Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em
SciELO
Similares em
SciELO -
 Similares em Google
Similares em Google
Compartilhar
Revista de la Facultad de Medicina
versão impressa ISSN 0120-0011
rev.fac.med. vol.62 no.4 Bogotá out./dez. 2014
https://doi.org/10.15446/revfacmed.v62n4.44498
DOI: http://dx.doi.org/10.15446/revfacmed.v62n4.44498
CASE REPORTS
Patient with neuropsychiatric symptoms and insulinoma of difficult preoperative localization
Paciente con síntomas neuropsiquiátricos e insulinoma de difícil localización preoperatoria
Angélica María González-Clavijo1, Luis Felipe Fierro-Maya2
1 Clínica Fundadores. Bogotá, Colombia.
2 Grupo de Endocrinología Oncológica, Instituto Nacional de Cancerología y Endocrinólogo Clínica Fundadores. Bogotá.
Correspondence: Angélica María González-Clavijo. Calle 25 No. 69D 51, Bogotá, Colombia. Phone: (57) 300-2117463. E-mail: angelik_md@yahoo.com.
Received: 20/07/2014 Accepted: 04/08/2014
Summary
This paper describes the case of a patient with neuropsychiatric symptoms who was diagnosed with hyperinsulinemic hypoglycemia with high suspicion of insulinoma, even after conventional diagnostic imaging was unable to locate it. A selective angiography of the pancreatic arteries and a calcium stimulation test were conducted to determine its location. The patient underwent a distal pancreatectomy using an intraoperative ultrasound, resulting in the disappearance of her symptoms.
Keywords: Insulinoma; Hypoglycemia; Psychiatry; Angiography (MeSH).
González-Clavijo AM, Fierro-Maya LF. Paciente con síntomas neuropsiquiátricos e insulinoma de difícil localización preoperatoria. Rev Fac Med. 2014;62(4):637-40. http://dx.doi.org/10.15446/revfacmed.v62n4.44498.
Resumen
Se describe el caso de una paciente con síntomas neuropsiquiatricos, a quien, finalmente, se le diagnosticó hipoglucemia hiperinsulinemica con alta sospecha de Insulinoma, aunque las imágenes diagnosticas convencionales no lograron localizarlo. Fue necesaria la realización de arteriografía selectiva de arterias pancreáticas y test de estimulación con calcio para su ubicación. La paciente fue llevada a pancreatectomia distal con ecografía intraoperatoria, consiguiendo la resolución de los síntomas.
Palabras clave: Insulinoma; Hipoglucemia; Psiquiatría; Angiografía (DeCS).
González-Clavijo AM, Fierro-Maya LF. Patient with neuropsychiatric symptoms and insulinoma of difficult preoperative localization. Rev Fac Med. 2014;62(4):637-40. http://dx.doi.org/10.15446/revfacmed.v62n4.44498.
Clinical case
The 49-year-old patient went to ER on three occasions in the six months previous to her last admittance for symptoms of agitation, delusions, gentle crying and sleepwalking. The patient was initially thought to suffer from a psychiatric disorder and was given benzodiazepine anxiolytics. On the third admittance, ER staff found low glucose levels (42mg/dL), which resulted in her hospitalization to correct the hypoglycemia and to study her case further.
A broader clinical history revealed an increase in food intake and a 10-kilogram weight gain in the previous three months. All medications except the intravenous dextrose at 10% were suspended and she was closely monitored to rule out the intake of glucose-lowering substances. A three-hour fasting test then revealed symptoms of psychomotor restlessness and capillary glucose levels of 44 mg/dL correlated to a plasma glucose level of 40 mg/dL. The plasma levels of insulin – tested by chemoluminescence – in the same sample were 32uU/mL and C-peptide levels in 2.7nmol/mL.
It was not possible to determine the levels of proinsulin or sulfonylureas. Plasma levels of cortisol, hepatic enzymes, creatinine and IGF-1 during fasting were normal. This led to the diagnosis of hyperinsulinemic hypoglycemia, so a a contrast enhanced abdominal computerized tomography (CT) was performed as well as an abdominal Magnetic Resonance Imaging (MRI) with Gadolinium were conducted to search for pancreatic lesions,but both were normal; an endoscopic ultrasonography also failed to find pancreatic lesions.
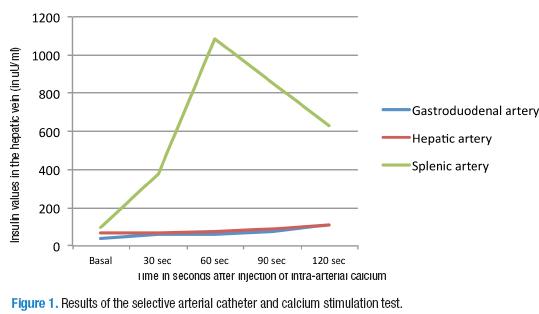
We then proceeded to perform a selective angiography of the pancreatic arteries and an arterial calcium stimulation test with hepatic vein sampling; with these test results we obtained a post-stimulation value almost 10 times higher than the basal level in the splenic territory (in the midportion, as it was not possible to place the catheter as far as the distal portion). The levels in other territories were not significantly elevated (Figure 1).
