What do we know about this problem?
EA is highly effective and commonly used in liver surgery for the intra and postoperative pain management. Nevertheless the role of EA within the setting of an ERAS program has been ques tioned. The risk of epidural hematoma caused by the possible prolonged prothrombin time after liver surgery and postoperative kidney failure due to hypotension, determine that EA cannot be recom mended in liver surgery for ERAS patients.
Recently, ESP block a safe, simple, and effective interfascial plane block has been described for thoracic and abdominal surgery.
What does this new study contribute?
It can contribute to give analgesia in high-risk patients, in laparoscopic surgery and maybe to be considered as part of ERAS guidelines for liver surgery.
Introduction
Liver resection is the treatment of choice for many liver tumors.
Epidural anesthesia (EA) ensures an excellent intra and postoperative pain relief.
However, coagulation abnormalities after surgery, hypotension due to sympathetic block and the presence of comorbid illnesses may be contraindications to EA, in according to the enhanced recovery after surgery (ERAS) recommendations in liver surgery.1
Recently, erector spinae plane (ESP) block a safe, simple, and effective interfascial plane block has been described for thoracic and abdominal surgery.2 The ESP block provides both somatic and visceral analgesia, which would make it a regional anesthetic technique ideal for abdominal surgery. When performed bilaterally it has been reported to be an effective alternative to thoracic epidural analgesia.3
We describe the case of a patient with Parkinson's disease (PD) and cardiac dysfunction undergoing laparoscopic right liver resection in whom a combined right continuous ESP block, contralateral transversus abdominis plane (TAP) and oblique subcostal TAP (OSTAP) blocks were performed for pain management.
Case report
Written informed consent was obtained from patient for this report. Ethics board approval for case report was not required by our institute.
A 63-year-old male patient (weight: 85 kg, height: 175 cm) was admitted with a diagnosis of hepatocellular carcinoma. Surgeon planned a laparoscopic right liver resection.
His past medical history included PD, diabetes mellitus type 2 and arterial hypertension.
Four years ago he showed a complete atrioventricular block and a dilated cardiomyopathy for which an implantable cardioverter defibrillator had been implanted.
On physical examination he had mild tremor, slowing of movements, stiffness, speech disturbance.
Limit in neck extension without other signs of probable difficult intubation.
A transthoracic echocardiogram confirmed cardiomy opathy and a left ventricular ejection fraction of 40%.
Spirometry was performed to assess lung function and showed moderate obstructive ventilatory failure.
Blood tests revealed a normal serum albumin level and blood count, no hydroelectrolyte disorder, high N-terminal probrain natriuretic peptide (824pg/mL) and a serum creatinine of 1.78mg/dL which corresponded to an estimated glomerular filtration rate using Cockcroft-Gault formula of 51mL/min.
In view of his general status, an admission in intensive care unit (ICU) was planned for postoperative clinical monitoring.
Anesthestic management was regional anesthetic technique for the intra and postoperative pain control associated with general anesthesia (GA).
In the preoperative room ECG and pulse oximetry were established and an arterial catheter was inserted into the radial artery under local anesthesia. A FloTrac catheter (Edwards Lifesciences, Irvine, CA) was the attached to the intrarterial access that was then connected to the EV1000/Volume View (Edwards Lifesciences). Continuous arterial pressure, cardiac index (CI), stroke volume index, and stroke volume variation (SVV) were monitored.
Defibrillator pads were applied to the chest. The Bispectral Index (BIS) and train-of-four monitoring were used to assess the brain activity and neuromuscolar blockade, respectively.
Intravenous midazolam (1 mg) was administered for patient comfort.
The GA was induced with 100-mg fentanyl, 160-mg propofol, and 70-mg rocuronium intravenously. Trachea was intubated and the lungs were mechanically ventilated with O2, air, and desflurane.
