INTRODUCTION
Primary postpartum haemorrhage (PPH) is traditionally defined as an estimated blood loss greater than 500 cc in the first 24 hours in cases of vaginal delivery, and of more than 1000 cc following cesar-ean section 1. It occurs in 2-4% of all vaginal deliveries and 6-7% of cesarean deliveries. It is severe in 1% of cases, with a blood loss greater than 1,000 cc 2. It is the most frequent cause of maternal mortality (19%) and morbidity in the world, accounting for 8% and 19.7% of maternal deaths in developed and developing countries, respectively 3. In Colombia, PPH accounts for 23% of all maternal deaths 4. Prevention and treatment of primary postpartum haemorrhage are critical in diminishing maternal mortality 5. Causes of obstetric bleeding after childbirth have been divided into four main groups as follows: tone, trauma, tissue, and thrombin, the most frequent being uterine atony at 70% 6-9.
Severe obstetric bleeding after childbirth is a life-threatening emergency, classified as a near-miss (extreme maternal morbidity) and it is ocurrence is mandatory to be reported to the epidemiological surveillance system 10. Given that the diagnosis of severe PPH based on the visual estimation of blood loss is not reliable and tends to underestimate the magnitude of the bleeding, several methods have been proposed based on more accurate clinical findings for estimating blood loss 11. All these methods are aimed at triggering a series of sequential, coordinated and timely actions by an interdisciplinary team in order to achieve the core objective of diminishing maternal morbidity and mortality from this cause. In Colombia, these actions are known as the "obstetric red code" 11. In this approach, the initial step to trigger actions is to make the diagnosis of the presence of cardiovascular shock. This management algorithm incorporates the recommendations from the World Health Organisation (WHO) guidelines 5 and of the Royal College of Gynaecology and Obstetrics 12. Effective implementation of these actions requires the activation of the rapid response team and priority allocation of hospital resources until the condition is resolved.
Delay in the identification of severe PPH is the main cause of maternal morbidity and mortality secondary to haemorrhage 11,13,14. The "obstetric red code" approach to diagnosis and treatment, though effective for bleeding control and improvement of patient survival once it is activated, is not very sensitive when it comes to identifying and reporting all cases of primary obstetric haemorrhage, considering that the presence of PPH could be judged as "not sufficiently" severe to warrant reporting. This means that although management by the treating staff is triggered, there is no formal activation of the obstetric red code in the institution. This "not sufficiently severe" PPH may be associated with significant maternal morbidity and risk of dying, and also with under-recording and under-reporting of haemorrhage cases to the epidemiological surveillance systems in Colombia.
The objective of this study is to explore the incidence of primary obstetric haemorrhage from the perspective of a more reproducible definition based on the use of one or more uterotonic medications in additional doses than those used routinely for active childbirth management, regardless of the activation of the obstetric red code; and to describe the interventions implemented for bleeding control, as well as the maternal outcomes with treatment initiated within the first 24 hours and maintained during 7 days in the postpartum period, and to evaluate the magnitude of under-recording.
MATERIALS AND METHODS
Case series of women with primary obstetric haemorrhage as part of a cohort of pregnant women who presented for vaginal or cesarean delivery between February 1 and October 31, 2016, at a public intermediate complexity hospital located in Bogotá that serves patients covered by the Colombian Social Security System (SSSC) and is a training centre for undergraduate and graduate medical students. Women with antepartum diagnosis of uterine rupture, placenta accreta, placenta praevia, coagulation disorders or disseminated intravascular coagulation were excluded, considering their indication for definite treatments other than the administration of uterotonics in the presence of PPH.
Cases of obstetric haemorrhage were defined as women requiring the use of additional medications (oxytocin, methylergonovine or misoprostol) apart from the dose of 10 units of oxytocin for the active management of childbirth during vaginal or cesarean delivery, as judged by the physician in charge of the obstetric service in accordance with institutional protocols and guidelines.
Sampling was consecutive. Based on the incidence of postpartum haemorrhage reported in the literature of 2-4% in vaginal delivery and 6-7% in cesarean delivery 13,15 and the reported frequency of 2,200 births per year at the institution, a sample size of 90 cases of obstetric haemorrhage was estimated, with a distribution of 50 cases after vaginal delivery and 40 cases after cesarean section during the study period, according to the historical proportion of cesarean sections performed at the institution 16.
