Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em
SciELO
Similares em
SciELO -
 Similares em Google
Similares em Google
Compartilhar
Revista Facultad de Ingeniería Universidad de Antioquia
versão impressa ISSN 0120-6230
Rev.fac.ing.univ. Antioquia no.68 Medellín jul./set. 2013
ARTÍCULO ORIGINAL
Automated design of customized implants
Diseño automatizado de implantes personalizados
Vicente Chulvi*1, David Cebrian-Tarrasón1, Álex Sancho2, Rosario Vidal1
1Deparatamento de Ingeniería Mecánica y Construcción, Universitat Jaume I. 12071. Castellón, España.
2Fundación ASCAMM. 08290. Cerdanyola del Vallès, Barcelona, España.
*Autor de correspondencia: teléfono: + 34 + 964 + 72 81 13, fax: + 34 + 964 + 72 81 06, correo electrónico: chulvi@uji.es.co (V. Chulvi)
(Recibido el 1 de mayo de 2011. Aceptado el 5 de agosto de 2013)
Abstract
This paper presents a model capable of design a customized cranial implant directly from a medical imaging process, whose output will be a file in a manufacture system recognizable format.
The proposed system has been created by linking two computer prototypes developed during the present research and studying the inner and outer related technologies. The core of the model is the KBS (Knowledge Based System) technology, able to store and manage medical data, as well as designer knowledge, in order to use this information in the implant design process. The aim of this project is to obtain a tool to improve the design process, the biocompatibility with patient and reduce final costs, which can be operated without necessity of wide knowledge from the user.
Keywords: Cranial implants, KBS, CAD, intelligent design, rapid prototyping
Resumen
Este artículo muestra un modelo que se postula como capaz para el diseño de un implante craneal personalizado directamente desde el proceso de toma de imágenes médica. La salida de este proceso de diseño se conseguirá en un formato capaz de ser reconocido por el sistema de manufactura.
El sistema propuesto se ha creado a partir de la unión de dos prototipos informáticos desarrollados durante la presente investigación, y a través del estudio de las tecnologías relacionadas o circundantes. El núcleo del modelo en la tecnología basada en el conocimiento (KBS), que debe permitir de almacenar y gestionar datos médicos y de diseño para poder aplicar dichos conocimientos durante el proceso de diseño del implante. El objeto de este proyecto es el de obtener una herramienta para mejorar el proceso de diseño, la biocompatibilidad con el paciente y reducir los costes finales, y que pueda ser operado sin necesidad del conocimiento completo de todas sus fases por el usuario.
Palabras clave: Implantes craneales, KBS, CAD, diseño inteligente, prototipado rápido
Introduction
The close future paradigm of medical industry will be surgical operations in which implants are fully adapted to the particular requirements of each patient. This vision will be fulfilled when new biomaterials are developed and new technologies for design and rapid manufacturing of such implants are implemented [1]. Patients exert more and more pressure in order to improve operation, duration and aesthetics of implants, and so are scientific working. Nowadays the techniques for the manufacture of implants are based on individual experience and point of view of surgeons and mechanics. Low resolution of current medical data acquisition techniques together with manual mechanizing result in slow and expensive final results [1-3].
The first reference about custom designed implants was provided by Dooley et al. [4]. It was a theoretical approach to intelligent systems to develop orthopaedic implants which could be incorporated into a design and manufacture system. A few years later Whittaker [5] presented a model in an attempt to automatize the process, which results in a slight improvement but not an automated process. Despite that, this approach is not so far from present models [6-8].
The procedure to automatize the process of customized craniofacial implant design begins with medical data acquisition using the most common techniques of 3D and 4D-image projection. Data provided with CT (Computerized Tomography) or MRI (Magnetic Resonance Imaging) are represented in a set of plane images (2D). Each image represents a transverse slice of the exploration area. Therefore, surgeons have to examine simultaneously a considerable amount of images in order to rebuild the 3D shape in their mind, what means an added difficulty to design. Rebuilding 3D shape from 2D medical data is a field of study under development [9]. The last step through the procedure of customized implant design consists in the development of an output file through CAD/CAM/CAE (Computer Aided Design / Computer Aided Manufacturing/ Computer Aided Engineering) technology [1012], which can be sent to a manufacturing machine. However, the incorporation of relatively new technologies to the automated design process, like FEM (Finite Element Method) simulation [13], tissue engineering scaffolds [14-15] and RP (Rapid Prototyping) [16-17], have turned it into a novel field, where different disciplines take part: medicine, computing, design and engineering.
