Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Biomédica
Print version ISSN 0120-4157On-line version ISSN 2590-7379
Biomédica vol.31 no.2 Bogotá Apr./June 2011
ARTÍCULO ORIGINAL
1 Departamento de Anestesiología, Clínicas Colsánitas, Bogotá, D.C., Colombia
2 Instituto de Investigaciones Clínicas, Facultad de Medicina, Universidad Nacional de Colombia, Bogotá, D.C., Colombia
Institución donde se ejecutó: Compensar EPSRecibido: 07/10/10; aceptado:12/02/11
Introduction. Perirectal block using four puncture places has been classically described for rectal surgery.
Objective. This paper was aimed at showing the quality of anesthesia and postoperative analgesia using a new two-puncture-site technique.
Materials and methods. Patients scheduled for ambulatory rectal surgery between January/2003 and December/2007 were included consecutively. The new two-puncture technique was used. Alternative anesthetic management and level of postoperative pain requirements were evaluated (rated visual analogue scale-VAS). Follow-up was done by telephone between 1st and 10th postoperative day to evaluate complications, pain (yes/no), and satisfaction level (1–5 points score).
Results. Four hundred and nine subjects were included; 50.61% were female. Mean age was 43 (95%CI: 41-44; range: 17-85), 12.7% were aged over 60. According to the American Society of Anesthesiology (ASA), 72.6% were classified as ASA1 and 26.1% ASA2. External and internal hemorrhoidectomy was performed on 31% of patients; 61.6% had two or more procedures. Lidocaine was used on 406 subjects. Ropivacaine was added for 9.2% of them and levobupivacaine for 89.4%. 394 patients were followed-up. Median follow-up was 4 days. A response was obtained from 346 subjects (84.6%); 105 (30.3%) recalled having suffered pain during the post-operative period, being most frequent in the lidocaine+ropivacaine group (17/39, 43.5%) than in the lidocaine+bupivacaine group (88/307, 28.6%). Satisfaction was evaluated by 336 subjects (82.1%), 332 of them (98.8%) awarding a score of 5. Two subjects (0.6%) scored this 2 and 1. Subjects did not mention complications.
Conclusions. The new peri-rectal two-puncture block technique is easy and also provides analgesia and a high degree of satisfaction.
Key words: pain, postoperative; nerve block; anesthesia, local; ambulatory surgical procedures.
Bloqueo perirrectal para cirugía anorrectal ambulatoria: una nueva técnica
Introducción. El bloqueo perirrectal de cuatro punciones ha sido descrito clásicamente para cirugía rectal. El objetivo de este artículo es describir la calidad de la anestesia y la analgesia posoperatoria cuando se utiliza una nueva técnica de dos punciones.
Materiales y métodos. Se incluyeron, consecutivamente, los pacientes programados para cirugía rectal ambulatoria entre enero de 2003 y diciembre de 2007. Se utilizó la nueva técnica anestésica de dos punciones. Se registraron las necesidades de manejo anestésico alternativo y el nivel de dolor posoperatorio por medio de una escala visual análoga graduada. El seguimiento fue telefónico (1 a 10 días posoperatorios) para evaluar complicaciones, dolor (sí/no) y nivel de satisfacción (escala, 1 a 5).
Resultados. Se incluyeron 409 sujetos. El 50,61 % eran mujeres. La edad promedio fue de 43 años, (rango, 17 a 85). El 12,7 % eran mayores de 60 años. De acuerdo con la clasificación de la American Society of Anesthesiology (ASA), el 72,6 % fueron ASA1 y 26,1 % ASA2. Se practicó hemorroidectomía externa e interna en 31 % de los pacientes; 61,6 % tuvo más de dos procedimientos. Se utilizó lidocaína en 406 sujetos. Se adicionó ropivacaína en 9,2 % y levobupivacaína en 89,4 %. La mediana de seguimiento fue de cuatro días. Se obtuvo respuesta de 346 sujetos (84,6 %); 105 (30,3 %) refirieron haber sufrido dolor durante el posoperatorio, lo que fue más frecuente en el grupo de lidocaína más ropivacaína (17/39, 43,5 %) que en el de lidocaína más bupivacaína (88/307, 28,6 %). La satisfacción se evaluó en 336 sujetos (82,1 %): 332 (98,8 %) la calificaron en 5, 2 sujetos (0,6 %) la calificaron en 2 y en 1. No hubo complicaciones.
