Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Revista de la Facultad de Medicina
Print version ISSN 0120-0011
rev.fac.med. vol.62 no.4 Bogotá Oct./Dec. 2014
https://doi.org/10.15446/revfacmed.v62n4.43754
DOI: http://dx.doi.org/10.15446/revfacmed.v62n4.43754
ORIGINAL RESEARCH
Evaluation of the diagnostic performance of platelet-derived indices for the differential diagnosis of thrombocytopenia in pediatrics
Evaluación del rendimiento diagnóstico de los índices plaquetarios en el diagnóstico diferencial de las trombocitopenias en pediatría
Nelson Hernando Aponte-Barrios1,2, Adriana Linares-Ballesteros1,2, Isabel Cristina Sarmiento-Urbina2, Gloria Inés Uribe-Botero2
1 Facultad de Medicina, Universidad Nacional de Colombia. Bogotá, Colombia.
2 Fundación Hospital de la Misericordia. Bogotá, Colombia.
Correspondence: Nelson Hernando Aponte-Barrios. Calle 8 bis D No. 81 B-65. Bogotá, Colombia. Telephone: +57 311 2833494. E-mail: drnelsonaponte@hotmail.com.
Received: 28/05/2014 Accepted: 30/07/2014
Summary
Background. Platelet-derived indices have a well-established correlation with the differential diagnosis of thrombocytopenia in adult-based research. These indices include mean platelet volume, platelet distribution width, and platelet-large cell ratio.
Objective. To determine the values of platelet-derived indices in a pediatric population with diagnoses of thrombocytopenia and their etiologic correlation.
Materials and methods. Analytic observational diagnostic-test study. The population for this analytical study was pediatric patients between 6 months and 18 years of age who had thrombocytopenia (<100x109/L). The study period was 18 months long.
Results. Of 54 subjects, 18 (33.3%) were diagnosed with idiopathic thrombocytopenic purpura, and 36 (66.7%) were diagnosed with acute leukemia. Mean age was 7.4 years and 6.8 years for immune thrombocytopenic purpura and acute leukemia, respectively. Mean platelet distribution width values for immune thrombocytopenic purpura and acute leukemia were 15.08 fL and 10.73, respectively. Mean MPV for immune thrombocytopenic purpura and acute leukemia was 11.7 fL and 9.8 fL, respectively. Mean platelet-large cell ratio was 38.26% and 24.97% for idiopathic thrombocytopenic purpura and acute leukemia, respectively. Differences in these three distinct platelet indices between idiopathic thrombocytopenic purpura and acute leukemia were statistically significant (p=0.00). The area under the ROC curve for platelet-derived indices showed that they were adequate for defining the causes of thrombocytopenia. MPV and platelet-large cell ratio had an area under the curve of 0.89 and 0.88, respectively, while platelet size deviation width had an area under the curve of 0.903.
Conclusions. Platelet-derived indices could be useful in the initial approach for the differential diagnosis of pediatric patients with thrombocytopenia.
Keywords: Thrombocytopenia; Purpura, Thrombocytopenic, Idiopathic; Mean Platelet Volume (MeSH).
Aponte-Barrios NH, Linares-Ballesteros A, Sarmiento-Urbina IC, Uribe-Botero GI. Evaluation of the diagnostic performance of platelet-derived indices for the differential diagnosis of thrombocytopenia in pediatrics. Rev Fac Med. 2014;62(4):547-52. http://dx.doi.org/10.15446/revfacmed.v62n4.43754.
Resumen
Antecedentes. Los índices plaquetarios tienen buena correlación con la etiología de la trombocitopenia en estudios realizados en adultos. Estos son: volumen plaquetario medio, ancho de distribución plaquetaria y porcentaje de plaquetas grandes.
Objetivo. Determinar las características de los índices plaquetarios en población pediátrica con trombocitopenia y su posible correlación etiológica.
Materiales y métodos. Estudio de prueba diagnóstica observacional analítico. Realizado con pacientes entre 6 meses y 18 años ingresados en un período de 18 meses con trombocitopenia <100x109/L.
Resultados. 54 pacientes: 18 (33,3%) con púrpura trombocitopénica inmune y 36 (66,7%) con leucemia aguda. Edad media para púrpura trombocitopénica inmune 7,4 años y 6,8 para leucemia aguda. Valores de ancho de distribución plaquetaria con media de 15,08 fL en púrpura trombocitopénica inmune y 10,73 para leucemia aguda. Media del volumen plaquetario medio para púrpura trombocitopénica inmune 11,7 fL y de 9,8 fL para leucemia aguda. Porcentaje de plaquetas grandes la media para púrpura trombocitopénica inmune 38,26% y 24,97% para leucemia aguda. Las diferencias de los tres índices para cada una de las enfermedades fueron estadísticamente significativas (p=0,00). Las curvas de Característica Operativa del Receptor de los índices plaquetarios fueron parámetros suficientes para distinguir las causas de trombocitopenia: volumen plaquetario medio y porcentaje de plaquetas grandes con un área bajo la curva de 0,89 y 0,88 y ancho de distribución plaquetaria 0,903.
