationships were found between vitamin D deficiency or insufficiency and other cardiometabolic variables such as elevated glucose, triglycerides, HOMA-IR, HDL, LDL, insulin, or blood pressure (see Table 3)
Table 3 Relationship between serum vitamin D insufficiency (21-29 ng/mL) and BF%.
| Characteristics | Crude Model* | Adjusted Model** | ||||
|---|---|---|---|---|---|---|
| RP | 95% CI | p | RP | 95% CI | p | |
| BF% by Slaughter | 1.19 | 1.08-1.77 | 0.036 | 1.31 | 1.18-2.02 | 0.039 |
| Fasting glucose (mg/dL) | 0.98 | 0.95-1.01 | 0.468 | 0.98 | 0.95-1.01 | 0.409 |
| Total Cholesterol (mg/dL) | 1.99 | 1.09-2.00 | 0.039 | 1.99 | 1.09-2.06 | 0.040 |
| HDL Cholesterol (mg/dL) | 0.99 | 0.97-1.34 | 0.269 | 0.94 | 0.97-1.80 | 0.362 |
| LDL Cholesterol (mg/dL) | 0.99 | 0.98-1.78 | 0.126 | 0.97 | 0.98-1.40 | 0.119 |
| Triglycerides (mg/dL) | 1.00 | 0.99-1.55 | 0.459 | 1.18 | 0.99-2.00 | 0.437 |
Note. *: Models obtained through binomial regression. **: Model adjusted by sex and age. BF%: Body Fat percentage. RP: prevalence ratio. CI: confidence interval.
Low serum vitamin D levels: deficiency (RP 1.15 95% CI 1.05-2.02) and insufficiency (RP 1.31 95% CI 1.18-2.02) showed a statistically significant relationship with excess BF% compared with those with an adequate BF% (see Table 4).
Table 4 Relationship between serum vitamin D deficiency (20 ng/mL) and BF%.
Note. ** Model adjusted by sex and age. BF%: Body Fat percentage. RP: prevalence ratio. CI: confidence interval.
Discussion
The results of this study show similarity in the sociodemographic characteristics of the studied population. On the other hand, significant differences according to sex were found in anthropometric variables such as waist circumference, hip circumference, waist-to-hip ratio, waist-to-height ratio, and the two skinfold thickness measures evaluated. Biochemical variables such as HDL cholesterol, fasting glucose, and fasting insulin also showed significant differences according to sex (Table 1). Differences in physical composition, hormonal biology, weight gain patterns, and sensitivity to genetic and environmental factors between both sexes need to be addressed [24]. This analysis is relevant during puberty, a modulating stage of metabolic factors such as insulin sensitivity due to important hormonal interactions [25].
Overall, 45.5% of the studied population had an increased BF%, observing a higher prevalence in women with a statistically significant difference. Regarding vitamin D levels, deficiency was found in 48.5% of the participants, and insufficiency in 16.6% (see Table 2). This data contrasts with a Mexican study, that evidenced vitamin D deficiency in 42.9% and insufficiency in 46.2% of a population between the ages of 5 and 20 [26]. In another Mexican population between the ages of 6 and 19, 11.5% were found to be deficient and 33.5% to be insufficient of vitamin D. Additionally, a study in the Iranian population between the ages of 7 and 18 showed a deficiency and insufficiency of 10.6% and 60.5%, respectively [27]. These differences highlight the variability of vitamin D status across populations, with a higher deficiency and a lower insufficiency in the population sample.
In this study, vitamin D deficiency showed a statistically significant relationship with excess body fat. Case-control studies have indicated that obesity is associated with vitamin D deficiency in Danish and Chinese pediatric populations [28,29]. Likewise, the results of studies conducted in Mexican and Chilean children suggest that as the percentage of body fat decreases, the concentration of vitamin D increases [26,30]. Meanwhile, a representative sample of American children and adolescents showed an relationship between low serum vitamin D levels and obesity [24]. Sex-related predispositions have been observed about vitamin D deficiency, with a tendency for obesity in males as well as for abnormal levels of HDL cholesterol and insulin resistance in females [24].
The association between obesity and vitamin D deficiency has been widely discussed. Due to its fat-soluble nature, one hypothesis suggests that adipose tissue sequesters vitamin D or the storage capacity of this vitamin in adipose tissue increases in obese children. This prevents the proper release of the vitamin and may result in deficiency states [9]. Additionally, several studies have shown that there is a difference in the gene expression of cytochromes P450-2 J2 and P450-27b1 in subcutaneous adipose tissue between obese and healthy individuals. This suggests that adipose tissue may be involved in vitamin D’s metabolism and its relationship is not limited to storage [31].
The relationship between low levels of vitamin D and obesity has been demonstrated in this and other studies, but there is still little clarity about temporality. This suggests that low levels of vitamin D are a marker, rather than a cause of obesity [32]. However, a bi-directional genetic analysis of multiple cohorts suggests that a higher BMI leads to lower vitamin D levels, while the effect of low vitamin D levels on BMI increase is likely to be discrete [33].
Particularly, vitamin D deficiency showed a statistically significant relationship with total cholesterol in this study. Although no studies in which this specific variable had statistical significance were found, different results have indicated the relationship between low levels of vitamin D and abnormalities in the lipid profile in children and adolescents. Two studies in the American pediatric population showed an inverse relationship between vitamin D levels and HDL cholesterol [24,27]. The main component of HDL cholesterol is apolipoprotein A-1. Vitamin D is essential to maintain adequate levels of apolipoprotein A-1 and to increase lipoprotein lipase activity [27].
Fasting glucose levels did not show a statistically significant relationship with vitamin D. However, several studies have found inverse relationship between vitamin D levels and glucose levels as well as insulin resistance (HOMA-IR) [24-26,30]. Regarding gender differences, research in North American and Mexican populations reported lower insulin sensitivity in girls, in which high HOMA-IR and high insulin levels were observed about low levels of vitamin D [24,25].
Although this study provides relevant evidence on the relationship between excess adiposity and vitamin D levels in a pediatric population, some limitations must be acknowledged. The cross-sectional design allows for the identification of relationships but does not permit causal inference. Additionally, certain potentially relevant variables-such as sun exposure, physical activity, dietary intake of vitamin D and calcium, sunscreen use, and pubertal stage-were not included due to data unavailability, which may result in residual confounding.
Regarding the estimation of body fat percentage, the Slaughter equation based on skinfold measurements was employed, a widely used method in epidemiological research. However, in cases of excess adiposity, this technique may present technical limitations that could affect the accuracy of fat mass estimation. Moreover, the use of a single cutoff point (>26%) for both sexes was based on previous local studies; nonetheless, future research could benefit from sex- and age-specific thresholds to better reflect physiological differences.
Future research should adopt longitudinal or interventional designs to clarify the directionality of the relationship between adiposity and vitamin D levels. Furthermore, incorporating behavioral, environmental, and developmental variables-such as pubertal status-would enhance the robustness of analytical models. Despite its limitations, this study contributes valuable evidence to inform public health strategies aimed at preventing nutritional deficiencies in pediatric populations in Latin America.
Conclusions
In conclusion, this study identified a high prevalence of low vitamin D levels among the studied pediatric population. Vitamin D deficiency was significantly associated with excess body fat, while insufficiency showed an inverse relationship with total cholesterol levels. These findings underscore the relevance of timely identification and management of both suboptimal vitamin D status and excess adiposity as part of early strategies to prevent future metabolic risk in children and adolescents.