Conclusiones. El bloqueo perirrectal de dos punciones es una técnica fácil que, además, provee analgesia y un alto grado de satisfacción.
Palabras clave: dolor posoperatorio, bloqueo nervioso, anestesia local, procedimientos quirúrgicos ambulatorios.
Anorectal surgery has been performed under neuraxial or general anesthesia (1). However in the last few years the great increase in outpatient surgery requires from anesthesiologists not only simple and safe anesthetic techniques, but also cost effective ones that provide the patient with proper postoperative analgesia. Studies have compared general, neuraxial, and local anesthesia with sedation for outpatient rectal surgery (2,3), the latter being described as safe and effective, with the advantage of decreasing the stay in the recovery room (4). Among the regional and local techniques several types of blocks, like the posterior perineal block, have been used (1). This is performed with the patient in lithotomy position and requires a superficial and deep infiltration of the ischiorectal fossa carries a high risk of intravascular injection of the local anesthetic agent. Other technique, used mainly by proctologists, is the perianal block in which the patient in prone jackknife position has four injections made in the mucocutaneous border of the anus with significant discomfort (5). For these reasons, this study presents a new anesthetic technique, the perirectal block which is performed under intravenous sedation using only two puncture sites. This paper was aimed at showing the quality of the anaesthesia and postoperative analgesia using a new two-puncture site technique.
Materials and methods
Four hundred and nine patients were scheduled for ambulatory rectal surgery at the ambulatory surgical unit of Compensar EPS in Bogotá, between January 2003 and December 2007. The anesthetic technique proposed was explained to all of the patients including the risks and the complications, and thereafter they signed the informed consent authorizing the anesthetic procedure. The perianal block with two injections was performed in all of the patients and the need of an alternative anesthetic management was assessed. The level of postoperative pain was measured using the graduated visual analogue scale (VAS). A telephonic postoperative interview was done between the 1st and 10th day to detect complications, the presence of pain (yes/no), and assess the level of satisfaction of the patients (in a scale of 5 points, 1-lowest, to 5 highest). Median and ranges are showed given that data did not have normal distribution.
TechniqueThe perianal block with 2 injections is a typical field block that requires 2 injections, one on each side of the anus, and directing the infiltration to 3 different places (figure 1). These places are: the rectal submucosa, the perineal tissues, (including the anal sphincter) (branchs of the hemorrhoidal nerves, internal pudendal nerves, and the anococcygeal nerves) and the subcutaneous tissue localized under the perianal mucocutaneous juncture (inferior gluteal nerves and perineal branches of minor nerves from the sacral plexus).
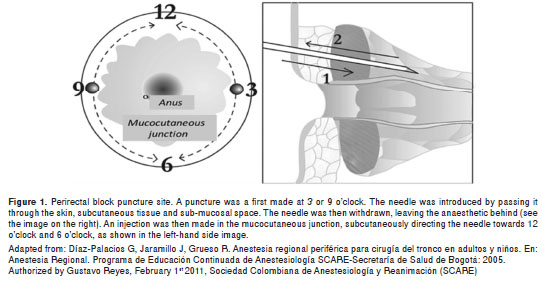
The patient is set in a prone jackknife position and the buttocks are separated from the midline with 4-inch sections of tape. After a mild sedation with midazolam and fentanyl administered with an intravenous access in any of the upper limbs, the anal mucocutaneous border is identified. The injections are performed in two points: at clock hand positions 3 and 9.
