Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Colombian Journal of Anestesiology
Print version ISSN 0120-3347
Rev. colomb. anestesiol. vol.37 no.4 Bogotá Oct./Dec. 2009
ESSAY
Practical Application of Nomograms of Remifentanil and Propofol
Aplicación práctica de los nomogramas de remifentanil y propofol
Luis Alberto Tafur B.*, Eduardo Lema Flórez**
* Médico anestesiólogo, Universidad del Valle, H.U.V. Clínica Visual y Auditiva, Instituto para Niños Ciegos y Sordos
del Valle del Cauca. E-mail: Tafur05@hotmail.com.
** Médico anestesiólogo, Universidad del Valle, H.U.V. Clínica Visual y Auditiva, Instituto para Niños Ciegos y Sordos
del Valle del Cauca. Docente Departamento de Anestesiología, Universidad del Valle. E-mail: lemaflorez@gmail.com
Recibido: Abril 11/2009 Aceptado: Diciembre 11/ 2009
SUMMARY
Nomograms are tools that allow the administration of medicines pharmacokinetically. The value of these nomograms has already been published in the Colombian Journal of Anesthesiology (RCA), which requires a practical approximation in the way these concepts should be used- efficiently and with confidence. In the present article the utilization of the nomograms are presented didactically via examples which permit the reader to assess her or his grade of comprehension and dispel doubts about the application of the pharmacokinetic concepts for remifentanil and propofol.
Key Words: Nomograms, pharmacokinetics, practical examples, propofol, remifentanil .Source: MeSH, NLM.
RESUMEN
Los nomogramas son una herramienta que permite la administración de medicamentos de una manera farmacocinética. La validación de dichos nomogramas ha sido publicada con anterioridad en la Revista Colombiana de Anestesiología, por lo cual se hace necesaria una aproximación práctica a la forma de utilizar estos conceptos de una manera eficiente y segura. En el presente trabajo se presenta la utilización de los nomogramas de una forma didáctica, a manera de ejemplos que permiten al lector confrontar su grado de comprensión y despejar dudas sobre la aplicación de los conceptos farmacocinéticos para el remifentanil y el propofol.
Palabras clave: nomogramas, farmacocinética, utilización, propofol, remifentanil. (Fuente: DeCS, BIREME)
Nomograms are a practical option for estimating the plasmatic (CP) concentration of a medicine and thus be able to administer it pharmacokinetically. (1). To be able to estimate and achieve the desired CP in a patient helps in the administration of a safer and more predictable anesthetic with fewer adverse effects (2-4).
1. Understanding nomograms
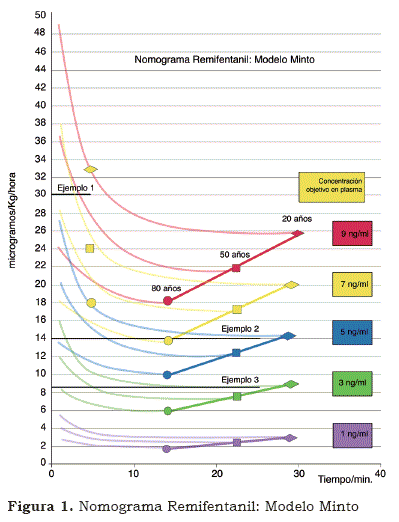
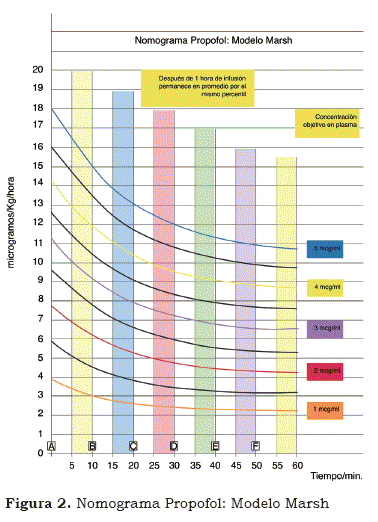
Nomograms have four variables: the first, in the axis of the X, corresponds to the time in minutes of the infusion of the medicine. The second, in the axis of the Y, represents the rate of infusion en mg/Kg/hour for propofol, and in mcg/Kg/hour for remifentanil. Administration in hours and not in minutes aids a rapid calculation, given that the infusion pumps for the most part are programmed in ml/hour. The curved lines represent the plasmatic concentrations (see figure 1 and 2).
