Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em
SciELO
Similares em
SciELO -
 Similares em Google
Similares em Google
Compartilhar
Colombian Journal of Anestesiology
versão impressa ISSN 0120-3347
Rev. colomb. anestesiol. v.38 n.1 Bogotá jan./mar. 2010
Multi-injection vs. single injection technique with localization of the medial nerve for infraclavicular block for upper limb surgery
Reinaldo Grueso Angulo*, Alejandra Sanín Hoyos**, Antonio J. Bonilla Ramírez**, Andrés García Carreño*** y Javier Cubillos Salcedo***.
* Departamento de Anestesiología. Hospital Universitario San Ignacio.
Profesor asistente, Facultad de Medicina Pontificia Universidad Javeriana. E-mail:
rgrueso@javeriana.edu.co
** Anestesióloga/o Hospital Universitario de San Ignacio, Profesor(a)
Instructor(a), Facultad de Medicina, Pontificia Universidad Javeriana, Bogotá.
*** Anestesiólogo Hospital Universitario de San Ignacio, Bogotá.
Recibido: enero 27 de 2010. Enviado para modificaciones: febrero 9 de 2010. Aceptado: febrero 16 de 2010.
ABSTRACT
Introduction. The purpose of this, randomized, controlled, observer-blind clinical trial, was to compare the efficacy of the neurostimulator-guided infraclavicular block of the brachial plexus, using two different techniques: multiple injection with localization of three different cords and the single injection technique with localization of the medial cord.
Methods. Two hundred and sixty (260) patients scheduled for upper limb surgery under Regional anesthesia were randomly distributed into two groups: multiple injection (MI) (129) or single injection (SI) (128). The primary outcome assessed was the efficacy of the block, meaning the absence of sedation beyond some established margins or the need to administer general anesthesia. Other outcomes measured were patient satisfaction and the presence of side effects.
Results. Both groups had comparable baseline characteristics. The time for administering the block was 9,6 minutes (±5,9) for SI vs. 10,4 minutes (±3,8) for MI, which was not clinically different. The primary outcome showed 7 failures in 129 MI patients (5,43 %) and 27 (21,09 %) of the SI 128 patients studied. This difference between the two techniques results in a RR of 3,89 with a CI (1,76 - 8,6) and p< 0,0002.
Conclusions. In a significant sample of patients and within a controlled environment, the effectiveness of the brachial plexus block using the conventional multiple injections technique with peripheral nerve stimulator was superior to stimulator-guided peripheral nerve single injection technique with localization of the medial cord.
Key words: Regional anesthesia, nerve block, infraclavicular block, brachial plexus (Source: MesH, NLM)
INTRODUCTION
During the last few decades, surgery has focused on managing patients on an ambulatory basis. This has led to the improvement of anesthetic techniques that promote fast recovery times for the patient with minimum side effects. At the level of the infraclavicular space, the brachial plexus is divided into three cords that are closely related to the subclavian vessels, organized in a compact arrangement and at very short distances from one another; so, upon injecting a particular volume of local anesthesia, the anesthetic agent spreads out evenly (1,2,3,4,5).
The medial cord that originates at the medial nerve is the most centrally localized nerve within the vascular-nerve bundle. Therefore, the local anesthetic solution is more evenly distributed to the other two cords (lateral and posterior) when the injection is administered upon eliciting the response to the medial cord stimulus than if the injection is administered after eliciting the response to the stimulus of the lateral cord which originates at the musculocutaneous nerve and is more superficially localized and further away from the rest. It is also known that in some cases this nerve may leave the vascular nerve bundle before the infraclavicular region, which may lead to injecting the anesthetic solution outside the nerve bundle (1,2,3,6).
There are several studies comparing multiple vs. single injection techniques. The success rates in these trials are controversial and no valid conclusions can be derived because some deficiencies have been identified in terms of their research design and the analyses of the data (7,8,9,10,11,12). Moreover, in the single injection groups, the anesthetic agent is administered upon eliciting the first motor response but this response is not medial nerve specific; furthermore, the use of a standard technique for all patients is not reported (5,6,13).
The purpose of this study is to show with a clinical trial that in patients scheduled for upper limb surgery the success rate of the stimulator-guided peripheral nerve infraclavicular block single injection technique, targeting the medial nerve, is similar in effectiveness to the success rate of the more commonly used multiple injection technique.
METHODS
Patients for this randomized, controlled clinical trial were recruited at the San Ignacio University Hospital from October 2005 to November 2007. The patients were eligible if they were going to undergo unilateral orthopedic surgery of the upper limb, the estimated surgical time exceeded thirty minutes, if they were classified as ASA I, II or III and were over 18 years old. The ethics committee of the San Ignacio University Hospital approved the study protocol and all the participants submitted their informed consent in writing.
