Introduction
Congenital anomalies are found in 2-3% of newborns and constitute a major public health problem; in Colombia, the most common anomalies of this type include alterations of the limbs, central nervous system defects and congenital heart disease (CHD).1 Given that CHD have the greatest impact, since 2010, pulse oximetry has been implemented in the U.S. as a routine screening method on all live newborns for early detection of congenital heart defects associated with hypoxia in the neonatal period. 2
Some studies associate the occurrence of CHD with teratogenic agents, and others, based on animal models extrapolated to humans, argue that the consumption of folic acid (also known as folate) during the first 3 weeks of pregnancy prevents heart disease caused by exposure to teratogens. 6-7 In this sense, it is known that initiating folic acid supplementation in humans one month prior to pregnancy reduces the incidence of neural tube defects by more than 70%;8 furthermore, there is epidemiological evidence that supplementing mothers with this vitamin protects the babies against various types of CHD. 9
The aim of this study was to obtain data on prenatal exposure variables of CHD patients treated in Cali, Colombia. Consequently, this research is the first step towards improving the understanding of the multiple factors related to CHD in the local context.
Materials and methods
A descriptive case series study was conducted using a random sample of 30 patients under 6 years of age with CHD treated in 2 institutions of Cali: DIME Clínica Neurocardiovascular (institution 1) and Clínica Versalles (institution 2). Isolated ductus arteriosus cases were excluded because only newborns without gestational age or disease status restriction were included in the study, as it is known that, regardless of exposure to other factors, gestational age and the presence of respiratory distress syndrome can affect ductal closure. 10
Patients treated between September 2014 and November 2015 were selected for this study. In the case of institution 1, which is a reference center for the diagnosis and management of cardiovascular diseases, the database of echocardiograms performed there was reviewed and the mothers of CHD patients born in the past 5 years were contacted by phone to invite them to participate in the study; calls were made in chronological order, that is beginning with the patient most recently treated. Once the mother agreed to participate, an appointment was made with her and the patient to formally carry out the informed consent process and administer the survey to the mother.
In order to select the patients in institution 2, which is a tertiary care center with the highest number of births in the city, all the care staff of the Obstetrics Service and the Newborn Intensive Care Unit were informed of the study, so that when new cases of newborns with CHD confirmed by echocardiogram were diagnosed, they informed the study staff, who also asked daily if there were any new cases, thus allowing an active search. When the CHD were confirmed, the informed consent process and the mother's survey were formally con-ducted. No patients were captured by screening with pulse oximetry.
The administered survey was an extensive instrument of more than 90 pages, validated in previous original studies and designed by the research groups Congenital and Perinatal Malformations, Medical Genetics and Dysmorphology (MACOS by its acronym in Spanish) and Epidemiology and Population Health (GESP by its acronym in Spanish). It sought to find out multiple socio-demographic and exposure variables such as drinking water, medicines, cigarettes, alcohol and other psychoactive substances, as well as the history of diseases and X-ray studies. At this point, it is worth noting that there may be memory bias when answering this type of survey.
The collected data were digitized in a Microsoft Excel sheet and a univariate and bivariate descriptive statistical analysis was performed using relative frequency distributions (%) presented in tables to describe the exposure characteristics found.
This study was approved by the Institutional Committee for the Review of Human Ethics of the Faculty of Health of the Universidad del Valle by means of approval act No. 04013 of April 5, 2013. Moreover, the principles of the Declaration of Helsinki11 and the regulations of Resolution 8430 of 1993 of the Colombian Ministry of Health were followed. 12
Results
Socio-demographic characterization
Of the 30 cases, 24 were captured in institution 1 and 6 in institution 2. The births took place in 13 health institutions, mostly in the Hospital Universitario del Valle and the Clínica Versalles, which means that 16 of the patients were born in one of these 2 institutions.
The sample studied was composed of 19 boys (63.33%) and 11 girls (36.67%). Regarding health insurance, 46.66% of the mothers were enrolled in the subsidized regime and 53.33% in the contributory regime, and 56.66% of them lived in Cali during the periconceptional period (3 months before and 3 months after the approximate date of conception or fertilization) (Table 1).
