Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Biomédica
Print version ISSN 0120-4157On-line version ISSN 2590-7379
Biomédica vol.29 no.4 Bogotá Oct./Dec. 2009
PRESENTACIÓN DE CASO
1 Facultad de Ciencias de la Salud, Universidad Autónoma de Bucaramanga, Floridablanca, Colombia
2 Facultad de Salud, Universidad Industrial de Santander, Bucaramanga, Colombia
Recibido: 26/01/09; aceptado:16/04/09
Introduction. Solitary neurofibromas are benign tumors, often the manifestation of neurofibromatosis, and reflect a hereditary pathology with several variants. The clinical manifestations of solitary neurofibromas change according to their location and can generate a variety of symptoms. Usually, solitary neurofibromas are located in the skin and rarely in other places. Surgical removal is the only treatment; malignant transformation and recurrence are unusual.
Objective. A case is reported of solitary neurofibroma in the abdominal wall of a 19-year-old patient without neurofibromatosis.
Materials and methods. Articles included are from Proquest, Pubmed and Ovid databases. Key words used were neurofibroma, tumors of the neural sheath, and case report. The search is current as of May 24, 2007.
Conclusions. This case appears to be the first one with these characteristics reported in the English and Spanish medical literature.
Key words: neurofibroma, nerve sheath neoplasm, case reports, abdominal wall, neuro-fibromatoses, fibroblasts.
Neurofibroma solitario en pared abdominal en paciente sin neurofibromatosis: reporte de caso
Introducción. Los neurofibromas solitarios son tumores benignos de carácter hereditario, que presentan variantes. Las manifestaciones clínicas cambian según su localización y, ocasionalmente, son similares a las de la neurofibromatosis. Usualmente, los neurofibromas están localizados en piel y raramente en otras partes. El único tratamiento es la resección quirúrgica. Su transformación maligna y recurrencia son poco usuales.
Objetivo. Reportar el caso de un paciente masculino de 19 años, sin neurofibromatosis, con un neurofibroma solitario en pared abdominal.
Materiales y métodos. Se incluyeron artículos encontrados en Proquest, Pubmed y Ovid. Las palabras clave utilizadas en la búsqueda fueron neurofibroma, tumores de la vaina neural y reporte de caso. La búsqueda está actualizada hasta el 24 de mayo de 2007.
Conclusiones. Éste parece ser el primer reporte de un caso con estas características en la literatura médica en inglés y en español.
Palabras clave: neurofibroma, neoplasias de la vaina del nervio, informes de casos, pared abdominal, neurofibromatosis, fibroblastos.
Schwanoma, neurofibroma and neurogenic sarcomas represent three presentations of neural sheath tumors. However, nearly 90% of the tumors are benign, and 10% of these benign cases have multiple locations. Neurofibromas can develop in any encapsulated nerve of the body and can be divided into: 1) solitary neurofibromas, which are well-defined and circumscribed tumors; 2) plexiforms, which are diffuse masses, formed of neural fibers; 3) multiple, like plexiforms, which are generally associated with hereditary diseases; and 4) infiltrating neurofibromas called diffused. Although neurofibromas are common in neurofibromatosis, that pathology must not be immediately concluded when finding one of these tumors, since occasionally solitary neurofibromas can be found in healthy people.
Neurofibromatosis is a hereditary, autosomal dominant disease, with a variety of clinical presentations and phenotypic manifestations in the bones, nervous system, eyes, skin, gastrointestinal tract and other body parts. Each can be classified as one of two types: type 1 neurofibromatosis, also known as von Recklinghausen`s disease, is characterized by peripheral manifestations, whereas type 2 neurofibromatosis has central nervous system alterations.
The association between solitary neurofibromas and neurofibromatosis has not yet been established (1-7). Schwann cells, mast cells, fibroblasts, perineural cells, endothelial cells and collagen are the main components of neurofibromas. Solitary neurofibromas are solid, well-circumscribed, differentiated and non-encapsulated tumors that tend to grow slowly in the skin of people between 20 and 30 years of age, and present without sex differences. Neurofibromas arising in other parts of the body are rare (2,3,5-9).
The damage caused by neurofibromas is influenced by their location. Cutaneous tumors cause surface deformation, whereas deeper masses can cause functional compromise and destruction as a result of the compression of neighboring organs. Although most are benign, some may cause secondary destruction as a result of the pressure exerted; consequently, symptoms depend on the size of the lesion (4,6).
With ultrasonography imaging, neurofibromas appear as smooth, well-defined and lobulated masses; with computed tomography (CT), they have a homogeneous, smooth and round appearance and often contain multiple cystic spaces caused by myxoid degeneration; and with magnetic resonance (MR) imaging, they demonstrate a target-like enhancement pattern with attenuation or signal intensity in the central portion different than at the periphery. Histology and immunohistochemical studies are necessary for exact diagnosis. Histological characteristics can change according to the quantity of mucine and myxoid tissue (3,4). Complete surgical resection is the only treatment for these tumors. Malignant transformation is unusual (1,5,10,11).