Conclusiones. Los índices plaquetarios fueron útiles para el acercamiento inicial al diagnóstico diferencial de trombocitopenias en niños.
Palabras clave: Trombocitopenia; Púrpura Trombocitopénica Idiopática; Volumen Plaquetario Medio (DeCS).
Aponte-Barrios NH, Linares-Ballesteros A, Sarmiento-Urbina IC, Uribe-Botero GI. Evaluación del rendimiento diagnóstico de los índices plaquetarios en el diagnóstico diferencial de las trombocitopenias en pediatría. Rev Fac Med. 2014;62(4):547-52. http://dx.doi.org/10.15446/revfacmed.v62n4.43754.
Introduction
Among the studies that evaluate the usefulness of platelet-derived indices for the differential diagnosis of the causes of thrombocytopenia, some can be found that show how mean platelet volume (MPV), platelet distribution width (PDW), and platelet-large cell ratio (P-LCR) have a good diagnostic correlation when compared to findings from the study of bone marrow. Among the studies carried out to determine differential diagnoses, it is worth mentioning thrombocytopenia secondary to disease of the bone marrow or to diseases that reduce platelet life-span (1,2), immune thrombocytopenic purpura and aplastic anemia (3-5), or thrombocytopenia due to megaloblastic anemia and other causes (6). These studies have been performed on the adult population, but never on the pediatric population.
Diagnostic methods for the study of blood cells and their assessment has advanced greatly: the techniques for their analysis have been simplified, and new methods have been developed that allow us to evaluate the different parameters that, today, are highly useful for the diagnosis of diverse pathologies (7). At present, we have hematology analyzers at our disposition that provide quick and very precise results that, in addition, have the capacity to measure blood cell parameters automatically. Among these parameters are the platelet-derived indices that generally are not used in the clinical context mainly because of an ignorance of their possible usefulness and, occasionally, because of difficulties encountered between laboratories related to the standardization of values.
It is important to be aware of the reference interval that could be useful for the diagnosis of certain pathologies (3, 6-10, 12). The cut-off points used to define the indices in the studies of adult populations that were reviewed are: MPV of 8.4-12 femtoliters, 8-14 femtoliters for the platelet distribution width, and greater than 12 fL for the platelet-large cell ratio (3,6,9).
The platelet-derived indices available in automated equipment are: mean platelet volume, platelet distribution width, and the platelet-large cell ratio. The mean platelet volume is a parameter that measures the average platelet size just as mean corpuscular volume does for red blood cells (3,6,10). The platelet distribution width expresses the variation in the size of the platelets and has shown usefulness in the differential diagnosis between reactive thrombocytosis and thrombocytosis associated with myeloproliferative disease. Furthermore, it works to differentially diagnose thrombocytopenia due to platelet destruction or decreased production (3-6,8). The percentage of large platelets refers to the proportion of platelet that have a size or more than 20 femtoliters, and for this reason it is another parameter that is provided automatically by current analyzers (3,5).
Platelets are essential for maintaining the integrity of the endothelium and for controlling hemorrhages when injury to the blood vessels occurs. They form a plug by aggregating and adhering to each other —primary hemostasis—. When the injuries to the vessels are very extensive, further participation from coagulation factors to produce a fibrin plug that is firmer and more stable —secondary hemostasis—. Thrombocytopenia is defined as a platelet count under 100x109/L (11–13). It is the most common cause of defects in primary hemostasis, and it can present along with bleeding in children.
Thrombocytopenia should be suspected in children with bleeding in mucous membranes or petechiae in the skin, but frequently its discovery is incidental in a complete blood count (CBC) ordered for other reasons (10–12,14). Thrombocytopenia can be caused by the reduction of the production of platelets, or by their destruction or removal from circulation. The management of thrombocytopenia is guided by an adequate knowledge of the cause and clinical course of the pathology. The main purpose of the treatment is not to reach a normal number of platelets, rather to raise them to safe levels for the patient, while preventing the appearance of bleeding that can jeopardize their life (3,6,14,15).
