Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
DYNA
Print version ISSN 0012-7353
Dyna rev.fac.nac.minas vol.82 no.191 Medellín May/June 2015
https://doi.org/10.15446/dyna.v82n191.44700
DOI: http://dx.doi.org/10.15446/dyna.v82n191.44700
Comfort perception assessment in persons with transfemoral amputation
Valoración de la percepción de confort en personas con amputación transfemoral
Juan Fernando Ramírez-Patiño a, Derly Faviana Gutiérrez-Rôa b & Alexander Alberto Correa-Espinal c
a Facultad de Minas, Universidad Nacional de Colombia, Medellín, Colombia. jframirp@unal.edu.co
b Facultad de Minas, Universidad Nacional de Colombia, Medellín, Colombia. dfgutierrezr@unal.edu.co
c Facultad de Minas, Universidad Nacional de Colombia, Medellín, Colombia. alcorrea@unal.edu.co
Received: July 30th, 2014. Received in revised form: November 14th 2014. Accepted: April 30th, 2015.
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.

Abstract
Historically, the design and fitting of prostheses had to rely on a slow process of trial and error, depending on the expertise of the prosthetist. Therefore, a clear definition of the concept of comfort and clear knowledge of its contributing factors are important when designing comfortable prostheses. However, there are currently no standardized methods to adequately measure prosthesis-related comfort. The aim of this study is to identify the factors that underlie the concept of comfort with prosthesis use in transfemoral amputees. Forty-one transfemoral amputees completed a questionnaire to evaluate the perception of comfort and to analyze the influence of six factors. It found a significant model that correctly classifies 84.9% of the cases. It can predict whether the patient feels comfort while using the prosthesis. Although all of the factors were significant, the factors with the greatest influence on the perception of comfort were functionality and pain.
Keywords: rehabilitation; trans-femoral amputees; prostheses; comfort.
Resumen
Históricamente, el diseño y ajuste de prótesis es un proceso lento de ensayo y error que depende de la experiencia del protesista. Por lo tanto, una definición clara del concepto de confort es importante para diseñar prótesis cómodas y para el conocimiento de los factores que le contribuyen. Sin embargo, actualmente no existen métodos estandarizados para medir adecuadamente el confort cuando se usan prótesis. Este estudio identifica los factores que subyacen en el concepto de confort al usar prótesis. 41personas con amputación transfemoral completaron un cuestionario para evaluar la percepción de confort y analizar la influencia de seis factores. Se encontró un modelo significativo que clasifica correctamente el 84,9 % de los casos, lo que permite predecir si el paciente siente confort durante el uso de la prótesis. Aunque todos los factores fueron significativos, los factores que más influyen en la percepción de confort fueron funcionalidad y dolor.
Palabras clave: rehabilitación; amputados transfemorales; prótesis; confort.
1. Background
Despite the frequent use of the term, there is no widely accepted definition of comfort. In transfemoral amputees, the term "comfort" is used in reference to two groups: the rehabilitation of the patient and the interactions with the residual limb and prosthetic socket.
For the first group, comfort is a subscale of the physical and social well-being of the individual's quality of life, which is represented by the degree of rehabilitation and is measured as the independence of the individual to perform daily activities [1]. Because no universal consensus exists regarding the optimal instrument, several questionnaires have been developed to assess the rehabilitation treatment [2] or prosthesis-related quality of life of transfemoral amputees [3-10]. In these instruments, mobility is commonly regarded as an important factor [11-13] together with pain.
When evaluating comfort, such as the interaction between the socket and the residual limb, the ability to perform common daily activities is directly related to both fit and discomfort [6,14-16]. Comfort may also be defined as a constitutive aspect of the satisfaction with the use of the prosthesis [8]. Pain sensations may be associated with discomfort, although pain and discomfort are not necessarily correlated because other factors may lead to discomfort [15,17]. The static and dynamic alignment of the prosthetic system during adaptation and the subsequent transmission and distribution of pressure determine the comfort of the amputee's gait [18]. In the measurement of comfort within the socket, several authors agree on the absence of a measurable scale of comfort [6,15,17,19,20]. In the literature, only one study attempted to directly measure the level of comfort felt by the amputee in the socket. That study offered the hypothesis that pain and comfort are subjective perceptions and adapted a numerical scale, initially used to measure pain [6].
The vast majority of studies that investigate the effects of prosthesis design on the amputee's performance have compared the biomechanical and physiological effects of different prostheses. Other studies have referenced the mechanical properties of the prosthesis that directly influence the comfort and performance of the amputee [21]. Unfortunately, currently, there are no standardized, well-accepted methods to adequately measure prosthesis-related comfort either for research or for clinical use.
