Introduction
Placing the patient in prone position (PP) is necessary for a wide variety of surgical procedures,1) both elective as well as urgent. Airway management in this position is very challenging for the anaesthetist because it impairs the usual manoeuvres for intubation by direct laryngoscopy, thus increasing the risk of injury to the cervical spine and making ventilation difficult.2-5
Although there are a few studies and case reports on tracheal intubation in the prone position (TIPP) published in the literature, the technique has been poorly described. In our country, this approach was advocated in the 1960s as an alternative technique by a team of Bogotá anaesthetists under the leadership of doctor Fernando Flórez Burgos, although there are no publications to support this statement.
A 56 year-old male patient, 80kg, was admitted to the emergency service in PP with a 12 cm knife protruding from his left upper back (Fig. 1). On assessment, he was alert, haemodynamically stable and breathing spontaneously. He had left hypoesthesia below the C5 sensory level, although muscle strength and movements were preserved. He had last had food intake 6 h before sustaining the injury.
Computed axial tomography imaging studies (Fig. 2) were performed in PP. Pneumothorax was ruled out and the exact position of the knife blade was determined. The knife had entered the spinal canal between the left pedicle of the second thoracic vertebra (T2) and close to the posterior facet of the third thoracic vertebra (T3).

Source: authors.
Fig. 2 Computed tomography of the thorax showing the knife in proximity of the spinal cord.
Pre-anaesthesia assessment was within normal limits. Airway was normal (Mallampati II, mouth opening >3cm, thyromental distance >6.5 cm, sternomental distance >12.5 cm). Non-invasive monitoring was initiated on arrival at the operating room.
Given the impossibility to place the patient in supine position (SP) because of the wound type, TIPP under general anaesthesia (GA) was planned. No fibre optic bronchoscopy was available at the time so a laryngeal mask was prepared in case of intubation failure. The patient was pre-oxygenated with 100% oxygen in PP for 3min (Figs. 3 and 4).
Before intubation, lidocaine spray was instilled in the oropharynx in order to diminish airway reflexes and improve intubation conditions. Once immobilised, the patient was moved up and the table headrest was removed, maintaining manual alignment of the head and neck with the help of a second anaesthetist (Fig. 5).
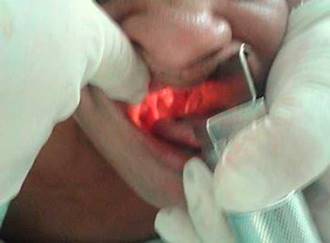
Intubation was performed by two anaesthetists. While the first held the head and neck to ensure alignment, the second, experienced in TIPP, stood on the left side of the patient and performed the intubation manoeuvre while holding the head. Opening the patient's mouth with the righthand, he performed laryngoscopy with his left hand. Because of the effect of gravity in PP, the mouth, the jaw and the tongue protrude, making laryngoscopy and vocal cord visualisation easier.
Anaesthesia induction was performed using propofol 1.8 mg/kg, fentanyl 3 mcg/kg and succinylcholine 1.25mg/kg. Adequate patient ventilation with the facial mask was confirmed. Then, the laryngoscope was introduced gently, keeping the head slightly extended and the jaw displaced downward (Fig. 6).
It was slightly challenging to hold the patient's head with the left arm, although intubation was successfully attained on the first attempt. Adequate ventilation was confirmed, and capnography confirmed the correct placement of the endotracheal tube (ETT).
The anaesthetist who performed the intubation was able to visualise the vocal cords promptly using a No. 3 Macintosh blade while holding the laryngoscope in his left hand and easily achieving tracheal intubation with a No. 8 ETT (Fig. 6).
Anaesthesia was maintained with sevoflurane at 0.8 MAC. Pressure ventilation of 10 mmHg at a 0.5 FiO2 and 5 mmHg positive end-expiratory pressure (PEEP) was used. Vecuronium 0.05 mg/kg IV was used for muscle relaxation. There were no complications during the course of the surgery. At the end of the procedure, the patient was placed in supine position, extubated and transferred to the post-anaesthetic care unit.
Discussion
Conventional anaesthetic management (including intubation) of patients taken to elective surgery in PP consists of standard GA induction, tracheal intubation in SP, followed by placement in PP.6
TIPP has been used only in trauma patients5,7-9) because ventilation is challenging in this position and there is a possibility of cervical and thoracic spine injury, although there are recent publications of the use of this technique in elective procedures with high success rates (98%) and few failed attempts (1.2%), making it a safe approach.10
Tracheal intubation may be performed equally well in PP as in SP, but it requires an anaesthetist with prior training in this technique. PP makes direct laryngoscopy intubation challenging due to the position of the patient's head on the surgical table. Displacing the head towards the upper end and removing the headrest makes it easier to access the airway. After GA induction in PP, the mouth and jaw protrude (fall) anteriorly, making laryngoscopy and intubation easier, although it may be slightly difficult to hold the head with the left arm and keep it aligned while performing intubation,7) thus requiring the help of a second anaesthetist.
Direct laryngoscopy (under general anaesthesia) in PP has been accomplished successfully, although it has been shown in other studies that laryngeal masks can also be used effectively.4
There are different strategies in the literature for airway management in PP, including the use of laryngeal mask, LM-Fastrach and LM CTrach, Proseal and videolaryngoscopy,3-16) and even different approaches to PP intubation (turning the head to one side, turning the patient al at once to a lateral position, and others in which the anaesthetist sits or kneels on the floor to perform the intubation manoeuvre with the patient in PP.7,10,16 In our case, this new "old" technique made it possible to access the airway on the first attempt.
Although PP is not the standard position in which to instrument the airway for direct laryngoscopy and endotracheal intubation under GA, our experience suggests that this is a feasible technique (relatively easy to perform) and could or should be considered in emergency situations or similar circumstances to those described in our case.
Ethical disclosures
Protection of human and animal subjects. The authors declare that no experiments in humans or animals were performed as part of this research.
Confidentiality of data. The authors declare having followed the protocols of their centre of work regarding patient data disclosure.
Right to privacy and informed consent. The authors obtained the informed consent of the patient and/or subject reported in the article; the form is kept by the corresponding author.











 texto em
texto em