For the remifentanil nomogram the straight lines represent concentration according to age. In the inferior extreme, are the 80-year-old patients, and in the superior, the 20-year-olds. The proportional division of these lines allows the placement of different ages. As such, the middle point represents patients of 50 years of age.
2. Remifentanil nomogram
The following step consists of establishing which is the desired CP according to the procedure. According to different studies, these are (5-6):
CP Intubation* = 7 - 8 ng/ml
CP Thorax surgery* = 6 -7 ng/ml
CP Abdominal surgery* = 5 - 6 ng/ml
CP Bland tissues* = 3.5 - 4 ng/ml
CP De-tubing* = 3 - 3.5 ng/ml
CP Sedation = 2 - 3 ng/ml
*Plasmatic concentrations combined with a hypnotic.
The following are some examples regarding the way to utilize nomograms during anesthesia. The method of preparing remifentanil is a choice for each anesthesiologist, keeping in mind that upon utilizing high concentrations the quantity of remifentanil per ml that is found stored in extension is a risk factor for the patient who goes into recuperation. In the examples 2 mg of remifentanil diluted in 500 ml of SSN (4 mcg/ml) are utilized.
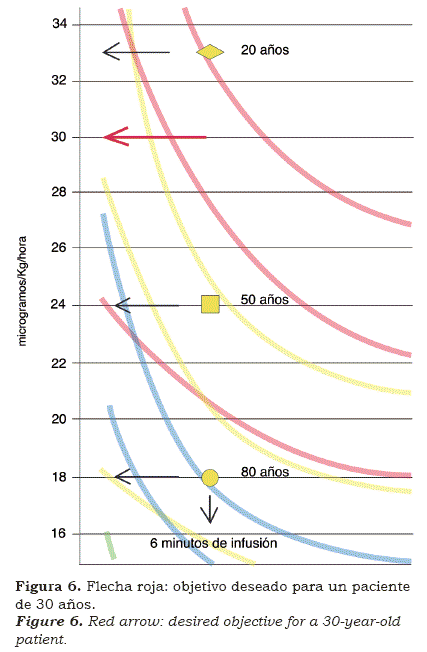
Example 1 (see figure 1). In the case of a patient 30 years old weighing 70 kilograms, which remifentanil infusion would be appropriate to achieve an objective of 7 to 8 ng/ml in plasma for the intubation?
Observing the remifentanil nomogram (see figures 1), the rhombus (20 years), the square (50 years) and the circle (80 years)- yellow- found on the thread, represent the plasmatic concentration between 7 and 8 ng/ml after six minutes’ infusion. As such, between the extremes of 20 and 80 years the different ages can be placed. Every time there is a patient 30 years old, she or he will need an infusion of 30 mcg/K/hour in six minutes in order to achieve the desired objective (see figures 6, red arrow).
30 (mcg/kg/hour) x 70 kg = 2100 mcg/hour
Since the concentration for this example is 4 mcg/ml:
(2100 mcg/hour) / (4 mcg/ml) = 525 ml/hour
The first rate of infusion is adjusted to 525 ml/hour in order to infuse 52 ml. Where do these 52 ml come from? Since the infusion should take six minutes, and this span of time is 10% of 60 minutes (1 hour), then:
525 ml/hour x 10% hour = 52 ml.
Therefore, each time the rate of infusion for intubation in 6 minutes is calculated, one divides the rate of infusion per hour based on 10 and one gets the volume to infuse.
