Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Investigación y Educación en Enfermería
Print version ISSN 0120-5307
Invest. educ. enferm vol.30 no.3 Medellín Sept./Dec. 2012
ARTÍCULO ORIGINAL / ORIGINAL ARTICLE/ ARTIGO ORIGINAL
Factors associated to the duration of exclusive breastfeeding
Factores asociados con la duración de la lactancia materna exclusiva
Fatores associados com a duração da lactância materna exclusiva
Jhon Henry Osorio Castaño1; Beatriz Eugenia Botero Ortiz2
1RN, M.Sc., Secretaría de Salud de Medellín, Colombia. jhonosca@hotmail.com.
2Physician, M.Sc., Comfenalco EPS, Colombia. bboteroo1@hotmail.com.
Receipt date: March 18th 2011. Approval date: March 23rd 2012.
Subventions: none.
Conflicts of interest: none.
How to cite this article: Osorio-Castaño JH, Botero-Ortiz BE. Factors associated to the duration of exclusive breastfeeding. Invest Educ Enferm 2012;30(3):390-397
ABSTRACT
Objective. To identify the scientific evidence available on factors associated to the duration of exclusive breastfeeding. Methodology. A systematic review without meta-analysis was performed. An electronic search strategy was conducted of primary articles published in Medline, Lilacs, Scielo, and Ovid from 1990 to 2010 in English, Spanish, and Portuguese. Observational and intervention studies were included, which sought to identify factors associated to the duration of exclusive breastfeeding for at least three months. Results. Some 195 studies were identified, but only 18 complied with the inclusion and quality criteria. A total of 66.6% measured the prevalence of breastfeeding up to six months. Fifty percent reported the use of a pacifier or baby bottle as the negative factor that most affects the duration of exclusive breastfeeding. Some 44.4% mentioned as positive factors in the duration of exclusive breastfeeding: high levels of schooling, multiparity, exposure to a breastfeeding program, and low family income. Conclusion. Literature available provides information on the factors associated to the duration of exclusive breastfeeding, although the methodological heterogeneity of the studies did not permit evaluating the scientific evidence of the results discussed.
Key words: breastfeeding; risk factors; prevalence; pacifiers; bottle feeding; review.
RESUMEN
Objetivo. Identificar la evidencia científica disponible acerca de los factores asociados a la duración de la lactancia materna exclusiva. Metodología. Revisión sistemática sin meta-análisis. Se realizó estrategia de búsqueda electrónica de artículos primarios publicados en Medline, Lilacs, Scielo y Ovid desde 1990 hasta 2010 en idioma inglés, español y portugués. Se incluyeron estudios observacionales y de intervención que buscaran identificar factores asociados a la duración de la lactancia materna exclusiva como mínimo por tres meses. Resultados. Se identificaron 195 estudios, pero solo 18 cumplieron con los criterios de inclusión y de calidad. El 66.6% realizó medición de prevalencia de lactancia materna hasta los seis meses. El 50% reportó el uso del chupo o biberón como el factor negativo que más afecta la duración de la lactancia materna exclusiva. El 44.4% mencionó como factores positivos en la duración de la lactancia materna exclusiva la escolaridad alta, la multiparidad, la exposición a un programa de lactancia materna y los ingresos familiares bajos. Conclusión. La literatura disponible provee información sobre los factores asociados a la duración de la lactancia materna exclusiva, aunque la heterogeneidad metodológica de los estudios no permitió evaluar la evidencia científica de los resultados narrados.
Palabras clave: lactancia materna; factores de riesgo; prevalencia; chupetes; alimentación artificial; revisión.