A triple-lumen 14-gauge catheter was inserted in the right internal jugular vein using ultrasound sonography. At this time, central venous pressure (CVP) systemic vascular resistence were monitored by the EV1000 hemodynamic system.
For the surgical pain control, in sterility and through the same ultrasound system, a combination of right continuous ESP block, contralateral TAP, and OSTAP block were performed.
The patient was turned into a left lateral position to perform the ESP block. The level of 12th rib and transverse process was located using a low-frequency linear trans ducer (6-13MHz, Sonosite SII, Bothell, WA). The transverse process of the 7th thoracic vertebra was further located counting upwards.
The ultrasound transducer was placed in a transverse orientation to identify the lateral tip of the right transverse process of the 7th thoracic vertebra.
The transducer was then rotated 90 degrees into a longitudinal parasagittal orientation over the transverse process.
A 18G, 110mm insulated needle (Contiplex; B. Braun, Melsungen, Germany) was introduced in plane approach of the ultrasound probe below erector spinae muscle over the transverse process.
After verifying the correct space with hydrodissection using 5 mL of saline 0.9%, a catheter was inserted and a bolus of 20mL 0.25% levobupivacaine was injected. The catheter was attached to the front of the chest (Fig. 1). In most of the cases the ESP block is performed before the catheter is inserted. This is a practical recommendation based on other clinical reports.
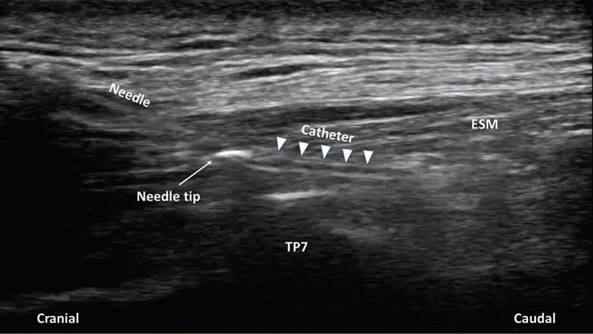
Source. Authors.
Figure 1 Ultrasound image of continuous erector spinae plane block. The image demonstrating needle placement and catheter insertion in a cranial to caudal direction deep to erector spinae muscle. ESM = erector spinae muscle, TP7 = transverse process of the seventh thoracic vertebra.
Subsequently, TAP and OSTAP blocks was performed contralaterally in according to the Hebbard approach, injecting 20 mL 0.25% levobupivacaine in each procedure for a total volume of 40mL.4
The intraoperative fluid and vasopressor/inotrope ad ministration was guided by the EV1000/Volume View parameters. The goal-directed fluid therapy was put in place to maintain SVV< 15%, CI > 2.2L/min/m2, and CVP < 5 cmH2O. The BIS value was maintained between 40 and 45.
Surgical time was 4h with a total blood loss of 700mL and urinary output of 400mL.
Total fluids administered were 1700 mL of crystalloids and 2 bolus of 4 mg ephedrine were administered: after GA induction and during parenchymal resection.
Thirty minutes before the end of the surgery 1 g of paracetamol was administer.
No other analgesic drugs were administered during surgery.
The surgery was uneventful and well tolerated by the patient. No rapid hemodynamic modifications were observed during the surgery.
At the end of surgery, the patient's trachea was extubated and he was transferred to the postoperative recovery room. The patient visual analog scale (VAS) was 0/10 at rest and when coughing.
After 1 hour he was admitted in ICU for postoperative clinical monitoring for 1 day and then in the liver surgery ward.
Postoperative analgesia included an infusion of 0.25% levobupivacaine (10mL/h) into the ESP catheters for 36 h and paracetamol 1 g every 8h.
The patient's VAS were 0-1 at rest, 1-2 on movement in the postoperative period. No other analgesic drugs were required.
Postoperative period was uneventful, vital signs, and mentalstatus were stable. He was discharged after4dayto the surgery.
