Introduction
Priapism is a prolonged penile erection that persists beyond or is not related to sexual interest or stimulation. It may be classified as ischemic (low flow), non-ischemic (high flow), and recurrent. The first type is the most commonly observed and is associated with the absence of cavernous blood flow and multiple causes such as hematological, immunological, neurological and metabolic disorders, malignancy, medications, toxins, among others. In contrast, the second type is caused by injury.1,2
In hemodialysis patients, priapism has been reported with a prevalence of 1 per 196 men.3 Several associated risk factors have been established, which are inherent in this type of therapy, such as acidosis, hypoxemia, hemoconcentration, inflammation, use of drugs (erythropoietin, heparin, prazosin, androgens, etc.), among others.4
On the other hand, infection with SARS-CoV-2, a virus that causes COVID-19, has been linked to the development of coagulopathy and thrombosis, with thromboembolic disease being a manifestation of COVID-19 in severe cases.5-7 From a pathophysiological perspective, infection with this coronavirus and hypercoagulability may be related to the development of priapism.
The following is a case of ischemic priapism in a patient with chronic kidney disease (CKD) on hemodialysis and active SARS-CoV-2 infection with mild COVID-19 symptoms. This report is relevant because this is a rare condition and allows considering that COVID-19 may cause priapism in patients with risk factors such as dialysis therapy and kidney disease.
Case presentation
A 65-year-old male patient on hemodialysis due to a history of stage 5 Ckd secondary to hypertension, with SARS-CoV-2 infection confirmed by RT-PCR and in outpatient follow-up for mild symptoms, consulted the emergency department of a quaternary care center due to a prolonged penile erection lasting 30 hours, painful in the last 12 hours, not induced by sexual activity, that began 18 hours after the last dialysis session was completed.
The patient had a history of secondary hyperparathyroidism and anemia associated with kidney disease. He had started renal replacement therapy 2 years earlier: he attended 3 4-hour weekly hemodialysis sessions with a high-flow dialyzer, Kt/V was >1.2 (adequate target), and the average weight gain in short interdialytic periods was 4%. He was also treated with oral nifedipine 30mg every 8 hours, prazosin 1mg every 8 hours, calcitriol 0.25mcg orally every other day, subcutaneous erythropoietin 4000U every week, and unfractionated heparin 4000U in the extracorporeal circuit during each hemodialysis session. He had been taking the antihypertensive medications for more than two years and did not receive 5-alpha-phosphodiesterase inhibitors.
The patient was initially assessed by the general medicine service, which found normal vital signs and penile erection on physical examination without other relevant results. No changes in skin coloring, edema, or abnormalities in the testicles were found in the assessment.
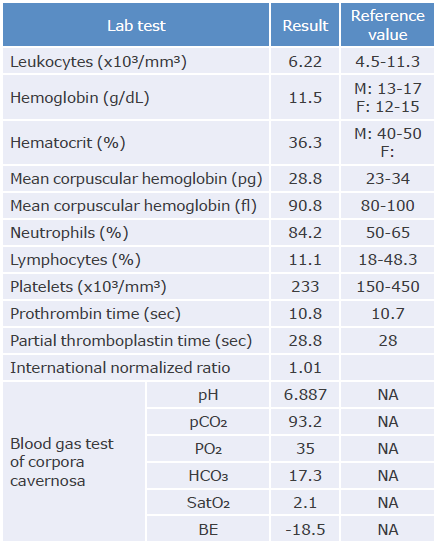
The urology department assessed the patient two hours after admission and corroborated the findings described above. Blood count and clotting time tests were performed, finding mild anemia, moderate lymphopenia (690/mm3), and normal prothrombin and thromboplastin times. Arterial blood gas test of the corpora cavernosa reported hypoxemia, hypercapnia, and acidosis (Table 1). D-dimer, LDH, and ferritin were not measured as this was a case of mild COVID-19.
Based on the clinical history, physical examination and laboratory test results, ischemic priapism was diagnosed. Corpora cavernosa drainage was performed and two intracavernous injections of epinephrine solution were administered, each with a dose of 2mL of 1/100 000, given five minutes apart. Pain and penile erection resolved within 24 hours of starting treatment, and the patient was advised to apply ice to the affected area. The urology department considered that priapism could have been related to dialysis treatment and postulated SARS-CoV-2 infection as an additional risk factor due to the association between COVID-19, coagulopathy, and thrombosis.