RESUMO
Objetivo. Identificar a evidência científica disponível a respeito dos fatores associados à duração da lactância materna exclusiva. Metodologia. Revisão sistemática sem meta-análise. Realizou-se estratégia de busca eletrônica de artigos primários publicados em Medline, Lilacs, Scielo e Ovid desde 1990 até 2010 em idioma inglês, espanhol e português. Incluíram-se estudos observacionais e de intervenção que procurassem identificar fatores associados à duração da lactância materna exclusiva no mínimo por três meses. Resultados. Identificaram-se 195 estudos, mas só 18 cumpriram com os critérios de inclusão e de qualidade. O 66.6% realizou medição de prevalência de lactância materna até os seis meses. O 50% reportaram o uso da chupeta ou mamadeira como o fator negativo que mais afeta a duração da lactância materna exclusiva. O 44.4% mencionaram como fatores positivos na duração da lactância materna exclusiva: a escolaridade alta, a multiparidade, a exposição a um programa de lactância materna e os rendimentos familiares baixos. Conclusão. A literatura disponível provê informação sobre os fatores associados à duração da lactância materna exclusiva, ainda que a heterogeneidade metodológica dos estudos não permitiu avaliar a evidência científica dos resultados narrados.
Palavras chaves: aleitamento materno; fatores de risco; prevalência; chupetas; alimentação artificial; revisão.
INTRODUCTION
In spite of national and international policies seeking to benefit the practice of breastfeeding for at least six months, reality shows a much lower duration. The mean duration of exclusive breastfeeding for Colombia is of 1.8 months, according to the results from the most recent Demography and Health Survey by PROFAMILIA (Encuesta de Demografía y Salud de Profamilia) conducted in 2010.1 Also, some studies have found that as the child gets older, breastfeeding times diminish. The risk factors identified for this event include not starting during the first hour after birth, using a baby bottle and including water and other foods during the first six months. Children breastfed for less than six months have a higher risk of becoming overweight or obese during the first years of life, a higher frequency of diarrhea and acute respiratory infections, and higher risk of constipation. Some protective factors have been identified like positive attitudes by the mother towards breastfeeding, adequate family support, adequate suction technique, and support through education by healthcare personnel.
The Ten-year Plan on Maternal breastfeeding (2010-2020)2 and the current National Plan on Public Health in Colombia3 contemplate among their strategies increasing the duration of exclusive breastfeeding. For this reason, it is necessary to evaluate the information from primary research regarding the duration of breastfeeding and the factors associated to this practice, which make women desist before the recommended times.
Among healthcare professionals, nurses play a relevant role in supporting breastfeeding, given that they have the greatest contact with mothers since the prenatal period; hence, awareness of the factors associated to this practice can result in the design of strategies tending to improve the duration of breastfeeding, which will benefit more mothers and children in this country.
The aim of this study was to identify the scientific evidence available regarding the factors associated to the duration of exclusive breastfeeding.
METODOLOGY
The studies included were observational and/or experimental, which evaluated the duration of exclusive breastfeeding for at least three months and its associated factors. Systematic reviews were also included, evaluating the duration of this practice and some interventions to improve it; from these, primary research were extracted that could be included in this review. The primary research had to be conducted with primiparous or multiparous women, of any age, during postpartum or not, without physical or psychological limitations that would affect the breastfeeding practice, with children born at term, weighing above 2 500 grams, with no limitation for breastfeeding, without hospitalization of the woman or the child due to causes other than postpartum for over 24 hours and in women without HIV infection. The variables evaluated in diverse studies included socio-demographic or clinical variables, as well as healthcare service, cultural, and family and/or personal variables.
The primary research articles were derived from a search in electronic data bases: Pubmed, Lilacs, Ovid, and Scielo from 1990 to 2010. Studies published in English, Spanish, and Portuguese were considered, but unpublished studies were not included. The search strategies included free terms and controlled vocabulary like breastfeeding, riks factors, pacifiers, prevalence. Exclusion was carried out by title and abstract. Thereafter, doubtful studies were obtained in full text, whenever these were available; once read, the decision was made on including them or not. A list was created of all the studies found through the search strategy and a thorough review was made of each list to detect duplicity of studies.