The main objectives of this study are to evaluate the utility of the platelet-related indices for the differential diagnosis of thrombocytopenia en clinical practice and to determine the operational characteristics of the platelet-derived indices in the pediatric population.
Materials and methods
An analytic observational diagnostic-test study was performed. The study included all patients accessing the emergency services of the Misericordia Hospital between January 1, 2012 and July 30, 2013 presenting a first episode of thrombocytopenia —platelet counts under 100x109/L–, aged between 6 months and 18 years old, and in whom a bone marrow study was carried out. The correlation between the etiological diagnosis of the thrombocytopenia and the values of the levels of the platelet-derived indices was assessed for each pathology.
Inclusion criteria. All patients on whom a bone marrow aspiration was carried out as part of the study of a presentation of thrombocytopenia, considered to be a platelet count under 100x109/L, and who had associated platelet-derived indices from a CBC performed in the institution.
Exclusion criteria. Patients that received medications that altered the production or function of platelets, like aspirin, chemotherapy, quinine, corticosteroids, etc. were excluded. Also, patients for whom the CBC reading equipment does not provide the results of the platelet-derived indices were excluded.
Results
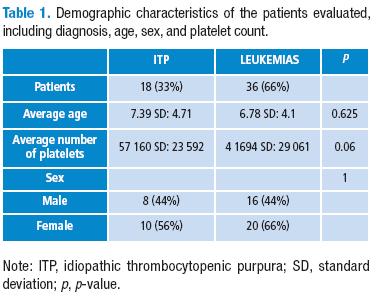
54 patients were analyzed, 18 (33.3%) with a diagnosis of idiopathic thrombocytopenic purpura (ITP), and 36 (66.7%) with a diagnosis of acute leukemia (AL). There was a proportion of 1.2 females for every male, for both ITP and LA. Age medians and average platelet counts for each of the pathologies. Neither showed statistically significant differences, which allows the two groups to be defined as homogenous (Table 1).
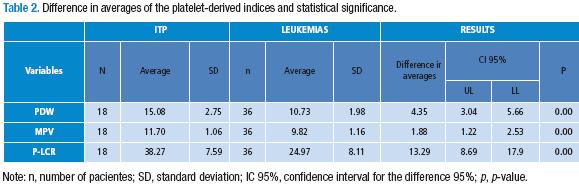
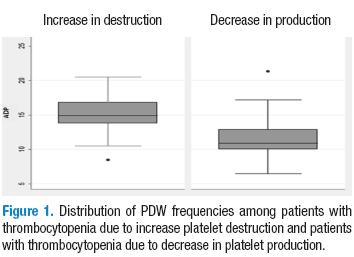
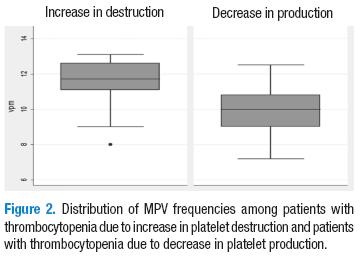
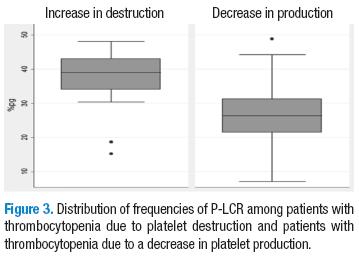
Table 2 shows in detail the average values for each of the platelet-derived indices for each of the conditions. Statistically significant differences in the averages of the three parameters were found (p=0.00). The values were higher for patients with ITP. This is shown in Table 2 and in Figures 1-3.
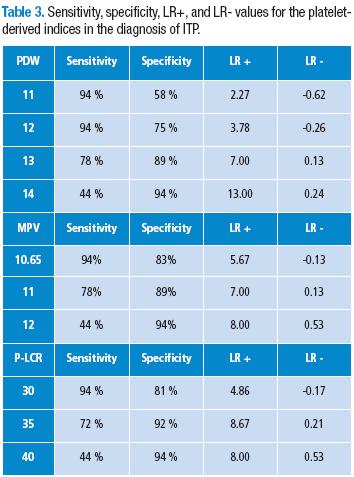
Each of the platelet-derived indices was analyzed with different cut-off points and of the obtained results, upon doing specificity, sensitivity and LR analyses, the values that showed the best diagnostic performance for ITP are presented in Table 3.