Procedure. Patients were identified by means of an active search in the institutional pharmacy of any released doses of the available uterotonics (oxytocin, methylergonovine or misoprostol) additional to the 10 units of oxytocin used for active childbirth management, and in the records of mandatory reporting of obstetric red code team activations. Clinical records were reviewed up to patient discharge and the 7-day follow-up visit. Data were collected using specific forms and were kept in a secure area under lock and key, with access restricted to the study personnel. They were then entered into an Excel database and analysed using EPIINFO 7.0, after quality verification.
The variables measured included maternal age, medical history, pregnancy-associated diseases, parity, a history of postpartum bleeding, weeks of gestational age at the time of delivery, presence of prenatal visits, haemoglobin concentration (g/dL) at the time of the last prenatal visit, uterine height, labour induction, delivery route, episiotomy, perineal tears, and neonatal weight and length. Outcome variables were the presence of obstetric bleeding defined by the use of medications (oxytocin, methylergonovine or misoprostol) additional to the dose of 10 units of oxytocin used for active management of childbirth during vaginal or cesarean delivery and during the next 24 hours after childbirth; cause of bleeding (hypotony, trauma, presence of tissue or postpartum coagulation abnormality; degree of shock estimated in accordance with the criteria defined in the "red code" protocol 11; estimated postpartum bleeding; and activation of the obstetric red code team. Interventions defined for obstetric bleeding control were: medical management (use of the uterotonics described), advanced medical management (uterotonics plus uterine tamponade), and surgical management (laparotomy for haemostatic uterine sutures or hysterectomy). Maternal outcomes included in the assessment were mortality, hysterectomy, admission to the intensive care unit, and need for blood transfusion.
Statistical analysis. Quantitative variables are expressed in the form of central trends, means or medians, and scatter measures according to the results of normalcy tests, and qualitative variables are expressed in absolute numbers and proportions.
Ethical considerations. This research project was submitted to the Ethics Committee of Universidad Nacional de Colombia Medical School for evaluation and was approved as set forth in Minutes 143 of September 10, 2015, and by the Ethics Committee of Hospital de Engativa ESE, on December 18, 2015.
RESULTS
During the study period there were in total 1,633 births: 1,080 vaginal deliveries and 553 cesarean sections, for a proportion of 33.8% cesarean deliveries. A total of 35 cases of obstetric haemorrhage were identified as defined by the additional use of uterotonics, for an overall incidence of 2.1% during the study period. By delivery route, the incidence of postpartum obstetric haemorrhage was 2.4% (26 cases) following vaginal delivery, and 1.6% (9 cases) following cesarean section. According to reporting based on obstetric red code activation, the incidence of postpartum obstetric haemorrhage was 0.83% (9/1080) after vaginal delivery and 0.36% (2/553) after cesarean section. There were no maternal deaths. Table 1 shows the demographic characteristics of the cases and the causes of PPH. In 24 out of 35 patients (68.6%), uteronic medications were administered on top of active childbirth management, and there was no activation of the institutional response protocol or the obstetric red code.
Six patients had a medical history and, of them, three were obese, one presented with repeated urinary tract infections, one was drug-dependent and another one had hypertriglyceridemia. There were no patients with anaemia before childbirth. Pregnancy-related diseases found in 11 patients included preeclampsia, hyperthyroidism, gestational diabetes and gestational hypertension. Table 1 shows the causes of postpartum hemorrhage. There were three cases of retained placenta as the cause of obstetric haemorrhage following vaginal delivery (11.5%), and no case of tissue retention following cesarean delivery. There were three trauma cases, one of them following cesarean section as a result of a cervical tear after a failed instrumentation attempt. There were no cases attributable to coagulation disorders.
Table 1 Demographic characteristics of obstetric postpartum haemorrhage cases at Hospital de Engativá, Bogotá, Colombia, 2016
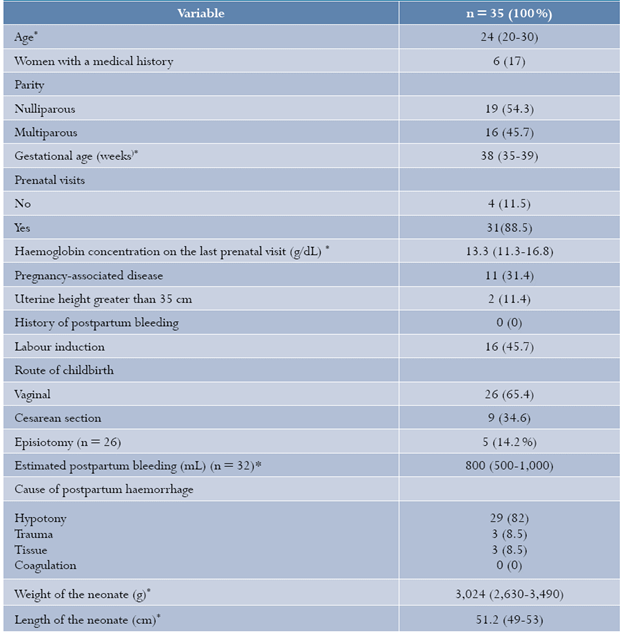
* Median (inter-quartile range).