After conducting the exclusion by title and abstract, we proceeded to evaluate the quality of each of the potential studies for said purpose. This evaluation used the CASPe critical reading program4, which was converted to Excel and had the following items: database, number of study, name of study, type of study, and the four categories of the program: Elimination (E), Detail (D), Results (R), and Application of Results (AR); which have a total of 11 questions. The way to score the studies was defined as suggested by the CASPe program, by assigning YES or NO if the study complied with the condition evaluated. It was defined as inclusion (I) if the study obtained four or more YES and as exclusion (E) if the study obtained three or less YES. Each of the researchers conducted an individual reading of the studies included and consolidated their own results; whenever some study generated differences, review was requested from a third researcher, who for the case was the project advisor. The meta-analysis was considered inappropriate due to the heterogeneity of the studies, not only because of their design, but also because of the categorization of the variables measured.
The studies included for systematic review were entered onto an Excel database that included the following characteristics: Number of study, database, reference (name of study, authors, journal); country, year, study design, objective, sample size, dependent variable, independent variables, intervention/control, and result. The research was approved by the Research Committee at Universidad CES.
RESULTS
A total of 195 studies were identified of which only 18 were included in the review. The reasons for excluding the remaining 177 articles were: discarded because of the title (107), discarded because of the abstract (13), not available (21), doubtful studies excluded (19), excluded due to quality criteria (17). Of the 18 studies included, eight were cross-sectional studies, seven cohort studies, one case and control study, and two clinical trials. It is important to indicate that in the studies included there are primary research articles identified in some systematic reviews from where the information was taken to search for them.
In the results of the 18 studies included, only three studies did not measure the prevalence of exclusive breastfeeding; four studies did not evaluate factors influencing negatively upon breastfeeding, and eight studies did not evaluate factors influencing positively.
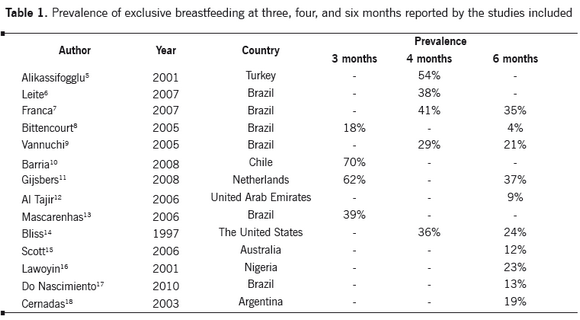
Of the studies measuring prevalence of exclusive breastfeeding, 66.6% did so up to six months, 33.3% up to four months, and 26.6% up to three months. All these studies evidenced an inverse behavior between duration of exclusive breastfeeding and age of breastfed children. As a child grows in months, exclusive breastfeeding decreases. Even studies measuring prevalence only up to three and four months show how the percentage of breastfed children diminishes.
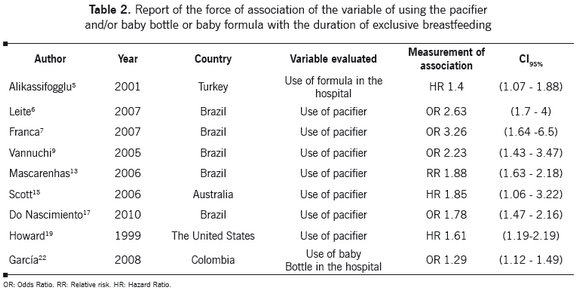
One of the variables that can negatively affect the duration of exclusive breastfeeding reported by 39% of the studies is the use of a pacifier.6,7,9,13,15-17,19 Two studies evaluated baby bottle or formula use in the hospital after delivery and found that it affected negatively the duration of said practice.5,22 Nine studies evaluating the variable of the use of a pacifier and baby bottle or baby formula in the hospital found a negative association as to how the exclusive breastfeeding practice is established. It is evident that the risk of discontinuing breastfeeding in children exposed to the pacifier or to the baby bottle is higher than in children not exposed to such element.