Discussion
Priapism is a disease that can be caused by multiple factors and is uncommon in dialysis patients. The present article reports on a male patient who consulted due to a 30-hour penile erection. He had a history of CKD that was treated with renal replacement therapy and prazosin (factors related to the development of priapism). He also had a confirmed diagnosis of SARS-CoV-2 infection, which increases the risk of thrombosis and may facilitate priapism physiopathologically.
There are several mechanisms that explain the association of kidney disease and dialysis with priapism. However, it is not possible to establish causality since there are no tests that could be used in clinical practice to make an accurate diagnosis.4,8,9
One of the risk factors for priapism associated with dialysis therapy is hemoconcentration by ultrafiltration.4,8 Although it is not easy to predict, the reported patient had an average interdialytic weight gain of 4% (within the expected range), he did not exceed this value in the period immediately before the erection and had not presented intradialytic hypotension or symptoms that could suggest excess ultrafiltration. Therefore, this aspect did not influence the onset of priapism.
According to some authors, erythropoietin affects the endothelium and influences the coagulation cascade, favoring platelet aggregation and inhibition of fibrinolysis.10-12 It also plays an important role in the endocrine system as it is associated with improved sexual function of men on dialysis and raising the testosterone and sex hormone-binding globulin levels.8,13 However, it is not clear whether this endocrine effect has something to do with the development of priapism or whether it may favor its onset because of the effect it causes on hemoconcentration and thrombosis. It should be noted that it was one of the medications the patient received for treating his anemia.
It should be noted that in this case, the patient was receiving prazosin, an antihypertensive drug that has been associated with the development of priapism due to the blocking effect of alpha-adrenergic receptors. There are several cases reported in the medical literature that support this association.1,14,15
Although heparin is an anticoagulant that has been shown to cause a rebound effect increasing the risk of thrombosis.16 17 It is widely used during hemodialysis to prevent coagulation of the extracorporeal circuit; however, its effect on the pathophysiology of priapism has yet to be verified.
In hemodialysis, contact of blood components with the membrane and extracorporeal circuit generates additional stress that facilitates the activation of the coagulation cascade, fibrinolysis, and platelet aggregation. This may also favor the formation of thrombi and the storage of fibrin degradation products in corpora cavernosa.8
So far, several conditions that could predispose dialysis patients to develop priapism have been described. Nevertheless, in this case, there was an additional condition unrelated to dialysis or kidney disease, which was SARS-CoV-2 infection. Two cases of COVID-19 patients with priapism have been reported in the literature,18,19 but they were patients with severe symptoms, multiple organ involvement, and no evidence of additional thromboembolic disease.
Similarly, venous thromboembolism has been reported as a complication of patients with COVID-19, especially in severe cases,5 because inflammation plays an important role in the development of thrombosis. Furthermore, high levels of interleukin-6, interleukin-1β, interferon-ү, monocyte chemoattractant protein-1 and other inflammatory cytokines that alter endothelial function and integrity are present in this type of patients, thus favoring the release of von Willebrand factor, the expression of adhesion molecules, and platelet and leukocyte recruitment.
On the other hand, hypoxia induces the activation of transcription factors that favor the expression of endothelial tissue factor, which, added to the downregulation of natural anticoagulants such as protein C and tissue factor inhibitor, generates a prothrombotic endothelial phenotype. It has also been established that complement activation and the generation of antiphospholipid antibodies are involved in the pathophysiology of COVID-19 thrombosis.5,20-22
It should be noted that patients with COVID-19 may have comorbidities or risk factors specific to the development of thrombosis, such as kidney disease, malignancy, lung disease, genetic factors, immobility, among others, which, added to the inflammatory state and endothelial injury described above, could facilitate thrombosis.20
Although priapism is not a frequent complication in patients with COVID-19,23 it is believed that obstruction of corpora cavernosa drainage venules may be secondary to coagulopathy and possible microemboli secondary to infection.18,19
Conclusions
At the time of writing this case report, there is no information available on cases of priapism in patients with mild manifestations of COVID-19, and it is not clear how the risk of thrombosis should be assessed in this group of patients. From a pathophysiological point of view, factors related to dialysis and kidney disease may have predisposed this patient to priapism, although it is not clear what role SARS-CoV-2 infection may have played in the development of this condition. Therefore, further studies are needed to confirm or rule out the association between COVID-19 and priapism in dialysis patients.