Based on these results a surgery was performed, and through palpation a nodule at the intersection of the body and tail of the pancreas along the upper edge was detected and then confirmed by intraoperative ultrasound with a diameter of approximately 17mm. The exploration was negative for any suspicious ganglionar enlargement. We were unable to enucleate the lesion due to heavy bleeding from a torn of the mesenteric vein, so a distal pancreatectomy was performed. The post-operative state of the patient was favourable and she was released with adequate glycemic control. The pathology report showed that there was a neuroendocrine neoplasia of 18x15mm, histology grade 1 ( 1), with less than 1 mitosis in 10 CAP, without lymphovascular invasion; an immunohistochemistry tested positive for chromagranin, synaptophysin, CDX2 and insulin, and the KI 67 was at 1%. The patient has remained asymptomatic and after six months of monitoring has shown no signs of relapse.
Discussion
Insulinoma is a rare neuroendocrine tumour of the pancreatic islet cells. Most cases are sporadic; however, in 4 to 5% of cases, it is associated with multiple endocrine neoplasia type 1 (2). Most documented cases are found in centres of reference such as the Mayo Clinic, which has published 237 cases in a 20-year period (1987 to 2007), revealing an average of 50 years of age at the time of surgery and a slight predominance of women (3).
The diagnosis of insulinoma is made by demonstrating hypoglycemia in the presence of hyperinsulinemia, either spontaneously or during the classic 72-hour fasting test, using the following six criteria: glucose levels in blood lower than 40 mg/dL with concomitant insulin levels higher or equal to 3uU/mL, C-peptide levels higher or equal to 200 pmol/L, proinsulin levels higher or equal to 5 pmol/L, B-Hydroxybutyrate levels lower or equal to 2.8 mmol/L and an absence of sulfonylurea metabolites in plasma or urine (2).
The symptoms of hypoglycemia are divided into symptoms of neuroglycopenia and autonomic symptoms. The first group includes headaches, double and/or blurred vision, confusion, dizziness, abnormal behaviour, lethargy, amnesia and, on rare occasions, convulsions and coma (2, 4-6); the autonomic symptoms include sweating, weakness, hunger, tremors, nausea, sensation of heat, anxiety, and palpitations (2,7).
On average, these symptoms are present for 1.5 years before a diagnosis is made, although some patients can have symptoms for decades before an appropriate diagnosis is made (3,5). This delay in diagnosis is more common in patients with insulinoma and neuropsychiatric symptoms, which results in a wrongful diagnosis in up to 64% of cases (8). There is a wide variety of psychiatric symptoms documented in the literature of patients with insulinoma (Table 1), so it is essential that the clinic be aware in their differential diagnosis, especially when psychiatric symptoms fluctuate over time or in their severity.
Surgical treatment of an insulinoma results in complete recovery in most cases, but the biggest challenge lies in locating the insulinoma prior to surgery. It is well known that the preoperative localization of the tumor increases the chances of success in surgery, minimizing surgical time and reducing the risk of complications; however, despite the technical advances in diagnostic imaging, tumours smaller than 2cm are difficult to locate, which means that other methods are necessary to establish their location.
The invasive options for testing are the endoscopic ultrasound (EUS), the selective intra-arterial calcium stimulation test, and the intraoperative ultrasound. The first has a sensitivity of 75 to 85% (3,14), but the success of diagnosis depends on the expertise of the operator and the location of the tumour, so this method is best suited for the tail of the pancreas. Selective arteriography of the pancreatic arteries and calcium stimulation, developed in 1989, is a dynamic test that involves injecting calcium gluconate in the superior mesenteric artery, the gastroduodenal artery and the splenic artery and collecting a sample from the hepatic vein to measure the insulin. The intra-arterial calcium triggers a liberation of insulin into the hyperfunctioning beta cells – insulinoma or nesidioblastosis - but not into the normal beta cells (15), so that if there is an elevated level of insulin after stimulation more than two times the basal level, it will be considered positive for a hyperfunctioning lesion, located in the irrigation territory of the stimulated artery. The sensitivity reported for the ASEC is between 80 and 94% (3,16).
Finally, the intraoperative ultrasound is a useful option when other methods have failed. Currently laparoscopic transducers are used to make the procedure less bloody. The intraoperative ultrasound has a reported sensitivity of 84 to 100% (17,18).
In the case of this particular patient, it was deemed necessary to use all of the techniques described to determine the exact location of the tumour. It was subsequently observed that the most successful methods in determining the precise location were the ASEC, the intraoperative ultrasound and direct palpation.