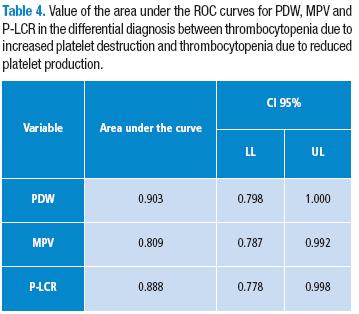
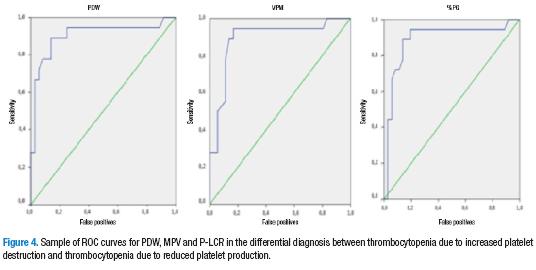
The values for the area under the ROC curve for each of the indices is within the confidence intervals. This indicates that they are parameters that are sufficient for distinguishing the two types of thrombocytopenia (low production and increased destruction), as expressed in a detailed manner in Table 4 and Figure 4.
Discussion
Thrombocytopenia is a common manifestation of several diseases. It is frequently found in patients that access emergency care, and for that reason it is important to have a diagnostic tool that helps distinguish between its two main causes: the reduction of platelet production and the destruction of platelets. The availability of an automated hemogram, a test that is quick and easily available in a clinic, makes this test a very useful element.
In the search for a new diagnostic approach, we find the platelet indices —mean platelet volume, platelet distribution width, and platelet-large cell ratio— that can be easily measured in new automatic analyzers. These indices have demonstrated good sensitivity and specificity in the differential diagnosis in studies of thrombocytopenia in the adult population. However, they have not yet been evaluated for the pediatric population. In some cases of severe thrombocytopenia, the automated machine may not be able to provide these indices —in this study it occurred in less than 5% of the analyses—, which, in some cases, may limit its use.
In this study, we found that the platelet-derived indices of mean platelet volume, platelet distribution width, and platelet-large cell ratio show significantly high values for cases of ITP compared to for patients with AL. The sensitivity, specificity, the positive p-value, and the negative p-value of the platelet-derived indices were appropriate for differentiating between thrombocytopenias due to platelet destruction (ITP) and thrombocytopenias due to low platelet production (AL), as was observed in studies on adults carried out in Tokyo by Kaito et al. (3) and by Bowles et al. (1), where patients diagnosed with ITP and aplastic anemia were compared.
The study by Numbenjapon et al. evaluated MPV, finding sensitivity of 82.3% and sensitivity of 93% with LR values of 11 for the diagnosis of ITP (2). Other studies found diagnostic performances close to 100%, with a lower performance for the platelet-large cell ratio compared to platelet distribution width and mean platelet volume, in patients with aplastic anemia and ITP. However, all of these studies were performed on the adult population (4,5).
The ROC curves are useful for comparing the superiority of different laboratory curves that measure the area beneath a curve. The larger it is, the more certain it is considered. Furthermore, it is considered to have fewer diagnosis errors than a test with a smaller area under the curve. A poor test is given marks of 0.5 to 0.6; a normal test is given marks of 0.6 to 0.75; a good test is given marks of 0.75 to 0.9; a very good test is given marks of 0.9 to 0.97; and an excellent test is given marks of 0.97 to 1. The results of this test show that the platelet-derived indices have good ROC curves for mean platelet volume and platelet-large cell ratio, with an area under the curve of 0.89 and 0.88, respectively. For platelet distribution width, the area was 0.903, which indicates a very good test.
When it comes to studies in adults, Kaito’s study showed ROC curves with an area under the curve for mean platelet volume of 0.910, of 0.930 for platelet-large cell ratio, and, for platelet distribution width, of 0.934. Another study found a value of 0.885 for mean platelet volume, a value similar to the one obtained in this study of a pediatric population (2,3).
The new analyzer have new platelet-derived parameters including the immature platelet indices or the immature platelet fraction. In Colombia, these analyzers are not widely available. However, they are parameters that should be taken into account in the future as possible elements that may contribute to the differential diagnosis of thrombocytopenias in children (16).
Conclusions
In the majority of patients, platelet-derived indices could be helpful for distinguishing between thrombocytopenia due to an increase in the destruction of platelet and thrombocytopenia due to a reduction in platelet production. This data may be available in the majority of institutions and may be very helpful in the initial approach for diagnosis and an initial therapeutic focus. This study works to promote the use of the automated hemogram report in a more appropriate way and to motivate awareness of the platelet-derived indices as a source of information for finding the etiology of thrombocytopenia in children.
Conflict of interest
None declared by the authors. Approved by the ethics committee of the Misericordia Hospital.
Financing
Project financed by Misericordia Hospital and the Universidad Nacional de Colombia.
Acknowledgments
None declared by the authors.