Although research on custom implants is narrowing its scope to focus on specific types of implants, no studies have been found that deal with specifically the automated design of craniofacial implants. This fact shows the difficulty to create a system that considers all the steps of the process. So, the aim of the present study is to deal with the technical design and implementation of software, which accelerates the medical implants' design process through the use of CAD (Computer Aided Design) and KBE-based tools (Knowledge Based Engineering). The purpose is to obtain a remarkable improvement both for patients and for service suppliers. The experimental results presented in this article show two computer applications, the first of them is aimed to create an STL (Stereolithography) format file from a CT scan file, and the second one develops an automated model of a volume to cover existing holes on a surface, beginning with a surface that could be the previous STL file.
Materials and methods
This research was based on the previous study of existing softwares (such as MIMICS, 3D Slicer, ImLib3D, MITK, OsiriX and Visualization Toolkit) and a study about materials used for implant manufacture and the existing techniques to carry it out.
Medical imaging is based on projection technologies. CT consists in an X-ray beam that crosses the analysed body and its projection is detected varying the attenuation in function of the density of the tissues gone through. Soft tissues will appear dark and bones will appear light. The result is a transversal section, a 2D projection of tissues along X-rays direction. MRI is a similar technique, but it uses a magnetic field instead of an X-ray beam. The result is also a transversal section 2D image. Nevertheless, one medical image has no sense on its own, but different images of the same patient can be related to each other and, moreover, have associated a set of patient data. Current image formats (TIFF, JPEG or GIF) are not enough. For that reason, it was proposed that the image processing of the present research follows the DICOM (Digital Imaging and Communications in Medicine) standard. This standard describes the files format and the specification of patient primordial data in an image, just as the required header, showing a common language to the different medical systems. Images come enclosed with measurements, calculations and other relevant descriptive information, as patient's name, birth date, data acquisition equipment, image size, pixel data, contrast used, etc.
The first computer application was defined as a prototype for reconstruction of a 3D image from a set of 2D DICOM images and conversion of VTK (Visualization Toolkit) format to an STL, which is recognizable for CAD programs. 3D Slicer is the most well known open source application found for visualization, medical data segmentation and 3D medical images reconstruction from DICOM files, and it has been developed over the graphic library OpenGL, using VTK for image processing. MIMICS (Materialised Interactive Medical Image
Control System) is an interactive commercial tool for the visualization and segmentation of CT images as well as MRI images and 3D rendering of objects. VTK is an open source library for computer visualization of images and graphics, at a higher level of abstraction than other rendering libraries, OpenGL or PEX. VTK applications can be directly written in C++, Tcl, Java or Python. Design and implementation of the library have been strongly influenced by oriented-to-objects programming principles. Operations on two or three dimensions and model generation could be carried out by this library with a few lines of code.
The technologies needed for the development ofthe second computer application, which must be able to realize an automated design of an implant, are KBS and CAD. There exist software applications based jointly in KBE and CAD. Their respective KBS modules only use the systems capacities associated to control of geometry variables, reutilization of geometry information and control and management of rules and restrictions. This feature provides the advantage of no excessive expert knowledge in KBS required for application development in an efficient manner. The present application was developed using the CATIA software suite, which has a module structure with specialized functions groups. It allows development applications based on both KBS and CAD, integrating the modules through APIs (Application Programming Interface) program libraries. In CATIA, the ''Knowledgeware'' module groups the functions related with knowledge (e.g., parameterize elements, create formulas or rules, check, etc.), and allows it to expand design features with knowledge elements. CATIA disposes of an FEM module (in the CAE section), which gives the opportunity to analyse the response and evolution of a physical system under simulated conditions of load, initial and boundary conditions, assuring the integration with the KBS. In the particular case of implants, FEM is used for strain an effort analysis from a given force field and evaluation of bone growth. Furthermore, there is the chance to predict the facial appearance after surgery through an FEM model applied to soft tissue.
The output of CATIA is presented in STL format, which allows to be directly transferred into an RP (Rapid Prototiping) machine. RP is the name given to the technology set used for three-dimension manufacture, directly from CAD data source. This system drives to a design improvement, as well as time manufacture reduction, better material use and excellent tolerances. A review of RP techniques applicable to implant manufacture can be seen in past research [18].