Conclusions
Although the insulinoma is a very rare and often benign neuroendocrine tumour, the symptoms of neuroglycopenia can have a great effect over a long period of time on the health of those affected, especially when these symptoms do not present themselves in a typical way, as in this case or in other reviewed cases with psychiatric manifestations. In these cases, it is important to bear in mind the diagnosis of hypoglycemia in the differential diagnosis, and when it has been confirmed, to refer the patient to a specialized centre that has the staff and the diagnostic tools to make the proper biomedical diagnosis and locate the lesion to provide a cure, since in most of the reviewed cases, the psychiatric symptoms were completely reversed when the disease at the root of the problem was treated.
Conflict of interest
None declared by the authors.
Financing
None declared by the others.
Acknowledgements
Thank you to the directors and colleagues of the Clínica Fundadores de Bogotá.
References
1. Klimstra DS, Modlin IR, Coppola D, Lloyd R V, Suster S. The pathologic classification of neuroendocrine tumors: a review of nomenclature, grading, and staging systems. Pancreas. 2010; 39:707-12. http://doi.org/fdfqrp. [ Links ]
2. Jensen RT, Cadiot G, Brandi ML, de Herder WW, Kaltsas G, Komminoth P, et al. ENETS Consensus Guidelines for the management of patients with digestive neuroendocrine neoplasms: functional pancreatic endocrine tumor syndromes. Neuroendocrinology. 2012; 95:98-119. http://doi.org/zjn. [ Links ]
3. Placzkowski KA, Vella A, Thompson GB, Grant CS, Reading CC, Charboneau JW, et al. Secular trends in the presentation and management of functioning insulinoma at the Mayo Clinic, 1987-2007. J Clin Endocrinol Metab. 2009; 94:1069-73. http://doi.org/fschdk. [ Links ]
4. Correia P, Panchani R, Ranjan R, Agrawal C. Insulinoma presenting as refractory seizure disorder. F1000Res. 2012; 1:15. [ Links ]
5. Dizon AM, Kowalyk S, Hoogwerf BJ. Neuroglycopenic and other symptoms in patients with insulinomas. Am J Med. 1999; 106:307-10. http://doi.org/b23k64. [ Links ]
6. Stucchi-Portocarrero S. Insulinoma, convulsiones y psicosis: a propósito de un caso. Rev Neuropsiquiatr. 2011; 74:279-81. [ Links ]
7. Mathur A, Gorden P, Libutti SK. Insulinoma. Surg Clin North Am. 2012; 89:1105-21. http://doi.org/fnrj63. [ Links ]
8. Ding Y, Wang S, Liu J, Yang Y, Liu Z, Li J, et al. Neuropsychiatric profiles of patients with insulinomas. Eur Neurol. 2010; 63:48-51. http://doi.org/cfbdnb. [ Links ]
9. Nakamura Y, Doi R, Kohno Y, Shimono D, Kuwamura N, Inoue K, et al. High-dose calcium stimulation test in a case of insulinoma masquerading as hysteria. Endocrine. 2002; 19:127-30. http://doi.org/c7wt73. [ Links ]
10. Colán TC, Gálvez GA, Zevallos DC. Síntomas psiquiátricos e insulinoma: reporte de caso. Rev Chil Neuropsiquiatr. 2013; 51:149-50. http://doi.org/zjp. [ Links ]
11. Kim KH, Kim ES, Kim Y Il, Na YW, Choi HJ, Kwon JH, et al. A Case of insulinoma with hypoglycemic encephalopathy. Korean Diabetes J. 2013; 14:98-101. http://doi.org/zjq. [ Links ]
12. Vilchez MF, Ferreyra L. Manifestaciones neuropsiquiátricas en insulinoma: presentación de un caso. Experiencia Médica. 2010; 26:1-5. [ Links ]
13. Renca S, Santos G, Cerejeira J. An insulinoma presenting with hypochondriac delusions and food refusal. Int Psychogeriatr. 2013; 25:1909-11. http://doi.org/zjr. [ Links ]
14. Rosch T, Lightdale C, Botet J, Boyce G, Sivak M, Yasuda K, et al. Localization of pancreatic endocrine tumors by endoscopic ultrasonography. N Engl J Med. 1992; 326:1721-6. http://doi.org/b554wz. [ Links ]
15. Doppman JL, Miller DL, Shawker TH, Gorden P. Insulinomas: localization with selective intraarterial injection of calcium. Radiology. 1991; 178:237-41. http://doi.org/zjs. [ Links ]
16. Guettier J-M, Kam A, Chang R, Skarulis MC, Cochran C, Alexander HR, et al. Localization of insulinomas to regions of the pancreas by intraarterial calcium stimulation: the NIH experience. J Clin Endocrinol Metab. 2009; 94:1074-80. http://doi.org/dggzdj. [ Links ]
17. Galiber A, Reading CC, Charboneau J, Sheedy P, James E, Gorman B. Localization of pancreatic insulinoma: Comparison of pre- and intraoperative US with CT and angiography. Radiology. 1988; 166:405-8. http://doi.org/zjt. [ Links ]
18. Boukhman MP, Karam JM, Shaver J, Siperstein A E, DeLorimier AA, Clark OH. Localization of insulinomas. Arch Surg. 1999; 134:818-23. http://doi.org/fvs3rq. [ Links ]