INTRODUCTION
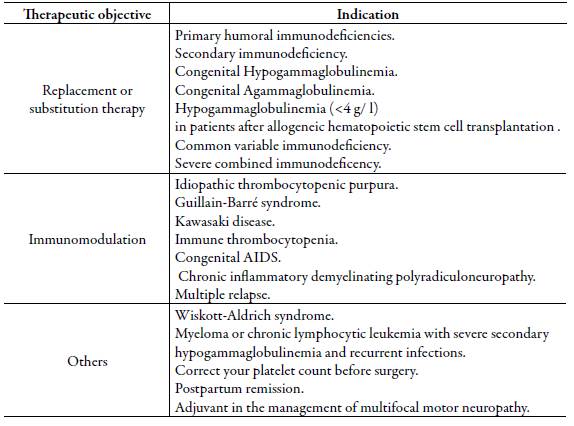
Non-specific intravenous human immunoglobulin (IVIG) is a valuable therapeutic resource in pathologies such as primary and secondary immunodeficiencies, autoimmune diseases, neurological disorders, infections, transplants, and others in which its efficacy has been demonstrated [1]. However, there are pathological conditions for which there is not yet a defined therapeutic strategy and due to similarity or biological plausibility some prescribers end up using it. Currently in Colombia, the Food and Drug Surveillance Institute (Invima by its initials in Spanish) has approved 39 registries in force or in the process of renewal and it is indicated for the replacement treatment in primary immunodeficiency, secondary immunodeficiency, congenital HIV, hypogammaglobulinemia (< 4 g/L) in patients after allogeneic hematopoietic stem cell transplantation and immunomodulation: Primary immune thrombocytopenia, Guil-lain Barré syndrome, and Kawasaki disease [2].
IVIG is a derivative of plasma from healthy donors, composed mainly of human immunoglobulin G (IgG), with small amounts of IgA and IgM. Being a group of different donors, it guarantees a diversified collection of antibodies with variable antigen binding regions. All samples are tested mainly for human immunodeficiency virus (HIV), hepatitis B, and hepatitis C [3]. IVIG is currently used to provide immediate passive immunity after suspected exposure to an organism for which there is no active immunization or if there is an inappropriate time to develop active immunization, and as replacement therapy for patients with antibody deficiencies. It has also been used successfully to treat immune thrombocytopenic purpura (ITP), Kawasaki syndrome (mucocutaneous lymph node syndrome), and chronic demyelinating inflammatory polyneuropathies (PDIC). [4] The therapeutic doses used vary from substitute doses (200-400 mg/kg weight) in immunodeficiencies; up to high doses (1-2 g/kg of weight) in autoimmune or inflammatory diseases [5]. The most common adverse reactions to IVIG are thrombocytopenia, hypersensitivity reactions, acute renal failure, increased serum viscosity, and hyponatremia. Discontinuation of IVIG treatment has resulted in remission of aseptic meningitis syndrome (AMS) [6].
Grouped heterogeneous IgG in IVIG provides many antibodies capable of opsonization and neutralization of infectious agents, as well as complement activation. Fc fragment of IgG molecule allows the molecule to interact through the Fc-gamma receptor in B cells and other cells of the phagocytic system. Fc fragment also interacts with plasma Fc-binding proteins. This interaction is essential for the activation of the complement and the elimination of microorganisms. In states of immunomodulatory and anti-inflammatory disease, it is believed that the Fc fragment of IgG and the Fc-gamma receptors on target cells, cells of the phagocytic system, interact to enhance or negatively regulate inflammatory and immune responses. In autoimmune cytopenia and inflammatory neurological disorders, blocking of Fc-gamma receptors in macrophages blocks the elimination of opsonized target cells and suppresses antibody-dependent cellular cytotoxicity, respectively. Immunoglobulins can also modulate the inflammatory response by preventing tissue damage mediated by the complement and regulating the induction of anti-inflammatory cytokines and cytokine antagonists. The immunomodulatory response may be facilitated by the immunoregulatory effects of antidiotypic antibodies on B cells and autoantibodies, regulation of T helper cell production, and apoptosis of gene expression in the immune system [4, 5].