Extrapolating the data of the nomogram one observes that the intubation doses in six minutes for the different ages are the following:
20 years - 33 mcg/Kg/h
30 years - 30 mcg/Kg/h
40 years - 27 mcg/kg/h
50 years - 24 mcg/kg/h
60 years - 22 mcg/kg/h
70 years - 20 mcg/kg/h
80 years - 18 mcg kg/h
Example 2. For the same patient readied for a laparoscopic cholecystectomy (abdominal surgery), what is the rate of infusion necessary to maintain a CP of 5 ng/ml?
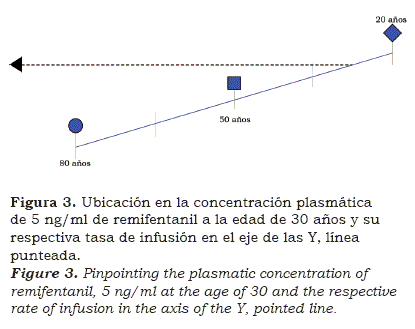
In the remifentanil nomogram (see figure 1), the straight lines represent the desired CP: violet line 1 ng/ml; green line 3 ng/ml; blue line 5 ng/ml; yellow line 7 ng/ml, and red line 9ng/ml. The CP of 2, 4, 6 and 8 ng/ml would be represented by a straight line equidistant between the superior and inferior CP. For the example, one must choose the blue line (5 ng/ml). On this line the patient’s age is graphed (see figure 3) and the rate of infusion per hour that corresponds to the axis in the Y is chosen; in this case, 14 mcg/kg/hour.
(14 mcg/Kg/hour) x 70 Kg = 980 mcg/hour. Since the concentration of remifentanil is 4 mcg/ml, then:
(980 mcg/hour) / (4 mcg/ml) = 245 ml/hour.
The infusión pump should be programed to 245 ml/hour to achieve a CP approximately 5 ng/ml.
Example 3. For the same case and at the moment of de-tubing the patient with the least incidence of cough possible, a CP between 3 and 3.5 ng/ml of remifentanil and a MAC between 0.1 and 0.2 of any halogenated or CP of propofol approximately 1.5 mcg/ml are required. What is the per hour rate of infusion of remifentanil required in order to maintain the desired CP?
For this CP the green line (3ng/ml) is placed according to the patient’s age, resulting in a rate of infusion per hour that corresponds to the axis of the (Y), being 8.5 mcg/kg/hour (figura 4). Keeping in mind the effectiveness according to the context of remifentanil, this infusion must be adjusted approximately 10 minutes before awakening.
(8.5 mcg/Kg/hour) x 70 Kg = 595 mcg/hour.
Since the concentration of remifentanil for this example is 4 mcg/ml, then:
(595 mcg/hour) / 4 mcg/ml = 149 ml/hour.
The rate of infusión of the pump is 149ml/ hour in order to de-tube the patient with the least incidence of cough.
3. Propofol nomogram
Therefore, as it is necessary to know what remifentanil CP is required in accordance with the moment of surgery and the type of intervention, it is also imperative to know which propofol CP is adequate:
CP Intubation* = 2.5 - 3.5 mcg/ml
CP Maintenance* = 1.8 - 2.5 mcg/ml
CP De-tubing* = 1 - 1.7 mcg/ml
CP Sedation = 1.5 - 2 mcg/ml
*Plasmatic concentrations combined with an opioid.
In contrast to remifentanil, which has T ½ Ke0 small (1.4 min.), propofol does not share this benefit (T ½ Ke0 = 2.8 min), which causes the amount of time to achieve a stable medicated state among the different compartments to be greater. As such, if the desire is to maintain a specific CP with the help of nomogram, the changes in the rate of infusion must be effected approximately every 10 minutes (see figure 2).
Example 4. Forty-year-old patient weighing 60 Kg who requires a propofol infusion in order to maintain a CP of 3 mcg/ml. What is the rate of infusion? The first step in determining this rate is to look at the curve in the nomogram with a plasmatic concentration of 3 mcg/ml, whose color is violet (see figure 6).