Incorrect measures of comfort cause delays in the adjustment of the socket by the prosthetic technicians, who must rely on a slow process of trial and error [16,18]. Historically, the design, construction, and fitting of prostheses have been an art, depending on the accumulated expertise of the practitioner [22]. This situation requires the use of non-standardized descriptive terms to express comfort, which must be explained to the patient, the practitioner and the prosthetic technician. Efforts should be directed at improving communication between patients and practitioners, to improve the quality of care provided to the growing numbers of persons with limb loss [23]. The non-standardized terms prevent the implementation of accurate clinical measurements of the patient's perception of comfort. Furthermore, each patient has a different way of assessing his/her perception of comfort [17], which may vary over time [24,25] and increases the difficulty of developing a standardized scale.
In the comfort theories based on studies on comfort in sitting, some issues are generally accepted [26]: (1) comfort is a construct of a subjectively defined personal nature; (2) comfort is affected by factors of various natures (physical, physiological, psychological); and (3) comfort is a reaction to the environment.
Therefore, a clear definition of the concept of comfort is important to the rehabilitation practitioners and researchers, as is knowledge about which factors contribute to the comfort with prosthesis use, and their relative importance. However, there is a lack of knowledge about comfort in persons with transfemoral amputation. Until now, relatively few studies have analyzed the factors that influence quality of life [27] in transfemoral amputees, but their relationships with the patient's comfort experience are generally unknown.
The aim of this research was to identify the factors that underlie the concept of comfort with prosthesis use in transfemoral amputees. In order to achieve this goal, whether there are significant differences between the persons with transfemoral amputation who feel comfort and persons who feel discomfort when using prosthesis, was determined through a modified scale.
2 Methods
2.1 Participants
The participants were invited by telephone using databases from organizations involved with disabled individuals. The study region was limited to Antioquia, Colombia, and the study included persons with unilateral transfemoral amputations and who used prosthesis for ambulation with or without an additional mobility aid.
The Universidad Nacional de Colombia ethics committee granted ethical approval for the study. After written consent, the subjects were asked to complete a questionnaire.
2.2 Questionnaire
To determine the factors that underlie the concept of comfort in transfemoral amputees, we prepared a questionnaire with 30 questions organized into the following six scales or factors: appearance, well-being, pain, functionality, psychological health and social health. These were based on the Prosthesis Evaluation Questionnaire (PEQ) for psychometric properties. Because the factors were not dependent on one another, only the factors relevant to the research question were used. The following questions were added to the PEQ: "Do you feel comfort when using your prosthesis?" "Which of these factors improves your comfort?" and "Which of these factors reduces your comfort?" The questionnaire was available in Spanish.
The original scale uses a 100 mm Visual Analog Scale (VAS), but for the purposes of the present study, we decided to change it because it has been reported in the literature that older and less educated patients experienced difficulty understanding the VAS response format, and the instructions of the questionnaire needed to be explained carefully [25,28,29]. Similar observations were reported by Guyatt et al. [30], who found subjects had fewer problems and required less training, by using a numerically based Likert scale as opposed to a VAS. The Italian validation of the PEQ suggests the need for simplifying the questionnaire format to be feasible for widespread clinical use [29,31]. The PEQ uses a VAS because the questions cover a wide variety of response types; however, the VAS is not necessarily more accurate than multiple-choice responses [32].
Responding to a 30 question survey can be tedious, especially when it is related to a sensitive topic. The PEQ design requires an instrument that captures the participants' attention, encourages reading, and is easy to answer. Therefore, we designed six boards measuring 43 x 28 centimeters, with one board for each factor (Fig. 1). The verbal scales of the six categories were adapted to the content of each question to allow a minimum and maximum response to each question. The final survey included 24 direct questions and 6 indirect questions. The final survey included 24 direct questions and 6 indirect questions (Appendix 1). Several distinguishing characteristics were used to define each factor to convey the concept it represented. Each board was named and was given a color, an image and a different pictogram to reinforce the concept of each factor on each board.A moderator was trained in the use of the instrument. The original questionnaire has an inclusion criterion that patients are able to read because it is a self-administered questionnaire. The literacy requirement could be a limitation to the widespread use of the instrument in clinical practice because a percentage of patients, especially older and less educated patients, have difficulty understanding written language or are visually impaired.
2.3 Conducting the analytical survey
Without defining "comfort," the moderator asked whether the participant felt comfort while using the prosthesis. Then, the participant answered the questions using the six boards. When necessary, the moderator read the questions and multiple-choice responses without further clarification. Finally, the moderator introduced all of the boards to the participant and asked the following questions twice, independently: "Which of these factors improves your comfort?" and "Which of these factors reduces your comfort?" There was no compensation for participation.
2.4 Statistical analyses
The statistical analysis used in the PEQ was factor analysis, which is a descriptive method that provides a direct view of the interrelationships between the variables, and allows information reduction. After finding the underlying structure among a number of variables, it is important to determine the relationships between the independent and dependent variables. The most appropriate statistical technique is logistic regression because it only requires data concerning whether an event occurred (e.g., whether the patient feels comfort or not) as a dependent variable for predicting the probability that the event may or may not take place. Logistic regression does not require any assumptions of normality, linearity or homogeneity of variance for the independent variables.