Table 1 Socio-demographic characteristics of the study cases.
| Characteristics | n (%) | ||
| Sex | Women | 11 (36.67%) | |
| Men | 19 (63.33%) | ||
| Place of residence during the periconceptional period | Cali | 17 (56.66%) | |
| Outside Cali | 13 (43.33%) | ||
| Health Care System | Contributive | 16 (53.33%) | |
| Subsidized | 14 (46.66%) | ||
Source: Own elaboration.
Among the mothers who lived in Cali during their periconceptional period, most resided in the central and eastern areas (Aguablanca district): 23.5% in commune 14 and 17.6% in commune 9; the remaining mothers lived in different communes during this period, that is, they were distributed without constituting aggregates. Both institutions where the study was conducted are in commune 2.
Characterization of the exposure
20 of the 30 pregnancies were not planned, and, on average, the mothers found out about their status during the 7th week. An average of 8 prenatal check-ups was obtained, and ultrasound studies detected some fetal structural abnormality in only 2 cases; no invasive prenatal diagnostic study was performed for any of these cases. In a third case, the ultrasound reported a placental abnormality.
Table 2 shows and describes the types of heart disease found in the patients included in the series, while Tables 3, 4 and 5 summarize the most relevant maternal exposures found in the research.
Table 2 Characterization of the patients included in the research.
| Case | Age at study entry | Heart disease | Associated abnormalities |
| 1 | 1 day | Transposition of the great arteries | None |
| 2 | 4 months | Double atrioventricular canal, single ventricle, transposition of the great arteries | Complete situs inversus, intestinal malrotation |
| 3 | 2 months | Tricuspid insufficiency | None |
| 4 | 7 days | Tetralogy of Fallot, patent ductus arteriosus, interatrial communication and hypoplasia of the valve, trunk and branches of the lungs | None |
| 5 | 1 day | Ventricular septal defect | Right preauricular sinuses, abnormal hand and foot dermatoglyphics, clinodactyly, hypoplasia of the middle phalanx of the fifth digit of the left hand |
| 6 | 1 day | Ventricular septal defect, patent foramen ovale | Down facies (Down syndrome confirmed by karyotype) |
| 7 | 5 days | Left lower pulmonary vein stenosis, ventricular septal defect, patent ductus arteriosus | Low-set ears, over-folded ears, prominent antihelix, hypoplastic helix crus, protruding cheekbones, microstomia, hands in trisomy, prominent heel (trisomy 18 confirmed by karyotype) |
| 8 | 1 day | Complete atrioventricular canal | None |
| 9 | 20 days | Patent ductus arteriosus, patent foramen ovale, mild to moderate mitral regurgitation, mild tricuspid regurgitation | None |
| 10 | 2 days | Tricuspid atresia, right ventricular hypoplasia, pulmonary atresia | None |
| 11 | 2 months | Truncus arteriosus | Hirsutism (on the face, back and limbs), absent earlobe, wide nasal bridge, micrognathism, micropenis. |
| 12 | 22 days | Double outlet right ventricle, severe pulmonary stenosis, transposition of the great arteries | None |
| 13 | 5 days | Atrioventricular valve dysplasia, moderate tricuspid regurgitation, situs inversus | None |
| 14 | 1 month | Dysplastic pulmonary valve with insufficiency and stenosis | None |
| 15 | 6 months | Ostium secundum atrial septal defect, patent ductus arteriosus | Epicanthal fold, short nose, smooth philtrum, anteverted nostrils |
| 16 | 1 year | Ventricular septal defect, patent foramen ovale | Down facies (Down syndrome confirmed by karyotype), hypothyroidism |