Patients with any of the following were excluded: any contraindication for Regional anesthesia (i.e.: injection site infection or anticoagulation; history of alcohol abuse or psychoactive drugs; peripheral neuropathy or brachial plexus injury in the opposite side; patients allergic to any of the study drugs; patients who were mentally disabled to respond to the questions and patients who rejected the Regional anesthesia technique.
Procedures
Upon signing the informed consent, the patients were randomly assigned to an intervention group using sealed opaque envelopes.
Non-invasive arterial blood pressure monitoring was used, in addition to continuous EKG recordings and pulse oximetry. A peripheral vein was catheterized with an 18 or 20-gauge catheter and patients received oxygen supplementation through a nasal tube at a rate of 2 L/min. Midazolam 0,03 mg/k was used for sedation.
Patients who were assigned to group 1 (Multiple Injections-MI) received a puncture with an insulated 50 mm needle (stimuplex® Braun), that was connected to a peripheral nerve stimulator programmed for an initial outflow current of 1,0 mA for 0,1 sec. The needle was advanced until the first medial nerve response was elicited (finger flexion and forearm pronation); then the stimulator outflow was cut down to 0,5 mA but if persistent movement continued, the first injection was administered. Then the stimulator power was raised up to 5,0 mA and the needle was mobilized until other hand movements were localized, identifying the radial nerve, the ulnar nerve or the muscolocutaneous nerve and a new injection was administered. This procedure was repeated one more time. So, the local anesthetic agent was injected with three different movements in total: the first was always the medial nerve and then two other different movements to mark the location of a brachial plexus nerve. A total volume of 40 cc of anesthetic solution was injected.
In group 2 (Single Injection-SI) the medial nerve was localized (finger flexion and forearm pronation) with an outflow current between 0,4 - 0,5 mA, and 40 cc of anesthetic solution were injected.
A clinical evaluation was performed after the block to determine the success or failure of the technique. The regional anesthetic technique was considered a failure if the patient met one or more of following criteria: intolerance to the surgical incision, tourniquet intolerance; additional infiltration of local anesthetic or required additional Fentanyl exceeding 1,5 mcg/k during the trans-operatory.
Post-operatory
At the end of the surgical procedure patients were transferred to the post-anesthesia recovery room (recovery phase II) and were discharged or moved to their room upon meeting the criteria for discharge.
The primary outcome assessed was success of the infraclavicular block technique and a comparison was made of the multiple-injection vs. the single-injection technique around the medial nerve area.
Other demographic variables were recorded such as age, gender, weight and size; the frequency of short and long-term side effects was described and finally a patient satisfaction survey was administered at the time of discharge from the recovery room, using a verbal scale with which the patient rated the technique as excellent, good, fair or poor. No additional questionnaires had to be answered.
STATISTICAL ANALYSIS
The primary efficacy outcome (successful block) was analyzed with an intention-to-treat approach. The estimated sample size was 260 patients to achieve 80 % power and to detect significant differences between the two groups with a 0,05 one-tailed p-value. The size of the sample was based on a 95 % success rate for the control group and 85 % for the experimental group. The analysis was based on a hypothetical test for the difference between two proportions of the two populations. No sub-group analyses were done.
The data for categorical variables were presented as incidence rates. The continuous variables were presented as ±SD averages.
RESULTS
260 patients were randomly included in the trial; 257 of them (98,8 %) were analyzed for final outcome. No information was made available for two patients assigned to the single injection group and 1 patient assigned to the multiple injection group was excluded because the surgery was cancelled (See figure 1).
Patients´ Characteristics
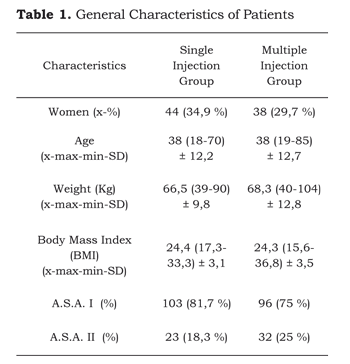
As shown in Table 1, the overall characteristics of the two groups of patients are similar. There was a minor difference in the ASA classification due to a larger number of patients classified as ASA II in the multiple injection group.
With regards to the average time for administering the block, no relevant differences were found between the two groups: 9,6 minutes (±5,9) in the single injection group and 10,4 minutes (±3,8) in the multiple injection group.
In terms of the primary outcome - defined as a successful block - there were 7 failures in 129 patients (5,43 %) in the multiple injection technique group while in the single injection group there were 27 failures in 128 patients studied (21,09 %). The difference between both techniques results in an RR value of 3,89 and a CI (1,76 - 8,6) with p< 0,0002.