3. Results
3.1. Participants' profile
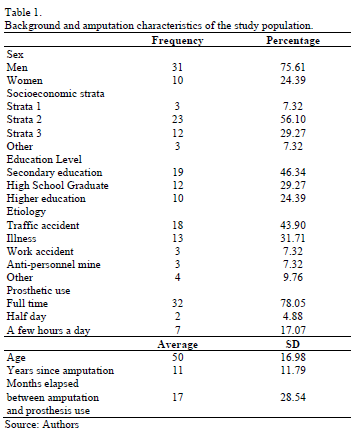
Although 85 individuals were invited, surveys were conducted with 41 participants. Table 1 provides detailed data regarding the study sample. The participants were 75.61% male and mainly belonged to socioeconomic strata 2 and 3, which are areas with many economic constraints. In Colombia, households are classified into six strata, with strata 1 identified as the poorest. The participants exhibited a low level of education: 46.34% of the participants did not complete high school, and only 24.39% of the participants obtained technical degrees or higher. Of the 41 surveys conducted, three were eliminated because of contradictions in the participants' answers.
3.2. Constructing dummy variables
The participants' answers were coded for the statistical analysis using dummy variables based on a scale of zero to five depending on the direction of the question (direct or indirect). The highest score corresponded to the most positive response, and the lowest score corresponded to the most negative response.
3.3. Sample size and division of the sample
The logistic regression technique is sensitive to the relationship between sample size and the number of predictor variables. At least five observations per each predictor variable should be used, and the sample size of each group should be considered. The smallest group must be larger than the number of independent variables. The technique requires that the sample is split into two sub-samples: one sample is used to estimate the model, and the other sample is used for validation. However, the study did not properly split the sample, and it was constructed from the responses obtained from participants, owing to the sample size.
3.3.1. Sample for validation
The coded responses of the same factor were averaged to obtain the values of the independent variables. The dependent variable was obtained from the answer to the question, "Do you feel comfort when using your prosthesis?" The validation sample has a size of 38 data points.
3.3.2. Sample for estimating model
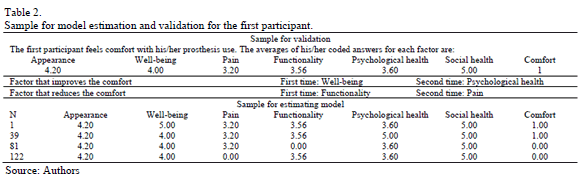
As in the validation sample, the coded responses of the same factor were averaged to obtain the values of each factor. The sample was extended until it was four times the initial size (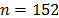 ). For the first 38 data points, the first factor that was chosen by the participant as enhancing comfort was replaced by 5, and the other values remained constant. For the next 38 data points, the second factor was treated the same way. For the first group (
). For the first 38 data points, the first factor that was chosen by the participant as enhancing comfort was replaced by 5, and the other values remained constant. For the next 38 data points, the second factor was treated the same way. For the first group (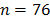 ), the dependent variable was converted to 1, which corresponded to comfort. The following 76 data points were treated in the same manner, except that the factors that reduce comfort were set to 0, and the dependent variable corresponding with discomfort was set to 0, which was used as the second group. All of the processes for the first participant are shown in Table 2.
), the dependent variable was converted to 1, which corresponded to comfort. The following 76 data points were treated in the same manner, except that the factors that reduce comfort were set to 0, and the dependent variable corresponding with discomfort was set to 0, which was used as the second group. All of the processes for the first participant are shown in Table 2.
3.4. Regression model
The model was estimated using SPSS Version 15 and the backward stepwise method with the Wald statistic as contrast. The 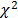 of the model is significant at
of the model is significant at 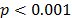 and the independent variables describing the dependent variable significantly differ with a Nagelkerke's R-Square of 0.654, which correctly classifies 84.9% of the cases.
and the independent variables describing the dependent variable significantly differ with a Nagelkerke's R-Square of 0.654, which correctly classifies 84.9% of the cases.
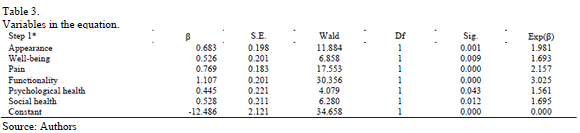
Table 3 presents the variables in the equation. The Wald statistic of the coefficients 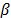 is significant for all of the factors (
is significant for all of the factors (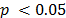 ). The
). The 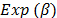 value represents the extent to which raising the corresponding measure by one unit influences the odds. Larger values belong to the functionality and pain factors. Then, eq. (1) shows the probability equation that was used to evaluate whether a transfemoral amputee feels comfort with the use of the prosthesis.
value represents the extent to which raising the corresponding measure by one unit influences the odds. Larger values belong to the functionality and pain factors. Then, eq. (1) shows the probability equation that was used to evaluate whether a transfemoral amputee feels comfort with the use of the prosthesis.