After asepsia and antisepsia, the lidocaine jelly lubricated index finger of the nondominant hand is inserted in the anus, with which a 1 1/2 inch 23 gauge needle is directed to the mucocutaneous rectal tissue. The needle is introduced perpendicularly to the skin in position 9 and it is advanced with posterior anterior direction with slight lateral deviation from superficial to deep, parallel to the lateral wall of the rectum. The structures traversed are the skin, subcutaneous tissue, anal sphincter, and the subcutaneous perianal tissue, which is identified because the tip of the finger in the rectum, touches the tip of the needle in this place. It is essential to be very careful to avoid puncturing the rectal mucosa or an accidental puncture of the finger.
After testing for aspiration of blood, and verifying a low resistance to injection, 5 to 7 mL of local anesthetic are injected into the submucosal tissue. Afterwards, an additional 5 ml of local anesthetic are infiltrated in the perineal tissues from deep to superficial as the needle is removed just until the subcutaneous anal tissue. At this point, the angle of the needle is changed to almost parallel to the skin and it is introduced under the mucocutaneous juncture, both in a forward and backwards direction infiltrating subcutaneously an additional 5 ml in the form of a split rhombus on this side of the anus.
The needle is removed and the process is repeated at the clock hand position 3 on the other side of the anus. After the 2 injections are performed, firm pressure over the anus and the puncture sites is applied and held for 3 min, to improve the spread of local anesthetic in the tissues. The dilation of the anal sphincter can be observed almost immediately and within few minutes, anesthesia of the skin, the anal mucosa and rectum is achieved.
Results
Four hundred and nine patients were included during this period of which 207 were women (50.61%). Their median age was 43 years old with extremes of 17 and 85 years overall, and for women and men the median of ages were respectively 41 (range: 17-76) and 47 years (range: 21-85). 52 patients (12.7%) were older than 60 years. All patients were ambulatory.
The physical status of the patients, according to the classification of the American Society of Anesthesiologists (ASA), was recorded for 402 of the 409 cases; 292 patients (72.64%) were ASA physical status I, 105 (26.12%) were ASA physical status II, and 5 patients were ASA physical status III (1.24%). In seven patients ASA status was not registered.
Mixed hemorrhoidectomy was performed in 127 patients (31.1%), only internal in 23 patients (5.6%), and only external in 3 (0.7%). Two or more procedures excluding mixed hemorrhoidectomy were performed in 256 patients (62.6%). These procedures included polypectomies in 119 patients (29%), fissurectomy in 83 patients (20.2%), sphincterotomy in 24 (5.8%), fistulectomy in 23 (5.6%), and prolapse correction in 5 (1.2%). Two patients had an anal tumor resection.Lidocaine was used in 406 patients; 274 patients (67.49%) received 200 mg or less, 108 (26.6%) received doses between 201 and 300 mg and 24 (5.91%) received doses between 301 and 500mg.
Ropivacaine was added in 38 patients. 19 patients (50%) received 112.5 mg or less. The follow-up of patients was done between 1 to 11 postoperative day in 394 patients, with a median follow-up of 4 days. Complete responses were obtained in 346 patients (84.6%), of whom 105 patients (30.35%), referred postoperative pain, more commonly among the patients who received lidocaine and ropivacaine (17/39, 43.5%) than among those who received lidocaine and bupivacaine (88/307, 28.6%). Satisfaction scores were obtained from 336 patients (82.1%) of whom 332 (98.8%) scored 5, 2 patients (0.6%) scored 4, and 2 patients scored 1 and 2 respectively (0.6%). No complications were identified among the patients during follow-up.Discussion
Although it was impossible to contact 60 patients, the response rate of this study was 84.6% for pain assessment, and 82.1% for satisfaction assessment. Other studies report the discharge of some patients 24 hours after the procedure and do not mention any postoperative ambulatory follow-up (1,2).