The improvement in the IVIG production parameters, according to the purity criteria required by the WHO, has been one of the factors that contributes to an increase in its clinical use despite the limited number of authorized indications [5]. However, in the country there is limited information about the profile of the IgG use that identifies the conditions under which it is opting for its selection. A search in the different electronic databases Science Direct, Medline, PubMed, Clinical key and up-to-date, only found a practical clinical guide for intravenous use of immunoglobulin (IVIG) published in a Mexican journal by a group of experts from different institutions [1]. A report was found related with the budgetary impact of the IVIG use carried out by several entities of the Colombian government [7] and, finally, other efficacy and safety studies, which supports the limited information on the use profile.
From the last report by Invima (February 2020) about the risk of shortage of immunoglobulin solution for injection, influenced by local over-demand (monthly consumption: 11 000 units. SISMED, 2019) [8], added to the increase in consumption of high-cost drugs in Colombia [9], the high price per unit (about COP $ 700 698), the high value that La Samaritana University Hospital has invested in its acquisition in the last three years (about COP $ 3 522 863 045), and, as there is a limited number of authorized indications for which a clinical use of IVIG is made. It is necessary to study the behavior in the prescription of this medicine so that an overview of its use is obtained.
METHODOLOGY
Descriptive observational cross-sectional study with retrospective collection of information was performed from January 1, 2017, to December 31, 2019. The present study was carried out over a period of three years (time point) in order to obtain an adequate sample size, which was analyzed in a single period of three years. It is not considered a longitudinal design since a temporal sequence was not established.
The study included all the medical records of patients who were prescribed at least one dose of IVIG during the study period and excluded those where it was not possible to obtain the weight of the patient. A demographic characterization of the population -clinical and pharmacological- was performed, and the indications proposed in the medical record were compared with the indications approved by Invima described in table 1. Coding and classification of diagnoses and comorbidities were used in the ICD-10 manual provided by WHO.
For the analysis, the statistical tools of the Microsoft Excel8 electronic sheet were used. Frequencies were estimated from the different quantitative and qualitative variables that were described in tables and percentage terms. The use of patient information was approved for etic committee in research according to the record of the meeting 04-2020.
RESULTS
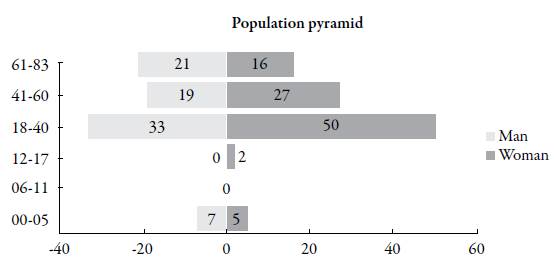
Information was obtained from 182 medical records, two were discarded because of the lack of information on their weight made it impossible to determine the dose (g/kg/day). Due to the wide age range, the population was described according to the classification by stages of development: IVIG was prescribed to people in early childhood (0-5 years), adolescence (12-17 years), early adulthood (18-40 years), middle adulthood (41-60 years) and late adulthood (61 years and older). The proportion of women was higher representing 56% (100/180). The use was predominant in women in early adulthood representing 27.8% (50/180). Other results can be found in figure 1.
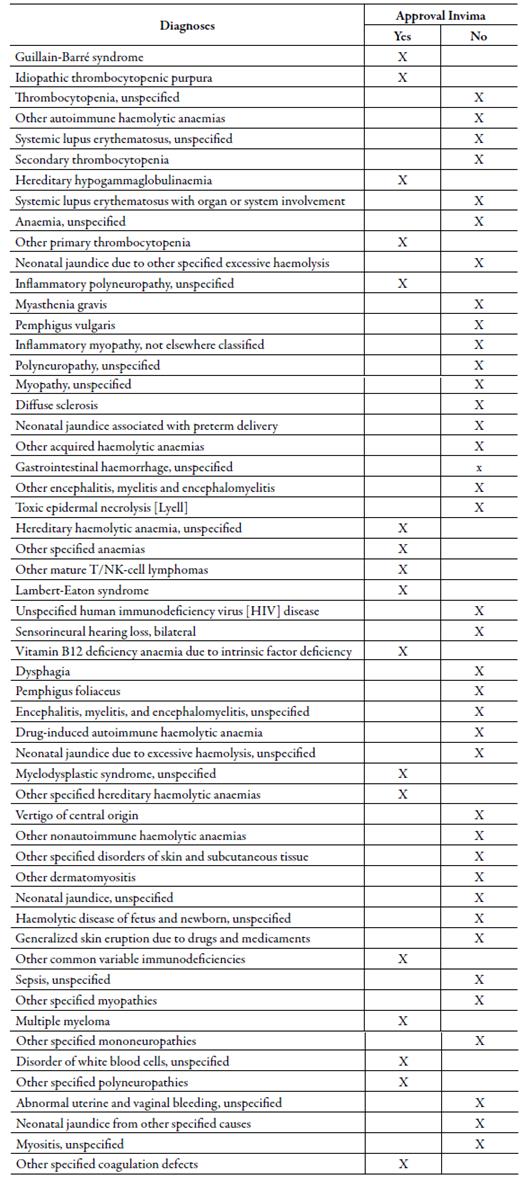
The diagnosis compilation, according to ICD-10, can be seen in table 2, where most of the indications are grouped in diseases of the blood, hematopoietic organs and other disorders that affect the mechanism of immunity and diseases of the nervous system, mainly idiopathic thrombocytopenic purpura (ITP) and Guillain-Barre syndrome (GBS), which could be determined by defining the number of patients by disease and individualized diagnosis.