The validation process using the corresponding sample showed that the estimated model classified 73.17% of cases.

4. Discussion
The aim of this study was to find the underlying factors of comfort with prosthesis use in persons with transfemoral amputation, through the modification of a previously validated questionnaire, which allows practitioners to overcome the implementation difficulties reported in the literature. Forty-one transfemoral amputees who used prosthesis and varied by age, sex, reason for amputation and years since amputation, completed a questionnaire using audio plugs to select their answers. Only persons with bilateral lower limb amputations were not included in this study.
The conducted empirical application detects the existence of statistically significant differences between patients who feel comfort or discomfort with the prosthesis. Therefore, it was possible to identify the factors that underlie the concept of comfort with prosthesis use in transfemoral amputees. The factors analyzed in this study were appearance, well-being, pain, functionality, psychological health and social health. Although all of the factors analyzed were significant, the factors with the greatest influence on the perception of comfort were functionality and pain, as in previous studies about factors related to quality of life [3].
In the literature, two main approaches to quality of life measurement can be found; functionalist and needs-based. The authors argued that human needs are the foundations for quality of life and that quality of life is the degree of satisfaction of those needs [33]. This is reminiscent of Maslow's hierarchy of need in which five levels of needs were identified and postulated that they are satisfied in strict sequence. Physiological needs are the physical requirements for human survival. If these requirements are not met, the human body cannot function properly, and will ultimately fail. Physiological needs are thought to be the most important; they should be met first. With their physical needs relatively satisfied, the individuals' safety needs take precedence and dominate behavior. Safety needs include health and well-being, safety net against accidents or illness and their adverse impacts.
This study concurs with these findings, because the functionality factor focuses on the ease, usefulness, convenience and mobility using the prosthesis. The influence of this factor may be due to the economic situation of the sample studied. Low-income patients may have difficulties acquiring more technologically advanced prosthetic systems, which would allow them to move more easily. A patient's desire to acquire a prosthetic system to meet all his/her functional needs may be a basic requirement to perceive comfort. After the basic necessities of functionality are covered, patients do not want the prosthesis to cause pain, which is an adverse impact of an illness.
It is, however, noteworthy that appearance, the third most important factor, differs from the third need: love and belonging. This can be explained by the high degree of vanity that culturally exists among Colombians. It is also evidenced that there are potential differences between the patients' and clinicians' goals, such as restoring the walking function versus appearance. The practitioner is primarily interested in subjective and objective measures relating to function and sometimes forgets the significant differences between the rehabilitation expectations of the patients, whereas the patient is often more interested in communicating their subjective personal impressions [19]. The organization into a hierarchy factors, will help researchers and designers to focus on specific therapeutic solutions for these patients.
Additionally, this finding provides tools to determine whether the patient experiences comfort with the use of the prosthesis, which are quick and easy to set up, administer, and analyze. This prediction will improve the communication between the patient, the doctor and the prosthetic technician. Practitioners will know when a person has actually become accommodated to a new prosthesis or a new prosthetic component. This will in turn avoid delays that could cause deterioration of the soft tissues of the residual limb, abnormal gait patterns of the amputee, decreased productive capacity and social reintegration of disabled patients and complexes such as depression after a traumatic loss of a limb [8] that result in personal and social losses given that most amputees in developing countries are young working people [34]. Most of the innovations made throughout the years have been aimed at helping amputees to return to their working lives [35].
For future applications of the instrument, the authors believe that the patient can complete the questionnaire without the presence of the moderator. In clinical practice, the patient could answer the questions using the boards in the waiting room without making a doctor's appointment. In future studies, the boards could be answered by the patient at home if the patient exhibits a sufficient education level and then mailed.
Because the PEQ was modified for the purpose of the present study, further testing is required to compare the PEQ's use, reliability, and responsiveness by using different response options.
In this study, we calculated summary scores for each scale. This approach assumes equality between the different levels of the response categories. Additional research, by using techniques such as Rasch Analysis, should be conducted to test this assumption.
5. Conclusions
The conducted empirical application detects the existence of statistically significant differences between patients who feel comfort or discomfort with the prosthesis.
Comfort for transfemoral amputees is determined by interactions among the following factors: functionality, pain, appearance, well-being, psychological health and social health. The degree of influence for each factor on the construct is similar to Maslow's hierarchy of needs.
Acknowledgments
We are grateful to all of the study participants. We express our deepest gratitude to Orthopraxis, the moderators, Robinson Chica for designing images for the boards, Francisco Restrepo for the layout of the boards, and all of the people who contributed directly and indirectly to this research.