| 17 | 1 month | Tetralogy of Fallot | Low-set ears, myelomeningocele, hydrocephalus, shortening of the second left metatarsal bone, abnormal dermatoglyphics |
| 18 | 4 years | Interatrial communication | Esophageal atresia, neonatal teeth (two incisors), big, protruding ears |
| 19 | 4 years | Double superior vena cava system, persistent left superior vena cava, dilated coronary sinus | Café-au-lait spots (one spot of 5cm in the lower right quadrant of the abdomen) |
| 20 | 2 years | Ventricular septal defect | Delayed psychomotor development, bilateral hydronephrosis, protuding forehead, arched eyebrows |
| 21 | 2 years | Subvalvular aortic stenosis, tricuspid but functionally bicuspid aortic valve, aortic vascular ring in the descending thoracic aorta without coarctation | None |
| 22 | 1 month | Single atrioventricular connection through a central atrioventricular valve, double-outlet right ventricle, blood vessels in abnormal position, right ventricular hypoplasia, right anterior aorta and left posterior pulmonary aorta, interatrial communication, single atrium, lack of interventricular septum, dilated left ventricle, hypoplastic pulmonary artery, patent ductus arteriosus, single atrioventricular valve, right aortic arch, tricuspid pulmonary atresia with severe infundibular and pulmonary stenosis | Right isomerism, esophageal atresia |
| 23 | 1 day | Ostium secundum atrial septal defect, moderate mitral regurgitation | Frontal hemangioma extending towards the right eye, anteverted nostrils, inverted nipples, megabladder, bilateral hydronephrosis, large, thick-walled, partitioned bladder mass, anasarca, anal atresia, urethral meatus agenesis, probable urogenital sinus, lumbar hemivertebra |
| 24 | 2 days | Right ventricle hypoplasia,pulmonary atresia | None |
| 25 | 2 years | Supracardiac pulmonary anomalous venous connection, interatrial communication, persistent left superior vena cava. | Café au lait spot on right shoulder with a diameter of 3cm, short nose, barely visible nasal tip, anteverted nostrils, long philtrum, protruding cheekbones, left cryptorchidism |
| 26 | 5 years | Ventricular septal defect, interatrial communication, pulmonary stenosis | Seizures, repeated respiratory infections, strabismus, flattened cervical vertebrae, delayed psychomotor development, self-injury (of the tongue), dolicocephaly, big ears, thick lips, pectus excavatum, right cryptorchidism, hypotonia |
| 27 | 4 years | Tetralogy of Fallot, mild stenosis at the origin of the right pulmonary branch | Atopic dermatitis, mild y-shaped syndactyly between toes 2 and 3, including penis. |
| 28 | 2 years | Pulmonary stenosis, patent foramen ovale | Neonatal jaundice, wide nose, small café-au-lait spots |
| 29 | 2 years | Ebstein anomaly, tricuspid insufficiency | Left pyelectasis, two café-au-lait spots <1cm on the abdomen |
| 30 | 2 years | Coarctation of the aorta, interatrial communication | Agenesis of the corpus callosum |
Source: Own elaboration.
Table 3 Periconceptional exposures found in this study.
| Case | Exposure in the 3rd month before conception | Exposure in the 2nd month before conception | Exposure in the 1st month before conception | Exposure in the 1st month after conception | Exposure in the 2nd month after conception | Exposure in the 3rd month after conception |
| 1 | None | Warfarin | Alcohol (beer, rum, aguardiente, whisky) | Acetaminophen, warfarin, alcohol (beer, rum, aguardiente, whisky) | Warfarin, alcohol (beer, rum, aguardiente, whisky) | Warfarin, alcohol (beer, rum, aguardiente, whisky) |