Table 2 Main diagnosis according to the international statistical classification of diseases and problems related to health (ICD-10) -WHO.

The most frequent indication in 2017 was GBS, followed by ITP, unspecified thrombocytopenia, secondary thrombocytopenia, and systemic lupus erythematosus (SLE). In 2018, GBS also predominated, followed by other autoimmune hemolytic anemias, unspecified thrombocytopenia, inflammatory polyneuropathy, neonatal jaundice due to other excessive hemolysis, and ITP. Finally, in 2019, there was a variation in which ITP was the main diagnosis, continued by GBS, hereditary hypogammaglobulinemia, myopathy, other autoimmune hemolytic anemias and SLE.
The service where most IVIG prescriptions appeared was hospitalization with 54% (98/180), followed by the emergency service with 46% (82/180). Regarding the medical specialty, the internist was identified as the highest IVIG prescriber with 28% (51/180) followed by the hematologist with 27% (50/180), and the one who prescribed the least frequently was the general surgeon with 0.5% (1/180).
Regarding the comorbidities, they were absent in 24% (38/180) of the patients, 35% (56/180) presented a comorbidity, 28% (46/180) presented two comorbidities, and 13% (20/180) presented three comorbidities. The most frequent pathological condition was SLE, followed by unspecified polyneuropathy. As the second comorbidity, the most prevalent was essential (primary) hypertension, followed by unspecified thrombocytopenia. Dysphagia was identified as the third comorbidity, followed by unspecified sepsis.
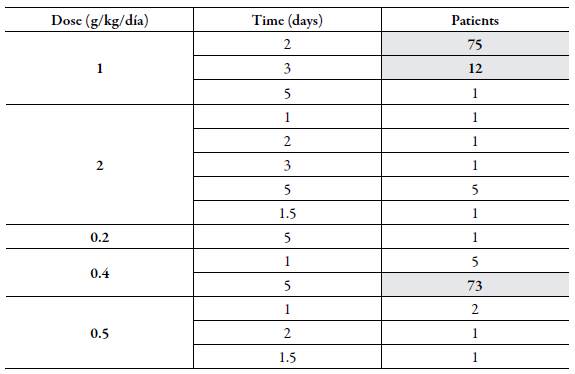
Table 3 shows the different doses prescribed as well as the number of patients who were under this management plan. The most frequently prescribed dose was 1 g/kg/day for 2 days, followed by 0.4 g/kg/day for 5 days and 1 g/kg/day for 3 days.
The most frequent diagnosis for the dose of 1 g/kg/day for 2 days was ITP, followed by unspecified thrombocytopenia and other autoimmune hemolytic anemias. For 0.4 g/kg/day in 5 days it was GBS, followed by SLE and inflammatory polyneuropathy.
Finally, for the dose of 1 g/kg/day in 3 days, the indication of greater prevalence was also ITP, followed by SLE and unspecified thrombocytopenia, however, it should be mentioned that this last dose was the most widely used in the early childhood population, particularly neonates.
Regarding concomitant medication, it was identified that 5% (9/180) of the patients have IVIG as the only treatment, 24% (43/180) have prescribed an additional medication to IVIG, 25% (45/180) have prescribed two concomitant medications and lastly 46% (83/180) consume three additional medications to IVIG. The most frequently medicine used concomitantly are corticosteroids (methylprednisolone, prednisone, and prednisolone) followed by chloroquine, folic acid, and azathioprine.