Herein, the first case of solitary neurofibroma in the abdominal wall of a patient without neurofibromatosis is reported. Electronic searches for reports of similar cases and other rare manifestations using the key words "neurofibroma," "neural sheath tumors," and "case report" were conducted in Proquest, Pubmed and Ovid databases for all English and Spanish articles with abstracts. In order maximize the number of articles, no date limit was set, and the search is current as of March 24, 2007. Initially, 1,360 articles were obtained, of which 157 fit the inclusion criteria. However, only the 22 were referenced in the current work with a focus on solitary neurofibroma in the patient without neurofibromatosis, or gave important theoretical contributions.
Case report
A case is presented of a 19-year-old male who, over the course of six months, noticed the presence of an abdominal bulge in the right inferior quadrant. It was located 17 cm from the midline, 3 cm above the anterior and superior iliac crests, and it was detected easily and superficially, well-defined, firm, and non-reductable. It was fixed to the abdominal wall and painful to deep palpation. No other findings at the physical examination or any other symptomatology were reported.
No important findings appeared in the personal or familial histories. To confirm the diagnosis, ultrasonography of soft tissues was conducted that permitted differentiation between abdominal hernia, lipoma, neurofibroma, schwannoma or other neoplasm common in this location. A well-defined, hypoechogenic, 1 x 2 cm mass was found attached to the abdominal wall (figura 1). The patient appeared to have a lipoma; conse-quently, surgical resection was done, without any complications, and with a satisfactory recovery.
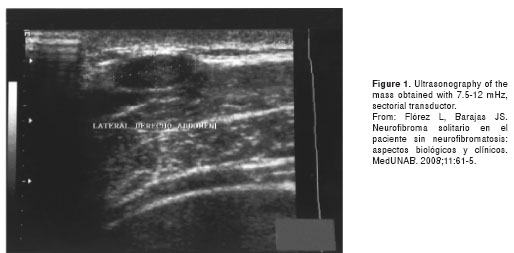
The pathology report from the extracted sample was as follows:
- Macroscopic description: pale pink, non- encapsulated, moderately smooth, nodular lesion, with well-delimited edges and measuring 18 x 8 x 6 mm.
- Microscopic description: benign non-encapsulated tumor, made up of fusiform cells, with several capillaries with prominent endothelium. The cells were deposited in interlaced bundles and collagen fibers. No signs of atypia or significant mitotic activity were present. A clear, benign, pattern without evidence of malignancy was found. Immunocytochemistry tests were not conducted because of the clear histological pattern, characteristic of a benign mass (figura 2). Diagnosis: resection of an abdominal wall: neurofibroma.
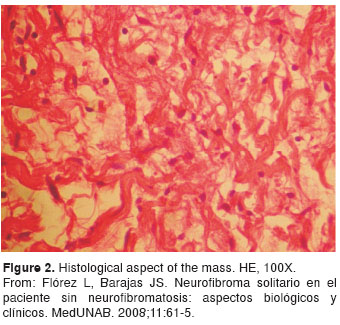
Patient's clinical progress was satisfactory, and a year later no other clinical signs or symptoms were present. Upon investigation of the patient's background and study of neurofibromatosis, no other similar pathology was present, nor was any other disease. Questioning and examining multiple members of the family detected no risks of neurofibromatosis. A genetic screening was not conducted.
Discussion
In a patient with a superficial mass in the abdomen, the following alternatives must be considered in differential clinical diagnosis. The possibility of inguinal hernias must be first considered; they are a common cause of pain and frequent abnormality of the abdominal wall. Other potential diagnoses include abscesses, benign and malignant tumors originating from muscle, nerve or fat tissue, and lymphatic regional nodes. A complete history and physical examination are important in difficult cases; imaging and histological studies can be used to guide diagnosis (11,12).
Abdominal neurogenic tumors are most commonly located in the retroperitoneum, particularly in the adrenal glands. However, other areas of the abdomen including the urinary bladder, the abdominal wall, and the biliary bladder can also be involved. Making a definitive pre-surgical diagnosis is very difficult and requires microscopical differentiation. When a diagnosis of solitary neurofibroma is made, other subclinical forms of neurofibromatosis must be excluded as well as to confirm that the mass was solitary (3,5,6,10).
Only one similar case has been reported, that of a 21-year-old male patient with a mass in the right inguinal region. During the physical examination, a firm mass was found fixed to the abdominal wall; CT and MR scans showed a mass within the right rectus sheath displacing the rectus muscle medially. No adenopathy was noted. The mass was surgically removed and upon histopathological exam, it was identified as a plexiform neurofibroma. The patient was interviewed a second time, and familial history of neurofibromatosis was uncovered. The patient exhibited light brown spots, suggesting a diagnosis of neurofibromatosis. The current case presentation seems to be the first report of a case of solitarily neurofibroma in the abdominal wall of a patient without neurofibromatosis, at least as reported in the English and Spanish medical literature (12).