| 2 | Smoker at home | Smoker at home | Smoker at home | Smoker at home | Acetaminophen, smoker at home | Smoker at home |
| 3 | NPH and aspart insulin, smoker at home | NPH and aspart insulin, smoker at home | NPH and aspart insulin, smoker at home | NPH and aspart insulin, smoker at home | NPH and aspart insulin, smoker at home | NPH and aspart insulin, smoker at home |
| 4 | Contraceptive injection, smoker at home | Contraceptive injection, smoker at home | Contraceptive injection, smoker at home | Contraceptive injection, metoclopramide, acetaminophen | Contraceptive injection | Contraceptive injection |
| 6 | None | Acetaminophen | None | Alcohol (beer) | None | Acetaminophen |
| 7 | None | None | None | Aspirin, metoclopramide | Aspirin, metoclopramide | Aspirin |
| 10 | None | None | None | None | None | Acetaminophen, metoclopramide |
| 11 | None | None | None | Acetaminophen | Acetaminophen, alcohol (rum, aguardiente, whisky) | None |
| 12 | Acetaminophen | Acetaminophen | Acetaminophen | Acetaminophen | Acetaminophen | Acetaminophen |
| 13 | Alcohol (beer), marihuana, smoker at home | Alcohol (beer), marihuana, smoker at home | Alcohol (beer), marihuana, smoker at home | Alcohol (beer), marihuana, smoker at home | Levothyroxine, Alcohol (beer), marihuana, smoker at home | Levothyroxine, marihuana, smoker at home |
| 14 | Smoker at home, alcohol (beer, rum, aguardiente, whisky) | Smoker at home, alcohol (beer, rum, aguardiente, whisky) | Acetaminophen, smoker at home, alcohol (beer, rum, aguardiente, whisky) | Acetaminophen, omeprazole, smoker at home, alcohol (beer, rum, aguardiente, whisky) | Acetaminophen, omeprazole, smoker at home | Smoker at home |
| 15 | Smoker at home | Smoker at home | Smoker at home | Smoker at home | Acetaminophen, smoker at home | Smoker at home |
| 17 | None | Smoker at home | Smoker at home | Smoker at home | Smoker at home | Smoker at home |
| 18 | None | None | None | Acetaminophen | Acetaminophen | Levothyroxine |
| 19 | Alcohol (beer), smoker at home | Alcohol (beer), smoker at home | Alcohol (beer), smoker at home | Acetaminophen, smoker at home | Ovules, acetaminophen, smoker at home | Smoker at home |
| 20 | Acetaminophen | Acetaminophen | Acetaminophen | None | None | None |
| 21 | Acetaminophen, smoker at home | Acetaminophen, smoker at home | Acetaminophen, smoker at home, alcohol (beer, rum, aguardiente, whisky) | Acetaminophen, metoclopramide, smoker at home, alcohol (beer, rum, aguardiente, whisky) | Smoker at home, misoprostol | Smoker at home |
| 22 | None | None | None | Alcohol (whisky cream) | None | None |
| 24 | None | None | None | None | None | Acetaminophen |
| 25 | None | Acetaminophen | Acetaminophen | Acetaminophen, alcohol (beer) | None | None |
| 27 | None | None | None | None | Acetaminophen | Acetaminophen |
| 28 | Smoker at work | Smoker at work | Smoker at work | Acetaminophen, smoker at work | Acetaminophen, smoker at work | Acetaminophen, smoker at work |
| 29 | None | None | None | None | Magnesium sulfate, acetaminophen | Magnesium sulfate, acetaminophen |
Source: Own elaboration.
Table 4 Maternal diseases and pregnancy exposures.
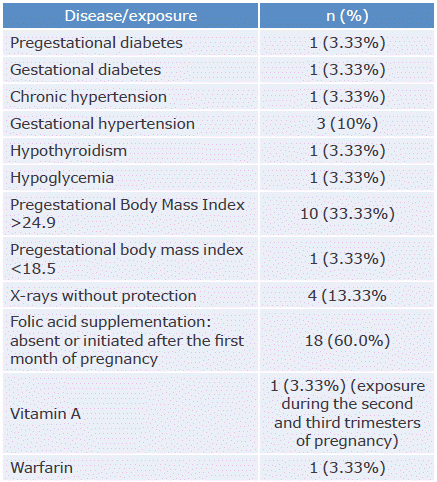
* The questionnaire included the quantification of alcohol and marijuana consumption; however, the mothers did not remember or could not specify the amount.
Source: Own elaboration.
Discussion
Socio-demographic aspects
41% of the mothers who lived in Cali during their periconceptional period resided in communes 14 and 9, which are composed of neighborhoods in strata 2 and 3 (Table 6).