In 29 of 35 patients with PPH, bleeding was controlled with medical management (Figure 1) based on the use of oxytocin at a dose of 20-60 IU (median 40 IU). In 19 of these 29 women (65.5%), methylergonovine had to be added at a median dose of 0.2 mg, and 12 women (41.3%) also required rectal administration of a median dose of 1,000 mg of misoprostol. In 11 cases in which obstetric red code activation was required, medications were administered concurrently.

PPH: Obstetric haemorrhage. ICU: Intensive Care Unit. PRBCs: Packed Red Blood Cells
Figure 1 Flow-chart of patients and maternal outcomes according to the route of delivery and activation of the obstetric red code in women with postpartum haemorrhage at Hospital de Engativá, Bogotá, Colombia, 2016
Of the remaining 6 patients with obstetric haemorrhage who required additional interventions, 4 patients after vaginal delivery responded to hydrostatic tamponade, and 2 who presented bleeding following cesarean section required surgical management: one haemostatic suture (B-Lynch) and one subtotal hysterectomy.
Haemoglobin levels were under 11 in 14 (63%) out of 22 patients in whom they were measured 6 hours after the bleeding episode. Of the women in whom the rapid response protocol was not activated, 63% developed postpartum anaemia; 50% required blood product transfusions, and 16% had to be admitted to the ICU. Advanced medical management of obstetric haemorrhage with hydrostatic tamponade 1,5,11 was used with 100% effectiveness in 4 women following vaginal delivery.
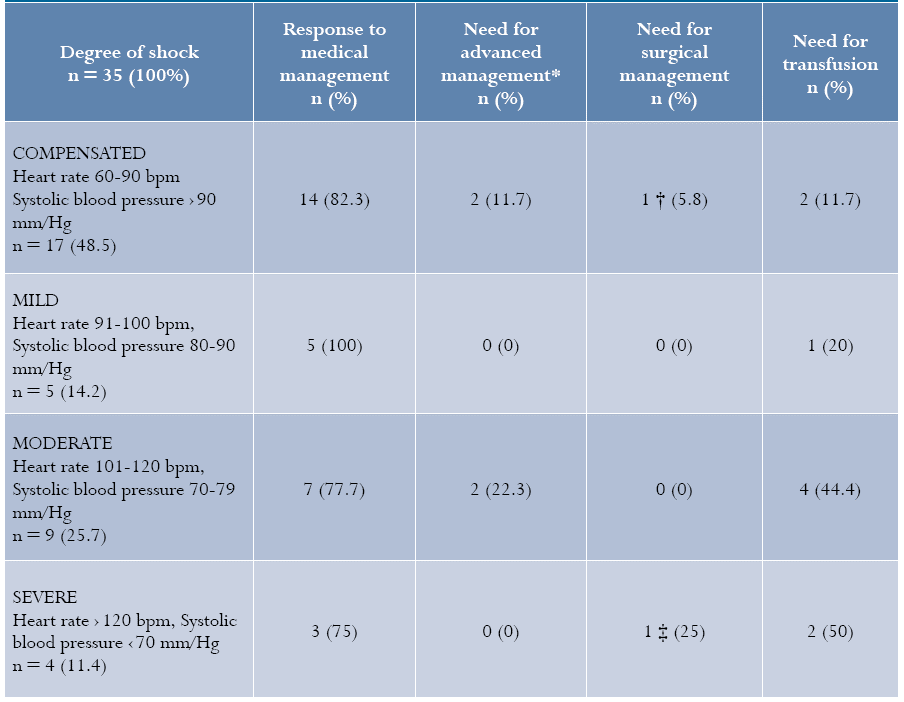
Responses to the treatments instituted according to the degree of shock at the time of case identification are shown in Table 2. The stratified analysis shows that a smaller proportion of women with the highest degree of shock responded to medical management and had a higher frequency of transfusions.
