Introduction
Diseases of cardiovascular origin are among the main causes of death in Colombian, Latin American and general populations; these have an important relationship with dyslipidemias, and according to figures from the National Institute of Health, are the leading cause of death in the country1.
Several epidemiological studies in apparently healthy Colombian populations have found a cardiovascular risk profile similar to that of developed countries, highlighting an elevated prevalence of hypercholesterolemia2-4. According to these reports, in Colombia, mixed dyslipidemia (hypercholesterolemia + hypertriglyceridemia) is the most frequent type of dyslipidemia (46.6%), in addition to being present in patients with a high cardiovascular risk (on average, a 14% 10-year risk according to the Framingham stratification). The risk factors that most frequently coexisted in this population were hypertension (93.2%), diabetes mellitus (28.5%), a personal history of cardiovascular disease (16.7%), and advanced age5. Since the publication of the Colombian clinical practice guidelines for the management of hypercholesterolemia in 2014, the prevalence and proportion of use of lipid-lowering therapies have not been measured2. However, numerous studies have shown that a very low proportion of dyslipidemic patients used lipid-lowering medications as often and for as long as their physicians prescribed6,7.
Statins and fibrates are mainly used for the management of dyslipidemias; statins are used to treat hypercholesterolemia and control cardiovascular risk, having a positive impact on major cardiovascular outcomes8; this group of medications is a pillar of the management of cardiovascular pathologies. In addition, recently published studies show that about 78% of statins used in Colombia are of high potency, leading to greater cardiovascular protection, with atorvastatin being the most widely used medication9.
The objective of this study was to establish the prevalence or proportion of the use of lipid-lowering drugs in a Colombian population during 2016.
Methods
A cross-sectional study was conducted on the use of lipid-lowering medications through a drug claims population database of people affiliated with the Colombian Health System among four insurers of the contributory regime with a presence throughout the country. This health system is divided between a subsidized regime (paid by the Colombian state) and a contributory regime (paid by the workers and employers contribution). All patients older than 18 years and of any gender who were regularly attending medical care for dyslipidemia or cardiovascular risk factors and received lipid-lowering treatment were included in the study.
We considered all the patients who received the drug over the course of 6 months (January-June 2016) to establish the prevalence of the use of lipid-lowering drugs. From the information on drug consumption systematically and uninterruptedly captured by the company that distributes it to the affiliated population, we collected the following groups of variables from the patients to whom drugs were distributed during the observation period:
1. Sociodemographic variables: age and sex.
2. Lipid-lowering drugs dispensed: (a) statins alone or in combinations, (b) fibrates, (c) cholestyramine, (d) ezetimibe, and (e) nicotinic acid. All statins, gemfibrozil, and cholestyramine are covered by the 2016 health benefits plan. For all other lipid-lowering medications, a justified request must be submitted to be dispensed by the health system10.
Data analysis was performed in SPSS Statistics, version 24.0 (IBM, USA) for Windows. Univariate analyses were performed to assess frequencies and proportions of categorical variables and measures of central tendency, position, and dispersion for the quantitative variables.
The study was classified as a risk-free investigation, ethical principles established by the Declaration of Helsinki were respected, and individual informed consent was not required for each patient.
Results
From a population of 4,328,688 patients, a total of 282,002 were prescribed a lipid-lowering drug during the 6 months of observation. The mean age was 64.2 ± 13.3 years and women comprised 50.4% of users. The population distribution by age is shown in figure 1.
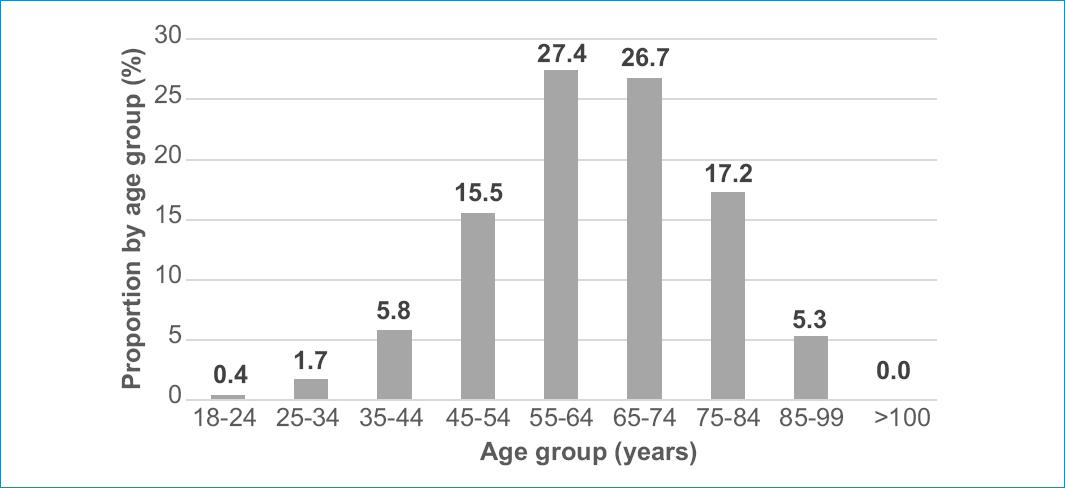
Figure 1 Distribution by age group of 282 002 patients under treatment with lipid-lowering drugs in Colombia, 2016.
The estimated prevalence of lipid-lowering drug use was 6.5% within the general population. Statins were the most commonly used lipid-lowering drugs at 86.3%, with a predominance of atorvastatin (81.0%) followed by lovastatin (14.4%) and rosuvastatin (4.4%) (0.2% other statins). The second group in terms of frequency of use was fibrates at 13.1% (particularly gemfibrozil, which accounted for 91.9% of the cases), and finally, 0.6% of the patients used ezetimibe. No patients consumed nicotinic acid.
Discussion
The present study was able to identify the prevalence of the use of lipid-lowering drugs in a Colombian population, presenting valuable information for decision-making by those involved in healthcare and the rational use of health system resources.
The prevalence of dyslipidemia has been estimated at 16.8% in Korea, 41.6% in Iran, 45.0% in Canada, 44.0% in Brazil, and 35.3% in some regions of Colombia11-15. According to data from the World Health Organization in the Americas, the prevalence of elevated cholesterol in men ranges from 31.8% to 56.1%, and in women, the prevalence for the northern zone is between 37.5% and 54.3%16. In Germany, it was estimated that 30.8% of adults with dyslipidemia received pharmacological treatment17, which, when compared with our 6.5% result, indicates that the frequency of use of lipid-lowering drugs is probably lower than expected for the Colombian population. These findings are worrying, as they may indicate underdiagnoses of dyslipidemia and under-utilization of lipid-lowering agents in patients when indicated, considering additional benefits that go beyond reduced blood lipids8.
Additional cardiovascular benefits could be obtained by extending the use of these drugs to patients with high cardiovascular risk or dyslipidemia who are not in pharmacological management, as these drugs interact with statins and their pleiotropic effects8,18,19. Research also supports all statins being included in the benefits plan of the Colombian Health System10, including atorvastatin, a high-potency statin that is the most commonly used in Colombia9.