Observing the beginning of the curve in the axis of the Y, one sees that the rate of infusion with which one should start is approximately 11 mg/ Kg/hour (point A in the figure).
If the propofol is prepared with a dilution of 2 mg/ ml. (1 tube of propofol of 20 ml + 80 cc of SSN):
60 Kilograms x 11 mg/Kg/hour = 660 mg/hour.
(660 mg /hour) / (2 mg/ml) = 330 ml/hour.
As such, the infusion is started at 330 ml/hour.
As the constant of the Ke0 of the propofol is not so fast, the state of stabilization will not be so fast. As such, the next change in the rate of infusion will be in 10 minutes or, rather, in point B. Observing the axis of the Y, the rate of infusion that corresponds to this point is approximately 9 mg/ Kg/hour.
60 Kg x 9 mg/Kg/hour = 540 mg/hour
(540 mg/hour) / (2 mg/ml) = 270 ml/hour.
As a result, the new rate of infusión after 10 minutes is 270 ml/hour.
Afterwards the infusion rate changes every 10 minutes, which corresponds to points C, D, E and F.
Unfortunately this type of infusion is not practical inasmuch as 10 minutes are needed in order to achieve the desired concentration, which is the reason that when managing propofol, a dose of rapid infusion of 2 mg/Kg is preferable, omitting points A and B and directly initiating the infusion at point C, a move which avoids 20 minutes of infusion.
Example 5. Returning to the case of the 40-yearold patient weighing 60 Kg who needs intubing after a dose of opioid, what would the rate of infusión be in order to maintain a CP of 2 mcg/ml of propofol?
The first thing is to pinpoint on the nomogram the curve of the desired plasmatic CP, which is the red curved line (2 mcg/ml).
Next, a dose of 2 mg/kg of propofol is applied in a rapid infusion. With this dose a plasmatic peak of 10 mcg/ml is achieved in one minute, and in three minutes a peak at the effect site of 3 mcg/ml.
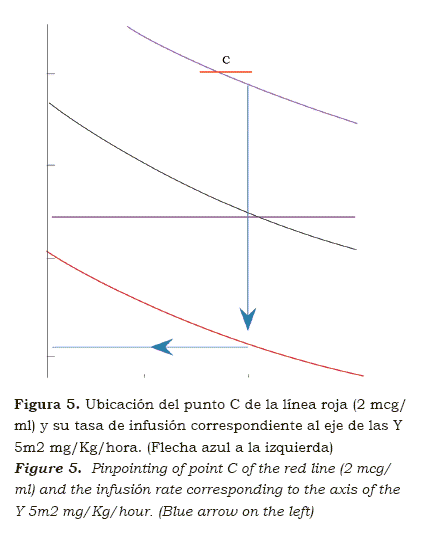
Immediately after finalizing the dose of 2 mg/kg the infusion is initiated. For this, one pinpoints the red line located on the nomogram. As one now has a loading dose with which 20 minutes of infusion were avoided, the infusion in point C is initiated as if 20 minutes of infusion had passed (red line, 2 mcg/ml; see figure 5). The infusion that corresponds to the axis of the Y is approximately 5.2 mg/Kg/hour). First step: dose of 2 mg/Kg.
60 Kg x 2 mg/Kg = 120 mg of propofol via rapid infusion.
Second step: infusion at 5.2 mg/Kg/hour.
5.2 mg/kg/hour x 60 kg = 312 mg/hour
As the dilution is 2 mg/ml, one gets the following:
(312 mg/hour) / (2 mg/ml) = 156 ml/hour.
After the infusión dose, the pump is adjusted so it will surpass 156 ml/hour.
Ten minutes after the initiation of the infusion, one moves to point D on the red line (2 mcg/ml), and observes at the axis of the Y that the rate of infusion corresponding to this point is approximately 4.8 mg/Kg/hour (144 ml/hour). Similarly, one proceeds to points E and F on the red line (2 mcg/ml). Via this technique one achieves the intubation dose and maintains the desired concentration.