It should be noted that of the patients considered a failure of the anesthetic technique, 3 (43 %) of the 7 patients in the multiple injection (MI) group required general anesthesia and in the single injection (SI) group, 11 of the 27 patients (41 %) required general anesthesia for their surgery. Most of the other patients required local anesthetic infiltration.
With regards to side effects, the descriptive analysis of outcomes provided information on 124 patients in the single injection group. 23 patients exhibited one side effect and three patients exhibited 2 side effects. In the multiple injection group, information was available from 126 patients, of which 26 showed one side effect while 2 patients showed 2 side effects. The most frequent side effect in both groups was vascular puncture, followed by incomplete Horner´s Syndrome; there was just one case of hematoma reported in the single injection group. There were no reports of pneumothorax among the patients participating in the trial.
In terms of patients´ satisfaction with the anesthetic technique, the following data were collected: 66,7 % rated the multiple injection (MI) technique as "excellent"; 27,9 % "good". 58,6 % of the single injection (SI) group said the technique was "excellent", while 30,5 % said it was "good". In general, the upper limb Regional anesthesia was well accepted and considered an adequate technique; around 90 % of the patients said they would be willing to go through that experience again.
DISCUSSION
The results of the trial were analyzed on a significant number of patients. It showed the superior efficacy of the brachial plexus block with the multiple injection technique, using the peripheral nerve stimulator to localize the three cords, as compared to the guided medial cord localization single injection technique.
The success rate in the multiple injection group was 95 % (122/129) while in the single injection group was 79 % (101/128). This success rate with peripheral Regional anesthesia for upper limb block is comparable to the results achieved at other institutions where regional peripheral anesthesia is a usual technique. This makes the results of this trial applicable in this type of scenarios.
The single injection technique showed a 3,88 times higher risk for anesthetic failure. The need for a protocol to define failure criteria should then be emphasized. A fentanyl dose above 1,5 mcg/k or the need for additional infiltration with local anesthetic agent at the surgical site, were considered failures according to this particular protocol.
Only 43 % (3/7) of the failures in the multiple injection group required general anesthesia to do the surgery, while in the single injection group the percentage was 41 % (11/27). We know that in clinical practice, regional peripheral anesthesia is usually accompanied by higher doses of sedatives to achieve deeper levels and this reduces the need for general anesthesia. For this reason we felt that by avoiding deep sedation levels, this trial allows for a realistic assessment of the effectiveness of Regional anesthesia for surgical procedures in both groups.
In terms of the secondary outcomes observed in this trial, there were no differences in the time of administration of the block since the average for both groups was 10 minutes. We feel that this is an efficient time for the onset of anesthesia, comparable to the induction time in general anesthesia. On the other hand, the localization of the medial cord stimulus for the single injection technique can be difficult in some cases and this is why the average time was similar to the multiple injection technique.
In most cases, patient satisfaction using both techniques was rated as excellent of good in around 90 % of the cases in both groups. While this was not the primary outcome, it is indeed interesting information about the acceptance of the technique by patients and should be considered an important driver for those groups of anesthesiologists who are increasing using the regional peripheral anesthetic techniques.
Despite the fact that the study limited the number of operators to a minimum, one of the disadvantages of this type of trials is the inter-individual variability when administering the block that could bias the results. However, this is an uncontrolled patient randomization factor.
The side effects identified in the trial are the same side effects most frequently reported in the literature, which are uncomplicated and manageable. The frequency of these side effects was similar for both groups and the average was around 20 %. The higher proportion of vascular punctures in the multiple injection group may be explained by the anatomic proximity of the brachial plexus to the vascular structures in the infraclavicular region and by the direction of the needle to localize the various cords. An interesting finding seldom reported in the literature was the presence of cervical sympathetic block in both groups; this responds to the proximal dissemination of the anesthetic agent and was more frequent in the single injection group. Probably this is due to the fact that the volume of the anesthetic solution is injected at one single compartment and hence may develop a higher pressure and facilitate its cephalic dissemination.
On the basis of our results we recommend the use of the multiple injection technique; however, the success rate in both groups should be noted, particularly taking into account the small number of patients that required general anesthesia in both groups (2,3 % of the multiple injection group and 8,5 % of the single injection group).
In our opinion this trial followed high methodological standards and this leads to the assumption that its results are reliable and can be used in the practice of regional peripheral anesthesia.
REFERENCES
1. Gerancher JC., Upper extremity nerve blocks. Anesthesiology Clinics of North America. 2000; 14 (2): 297-319.
2. Hadzic A, Vloka JD., Infraclavicular brachial plexus block, en Peripheral nerve blocks. McGraw-Hill, New York; 2004. Páginas 131-140.
3. Raj PP., Montgomery SJ., nettles d et al. Infraclavicular brachial plexus block : a new approach. Anest Analg 1973; 52: 897-904.