Regarding the agreement with the Invima indications, table 4 shows that 29% (16/55) of the diagnoses for which IVIG was prescribed is in accordance with the approval of this regulatory entity and 71% (39/55) are off label uses, which in Colombia are known as Uses not indicated in the Sanitary Registry (UNIRS).
DISCUSSION
Regarding the sex and age, more than half of the patients in this study are young women of productive age, which agrees on the epidemiological data of autoimmune diseases such as SLE, polyomyositis [10]. However, in nervous diseases such as chronic inflammatory demyelinating polyneuropathy (CIDP), it is more common in the fifth and sixth decade of life [11]. This, when compared with other results of the study, also reflects a significant percentage of prescribed patients with IVIG between 41 and 60 years. It is worth mentioning that both SAD and CIDP are part of the diagnoses in which IVIG is prescribed in the institution.
Regarding the analysis of the diagnoses that justified the use of immunoglobulin during this period, it can be detailed that the main diagnosis was GBS. However, the frequency of use is grouped in the treatment of patients mainly with diseases of the blood and hematopoietic organs and other disorders that affect the immunity mechanism, particularly the diagnosis of ITP, followed by nervous diseases, led by GBS, already mentioned above, and then by diseases of the musculoskeletal system and connective tissue, in which the main diagnosis was SLE. Finally, certain conditions of the perinatal period, in which there was a higher prevalence of the population in neonatal jaundice due to other specified excessive hemolysis. These diagnoses explain that specialties with the highest incidence of prescriptions were internal medicine, hematology, and neurology.
The main indications for IVIG treatment are some of the primary immunodeficiencies and secondary immunodeficiencies that include a significant antibody deficiency, where they are used as replacement therapy [12]. This also coincides with the frequencies obtained, since these are grouped within the category of diseases of the blood and of hematopoietic organs and other disorders that affect the mechanism of immunity.
These included hereditary hypogammaglobulinemia, hereditary hemolytic anemia, specified coagulation defects, common variable immunodeficiencies, specified hereditary hemolytic anemias, leukocyte disorders, anemia due to vitamin B12 deficiency because of intrinsic factor deficiency, among others. Thus, it was the category that presented the largest population in which use of IVIG.
ITP is an acquired autoimmune disease with a highly variable clinical course, which makes its diagnosis, treatment and follow-up depend on the situation of the patient. In general, the first line treatment is glucocorticoids, however, the use of IVIG is indicated as first line treatment in cases of severe active bleeding, when glucocorticoid treatment is contraindicated, when an immediate rise in platelet count is required, and as an adjunctive treatment if monotherapy fails. This is why it is usually used together with methylprednisolone, the most frequent concomitant medication among the patients evaluated. The dose recommended by the clinical practice guideline is 1 g/kg/day for 2 days, which is consistent with the findings of this study [13].
Regarding GBS, plasmapheresis and administration of IVIG at a dose of 0.4 g/kg/day for 5 days are among the indicated treatments [10], which was the most predominant dose in the study for this diagnosis. In addition to this, a pilot study demonstrated that the combination of intravenous immunoglobulin and methylprednisolone could be beneficial in accelerating recovery from neurological disability in patients with Guillain-Barre syndrome [14]. Again, this glucocorticoid behaves as a concomitant medication within the treatment for these autoimmune disorders, which explains the prevalence of its use within the study population.
Another common diagnosis in the study population was SLE, for which only the management of exacerbations and symptoms -which arise as side effects- ensuring an acceptable quality of life is recommended. There is a variety of treatments, among them is the use of corticosteroids for pain and fatigue, which, within the study, are the drugs of greatest concomitant use with IVIG. Likewise, associations such as dermatitis and arthritis sometimes respond to antimalarials, among them the most widely used are chloroquine sulfate and hydroxychloroquine, which, when observing the results, is part of the concomitant medications of patients. Serious manifestations of SLE should be treated with high doses of corticosteroids such as prednisone, prednisolone (1-2 mg/ kg/day) in divided doses. After the active phase has been controlled for several days in a single morning dose, doses are decreased as rapidly as the clinical situation allows. Cytotoxic agents (azathioprine, chlorambucil, cyclophosphamide, methotrexate) are useful to control active disease and reduce exacerbations and steroid needs, and, on the other hand, azathioprine also have a high prevalence reflected within the results found [14].