Example 6. A 40-year-old patient weighing 60 Kg has maintained a CP of propofol of approximately 2 mcg/ml and a CP of remifentanil of 5 ng/ml. It is now time to terminate the anesthesia for which one adjusts the remifentanil infusion to achieve a CP of 3 ng/ml. As mentioned earlier, now a CP of approximately 1.5 mcg/ml of propofol is required to de-tube with a minimum of cough.
The first thing is to locate on the nomogram the CP of 1.5 mcg/ml, which corresponds to the black curve found between the orange curve (1 mcg/ml) and the red curve (2 mcg/ml).
In order to achieve this concentration one takes point F directly from the black line (1.5 mcg/ml) (see figure 2). Taking the rate of infusion that corresponds to this point in the axis of the Y, one observes that it is approximately 3.1 mg/Kg/hour. As as result, one adjusts the infusion at 93 ml/hour 10 minutes before detubation.
The use of these nomograms allows having an orientation concerning how to obtain the desired plasmatic concentration, administering anesthesia in more precise quantities and in accord with the moment and characteristics of the surgery. The usefulness of these nomograms lies in the fact that they are reliable instruments and 100% accessible to the community of anesthesiologists. The administration of medications via the use of these nomograms is not for children or for obese patients.
REFERENCIAS
1. Tafur LA, Gómez JM, Parra LE. Validación de nomogramas de remifentanil y propofol para la administración de anestesia total endovenosa. Rev. Col. Anest. 2009; 37:21-8.
2. Ausems ME, Vuyk J, Hug CC Jr, Stanski DR. Comparison of a computer-assisted infusion versus intermittent bolus administration of alfentanil as a supplement to nitrous oxide for lower abdominal surgery. Anesthesiology. 1988;68(6):851-61.
3. Russell D, Wilkes MP, Hunter SC, Glen JB, Hutton P, Kenny GN. Manual compared with target-controlled infusion of propofol. British Journal of Anaesthesia 1995; 75:562-6.
4. Engbers FHM. Target controlled infusion in practice. European Journal of Anesthesiology.1995; 12 (Suppl. 10):88-90.
5. Troy AM, Huthinson RC, Easy WR, Kenney GN. Tracheal intubating conditions using propofol and remifentanil target-controlled infusions. Anaesthesia. 2002;57(12):1204-7.
6. Lee B, Lee JR, Na S. Targeting smooth emergence: the effect site concentration of remifentanil for preventing cough during emergence during propofolremifentanil anaesthesia for thyroid surgery. Br J Anaesth. 2009;102(6):775-8.
1. Tafur LA, Gómez JM, Parra LE. Validación de nomogramas de remifentanil y propofol para la administración de anestesia total endovenosa. Rev. colomb. anestesiol. 2009; 37:21-8. [ Links ]
2. Ausems ME, Vuyk J, Hug CC Jr, Stanski DR. Comparison of a computer-assisted infusion versus intermittent bolus administration of alfentanil as a supplement to nitrous oxide for lower abdominal surgery. Anesthesiology. 1988;68(6):851-61. [ Links ]
3. Russell D, Wilkes MP, Hunter SC, Glen JB, Hutton P, Kenny GN. Manual compared with target-controlled infusion of propofol. British Journal of Anaesthesia 1995; 75:562-6. [ Links ]
4. Engbers FHM. Target controlled infusion in practice. European Journal of Anesthesiology.1995; 12 (Suppl. 10):88-90. [ Links ]
5. Troy AM, Huthinson RC, Easy WR, Kenney GN. Tracheal intubating conditions using propofol and remifentanil target-controlled infusions. Anaesthesia. 2002;57(12):1204-7. [ Links ]
6. Lee B, Lee JR, Na S. Targeting smooth emergence: the effect site concentration of remifentanil for preventing cough during emergence during propofolremifentanil anaesthesia for thyroid surgery. Br J Anaesth. 2009;102(6):775-8. [ Links ]











 text in
text in