4. Rodriguez J., Bárcena M., Restricted infraclavicular distribution of the local anesthetic solution after Infraclavicular brachial plexus block. Regional anesthesia and Pain Medicine. 2003; 28 (1): 33-36.
5. Wilson JL., Brown DL., Wong GY., et al. Infraclavicular braquial plexus block: parasagital anatomy important to the coracoide technique. Anesth Analg 1998; 87: 870-3.
6. Sandhu N., Capan L., Ultrasound-guided Infraclavicular brachial plexus block. Br J Aneaesth, 2002; 89: 254-9.
7. Borgeat A., Ekatodramis G., dumont ch. An evaluation of the infraclavicular block via a modified approach of the Raj technique. Anesth Analg 2001; 93: 436-441.
8. Gaertner E., Estebe J.P., Infraclavicular plexus Block: Multiple injection versus single injection.Regional anesthesia and Pain Medicine.2002; 27,(6): 590-594.
9. Rodriguez J, Bárcena M. A Comparison Of Single versus Multiple Injections on the extent of Anesthesia witn Coracoid Infraclavicular brachial plexus Block. Anesth Analg 2004; 99: 1225-30.
10. Rodriguez J., Taboada-Muñiz M . Median Versus Musculocutaneous Nerve Response with Single-Injection Infraclavicular Coracoid Block. Regional anesthesia and Pain Medicine, 2004; Vol 29, No 6 (November-December),: 534-538.
11. Rodriguez J., Bárcenas M., Increased Success Rate with Infraclavicular Brachia Plexus Block Using a Dual Injection Technique. Journal of Clinical Anesthesia , 2004; 16: 251-256.
12. Wiffler K.,. Coracoid block: a safe and easy technique. Br J Anaesth 1981: 53: 845-48.
13. Rodriguez J., Bárcenas M., Infraclavicular brachial plexus Block Effects on respiratory function and extent of the block. Regional anesthesia and Pain Medicine 1998; 23(6): 564-568.
1. Gerancher JC., Upper extremity nerve blocks. Anesthesiology Clinics of North America. 2000; 14 (2): 297-319. [ Links ]
2. Hadzic A, Vloka JD., Infraclavicular brachial plexus block, en Peripheral Nerve Blocks. McGraw-Hill, New York; 2004. Páginas 131-140. [ Links ]
3. Raj PP., Montgomery SJ., nettles d et al. Infraclavicular brachial plexus block : a new approach. Anest Analg 1973; 52: 897-904. [ Links ]
4. Rodriguez J., Bárcena M., Restricted infraclavicular distribution of the local anesthetic solution after Infraclavicular brachial plexus block. Regional Anesthesia and Pain Medicine. 2003; 28 (1): 33-36. [ Links ]
5. Wilson JL., Brown DL., Wong GY., et al. Infraclavicular braquial plexus block: parasagital anatomy important to the coracoide technique. Anesth Analg 1998; 87: 870-3. [ Links ]
6. Sandhu N., Capan L., Ultrasound-guided Infraclavicular brachial plexus block. Br J Aneaesth, 2002; 89: 254-9. [ Links ]
7. Borgeat A., Ekatodramis G., dumont ch. An evaluation of the infraclavicular block via a modified approach of the Raj technique. Anesth Analg 2001; 93: 436-441. [ Links ]
8. Gaertner E., Estebe J.P., Infraclavicular plexus Block: Multiple injection versus single injection.Regional Anesthesia and Pain Medicine.2002; 27,(6): 590-594. [ Links ]
9. Rodriguez J, Bárcena M. A Comparison Of Single versus Multiple Injections on the extent of Anesthesia witn Coracoid Infraclavicular Brachial Plexus Block. Anesth Analg 2004; 99: 1225-30. [ Links ]
10. Rodriguez J., Taboada-Muñiz M . Median Versus Musculocutaneous Nerve Response with Single-Injection Infraclavicular Coracoid Block. Regional Anesthesia and Pain Medicine, 2004; Vol 29, No 6 (November-December),: 534-538. [ Links ]
11. Rodriguez J., Bárcenas M., Increased Success Rate with Infraclavicular Brachia Plexus Block Using a Dual Injection Technique. Journal of Clinical Anesthesia , 2004; 16: 251-256. [ Links ]
12. Wiffler K.,. Coracoid block: a safe and easy technique. Br J Anaesth 1981: 53: 845-48. [ Links ]
13. Rodriguez J., Bárcenas M., Infraclavicular Brachial Plexus Block Effects on respiratory function and extent of the block. Regional Anesthesia and Pain Medicine 1998; 23(6): 564-568. [ Links ]











 texto em
texto em