Table 6 Socioeconomic strata in Colombia according to the National Administrative Department of Statistics.
| Stratum | Description |
| 1 | Low-low. Beneficiaries of home utility subsidies. |
| 2 | Low. Beneficiaries of home utility subsidies. |
| 3 | Middle-low. Beneficiaries of home utility subsidies. |
| 4 | Middle. They are not beneficiaries of subsidies, nor do they pay surcharges; they pay exactly the amount that the company defines as the cost for providing home utilities. |
| 5 | Middle-high. They pay surcharges (contribution) on the value of home utilities. |
| 6 | High. They pay surcharges (contribution) on the value of home utilities. |
Source: Elaboration based on the data by National Administrative Department of Statistics.14
In commune 14, 68.4% of the houses are classified as stratum 1 and 31.6% as stratum 2; 17.7% of office machinery factories (telephones, computers, printers, photocopiers, video projectors, guillotines, etc.), 11.8% of automotive industries and 10.7% of electricity, gas and water suppliers of the city are located in this place. Some of its main problems are the lack of adequate green areas and environmental education programs, and inadequate solid waste disposal. 13
On the other hand, the commune 9 is characterized because 10% of the households are stratum 1, 20% are stratum 2, and 70% are stratum 3. This place concentrates 32.69% of the recycling centers and 25% of the tanneries and centers of preparation of leathers (footwear) of the city.13
These findings explain the need for a specific and detailed analysis of risk factors associated with congenital anomalies in these geographical areas.
Exposure aspects
An unplanned pregnancy increases the chances of risk exposure during the periconceptional period, as a woman who is not aware of her condition continues to engage in behaviors she might not have if she knew. In addition, late pregnancy awareness does not allow for the timely consumption of the necessary micronutrients. In this study, 66.66% of the pregnancies were unplanned.
Quality of prenatal care
The mothers assisted, on average, to 8 prenatal checkups, which is an acceptable number. All of them underwent at least 1 obstetric ultrasound, although this examination only detected anomalies in 3 cases; thus, considering that ultrasound findings in one of the cases revealed a placental anomaly, only 2 patients were diagnosed with fetal structural anomalies. It should be noted that the 2 mothers diagnosed with fetal structural anomalies belong to the contributory regime, which means that some fetal structural anomaly was detected in 12.5% of the mothers in the contributory regime and none in the mothers enrolled in the subsidized regime. This may suggest that there is less access to timely and quality ultrasound for the mothers in the latter, as previously reported. 15
Maternal hypertension
Chronic maternal hypertension has been associated with CHD (OR: 1.81, 95% CI: 1.61-2.03), 16 specifically with ventricular septal defects, common atrioventricular canal defect and truncus arteriosus. It has been found that there is increased prevalence of non-critical CHD in children of women who develop preeclampsia after the 34th week, and that the prevalence of critical and non-critical heart disease increases in children of women who develop preeclampsia before the 34th week. 17 Significant associations between maternal hypertension and CHD in general have been observed for treated (RR: 2, 95% CI: 1.5-2.7) and untreated patients (RR: 1.4, 95% CI: 1.2-1.7), as well as for hypertension (RR: 1.8, 95 CI%: 1.5-2.2). 18
This study found that 4 of the mothers had hypertension: 1 of them had chronic hypertension and her child presented tricuspid insufficiency, while the other 3 mothers had gestational hypertension with onset before the 34th week and their children presented syndromic cardiopathies.
Maternal diabetes
It is well known that the incidence of congenital abnormalities, including heart disease, is high in children of diabetic mothers.5 Traditionally, it was thought that this increased risk was limited to patients with diabetes at the time of conception; however, it has been suggested that hyperglycemia caused by gestational diabetes may also influence cardiac development, which has been particularly associated with abnormalities such as patent ductus arteriosus, pulmonary stenosis and interventricular septal hypertrophy. 19 Likewise, Ornoy20 proposes hyperglycemia-induced oxidative stress as a teratogenic mechanism of maternal diabetes.
This study also found that 2 of the mothers had diabetes: the first, mother of a patient with isolated tricuspid insufficiency, had preconceptional type 1 diabetes -which is associated with CHD (OR: 4.65, 95%CI: 4.13-5.24), 16 specifically coarctation of the aorta,4 while the second, mother of a patient with Ebstein's anomaly and tricuspid insufficiency, had gestational diabetes. It is noteworthy that alterations in the tricuspid valve were observed in 3 of the 4 cases of maternal hypertension and in the 2 cases of gestational diabetes.