Results (development of the model)
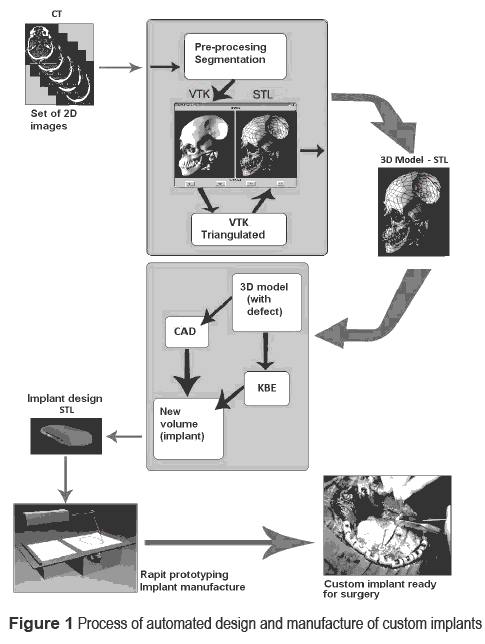
Figure 1 illustrates the global process of automated design and manufacture of customized implants, as has been considered in the present work. Processes enclosed inside the shaded boxes represent the two software prototypes designed during the project development. The procedure of customized craniofacial implant design began with medical data acquisition with the already mentioned technology of CT. This process provided a set of two-dimension images (transversal slices). In order to reconstruct the three-dimension model, medical images must be treated. There exist two main steps in order to obtain the desired results, that we named preprocessing and segmentation.
During the first step of the pre-processing, there was an attempt to improve the image as much as possible, since images from CT have a considerable quantity of ''noise''. Transverse slices are frequently performed in all organs and tissues within the exploration range. A previous process, segmentation, is needed to select the objects of the organ or tissue considered whose transformation to 3D is desired. Tissues (bone, skin, encephalic mass, etc.) can usually be differentiated by the grey scale represented in the medical image, in the segmentation process it is usual to select a point in a region to be transformed, and its value in the grey scale is used as a reference value.
Once the area to be treated was selected, the procedure continued with the 3D model building. Each transversal slice image is composed by a bidimensional matrix of pixels, each one having a (x, y) position. If individual images are overlaid, the pixels in every image for given (x, y) coordinates will be aligned. Thus, pixels can be labelled with three dimensional coordinates. They maintain their original (x, y) coordinates and take a new z coordinate. The z coordinate is simply the slice number to which pixels are associated. The concept of slices is eliminated and all pixels of all the images are represented in a unique three-dimensional image. The new volume unit so created is called voxel (which is a portmanteau word from volumetric and pixel), which dimensions are 1 pixel wide x 1 pixel height x 1 pixel length.
Since most of the applications in open source capable of treating medical images and convert those into a 3D geometry are based on VTK, the next step was to develop a module to convert the VTK file into an STL file, that CAD programs could recognise it. This development began with the installation of the VTK library, which requires the compilation of the VTK source code (in order to generate C++ libraries) and VTK wrapping code (to generate executables in Java, Tcl and Python). TKinter library - DLL (Dynamic-link library) - for Python, which is an open source library used to develop user interfaces, has been used to develop the interface.
The first action carried out by the algorithm is to create a vtkTriangleFilter type object. This object has a method that allows triangulating a VTK model. Previous to the creation of the STL model, the triangulation of VTK object must be done since STL format only accepts triangular faced models. Subsequently, a vtkSTLWriter type object was created, which has a function that allows converting a triangulated VTK model to STL format.
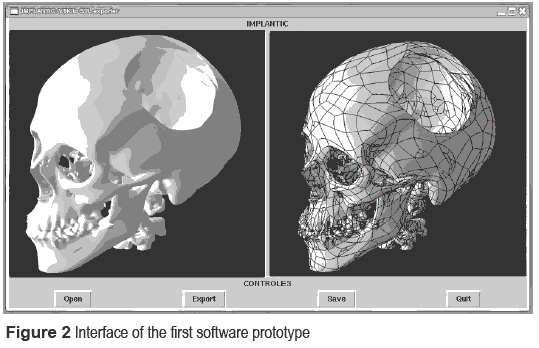
The first computerprogram developmentincludes the steps of pre-processing, segmentation, 3D building and file format conversion. This is, in general lines, a prototype to recognize data and convert them in a recognizable format for CAD software. As shown in the figure 2, the interface of the prototype has two graphic windows, where the model can be visualized both in VTK format and STL (triangulated) format. Once the STL model appears in the corresponding graphic window, it could be saved in that format and be retrieved in any CAD software.