DISCUSSION
The incidence of obstetric haemorrhage in this study was 2.1% lower than the one reported in the world literature (4-6%), as well as the one reported previously for the same institution 1,3,8,13. The incidence determined on the basis of the use of additional medications other than the ones used for active management of childbirth, after excluding cases in which preventive use of postpar-tum uterotonics was documented, was 3.5 higher than the reported incidence, according to the case definition used by the Colombian Epidemiological Surveillance System (SIVIGILA). In women who required the additional use of uterotonics, there was maternal morbidity and transfusion requirement in 50% of the cases, and invasive management in 16%. This observation points to the benefit of using more repeatable methods for diagnosing PPH, such as the use of uterotonic medications, and of assessing different cut-off points based on progressive needs.
Cesarean section has been reported as a risk factor, and a higher incidence of PPH is described in association with cesarean delivery 12. However, in this study, the incidence of post-cesarean PPH was lower compared to the incidence following vaginal delivery (1.6% vs. 2.4%). These differences may be attributed to the exclusion of cases with PPH causes identified antepartum, including placenta praevia and placenta accreta, and to the inclusion of a population with low-risk characteristics for PPH.
The low frequency of red code activation reflects the challenge for the staff responsible for childbirth when faced with the need of making a clinical diagnosis of severe obstetric haemorrhage 13,14. A review of the literature including 36 studies assessed visual estimation of blood loss 14 and observed that clinical estimation was inaccurate when compared to the use of collection bags. However, the use of collection bags did not prevent delays in decision-making or obstetric bleeding progression. The advantages of false positive results with the use of this method for estimating blood loss would be early management in patients with no severe but abnormal bleeding 13, and avoiding the need for institutional protocol activation, notification and overuse of resources in response to this obstetric emergency, based on the clinical judgement of the treating staff. In contrast, a false negative result leads to late initiation of management because of the underestimation of the blood loss, resulting in serious consequences and increased maternal morbidity.
Our observations regarding the cause of PPH are consistent with a study conducted in low income countries, in which 82% of the cases of obstetric haemorrhage reported were attributable to uterine atony 15.
A treatment protocol for obstetric haemorrhage has been consolidated as a sequence of interventions of increasing complexity and degree of invasion 5,11,12. Reported success rates of initial medical management with uterotonics and massage is 60-70% 6. In this study, medical management following obstetric red code activation was successful in 6/11 cases (54.5%), and in 29/35 (82%) in those cases in which the obstetric red code was not activated. This difference could be due to differences in bleeding volume and severity that lead treating staff to the selective activation of the institutional protocol: in women with larger estimated bleeding, predefined coordinated actions are implemented together with initiation, although late, of advanced medical or surgical management, while in women with abnormal bleeding requiring the use of additional uterotonics besides the ones used in active childbirth management, and no red code activation, the response to medical treatment is close to 80%. Along the same lines, the stratified analysis of the women's response to the treatment based on the degree of shock showed that, the higher the degree of shock, the lower the proportion of cases that responded to medical treatment, and the higher the frequency of transfusions.
The need for transfusion and ICU admission of patients with PPH in whom the obstetric red code was not activated points to the importance of assessing the impact of prompt identification and activation of the rapid response protocol triggered by the use of a specific uterotonic drug, or by the use of one or more of those medications, because the little validity of clinical estimation of bleeding and the time that it takes to recognise the signs of shock, even in cases of haemorrhage considered as non-severe 13 have repercussions in terms of response to treatment and maternal outcomes.
The effectiveness of hydrostatic tamponade found in our case series is consistent with the reports of several observational studies showing that hydrostatic tamponade resolves 74% to 90% of all obstetric haemorrhages that do not respond to medical management during vaginal delivery 17-20, and it is recommended as the first line of advanced management when the cause of bleeding is atony 12. In women with obstetric haemorrhage following cesarean section, the second line treatment was surgical in accordance with the WHO recommendations 5 and because of the availability of the surgical resource at the institution. This finding is also related to the institutional protocol 11 which recommends that women in severe shock according to the guidelines must be taken to surgery as soon as possible and given blood products for prompt resuscitation.
The strength of this study is the active identification of the cases through the use of reliable sources such as release of medications from the pharmacy in order to control for measurement, reporting and poor classification biases. This allowed the identification of women with obstetric bleeding who would not have been detected using the activation of the rapid response team or the need for blood product transfusions as criteria. The observational nature of the study, the fact that it is based on records, and the low observed incidence of the event, are limitations of this work.
CONCLUSIONS
The findings of this study point to the need of assessing the effectiveness and safety of more reproducible diagnostic methods in order to determine the right timing for initiating treatment per protocol in women with severe postpartum haemorrhage, regardless of the route of delivery, and to encourage activation of the rapid response team, given the evidence of morbidity and adverse maternal outcomes in those women in whom the obstetric red code was not activated.











 text in
text in