Maternal thyroid disease
Studies such as Liu et al.16 have associated thyroid disorders with CHD (OR: 1.45, 95%CI: 1.26-1.67). In the present investigation, 1 of the mothers had hypothyroidism and her child (case 18) presented ventricular septal defect.
Maternal hypoglycemia
In animal models, hypoglycemia has been found to be potentially teratogenic during embryogenesis. 8 This study found that 1 of the mothers had hypoglycemia and her child had subvalvular aortic stenosis, tricuspid (but functionally bicuspid) aortic valve and aortic vascular ring in the descending thoracic aorta without coarctation.
Maternal body mass index
Previous studies have reported an association between maternal body mass index (BMI) and the occurrence of CHD; in general, the higher the BMI, the higher the OR for CHD. 21 Low maternal weight, on the other hand, appears to increase the risk for aortic stenosis. 22
This study found that 10 of the mothers started the pregnancy with BMI above normal values (>24.9) and 1 with BMI lower than normal values (< 18.5), which may indicate that BMI alterations are an important factor for the development of heart disease in the study population.
Exposure to X-rays
It has been found that the risk of inducing embryonic death or congenital anomalies after irradiating a newly fertilized egg with the usual range of doses used in diagnostic radiology is very low compared to the spontaneous risks. However, these findings are not considered a reason not to take precautions when possible, in part due to the possibility of epigenetic alterations. 23 In this sense, Ornoy20 proposes that the teratogenic mechanism of ionizing radiation is the induction of oxidative stress.
This research found that 4 of the mothers underwent x-ray studies during pregnancy without protection, and that 3 of these children had non-syndromic heart disease and 1 had syndromic heart disease.
Exposure to tobacco
Mothers who smoke during the first trimester have been reported to be at increased risk of having children with CHD (OR: 1.16, 95%CI: 1.08-1.24). A dose-dependent effect and a very strong association have also been observed in some specific defects such as pulmonary valve disease, pulmonary artery anomalies and isolated interatrial communication. 24 In this sense, passive periconceptional exposure to tobacco has been established as an independent risk factor for heart disease25,26 and the teratogenic mechanism of tobacco is the induction of oxidative stress. 20
None of the mothers in this study smoked during pregnancy, so there appears to be an awareness of the potential dangers of smoking among them, but this was not the case for passive smoking exposure, as 36.66% of them were exposed.
Exposure to alcohol
Maternal alcohol consumption is known to cause multiple birth defects included in fetal alcohol syndrome (FAS), among them, heart disease. Only 10% of those affected with alcohol embryopathy meet all the criteria for FAS, while the remaining 90% fall somewhere else on the spectrum.
Multiple studies have shown that maternal alcohol consumption increases the risk of CHD3,16,27 and teratogenic mechanisms include disruption of midline expansion; 28,29 apoptosis and alteration of neural crest and anterior precordal mesoderm cell migration; 30-32 disruption of several signaling pathways such as shh, fgf8, foxa2 and goosecoid; 29,33 and induction of oxidative stress. 20,34 This study found that 30% of the mothers consumed some alcohol, perhaps indicating a lack of awareness that there is no safe time or dose for alcohol consumption during pregnancy.