IVIG or plasmapheresis may be indicated in cases of lupus nephritis, pancytopenia, and resistant thrombocytopenia, among others. These comorbidities were common findings for these patients, since the use of IVIG in patients with SLE was based on unspecified thrombocytopenia that caused relapses in these patients, this explains that this pathology behaved as the main diagnosis and main comorbidity. The usual immunomodulatory dose of IVIG in SLE is 1 to 2 g/kg/day [15].
In hemolytic incompatibility disease ABO is one of the most frequent causes in indirect hyperbilirubinemia or also known as jaundice due to other specified excessive hemolysis. The treatment of choice is plasmapheresis and exchange transfusion, however the use of high doses of intravenous immunoglobulin has been extended for patients with Rh isoimmunization or ABO, since it has been determined that it reduces the need for exchange transfusion, the duration of phototherapy and the length of hospital stay, it is an alternative of great benefit. The current recommendation on the use of immunoglobulin is to administer 0.5 to 1 g/kg in neonates with hemolytic disease if the level of total serum bilirubin is increasing despite intensive phototherapy or if the level of total serum bilirubin is at 2 mg/dL or 3 mg/dL of the exchange transfusion level. This is determined according to gestational age and postnatal age, and it is accepted to repeat the dose in 12 hours, if necessary, which are two dose regimens that were used in neonates within the institution. The duration or repetition of the established dose depended on the evolution of the patient observing neonatology, which is a procedure to be carried out according to clinical practices [16].
In addition to the immunomodulators previously mentioned within the management plan for the different diagnoses, it is also important to recognize the frequency of the use of folic acid within this population, this can be associated with the prevention of folate deficiency secondary to chronic hemolysis [17], such as those who manifested autoimmune hemolytic anemia or relapse of SLE. It should be clarified that IVIG is not a first-line treatment since there are other alternatives such as corticosteroids and plasmapheresis, therefore, regarding pharmacological management, it is observed that the percentage of patients under treatment with IVIG alone is very low.
Regarding comorbidities, the number of patients without pathologies is important according to the sample. Among the patients with comorbidities, it was possible to identify that the manifestations found are due to complications of the main diagnosis, for example pancytopenia, thrombocytopenia and hemolytic anemia are a frequent and potentially serious complication in systemic autoimmune diseases [18] or inflammatory polyneuropathy and dysphagia, complications of GBS. High blood pressure as comorbidity is probably not associated with the main diagnosis, but rather with its prevalence in the world population since it was not described in the medical record as secondary high blood pressure.
Regarding the approval of Invima indications, of the diagnoses for which the use of IVIG was justified, it was difficult to determine because the uses authorized by this entity are not specific. Although it delimits the authorized diagnoses as first choice treatment, it is not clear in the main alterations to be used as a second-choice treatment or as an aid in the management plan, which causes a degree of freedom and individualization of the use of this medicine by the prescribing service or prescribing specialty, based on international clinical practice guidelines. Therefore, the UNIRS percentage of IVIG in the HUS was 71%, which is a significant value in which the country is at risk of shortages of IVIG and, without a study that allows visualizing the general panorama of Colombia, the uneasiness about a common denominator in the different institutions that offer this treatment within the patient management plan appears. This in turn, in the short or medium term can generate a public health problem in the country, because the supply of this medicine is not achieved for those patients who require this first choice treatment, as a vital necessity.
The most predominant population prescribed IVIG was young adult women in indications related to diseases of the blood and hematopoietic organs and other disorders that affect the mechanism of immunity, nervous diseases, diseases of the musculoskeletal system, connective tissue, and certain conditions of the perinatal period.
Patients with autoimmune diseases within the study were characterized by having only the diagnosis that justified the use of IVIG or, more frequently, they had comorbidities such as SLE, polyneuropathy and unspecified thrombocytopenia, complications of the main diagnosis.
The diagnoses for which there is an Invima approval are not specific, which implies that there is not a defined therapeutic strategy with IVIG and therefore that prescribers for similarity or biological plausibility are using it.
From this study, indications were identified where IVIG seems to play an important role at a clinical level, such as chronic inflammatory demyelinating polyneuropathy, autoimmune hemolytic anemia, polymyositis, systemic lupus erythematosus, and other disorders. However, despite being found as UNIRS uses, it is necessary to carry out an a posteriori literary review to evaluate the efficacy and safety of IVIG for each of these diagnoses.