Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em
SciELO
Similares em
SciELO -
 Similares em Google
Similares em Google
Compartilhar
Acta Neurológica Colombiana
versão impressa ISSN 0120-8748
Acta Neurol Colomb. vol.29 no.2 Bogotá abr./jun. 2013
Caso clínico
Meningoencefalitis por neurotoxocarosis
Neurotoxocarosis, a meningo-encephalitis
Patricia Quintero Cusguen, Ángela María Gutiérrez Álvarez
Patricia Quintero-Cusguen MD. Unidad de Neurología, Hospital Universitario de La Samaritana, Bogotá-Colombia. NEUROS Grupo de investigación de la Universidad del Rosario, Bogotá-Colombia.
Ángela María Gutiérrez-Álvarez MD MSc. Servicio de Neurología, Hospital Santa Bárbara, Soria, España.
Correspondencia: angelam.gutierrez@gmail.com
Recibido: 11/01/13. Revisado: 15/02/13. Aceptado: 21/02/13.
RESUMEN
La toxocariasis humana es causada por la migración a todo el organismo de la larva de Toxocara y se manifiesta por una gran variedad de síntomas. La infección del sistema nervioso central se determina por la presencia de síntomas neurológicos asociados a un diagnóstico histopatológico, parasitológico o a una prueba de inmunodiagnóstico positiva en suero o líquido cefaloraquídeo. Este reporte describe un caso de neurotoxocariasis que se manifestó con cefalea y epilepsia. La paciente vivía en un hogar humilde con sus dos hijos y cuatro cachorros, lo que aporta una información epidemiológica positiva e importante. Se encontraron anticuerpos anti Toxocara canis positivos en sangre de la paciente y los estudios de serodiagnósticos también fueron positivos para sus hijos. Este artículo pretende hacer una breve revisión sobre esta rara helmintozoonosis; resume los aspectos epidemiológicos más importantes y presenta las formas de diagnóstico y tratamiento disponibles.
PALABRAS CLAVE: Toxocara; Toxocara canis; Epidemiología, Sistema Nervioso (DeCS).
SUMMARY
Human toxocariasis is due to Toxocara species larvae migration through their organism, causing a great variety of symptoms. Central nervous system infection is defined by neurologic symptoms in conjunction with histopathological or parasitological diagnosis, a positive immunodiagnostic test result for serum or cerebrospinal fluid. This report describes one case of neurotoxocariasis manifested by headache and epilepsy. The patient lived in a modest home with her sons and four puppies thereby providing positive epidemiological information. The patient’s blood revealed positive anti-Toxocara canis antibodies. Serodiagnosis studies of her sons also proved positive. This paper attempts giving a synoptic overview of this almost unknown helminthozoonosis; summarises the most important epidemiological parameters and presents the diagnostic and therapeutic possibilities available today.
KEY WORDS: Toxocara canis, Toxocara, Epidemiology, Nervous system (MeSH).
INTRODUCTION
Toxocarosis is caused by a roundworm (nematode) called Toxocara canis, a systemic parasitosis of dogs, wolves, foxes which can infest human beings (1). It usually appears as visceral larva migrans. It is rarely or very infrequently found that the central or peripheral nervous system is compromised (2). The frequency with which the central nervous system (CNS) is affected really remains unknown; there have been cases where it has not been accompanied by neurological manifestations in spite of there having been positive anti-Toxocara Canis antibodies in cerebrospinal fluid (CSF) (3). Several studies have found that coming into contact with dogs has been associated with increased seroprevalence level and an increased risk of developing toxocarosis. It has been reported that the risk of toxocarosis increases threefold if a dog is present in the household and increases over fivefold if a litter of puppies has been present in the house (4). This paper reports a patient with neurotoxocarosis and tries to give a synoptic overview of direct contact with dogs as a risk factor for this almost unknown helminthozoonosis.
Presentation of case
A female, 46 year-old patient consulted as she presented versive crisis with secondary generalisation. She was referred having two months’ evolution, overall headache, vomiting on many occasions, diplopia and loss of strength/sensitivity in the right hemibody during the 20 days prior to consultation. She also presented non-specific abdominal pain.
Neurologic examination revealed bilateral paresis of the sixth nerve, nuchal rigidity and right hemiparesis and hemihypoesthesia.
The patient lived in a modest home with her sons and four puppies thereby providing positive epidemiological information.
The above clinical picture and the suspicion of a meningeal process and intracranial hypertension led to studying this patient.
Haemogram on being admitted: 8,130 leuc; 71% N; 18% L; 0.5% E; 15.5 g/dl HB; 47% HCT; 217,000 platelet count, negative VDRL. Electrolites: 140 mEqL sodium; 3.8 mEqL potassium; 105 mEqL calcium; non-reactive HIV. IgG toxoplasma in sera: positive 1/256.