Other variables evaluated in the studies associated negatively to duration of exclusive breastfeeding were: planning and/or returning to work prior to six months,15-18,20,21 smoking during the pregnancy,13,15,22 problems with the onset of breastfeeding like trauma to the nipple,6,15 low maternal schooling,7,17 maternal age under 34 years,7,18 primiparity,7,9 cesarean delivery,8 single mother,22 and unfavorable opinion of breastfeeding by physicians and nursing personnel.20 Upon evaluating the studies in search of variables positively associated to the duration of exclusive breastfeeding, it was shown that of the 18 studies, eight did not find association among variables that could indicate the presence of a protective factor for the practice of exclusive breastfeeding.5-7,9,10,19,17,22
Studies identifying protective factors indicate that low family income – defined as less than the minimum wage,8,21 higher educational levels,12 multiparity11,20 and exposure to a breastfeeding program11,14 increase the duration of exclusive breastfeeding.
DISCUSSION
This systematic review evaluated the variables positively or negatively affecting the duration of exclusive breastfeeding reported in 18 primary research articles. The methodological designs of the 18 studies did not permit homogenizing the way of measuring the risk and protection factors associated to the duration of exclusive breastfeeding. The multiplicity, ambiguity, and poor precision of the variables measured become the first point of discussion if valid and applicable results are sought and which are of help in providing healthcare services.
Policies supporting exclusive breastfeeding and strategies implemented for said purpose have somehow been inefficient or perhaps inadequately measured. This aspect is clear in the tendency shown in the practice of breastfeeding to diminish as the child advances in age in the diverse studies evaluated. Studies measuring prevalence at three months did not report figures above 75%. At six months, prevalence reported by the studies included was considerably lower. For Colombia, it is expected that at six months the prevalence of exclusive breastfeeding be at 54%.23 The highest prevalence reported in the studies is of 37%8 and even so, it is low compared to the 50% goal by the World Health Organization (WHO).
It is clear that using the pacifier and/or baby bottle becomes the main risk factor for the duration of exclusive breastfeeding. This commonly accepted cultural practice intervenes in the physiological process of breastfeeding. The infant requires greater effort to suction the milk from the mother's breast toward the mouth and the use of pacifiers and baby bottles changes the sensation and the suction effort disappears.
It is important to indicate that using a pacifier or baby bottle to feed the baby, whether in healthcare institutions or in family environments, generates difficulties for establishing or continuing with the practice of maternal breastfeeding, given that the use of a pacifier or baby bottle can lead the child to decreased sucking frequency, which creates a negative physiological effect on the mammary stimulation and, thereby, on the production of milk. Pacifiers and baby bottles are widely used throughout the world,24 and although the studies included in this systematic review show their negative relation with the duration of maternal breastfeeding; its use has more cultural and family roots. This is how in the social representations of using a pacifier or baby bottle, the inherence of generational practices for the new mother may be concluded; that other women use pacifiers is interpreted as something good for the baby.24 But it is not only a cultural manner, for mothers, pacifiers are a way of soothing the child.25
Some studies indicate the existence of a dosage-response relationship26,27 between pacifier or baby bottle use and the duration of exclusive breastfeeding and, hence, healthcare professionals, who have a big responsibility in promoting and supporting breastfeeding, should in no way promote the use of a baby bottle or pacifier in healthcare institutions or in family environments.24 It is how nurses become key players in promoting and supporting the practice of l breastfeeding.
Adequate training on the topic permits these professionals to understand the importance of breastfeeding within the context of complying with the goals proposed within the Development Objectives of the Millennium, the 10-year Plan on Maternal Breastfeeding, and the National Plan on Public Health. Nurses, as agents providing care and educators in self-care actions, can influence future and current mothers to conduct exclusive breastfeeding. Another one of the variables that negatively affect the duration of maternal breastfeeding, reported with greater frequency by the studies, is that women go to work during the time they are engaged in this type of nutrition. Although culturally and socially women who are dedicated to household chores have lower risks of abandoning the practice tan those who work outside the house, in Colombia, the average duration of maternal breastfeeding among women who work and those who stay at home was the same, 5.9 months.23 Hence, more sound strategies are required that permit breastfeeding mothers to know and practice the diverse forms of collecting and preserving the maternal milk.