Folic acid intake
Folate is necessary for the synthesis of purines and pyrimidines, and therefore, it is important for proper cell proliferation. This micronutrient is also necessary for the synthesis of S-Adenosyl methionine, the main donor of methyl groups, and for adequate epigenetic regulation. 35,36
It is well known that starting folic acid supplementation 1 month before pregnancy reduces over 70% of neural tube defects. 8 Worldwide, it is recommended that all women who may become, plan to become, or are pregnant take a daily supplement of 0.4mg to 0.8mg (400-800µg) of this vitamin. 37
On the other hand, by using animal models extrapolated to humans, it has been found that the consumption of folic acid during the first 3 weeks of pregnancy prevents heart disease due to teratogenic exposure. 6,7 There is epidemiological evidence in humans that maternal folate supplementation is associated with a significant decrease in the risk of CHD (RR: 0.72; 95%CI: 0.63-0.82). 9
This study found that only 10% of mothers started folic acid supplementation 1 month before conception, 30% during the first month of pregnancy, 36.66% after the first month, 16.66% did not receive supplementation and 6.66% took some multivitamin after the first month of pregnancy. The methodology used does not allow stating that the folate consumed did not have a protective effect against congenital anomalies. However, it showed that a high percentage (60%) of mothers did not consume it in the way recommended to generate a protective effect against neural tube defects nor in the way theoretically suggested by animal studies to achieve a protective effect against heart disease. Thus, although 83.34% of mothers received folic acid supplementation, it could only have a potential protective effect against neural tube defects and heart disease in the 10% who initiated it 1 month before conception, and it only had a potential protective effect against CHD in the 30% who initiated it during the first month of conception.
It is very interesting that the teratogenic mechanism of several of these factors (diabetes, X-rays, cigarettes, alcohol) is the generation of oxidative stress, since insufficient or inappropriate consumption of folic acid, which has an antioxidant action, may facilitate teratogenesis by these factors.
Vitamin A intake
The teratogenic effect of retinoic acid -a vitamin A derivative- on cardiovascular morphogenesis has been demonstrated in animal models at both higher38,39 and lower than normal doses. 40,41 In this study, 6.66% of the mothers took a multivitamin and were unaware of its vitamin A content, and even 3.33% claimed to have specifically consumed vitamin A. In this regard, there is a need to raise awareness of the risk of excessive supplementation and the need to discuss micronutrient intake with the physician.
Use of warfarin
Exposure to warfarin between the 6th and 9th week of pregnancy results in hypoplasia of the nasal bone; depressed nasal bridge; deep depression between the nose wings and nasal tip; punctate calcifications of the epiphysis of the axial skeleton, proximal femur, and calcaneus bone (which disappear after the first year); hypoplastic distal phalanges that look like inverted triangles; low birth weight; and sometimes CHD. Moreover, exposure between the 14th and 20th week produces microcephaly, hydrocephaly, Dandy-Walker malformation, agenesis of the corpus callosum, cerebellar degeneration, seizures, spasticity, intellectual disability, language disorders, optic atrophy, cataracts, microphthalmia, Peters anomaly, intrauterine growth restriction and scoliosis. 8
This study found a mother exposed to warfarin since the 9th week; her child presented with non-syndromic transposition of the great arteries and none of the other characteristics of fetal warfarin syndrome. Thus, it is evident that there is a need to educate medical personnel about drug teratogenesis and pharmacological alternatives in order to obtain therapeutic effects with drugs without teratogenic potential.
Use of misoprostol
Prenatal exposure to misoprostol in the first trimester of pregnancy for abortion purposes has been associated with Moebius sequence, limb defects, among other congenital anomalies. 42 For example, Pachajoa et al.43 reported a case of prenatal exposure to misoprostol in which the newborn presented CHD.
This study found a mother exposed to this drug in the second month of pregnancy, with a child that had subvalvular aortic stenosis, tricuspid but functionally bicuspid aortic valve and aortic vascular ring in the descending thoracic aorta.
The limitations of this research include that the sample used was small and the methodology employed has risk of memory bias. In addition, exposures were evaluated only through questions to the patients' mothers and reviews of available medical history at the time of evaluation, while no laboratory exams were performed to determine exposures.
Conclusions
This case series presents several prenatal exposures associated with potential risk for CHD, such as maternal diabetes, vitamin A intake, undergoing unprotected x-ray studies, altered pregestational BMI, alcohol consumption, passive smoking and inadequate folic acid supplementation.
Insufficient or untimely intake of folic acid could facilitate the generation of teratogenic effects of oxidizing substances. Therefore, women in Cali should be educated about the importance of adequate folic acid intake and the risks of exposure to teratogenic agents during pregnancy.
Prenatal detection of congenital defects, including heart disease, was low (10%), which highlights the need to implement neonatal CHD screening with pulse oximetry.