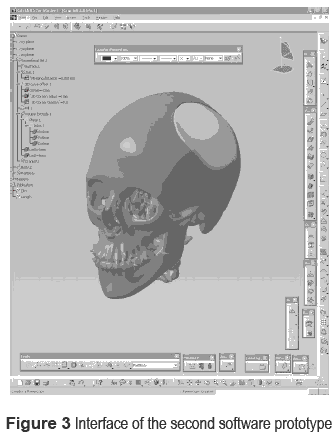
The next step consisted in developing a second computer program prototype through CATIA software, which models automatically a volume to cover a hole in an object. The use of the 3D STL model from the first computer program prototype showed the possibility to create a custom implant design adapted to the patient's anatomy, improving structural, functional and aesthetic biocompatibility. The modelling of the prototype requires, firstly, the manual definition and testing of all the steps of the modelling in order to ensure that is working correctly. These steps are: locate the hole(s) on the surface by means of object geometrical boundaries analysis; set the gap from the hole boundaries that will be the outline of a new area; create the area that will become the outer surface of the implant, considering the curvature radius of the hole's zone; and extrude a volume from the surface. Once the manual process is done, the automation of these steps is done through the knowledge management module. Most of the instructions used by the program are developed through APIs. Once the modelling process had been defined, instructions are recorded into a macro in a code recognised by CATIA by means of language VBScript. In order to conclude the customized design for final user, some geometrical rules and restrictions can be included in the prototype by means of databases, like ''gap between hole (cranium defect) and modelled volume (implant)'' and ''thickness''. The result of running the program is shown in figure 3, as it is viewed in CATIA's interface. Finally, the resulting implant must be exported into a format compatible with the manufacturing process, rapid prototyping in our case. The format used in this case is STL, an instruction has been added to the algorithm in order to save the implant in a file ready to be transferred to an RP machine.
Discussions
The model, as shown in figure 1, has been built from two software prototypes, which have been linked for the final result. The first software prototype was to convert medical images to a 3D model in STL format. This application improves those existing in the market since it not only reconstructs a 3D image from a set of 2D image, but also prepares it for being used in next design steps. Therefore, the advantage of the first software prototype consists in time reduction and less human manipulation. The second software prototype comprises the automated implant design process. Initial tests show that the creation of a cover for a hole (this is, an implant) over a cranium is possible in an automatic mode by means of KBS. However, medical knowledge should be broadened in order to optimize the KBS database, which should make it possible to differentiate natural skull holes from defects, recognize cranial zone affected, set implant width and mechanical properties in function of cranial zone, etc.
Along with the advantages mentioned above, RP allows raising the proposal of using the technology of tissue engineering scaffolds, in which an implant is used as a ''scaffold'' that will work as a base to regenerate the tissue [19]. This ''scaffold'' form can be achieved with RP techniques, which allow to control independently the porosity and the pores' size by varying the working parameters of the machine. Figure 4 shows the aspect of an application of this kind of technique. Within this same proposal, the use of biomaterials can be taken into consideration, creating implants combining bio-stable polymers with bio-degradable polymers, that at the same time the regenerated tissue fills the existing pores in the implant and new pores are created in order that the tissue can continue its expansion. The material proposed as a bio-stable polymer is PEEK (Poli-ether-ether-ketone), which is used at present in implant manufacturing and has been tested in RP manufacturing, and the material proposed as bio-degradable is HA (Hidroxiapatite), natural bone component that has been experimentally tested together with PEEK using scaffolds technology [20].
Conclusions
The present work presents a process to improve the automated design and manufacture of customized cranial implants. The results showed that a computer application for automated design of customized cranial implants will provide numerous advantages, both for customers as well as for surgeons, manufacturers and designers. Custom implants will improve functional and structural biocompatibility, aesthetic, functionality, quality of life, and they can also provide a less invasive surgery. Automating the process would lead, ostensibly, to reduction in design and manufacture time and consequently to lower costs, which provides new market opportunities.
Society in general demands those advantages, and they will become a serious necessity in a near future. The computer software prototypes presented in this article, as well as the proposals developed during the research, establish the essential bases for the final ideal application.
Acknowledgments
The research presented in this paper was partially funded by the Ministerio de Industria, Turismo y Comercio of Spain (project ref. FIT-300100- 2006-64) and by the Ministerio de Educación y Ciencia of Spain (project ref. DPI2006- 15570-C02).
The authors also gratefully acknowledge the cooperation of the staff of Plastiasite, S.A., Neos Surgery, S.L. and Fundación ASCAMM.