References
[1] Bosmans, J., Suurmeijer, T., Hulsink, M., van der Schans, C., Geertzen, J. and Dijkstra, P., Amputation, phantom pain and subjective well-being: a qualitative study. International Journal of Rehabilitation Research, 30 (1), pp.1-8, 2007. DOI: 10.1097/MRR.0b013e328012c953 [ Links ]
[2] Kent, R. and Fyfe, N., Effectiveness of rehabilitation following amputation. Clinical Rehabilitation, 13 (1), pp. 43-50, 1999. DOI: 10.1191/026921599676538002 [ Links ]
[3] Demet, K., Martinet, N., Guillemin, F., Paysant, J. and André, J-M., Health related quality of life and related factors in 539 persons with amputation of upper and lower limb. Disability and Rehabilitation, 25 (9), pp. 480-486, 2003.DOI: 10.1080/0963828031000090434 [ Links ]
[4] Gallagher, P., Franchignoni, F., Giordano, A. and MacLachlan, M., Trinity amputation and prosthesis experience scales: A psychometric assessment using classical test theory and rasch analysis. American Journal of Physical Medicine Rehabilitation, 89 (6), pp. 487-496, 2010. DOI: 10.1097/PHM.0b013e3181dd8cf1 [ Links ]
[5] Hagberg, K., Brånemark, R. and Hägg, O. Questionnaire for Persons with a Transfemoral Amputation (Q-TFA): initial validity and reliability of a new outcome measure. Journal of Rehabilitation Research and Development, 41 (5), pp. 695-706, 2004. doi: 10.1682/JRRD.2003.11.0167 [ Links ]
[6] Hanspal, R., Fisher, K. and Nieveen, R., Prosthetic socket fit comfort score. Disability and Rehabilitation, 25 (22), pp. 1278-1280, 2003. DOI: 10.1080/09638280310001603983 [ Links ]
[7] Legro, M., Reiber, G., Smith, D., del Aguila, M., Larsen, J. and Boone, D., Prosthesis evaluation questionnaire for persons with lower limb amputations: Assessing prosthesis-related quality of life. Archives of Physical Medicine and Rehabilitation, 79 (8), pp. 931-938, 1998. DOI: 10.1016/S0003-9993(98)90090-9 [ Links ]
[8] Rybarczyk, B., Nyenhuis, D., Nicholas, J., Schulz, R., Alioto R, Blair C., Social discomfort and depression in a sample of adults with leg amputations. Archives of Physical Medicine and Rehabilitation [Online]. 73 (12), pp. 1169-1173, 1992. [date of reference July 27th of 2010]. Available at: http://www.archives-pmr.org/article/0003-9993(92)90116-E/pdf [ Links ]
[9] Ware, J., Kosinski, M. and Keller, S., A 12-Item short-form health survey: Construction of scales and preliminary tests of reliability and validity. Medical Care [Online]. 3 (34), pp. 220-233, 1996. [date of reference July 26th of 2010]. Available at: http://www.jstor.org/stable/3766749 [ Links ]
[10] Ware, J. and Sherbourne, C., The MOS 36-item short-form health survey (SF-36): I. Conceptual framework and item selection. Medical Care, 6 (30), pp. 473-483, 1992. DOI: 10.1097/00005650-199206000-00002 [ Links ]
[11] Franchignoni, F., Orlandini, D., Ferriero, G. and Moscato, T., Reliability, validity, and responsiveness of the locomotor capabilities index in adults with lower-limb amputation undergoing prosthetic training. Archives of Physical Medicine and Rehabilitation, 85 (5), pp. 743-748, 2004. DOI: 10.1016/j.apmr.2003.06.010 [ Links ]
[12] Rommers, G., Vos, L., Groothoff, J. and Eisma, W., Mobility of people with lower limb amputations, scales and questionnaires: A review. Clinical Rehabilitation, 15 (1), pp. 92-102, 2001. DOI: 10.1191/026921501677990187 [ Links ]
[13] Treweek, S. and Condie, M., Three measures of functional outcome for lower limb amputees: a retrospective review. Prosthetis and Orthotics International, 22 (3), pp. 178-185, 1998. DOI: 10.3109/03093649809164482 [ Links ]
[14] Van de Meent, H., Hopman, M. and Frölke, J., Walking ability and quality of life in subjects with transfemoral amputation: A comparison of osseointegration with socket prostheses. Archives of Physical Medicine and Rehabilitation, 94 (11), pp. 2174-2178, 2013. DOI: 10.1016/j.apmr.2013.05.020 [ Links ]
[15] Neumann, E., Measurement of socket discomfort-part I: Pressure sensation. Journal of Prosthetics and Orthotics, 13 (4), pp. 99-110, 1992. DOI: 10.1097/00008526-200112000-00010 [ Links ]