The perianal block with 2 injections is a simple technique to perform as it is field block with both superficial and deep infiltration. As it is performed under mild sedation which theoretically decreases the possibility of respiratory depression, decreases the pain of the infiltration and shortens the duration of stay in the post anesthesia care unit (PACU), it has advantages reflected in the well-being of the patientsâ recovery. In addition, when compared to other techniques used in these procedures, like the perianal block with four injections, it has, theoretically, less risk of intravascular injection of the local anesthetic, as it is a field block where the depth of the needle is controlled easily with the fingertip and is less likely to produce pain, as it requires only two injections. It also provides adequate postoperative analgesia which is easily complemented with oral non-opioid analgesics in a multi modal scheme, as presented in the large number of patients with no postoperative pain in the postoperative care unit. To the best of our knowledge, there have been no previous reports of a two-puncture technique being used for performing this block.
In this study, we found better anesthesia with levobupivacaine as compared to ropivacaine. The literature describes that ropivacaine provides longer analgesia (6,7) but there are no studies comparing these 2 anesthetics in perianal blocks. We believe that the observed difference should be carefully analyzed as many more patients received levobupivacaine (368, 90.64%) than ropivacaine (38, 9.35%), because ropivacaine was not marketed anymore when the study was performed. In this study no side effects which have been described with other techniques used in these procedures, such as nausea, vomiting or urinary retention were observed. (1,2).
Even though this is a case series, this study describes the results of using 2 instead of 4 injections under mild sedation, which allowed the performance of the anorectal procedures described without the need of general anesthesia or complementing the block during the procedure. It can be expected that this technique has a better cost-effectiveness ratio when used in these procedures, compared to other regional and general techniques described, although further studies are required to verify this assertion.
As no follow-up was possible in 18% of the patients, there are some limitations of the results of the study, although in none of the 409 patients were there any complications or events recorded during their short stay in the post anesthesia care unit.
Analytical type studies are required to determine the effectiveness and safety of this technique compared to others frequently using these procedures, although no complications or adverse events were found in this case series.
Acknowledgements
We would like to thank Compensar, EPS, Colombia. Also to Gustavo Reyes, who draw the figure.
Conflict of interests
We declare that none of the authors has any conflict of interest in this publication.
Funding
No funds were received for this study from any pharmaceutical company. This study was performed during our daily clinical practice in anesthesiology.
Correspondencia: Javier H. Eslava-Schmalbach, Facultad de Medicina, Universidad Nacional de Colombia, Carrera 30Nº45-03, oficina 205, Bogotá, D.C., Colombia
Telefax: (+571) 316 5000, extensión 15186 jheslavas@bt.unal.edu.co
2. Read TE, Henry SE, Hovis RM, Fleshman JW, Birnbaum EH, Caushaj PF, et al. Prospective evaluation of anesthetic technique for anorectal surgery. Dis Colon Rectum. 2002;45:1553-8. [ Links ]
3. Li S, Coloma M, White PF, Watcha MF, Chiu JW, Li H, et al. Comparison of the costs and recovery profiles of three anesthetic techniques for ambulatory anorectal surgery. Anesthesiology. 2000;93:1225-30. [ Links ]
4. Esser S, Khubchandani I, Rakhmanine M. Stapled hemorrhoidectomy with local anesthesia can be performed safely and cost-efficiently. Dis Colon Rectum. 2004;47:1164-9. [ Links ]
5. Sobrado CW, Habr-Gama A. Hook-needle puncture. A new technique of local anesthesia for anorectal surgery. Dis Colon Rectum. 1996;39:1330-1. [ Links ]
6. Asik I, Kocum AI, Goktug A, Turhan KS, Alkis N. Comparison of ropivacaine 0.2% and 0.25% with lidocaine 0.5% for intravenous regional anesthesia. J Clin Anesth. 2009;21:401-7. [ Links ]
7. Kanai A, Osawa S, Suzuki A, Ozawa A, Okamoto H, Hoka S. Regression of sensory and motor blockade, and analgesia during continuous epidural infusion of ropivacaine and fentanyl in comparison with other local anesthetics. Pain Med. 2007;8:546-53. [ Links ]