References
1. M. Cabrera, J. Burgelmen, M. Boden, O da Costa, C. Rodríguez. eHealth in 2010: Realising a Knowledge- based Approach to Healthcare in the EU. European Commission Directorate-General Joint Research Centre Technical Report EUR 21486. Seville, Spain. 2004. [ Links ]
2. P. D'Urso, W. Earwaker, T. Barker, M. Redmond, R. Thompson, D. Effeney, F. Tomlinson. ''Custom cranioplasty using stereolithography and acrylic''. British Journal of Plastic Surgery. Vol. 53. 2000. pp. 200-204. [ Links ]
3. H. Eufinger, C. Rasche, M. Wehmoller, K. Schmiederc, M. Scholzc, S. Weihed, P. Scherera. ''CAD/CAM titanium implants for cranioplasty--an evaluation of success and quality of life of 169 consecutive implants with regard to size and location''. Computer Assisted Radiology and Surgery. Vol. 1281. 2005. pp. 827-31. [ Links ]
4. R. Dooley, G. Heimke, A. Dingankar, E. Berg, E. Kimbrough. ''Automated design and analysis system for design of custom orthopedic implants''. Proceedings of the first international conference on Industrial and engineering applications of artificial intelligence and expert systems. Vol. 1. 1988. pp. 405-12. [ Links ]
5. D. Whittaker. ''Custom-designed hip implants through knowledge-based engineering''. Materials & Design. Vol. 12. 1991. pp. 103-4. [ Links ]
6. O. Tziovaras. Customised implant design for the knee joint. X Congreso Internacional de Ingeniería de Proyectos. Valencia, España. 2006. pp. 630-635. [ Links ]
7. T. Wu, L. Fietena, M. Engelhardt. ''Knowledge-based individual implant design based on reference models for craniofacial reconstruction''. International Journal of Computer Assisted Radiology and Surgery. Vol. 1. 2006. pp. 259-61. [ Links ]
8. A. Rose, M. Klein, T. Krueger. Individual bone implant modeling using planned resection lines for facial and cranial tumor resection. 4th European Conference of the International Federation for Medical and Biological Engineering. Ed. Springer Berlin - Heidelberg. Berlin, Germany. Vol. 22. 2009. pp. 944-947. [ Links ]
9. J. Gao, W. Xu, Z. Ding. ''3D finite element mesh generation of complicated tooth model based on CT slices''. Computer Methods and Programs in Biomedicine. Vol. 82. 2006. pp. 97-105. [ Links ]
10. M. Truscott, D. de Beer, G. Booysen, L. Barnard. Bone Development through CT/CAD/CAM/RP. 10èmes Assises Européennes de Prototypage Rapide. AFPR - Association Française de Prototypage Rapide. Paris, France. 2004. pp.107-114 [ Links ]
11. S. Singare, L. Yaxiong, L. Dichen, L. Bingheng, H. Sanhu, L. Gang. ''Fabrication of customised maxillo- facial prothesis using computer-aided design and rapid prototyping techniques''. Rapid Prototyping Journal. Vol. 12. 2006. pp. 206-13. [ Links ]
12. L. Hieu, N. Zlatov, J. Vander, E. Bohez, L. Khanh, P. Binh, P. Oris, Y. Toshev. ''Medical rapid prototyping applications and methods''. Assembly Automation. Vol. 25. 2005. pp. 284-292. [ Links ]
13. J. Ho, S. Kleiven. ''An automatic method to generate patient specific finite element head model''. Journal of Biomechanics. Vol. 39. 2006. pp. S428-S. [ Links ]
14. B. Starly. Biomimetic design and fabrication of tissue engineered scaffolds using computer aided tissue engineering. PhD Thesis. Drexel University. Philadelphia, Pennsylvania, USA. 2006. [ Links ]
15. S. Lohfeld, V. Barron, P. McHugh. ''Biomodels of bone: a review''. Annals of Biomedical Engineering. Vol. 33. 2005. pp. 1295-1311. [ Links ]
16. I. Gibson, L. Cheung, S. Chow, W. Cheung, S. Beh, M. Savalani, S. Lee. ''The use of rapid prototyping to assist medical applications''. Rapid Prototyping Journal. Vol. 12. 2006. pp. 53-58. [ Links ]
17. M. Naing, C. Chua, K. Leong, Y. Wang. ''Fabrication of customised scaffolds using computer-aided design and rapid prototyping techniques''. Rapid Prototyping Journal. Vol. 249. 2005. pp. 259. [ Links ]
18. V. Chulvi, C. Muñoz. Prototipado rápido + PEEK = Andamios para huesos. XI Congreso Internacional de Ingeniería de Proyectos (AEIPRO). Lugo, España. 2007. pp. 602-612. [ Links ]
19. A. Lipowicz. ''Advanced methods of hard tissue scaffold and implant fabrication''. Journal of Biomechanics. Vol. 39. 2006. pp. S216 [ Links ]
20. G. Converse, W. Yue, R. Roeder. ''Processing and tensile properties of hydroxyapatite-whisker- reinforced polyetheretherketone''. Biomaterials. Vol. 28. 2007. pp. 927-935. [ Links ]