[16] Zheng, Y., Mak, A. and Leung, K., State-of-the-art methods for geometric and biomechanical assessments of residual limbs: a review. Journal of Rehabilitation Research and Development [Online]. 38 (5), pp. 487-504, 2001. [date of reference June 28th of 2010]. Available at: http://www.rehab.research.va.gov/jour/01/38/5/pdf/zheng.pdf [ Links ]
[17] Harms-Ringdahl K, Brodin H, Eklund L, Borg G., Discomfort and pain from loaded passive joint structures. Scandinavian Journal of Rehabilitation Medicine [Online]. 15 (4), pp. 205-211, 1983. [date of reference June 26th of 2010]. Available at: http://www.ncbi.nlm.nih.gov/pubmed/6648392 [ Links ]
[18] Meier, R. 3rd, Meeks, E. and Herman, R., Stump-socket fit of below-knee prostheses: Comparison of three methods of measurement. Archives of Physical Medicine and Rehabilitation [Online]. 54 (12), pp. 553-558, 1973. [date of reference July 10th of 2010]. Available at: http://www.ncbi.nlm.nih.gov/pubmed/4759446 [ Links ]
[19] Miller, L. and McCay, J., Summary and conclusions from the academy's sixth state-of-the-science conference on lower limb prosthetic outcome measures. Journal of Prosthetics and Orthotics [Online]. 18 (1s), pp. 2-7, 2006. [date of reference July 12th of 2010]. Available at: http://www.oandp.org/jpo/library/2006_01S_002.asp [ Links ]
[20] Smith, D., Special challenges in outcome studies for amputation surgery and prosthetic rehabilitation. Journal of Prosthetics and Orthotics [Online]. 18 (1s), pp. 116-118, 2006. [date of reference July 12th of 2010]. Available at: http://www.oandp.org/jpo/library/2006_01S_116.asp [ Links ]
[21] Major, M., Twiste, M., Kenney, L. and Howard, D., Amputee independent prosthesis properties-a new model for description and measurement. Journal of Biomechanics, 44 (14), pp. 2572-2575, 2011. DOI: 10.1016/j.jbiomech.2011.07.016 [ Links ]
[22] Papaioannou, G., Mitrogiannis, C., Nianios, G. and Fiedler, G., Assessment of amputee socket-stump-residual bone kinematics during strenuous activities using Dynamic Roentgen Stereogrammetric Analysis. Journal of Biomechanics, 43 (5), pp. 871-878, 2010. DOI: 10.1016/j.jbiomech.2009.11.013 [ Links ]
[23] Pezzin, L., Dillingham, T., MacKenzie, E., Ephraim, P. and Rossbach, P., Use and satisfaction with prosthetic limb devices and related services. Archives of Physical Medicine and Rehabilitation, 85 (5), pp. 723-9, 2004. DOI: 10.1016/j.apmr.2003.06.002 [ Links ]
[24] Neumann, E., Measurement of socket discomfort-part II: Signal detection. Journal of Prosthetics and Orthotics, 13 (4), pp. 111-122, 2001. doi: 10.1097/00008526-200112000-00011 [ Links ]
[25] Zidarov, D., Swaine, B. and Gauthier-Gagnon, C., Quality of life of persons with lower-limb amputation during rehabilitation and at 3-month follow-up. Archives of Physical Medicine and Rehabilitation, 90 (4), pp. 634-645, 2009. DOI: 10.1016/j.apmr.2008.11.003 [ Links ]
[26] De Looze, M., Kuijt-Evers, L. and van Dieën J., Sitting comfort and discomfort and the relationships with objective measures. Ergonomics, 46 (10), pp. 985-997, 2003. DOI: 10.1080/0014013031000121977 [ Links ]
[27] Sinha, R., van den Heuvel, W. and Arokiasamy, P., Factors affecting quality of life in lower limb amputees. Prosthetis and Orthotics International, 35 (1), pp. 90-96, 2011. DOI: 10.1177/0309364610397087 [ Links ]
[28] Ferrand-Ferri, P., Rodríguez-Piñero Durán, M., Echevarría-Ruiz de Vargas, C. and Zarco-Periñán, M.J., Versión española del Prosthesis Evaluation Questionnaire (PEQ): Parte inicial de su adaptación transcultural. Rehabilitación, 41 (3), pp. 101-107, 2007. DOI: 10.1016/S0048-7120(07)75496-8 [ Links ]
[29] Miller, W., Deathe, A. and Speechley, M., Lower extremity prosthetic mobility: a comparison of 3 self-report scales. Archives of Physical Medicine and Rehabilitation, 82 (10), pp. 1432-1440, 2001. DOI: 10.1053/apmr.2001.25987 [ Links ]
[30] Guyatt, G., Townsend, M., Berman, L. and Keller, J., A comparison of Likert and visual analogue scales for measuring change in function. Journal of Chronic Diseases, 40 (12), pp. 1129-1133, 1987. DOI: 10.1016/0021-9681(87)90080-4 [ Links ]