Discussion
ESP block is an effective analgesic technique for breast, thoracic, bariatric, and abdominal surgery.3,5-7
The exact mechanism of action has not yet been established and is still under study. However, many authors conclude that the local anesthetic injection below the erector spinae muscle on the transverse process involves the spread in the paravertebral space leading the effective analgesia for somatic and visceral pain.3
Several anatomical studies have shown a wide cranio-caudal distribution of the local anesthetic, with different extension along the trunk depending on the injection level, local anesthetic volume, and anatomical variables. Nevertheless, many of them describe that the injection of 20 mL of fluid at the T7 level determines a diffusion from the upper thoracic vertebral segments to the lumbar ones.8
When ESP block is performed at the T7-8 level, it provides adequate analgesia in laparoscopic cholecystectomy, laparoscopic inguinal hernia repair, left lobe liver resection, urological, and bariatric surgery.3,9,10
In this case, we decided to perform a combined continuous right ESP block, contralateral TAP, and OSTAP blocks.
The somatic pain from the surgical field, due to skin incision and laparoscopic ports insertion, was covered by the contralateral TAP and OSTAP blocks, while the visceral pain relief caused by the right liver parenchimal resection was covered by ESP block.
We could choose to perform a bilateral ESP block. However, the safety of the block is not yet established, and a local anesthetic contralateral spread may occur.11
In a patient with impaired cardiac function and an altered autonomic nervous system due to PD, an unex pected double contralateral spread in epidural space can result in hemodynamic instability.
We could have also used a continuous bilateral TAP and OSTAP blocks, but we only had a bilateral somatic pain relief; the right visceral pain due to liver resection was not covered. Furthermore, the catheter placement is within the surgical field.12
Quadratus lumborum block with catheters is an option as it provides somatic and visceral analgesia. However, it is a more invasive technique than the ESP block and could cause an accidental motor block.13
EA is highly effective and commonly used in liver surgery for the intra and postoperative pain management. Nevertheless the role of EA within the setting of an ERAS program has been questioned. The risk of epidural hematoma caused by the possible prolonged prothrombin time after liver surgery and postoperative kidney failure due to hypotension, determine that EA cannot be recommended in liver surgery for ERAS patients.1
Moreover, important innovations have been introduced with laparoscopy in liver surgery. These new approaches are associated with less postoperative pain than open surgery, and EA can be an excessive analgesic technique, especially in patients with multiple comorbidities.
EA allow to maintain a low CVP and that significantly reduces the intraoperative bleeding with improving splanchnic perfusion. However, a sympathetic block in a patient with cardiovascular instability and autonomic dysfunction due to PD, can lead to sudden or exaggerated response to central neuraxial block as severe hypotension.14
Benefits have been demonstrated in favor of abdominal wall blocks as part of an ERAS program for liver resection.15
Frequently, oral and intravenous analgesic drugs are used for liver resection, but they may generate some undesirable effects in multicomorbidities patients. Opioids may exacerbate the neurological symptoms of PD, and increase the risk of nausea and vomiting.
Renal and platelet function may already be impaired in patients with liver disease and the Non-steroidal anti inflammatory drugs administration may worsen the functionality of both.
In conclusion, a combination of ESP block on 1 side and TAP and OSTAP blocks on the other side can be an effective approach for intra and postoperative analgesia in the high risk patient undergoing laparoscopic right liver resection.
Continuous ESP block provides adequate somatic and visceral analgesia. In addition, regional anesthesia has not exacerbated the symptoms of PD. Additional clinical research, including the randomized perspective controlled studies are required in liver surgery to ensure safety and efficacy.
Ethical responsibility
Human and animal protection: the authors state that no human or animal experiments have been carried out for this study.
Right to privacy and informed consent: the authors obtained the authorization and informed consent from the patient guaranteeing patient information confidenti ality in accordance with the principles of the Declaration of Helsinki.











 text in
text in 