References
1. Bowles KM, Cooke LJ, Richards EM, Baglin TP. Platelet size has diagnostic predictive value in patients with thrombocytopenia. Clin Lab Haematol. 2005;27:370-3. http://doi.org/fq6834. [ Links ]
2. Numbenjapon T, Mahapo N, Pornvipavee R, Sriswasdi C, Mongkonsritragoon W, Leelasiri A, et al. A prospective evaluation of normal mean platelet volume in discriminating hyperdestructive thrombocytopenia from hypoproductive thrombocytopenia. Int J Lab Hematol. 2008;30:408-14. http://doi.org/dxrmbh. [ Links ]
3. Kaito K, Otsubo H, Usui N, Yoshida M, Tanno J, Kurihara E, et al. Platelet size deviation width, platelet large cell ratio, and mean platelet volume have sufficient sensitivity and specificity in the diagnosis of immune thrombocytopenia. Br J Haematol. 2005;128:698-702. http://doi.org/brvcgh. [ Links ]
4. Lee WS, Kim TY. Mean platelet volume and platelet distribution width are useful in the differential diagnosis of aplastic anemia and idiopathic thrombocytopenic purpura. Clin Chem Lab Med. 2010;48:1675-6. http://doi.org/fnz3gm. [ Links ]
5. Ntaios G, Papadopoulos A, Chatzinikolaou A, Saouli Z, Karalazou P, Kaiafa G, et al. Increased values of mean platelet volume and platelet size deviation width may provide a safe positive diagnosis of idiopathic thrombocytopenic purpura. Acta Haematol. 2008;119:173-7. http://doi.org/cqvmp8. [ Links ]
6. Borkataky S, Jain R, Gupta R, Singh S, Krishan G, Gupta K, et al. Role of platelet volume indices in the differential diagnosis of thrombocytopenia: a simple and inexpensive method. Hematology. 2009;14:182-6. http://doi.org/ddhdrq. [ Links ]
7. Briggs C, Harrison P, Machin SJ. Continuing developments with the automated platelet count. Int J Lab Hematol. 2007;29:77-91. http://doi.org/dhj8h7. [ Links ]
8. Farias MG, Schunck EG, Dal Bó S, de Castro SM. Definition of reference ranges for the platelet distribution width (PDW): a local need. Clin Chem Lab Med. 2010;48:255-7. http://doi.org/b3zwfc. [ Links ]
9. Brummitt DR, Barker HF. The determination of a reference range for new platelet parameters produced by the Bayer ADVIA120 full blood count analyser. Clin Lab Haematol. 2000;22:103-7. http://doi.org/bdwvfw. [ Links ]
10. Lanzkowsky P. Chapter 12 - Disorders of Platelets. In: Lanzkowsky P, editor. Manual of Pediatric Hematology and Oncology. 5th edition San Diego: Academic Press; 2011. pp. 321-77. http://doi.org/dj4bfc. [ Links ]
11. Monteagudo E, Fernández-Delgado R, Sastre A, Toll T, Llort A, Molina J, et al. Protocol for the study and treatment of immune thrombocytopenic purpura (ITP). ITP-2010. An Pediatr (Barc). 2011; 74:414.e1-8. [ Links ]
12. Provan D, Stasi R, Newland AC, Blanchette VS, Bolton-Maggs P, Bussel JB, et al. International consensus report on the investigation and management of primary immune thrombocytopenia. Blood. 2010;115:168-86. http://doi.org/bwdf3s. [ Links ]
13. Rodeghiero F, Stasi R, Gernsheimer T, Michel M, Provan D, Arnold DM, et al. Standardization of terminology, definitions and outcome criteria in immune thrombocytopenic purpura of adults and children: report from an international working group. Blood. 2009;113:2386-93. http://doi.org/dj3ss8. [ Links ]
14. Consolini DM. Thrombocytopenia in infants and children. Pediatr Rev. 2011;32:135-51. http://doi.org/fgq2pz. [ Links ]
15. Psaila B, Petrovic A, Page LK, Menell J, Schonholz M, Bussel JB. Intracranial hemorrhage (ICH) in children with immune thrombocytopenia (ITP): study of 40 cases. Blood. 2009;114:4777-83. http://doi.org/c2sv5z. [ Links ]
16. Yamaoka G, Kubota Y, Nomura T, Inage T, Arai T, Kitanaka A, et al. The immature platelet fraction is a useful marker for predicting the timing of platelet recovery in patients with cancer after chemotherapy and hematopoietic stem cell transplantation. Int J Lab Hematol. 2010;32:e208-16. http://doi.org/cr7p45. [ Links ]