Smoking during pregnancy or during the postpartum period was another variable frequently described in the studies included. This factor, measured via meta-analysis, reported an adjusted OR of 1.5 (CI95%: 1.34-1.68), indicating that women exposed to cigarettes have a higher risk of abandoning breastfeeding.28 One of the explanations for this result seems to be founded on the physiological effect of nicotine upon prolactin production.
The social and economic factors different from employment during the period of exclusive breastfeeding turned out contradictory in the diverse studies included. Variables like low socio-economic level were presented as risk factors,13 while at the same time behaving as a protective factor given that maternal milk is a cost-effective option for these mothers;8,21 likewise, maternal level of schooling10,12 presented ambiguities regarding the classification as a variable positively or negatively affecting the duration of exclusive breastfeeding.
The protective factors evaluated in the different studies, like planned pregnancy,15 preference of the father for breastfeeding,15 attendance to prenatal controls,8 educational programs on breastfeeding,11,14 among others, can represent lines of action to promote breastfeeding in public healthcare programs worldwide.
Among the limitations in this study, we have: access only to some electronic databases, leaving aside other databases with special importance, above all for the development of a type of research like a systematic review. This situation could not be waived due to their restricted access; a situation similar to excluding over 45% of the potential studies for the quality review given that they are not freely available for consultation. Also, the methodological heterogeneity of the studies is another important limitation, given that it was not possible to perform statistical analyses that conferred greater validity to the results discussed.
One of the important recommendations in this study is related to adjusting the methodological designs of the studies regarding the categorization of variables to evaluate factors associated to the duration of exclusive breastfeeding. The articles included in this research did not permit evaluating with preciseness and validity what factors affect or protect this practice; and one of the possible ways is by standardizing the variables to evaluate. Awareness and identification of the factors associated to the duration of exclusive breastfeeding may contribute to the formulation of intervention and investigation strategies that permit – on the one hand – improving the negative practices around this type of nutrition; stimulating and promoting those positive practices to accomplish an adequate breastfeeding duration; and on the other hand, identifying those social and cultural dynamics specific of the different groups of women to explore reasons or motivations for not breastfeeding.
REFERENCES
1. Profamilia. Encuesta Nacional de Demografía y Salud 2010. Colombia. Bogotá:Ministerio de la Protección Social; 2011. [ Links ]
2. Ministerio de la Protección Social. Plan Decenal Lactancia Materna. [Internet] . Bogotá: Ministerio de la Protección Social; 2008 [cited 2008 August 2] . Available from: http://www.minsalud.gov.co/alcaldes/Paginas/Plan%20Decenal%20de%20Lactancia%20Materna.aspx [ Links ]
3. álvarez G. Plan Nacional de Salud Pública: Avances y retos en el fortalecimiento de la Salud Pública en Colombia. Bogotá: Ministerio de la Protección Social; 2008. [ Links ]
4. Red Caspe [Internet] . Alicante: Critical Appraisal Skills Programme Español [cited 2012 May 22] . Available from: http://www.redcaspe.org/drupal/ [ Links ]
5. Baltas Z, Arvas A. Factors influencing the duration of exclusive breastfeeding in a group of Turkish women. J Hum Lact. 2001; 17(3):220-6. [ Links ]