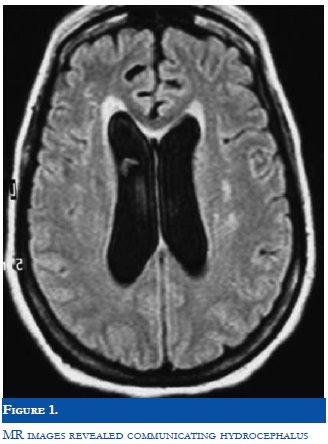
CT scan and MR images revealed communicating hydrocephalus (Figure 1).
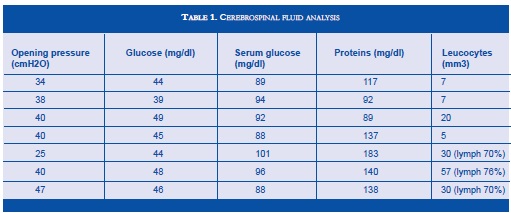
Lumbar punctures: high opening pressures, hypoglycorrachia and hyperproteinorrachia (Table 1). PCR for TBC, KOH - BK- cryptococus and histoplasma were negative, ADA in CSF 0U/L. Negative cytology of CSF - PCR for TBC - coccidioidomycosis - histoplasma - fungal and cysticercosis culture, toxoplasmosis IgM, were also negative.
A few days later, the results from analysing the patient’s blood revealed positive anti-Toxocara canis antibodies (1.79). Any index equal or greater than 1.1 is considered positive. Treatment was started with albendazole and methylprednisolone. Her further clinical course, however, was not satisfactory; she suffered progressive clinical deterioration and then died. Serodiagnosis studies of her sons also proved positive (2.278 and 3.291 ); treatment was thus given to both of them.
DISCUSSION
Toxocara Canis seroprevalence is especially high in developing countries, especially in rural areas and some tropical regions. However, such disease often goes undiagnosed due to not being recognised by physicians or because appropriate testing is not available. The infection route is oral, caused by accidently consuming infected eggs before they hatch in the first portion of the intestine (due to geophagia from consuming contaminated raw vegetables or fruit as well as from poor personal hygiene). The larvae pass through the intestinal mucosa and reach the whole organism via the circulatory system. The symptoms depend on the affected tissue and/or organ, the severity of infection and the degree of the immune response so induced. Children become more frequently affected than adults (2). Clinically, it causes alterations such as fever, respiratory symptoms, muscular and abdominal pain, hepatomegaly, accompanied by high eosinophilia and high anti-Toxocara antibody titres. The severity of damage and inflammation of the CNS is related to the number of larvae entering the brain. A diagnosis of neurotoxocariasis is based on several findings: high T. canis antibody serum titres, eosinophilia in blood or CSF and close contact with dogs. The clinical spectrum of CNS toxocariasis involves syndromes such as eosinophilic meningoencephalitis, encephalitis, lesions occupying extramedular spaces, cerebral vasculitis, epilepsy and behaviour disorders (5).
Interestingly, our case did not present peripheral nor central eosinophilia. The absence of eosinophilia does not rule out a diagnosis of toxocariasis; a negative spinal fluid test result does not rule out CNS involvement. A definitive laboratory diagnosis can be achieved by pathology examination of various organ specimens, including liver, brain, or the lungs. Cerebral CT and MRI findings in neurotoxocariasis are usually non-specific.
Neurological manifestations of toxocariasis are treated with benzimidazole components, usually being albendazole, corticosteroids or diethylcarbamazine. Prognosis is usually favourable if the disease is diagnosed and treated early.
Toxocara canis epidemiology has been studied in humans and an association between having direct contact with dogs and toxocariasis has been proposed, especially if dogs are under 1 year of age (4). Some authors have proposed that humans may become infected through ingesting embryonated eggs which have been picked up directly from a dog’s coat. Owning a dog has been significantly associated with seropositivity to anti-Toxocara antibodies. The infection rate tends to decrease with an animal’s increasing age, being lower in well-cared for pet dogs. Anthelmintic drug intervention for puppies within the first weeks of life, regulations for preventing dogs from entering parks and playgrounds and requiring owners to remove their pets’ faeces from public areas could help prevent most cases of human toxocariasis (4).
REFERENCES
1. GILLESPIE SH. The epidemiology of Toxocara canis. Parasitol Today 1988;4:180-182. [ Links ]
2. FINSTERER J, AUER H. Neurotoxocarosis. Rev Inst Med Trop S Paulo 2007;49(5):279-87. [ Links ]
3. MOREIRA-SILVA SF, RODRIGUES MG, PIMENTA JL, ET AL. Toxocariasis of the central nervous system: with report of two cases. Rev Soc Bras Med Trop 2004;37:169-74. [ Links ]
4. WOLFE A, WRIGHT IP. Human toxocarosis and direct dog contact. Suppl Compend Contin Educ Pract Vet 2004;26(6):12-16. [ Links ]
5. VIDAL JE, SZTAJNBOK J, SEGURO AC. Eosinophilic meningoencephalitis due to toxocara canis: case report and review of the literature. Am J Trop Med Hyg 2003;69(3):341-3. [ Links ]