[31] Ferriero, G., Dughi, D., Orlandini, D., Moscato, T., Nicita, D. and Franchignoni, F., Measuring long-term outcome in people with lower limb amputation: Cross-validation of the Italian versions of the prosthetic profile of the amputee and prosthesis evaluation questionnaire. Europa Medicophysica [Online]. 1 (41), pp. 1-6, 2005. [date of reference September 24th of 2010]. Available at: http://www.researchgate.net/profile/Franco_Franchignoni [ Links ]
[32] Fitzpatrick, R., Davey, C., Buxton, M. and Jones, D., Evaluating patient-based outcome measures for use in clinical trials. Health Technology Assessment. [Online]. 2 (14), pp. 1-74, 1998. [date of reference June 25th of 2010]. Available at: http://www.soton.ac.uk/~hta [ Links ]
[33] Hörnquist, J., The concept of quality of life. Scandinavian Journal of Social Medicine, 10 (2), pp. 57-61, 1982. DOI: 10.1177/140349489001800111 [ Links ]
[34] Restoration. From surgery to community reintegration. Disability and Rehabilitation, 26 (14-15), pp. 8318-36, 2004. DOI: 10.1080/09638280410001708850 [ Links ]
[35] Loaiza, J. and Arzola, N., Evolución y tendencias en el desarrollo de prótesis de mano, DYNA [Online]. 78 (169), pp 191-200, 2011. [date of reference July 25th of 2013]. Available at: http://www.scielo.org.co/scielo.php?script=sci_arttext&pid=S0012-73532011000500022&lng=en&nrm=iso [ Links ]
J.F. Ramírez-Patiño, graduado de Ing. Mecánico de la Universidad Nacional de Colombia en 1999, MSc en Ingeniería Mecánica de la Universidad Simón Bolívar, Venezuela en 2002 y Dr. en Ingeniería de la Universidad Nacional de Colombia en 2011. Profesor de tiempo completo del Departamento de Ingeniería Mecánica, Facultad de Minas, Universidad Nacional de Colombia.
D.F. Gutiérrez-Rôa, graduada de Ing. Industrial de la Universidad Mayor de San Simón, Bolivia en 2004, Esp. en Sistemas de Gestión de Calidad en 2006 y MSc en Ingeniería Administrativa de la Universidad Nacional de Colombia en 2010.
A.A. Correa-Espinal, graduado de Ing. Industrial de la Universidad Nacional de Colombia en 1995, MSc en Ingeniería Industrial de la Universidad de los Andes, Colombia en 1999 y Dr en Estadística e Investigación Operativa de la Universidad Politécnica de Cataluña, España en 2007. Profesor de tiempo completo del Departamento de Ingeniería de la Organización, Facultad de Minas, Universidad Nacional de Colombia.
Appendix 1
Factors, questions and multiple answers for assessment the perception of comfort in persons with transfemoral amputation:
Apariencia
1. ¿Qué tan agradable es el contacto de su muñón con su socket?
- Nada agradable
- Muy poco agradable
- Poco agradable
- Medianamente agradable
- Muy agradable
- Exageradamente agradable
2. ¿Qué tan bien luce Usted con su prótesis?
- No luzco bien
- Luzco muy poco bien
- Luzco poco bien
- Luzco medianamente bien
- Luzco muy bien
- Luzco exageradamente bien
3. ¿Durante el uso de su prótesis, cuánto le molesta el sonido que produce?
- No me molesta
- Me molesta muy poco
- Me molesta poco
- Medio me molesta
- Me molesta mucho
- Su sonido es insoportable
4. ¿Cuántas veces ha dañado su prótesis a su ropa?
- Nunca la ha dañado
- La ha dañado muy pocas veces
- La ha dañado pocas veces
- La ha dañado algunas veces
- La ha dañado muchas veces
- Siempre la daña
5. ¿Qué tanto le limita su prótesis la elección de ropa y zapatos?
- No me limita
- Me limita muy poco
- Me limita poco
- Me limita medianamente
- Me limita mucho
- Siempre me limita
Bienestar
6. Usando su prótesis, ¿qué tanto aumenta la sudoración de su muñón?
- No aumenta
- Aumenta muy poco
- Aumenta poco
- Aumenta medianamente
- Aumenta mucho
- Aumenta exageradamente
7. En el último año, ¿cuántas veces ha tenido que cambiar de socket porque su muñón ha cambiado de tamaño?
- Cero veces
- Una vez
- Dos veces
- Tres veces
- Cuatro veces
- Cinco veces o más
8. ¿Ha sentido o detectado algún brote o salpullido en su muñón por el uso de su prótesis?
- Nunca lo he sentido
- Muy pocas veces lo he sentido
- Pocas veces lo he sentido
- Algunas veces lo he sentido
- Muchas veces lo he sentido
- Siempre lo he sentido
9. ¿Qué tan a menudo se le generan ampollas, raspones o moretones en su muñón por el socket?