Other cases of solitary neurofibroma in patients without neurofibromatosis have been reported in body regions with slightly less frequency. These include the nasal cavity (1), palatine tonsil (13), soft palate (2), subglottical (14), as an isolated cervical mass (15), intramedullary (16), on the common bile duct (10), kidney (5), ileum (17), colon (18), anal canal (19), spermatic cord (11), scrotum (20,21) and vulva (22).
There are not conflicts of interest.
Costs were financed by the patient and the authors.
Correspondencia:
Juan Sebastián Barajas-Gamboa, carretera a Floridablanca N° 149-30, Condominio La Zafra, Torre 1, apartamento 201, Floridablanca, Santander, Colombia.
Teléfonos: (311) 464 9642 y (300) 312 2126 jbarajas2@unab.edu.co y jsbarajas@ucsd.edu
1. Hirao M, Gushiken T, Imokawa H, Kawai S, Inaba H, Tsukuda M. Solitary neurofibroma of the nasal cavity: Resection with endoscopic surgery. J Laryngol Otol. 2001;115:1012-4. [ Links ]
2. Sinha R, Paul R, Sen I, Sikdar B. A solitary huge neurofibroma of the soft palate. J Laryngol Otol. 2002;116:637-8. [ Links ]
3. Rha S, Byun J, Jung S, Chun J, Lee H, Lee J. Neurogenic tumors in the abdomen: tumor types and imaging characteristics. RadioGraphics. 2003;23:29-43. [ Links ]
4. Shaida A, Yung M. Neurofibroma of the pinna. Ear Nose Throat J. 2007;86:36-8. [ Links ]
5. Kostakopoulos A, Chorti M, Protogerou V, Kokkinou S. Solitary neurofibroma of kidney: clinical, histological and chromosomal appeareance. Int Urol Nephrol. 2003;35:11-3. [ Links ]
6. Venadero F, Rodríguez M, Merelo V, Cervantes A, Ramos A. Neurofibroma solitario. Comunicación de dos casos. Rev Cent Dermatol Pascua. 2004;13:99-102. [ Links ]
7. Panteris V, Vassilakaki T, Vaitsis N, Elemenoglou I, Mylonakou I, Karamanolis D. Solitary colonic neurofibroma in a patient with transient segmental colitis: case report. World J Gastroenterol. 2005;11:5573-6 [ Links ]
8. Kilmurray L, Ortega L, Martínez A, Sanz J. Neurofibroma with psammoma bodies. Histol Histopathol. 2006;21:965-8. [ Links ]
9. Viskochil D. It takes two to tango: mast cell and Schwann cell interactions in neurofibromas. J Clin Invest. 2003;112:1791-3. [ Links ]
10. Li F, Cheng J, He S, Li N, Zhang M, Zhang X, et al. Primary neurofibroma of the common bile duct as an unusual cause of obstructive jaundice: A case report. Dig Dis Sci. 2005;50:1166-8. [ Links ]
11. Deliveliotis C, Albanis S, Skolarikos A, Varkaraki J. Solitary neurofibroma of the spermatic cord. Int Urol Nephrol. 2002;34:373-5 [ Links ]
12. Chang C, Provost D, LeVoyer T, Ellison R. Abdominal wall neurofibroma presenting as an inguinal hernia. Mil Med. 2004;169:192-3. [ Links ]
13. Surwald C, Salam M, Rowe R. A solitary neurofibroma of the palatine tonsil. J Laryngol Otol. 2002;116: 1050-2. [ Links ]
14. Tanaka H, Patel U, Coniglio J, Rubio A. Solitary subglottic neurofibroma: MR Findings. AJNR Am J Neuroradiol. 1997;18:1726-8 [ Links ]
15. Amor-Dorado J, Candia J, Costa C, Mate A, Rossi J. Neurofibroma cervical solitario. ORL-DIPS. 2002;29:192-5. [ Links ]
16. Sharma V, Newton G. Cervical intramedullary neurofibroma. J Korean Med Sci. 1990;5:165-7. [ Links ]
17. Watanuki F, Ohwada S, Hosomura Y, Okamura S, Kawashima Y, Tanahashi Y, et al. Small ileal neurofibroma causing intussusception in a non-neurofibromatosis patient. J Gastroenterol. 1995;30:113-6. [ Links ]
18. Abramson L, Orkin B, Schwartz A. Isolated colonic neurofibroma manifested by massive lower gastrointestinal bleeding and intussusception. South Med J. 1997;90:952-4. [ Links ]
19. Frick E Jr, Lapos L, Vargas H. Solitary neurofibroma of the anal canal: report of two cases. Dis Colon Rectum. 2000;43:109-12. [ Links ]
20. Turkyilmaz Z, Sonmez K, Karabulut R, Dursun A, Isik I, Basaklar C, et al. A childhood case of intrascrotal neurofibroma with a brief review of the literature. J Pediatr Surg. 2004;39:1261-3. [ Links ]
21. Issa MM, Yagol R, Tsang D. Intrascrotal neurofibromas. Urology. 1993;41:350-2. [ Links ]
22. Venter P, Rohm G, Slabber C. Giant neurofibromas of the labia. Obstet Gynecol. 1981;57:128-30. [ Links ]