6. Leite M, García C, Plácido M. Factores asociados a la situación de lactancia materna exclusiva en niños menores de 4 meses en Botucatu-SP. Rev Latino-am Enfermagem. 2007; 15(1):62-9. [ Links ]
7. Franca G. Brunken G. Da Silva S. Escuder M. Venancia S. Determinantes da amamentacao no primeiro ano de vida em Cuiabá, Mato Groso. Rev Saúde Pública 2007; 41(5):711-8. [ Links ]
9. Vannuchi M. Thomson Z. Escuder M. Tacla M. Vezozzo K. De Castro L. et al. Perfil do aleitamento materno em menores de um ano no municipio de Londrina, Paraná. Rev Bras Saúde Matern Infant. 2005; 5(2): 155-62. [ Links ]
10. Barria M. Santander G. Victoriano T. Factors associated with exclusive breastfeeding at 3 months postpartum in Valdivia, Chile. J Hum Lact. 2008; 24(4):439-45. [ Links ]
11. Gijsbers B. Mesters I. Knottnerus A. Schayk C. Factors associated with the duration of excluisve breastfeeding in asthmatic families. Health Educ Res. 2008; 23(1):158-69. [ Links ]
12. Al Tajir H. Sulieman H. Badrinath P. Intragroup differences in risk factors for breastfeeding outcomes in a multicultural communitiy. J Hum Lact. 2006; 22(1):39-47. [ Links ]
13. Mascarenhas M. Albernaz E. Da Silva M. Silveira R. Prevalence of exclusive breastfeeding and its determiners in the first 3 months of life in the South of Brazil. J Pediatr (Rio J). 2006; 82(4):289-94. [ Links ]
14. Bliss M. Wilkie J. Acredolo C. Berman S. Tebb K. The effect of discharge pack formula and breast pumps on breastfeeding duration and choice of infant feeding method. Birth. 1997;24(2):90-7. [ Links ]
15. Scott J. Binns C. Oddy W. Graham K. Predictors of breastfeeding duration: evidence from a cohort study. Pediatrics. 2006; 117(4):e646-55. [ Links ]
16. Lawoyin T. Olawuyi J. Onadeko M. Factors associated with exclusive breastfeeding in Ibadan, Nigeria. J Hum Lact. 2001;17(4):321-5. [ Links ]
17. Do Nascimiento M. Moura M. Franco S. Issler H. Ferraro A. Grisi S. Exclusive breastfeeding in Southern Brazil: Prevalence and associated factors. Breastfeed Med. 2010; 5(2):79-85. [ Links ]
18. Cernadas J, Noceda G, Barrera L, Martinez A, Gards A. Maternal and perinatal factors influencing the duration of exclusive breastfeeding during the first 6 months of life. J Hum Lact. 2003;19(2):136-44. [ Links ]
19. Howard C. Howard F. Lanphear P. Blieck E. Eberly S. Lawrence R. The effects of early pacifier use on breastfeeding duration. Pediatrics. 1999; 103(3):E33. [ Links ]
20. Lee W. Wong E. Lui S. Chan V. Lau J. Decision to breastfeed and early cessation of breastfeeding in infants below 6 months old-a population-based study of 3204 infants in Hong Kong. Asia Pac J Clin Nutr. 2007;16(1):163-71. [ Links ]
21. Kaneko A. Kaneita Y. Yokoyama E. Miyake T. Harano S. Suzuki K. et al. Factors associated with exclusive breastfeeding in Japan: for activities to support child-rearing with breastfeeding. J Epidemiol. 2006; 16(2):57-63. [ Links ]
22. García J, Ramirez N. Factores asociados a la lactancia materna exclusiva en población pobre de áreas urbanas de Colombia. Rev. Salud Pública. 2008; 10(1):71-87. [ Links ]
23. Cabrera G, Mateus J, Giron, S. Duración de la lactancia exclusiva en Cali, Colombia. Colomb Med. 2004; 35(3):131-37. [ Links ]
24. Lamounier J. O efeito de bicos e chupetas no aleitamento materno. Jornal de Pediatria [revista en internet] 2003; 79(4):284-6. [ Links ]
25. Sertorio S. Silva I. The symbolic and utilitarian facets of pacifiers according to mothers. Rev Saude Publica. 2005; 39(2):156-62. [ Links ]
26. Soares M. Giugliani E. Braun M. Salgado A. Oliveira A. Aguiar P. Uso de chupeta e sua relacao com o desmame precoce em populacao de criancas nascidas em Hospital Amigo da Crianza. J Pediatr (Rio J) 2003;79(4):309-16. [ Links ]
27. Susin L. Giugliani E. Kummer S. Influence of grandmothers on breastfeeding practices. Rev Saude Publica. 2004. [citado 05 de febrero de [ Links ]
28. Horta B. Kramer M. Platt R. Maternal Smoking and the Risk of Early Weaning: A Meta-Analysis. Am J Public Health. 2001; 91(2):304-7. [ Links ]