- Nunca los he tenido
- Muy pocas veces los he tenido
- Pocas veces los he tenido
- Algunas veces los he tenido
- Muchas veces los he tenido
- Siempre los he tenido
10. ¿Con qué frecuencia las molestias ocasionadas por el uso de su prótesis, le han incapacitado realizar sus actividades cotidianas?
- Nunca
- Muy pocas veces
- Pocas veces
- Algunas veces
- Muchas veces
- Siempre
Dolor
11. Usando la prótesis, ¿Con que frecuencia ha sentido dolor en su muñón?
- Nunca
- Muy pocas veces
- Pocas veces
- Algunas veces
- Muchas veces
- Siempre
12. Usando su prótesis, ¿Con que frecuencia ha sentido dolor en su otra pierna?
- Nunca
- Muy pocas veces
- Pocas veces
- Algunas veces
- Muchas veces
- Siempre
13. Usando su prótesis, ¿Con que frecuencia ha sentido dolor en su espalda?
- Nunca
- Muy pocas veces
- Pocas veces
- Algunas veces
- Muchas veces
- Siempre
14. ¿Con que frecuencia ha dejado de usar su prótesis debido al dolor que ésta le causa?
- Nunca
- Muy pocas veces
- Pocas veces
- Algunas veces
- Muchas veces
- Siempre
15. ¿Con que frecuencia ha sentido dolor mientras se coloca su prótesis?
- Nunca
- Muy pocas veces
- Pocas veces
- Algunas veces
- Muchas veces
- Siempre
Funcionalidad
16. ¿Qué tan bien se ajusta su socket a su muñón?
- No se ajusta bien
- Se ajusta muy poco bien
- Se ajusta poco bien
- Se ajusta medianamente bien
- Se ajusta muy bien
- Se ajusta exageradamente bien
17. ¿Qué tan pesada siente su prótesis?
- Nada pesada
- Muy poco pesada
- Poco pesada
- Medianamente pesada
- Muy pesada
- Exageradamente pesada
18. Cuando usa su prótesis, ¿su socket le dificultad estar sentado?
- Nunca
- Muy pocas veces
- Pocas veces
- Algunas veces
- Muchas veces
- Siempre
19. ¿Cuánto esfuerzo requiere para realizar sus actividades cotidianas utilizando su prótesis?
- Ningún esfuerzo
- Muy poco esfuerzo
- Poco esfuerzo
- Algún esfuerzo
- Mucho esfuerzo
- Esfuerzo exagerado
20. ¿Qué tan fácil es ponerse su prótesis?
- Nada fácil
- Muy poco fácil
- Poco fácil
- Medianamente fácil
- Muy fácil
- Exageradamente fácil
21. ¿En cuál de los siguientes niveles de movilidad se clasificaría usted?
- Puede caminar a un ritmo fijo
- Puede caminar sobre obstáculos
- Puede caminar a un ritmo variable
- Puede caminar libremente
Psicológico
22. ¿Qué tan feliz se siente con su prótesis?
- Nada feliz
- Muy poco feliz
- Poco feliz
- Medianamente feliz
- Muy feliz
- Exageradamente feliz
23. ¿Qué tan frecuentemente se siente frustrado con su prótesis?
- Nunca
- Muy pocas veces
- Pocas veces
- Algunas veces
- Muchas veces
- Siempre
24. Usando su prótesis, ¿siente usted que la gente la observa?
- Nunca
- Muy pocas veces
- Pocas veces
- Algunas veces
- Muchas veces
- Siempre
25. Usando su prótesis, ¿con qué frecuencia hace uso de piscinas, gimnasios o centros recreativos?
- Nunca
- Muy pocas veces
- Pocas veces
- Algunas veces
- Muchas veces
- Siempre
26. Usando su prótesis, ¿con qué frecuencia ha evitado relacionarse con personas desconocidas?
- Nunca
- Muy pocas veces
- Pocas veces
- Algunas veces
- Muchas veces
- Siempre
Social
27. Usando su prótesis, ¿con qué frecuencia evita hacer actividades que puedan generar reacciones en los demás?
- Nunca
- Muy pocas veces
- Pocas veces
- Algunas veces
- Muchas veces
- Siempre
28. Usando su prótesis, ¿Con qué frecuencia se ha sentido rechazado por su familia?
- Nunca
- Muy pocas veces
- Pocas veces
- Algunas veces
- Muchas veces
- Siempre
29. Usando su prótesis, ¿Con qué frecuencia se ha sentido rechazado por su entorno social?
- Nunca
- Muy pocas veces
- Pocas veces
- Algunas veces
- Muchas veces
- Siempre
30. Usando su prótesis, ¿con qué frecuencia se ha sentido incapaz de cuidar de alguien más?
- Nunca
- Muy pocas veces
- Pocas veces
- Algunas veces
- Muchas veces
- Siempre