Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Revista colombiana de Gastroenterología
Print version ISSN 0120-9957
Rev Col Gastroenterol vol.27 no.3 Bogotá July/Sept. 2012
Endoscopic submucosal dissection (ESD) for early gastric cancer: State of the art
Elías Alfonso Forero Piñeros, MD (1), Vitor Arantes, MD (2), Takashi Toyonaga, MD (3)
(1) Chief of Endoscopy and Gastroenterology. Hospital Central de la Policía, Bogotá, Colombia.
(2) Assistant Professor of Surgery. Institute Alfa of Gastroenterology. Federal University of Minas Gerais, Belo Horizonte, Brazil.
(3) Associate Professor, Department of Gastroenterology, Kobe University Hospital, Kobe, Japan.
Received: 06-03-12 Accepted: 17-08-12
Abstract
The treatment of early gastric cancer has undergone revolutionary changes in the decades since the advent of endoscopic management. Currently, most of these early lesions are treated with endoscopic submucosal dissection (ESD). Due to the excellent screening program implemented in Japan almost half of all cases of gastric cancer there are treated with ESD. The aim of this review article is to facilitate the use of this technique by Latin American endoscopists and thus benefit our patients. To this end we provide a detailed description of ESD, show the current state of indications for this technique, and explain the limitations of this technique. This study was conducted by endoscopists trained in ESD in Japan and supervised by an expert Japanese endoscopist (TT) who had performed more than 4,000 with endoscopic submucosal dissections as of the beginning of 2012.
Key words
Submucosal dissection, early gastric cancer, ESD.
INTRODUCTION
Gastric cancer is the fourth most common cancer and second leading cause of cancer death in the world. It is generally a disease with poor prognosis. Less than 25% of patients survive for 5 years. This is related to the fact that a large percentage of cases throughout the world are diagnosed in advanced stages, and the majority of these are adenocarcinomas (1).
Endoscopic submucosal dissection ESD- is the greatest advance in therapeutic endoscopy for management of early gastric cancer in recent years. It was developed in Japan in the 1990s, and is currently the definitive management of nearly half of the gastric cancers diagnosed in this country where 10,000 new cases are detected annually. Each day its acceptance and use grow in the rest of the world. In addition, ESD has advantages over surgical management which had previously been the standard treatment: it is less invasive and cheaper, it produces less morbidity and mortality, and it results in better quality of life for the patient by preserving the organ.
Because of the extremely low incidence of lymph node involvement in the early stages of this disease, local endoscopic resection can be curative for many cases. In 1984 the first case of gastric endoscopic mucosal resection EMR- was published. Although EMR has benefits that cannot be achieved with surgery for certain early lesions, endoscopic resection through ESD is "en bloc" which is indispensable for complete histopathologic staging. Not only does this allow for healing, it permits the physician to really define possible next steps. Although other endoscopic techniques have been developed to destroy these tumors, none allows removal of the complete pathological specimen without which neither the stage of the disease, the exact prognosis for the patient, nor whether the procedure was curative can be determined.
This endoscopic treatment does not preclude surgical treatment if required later. Histopathologic evaluation of the entire lesion defines not only the depth of invasion, but also the degree of differentiation and extent of vascular lymph involvement. Thus the physician can predict the risk of metastasis to lymph nodes using published data from similar patients. This risk is compared against the known risks of conventional surgery thus defining the action which needs to be taken.
EMR and ESD are not popular in the West because few cases are available with the appropriate indications. This is related to lower incidences than in Japan and the lack of adequate screening programs. Consequently there are very low rates of early diagnosis of gastric cancer. In addition, Japanese and Western pathologists have different histopathologic criteria for early mucosal intestinal cancer. As a result, the majority of early diagnoses by Japanese pathologists would not be recognized as cancer in the West (2). Still, the ESD is a technique that is still being developed, and both its acceptance and its use are growing. This is true even in the West where the morbidity and mortality of conventional surgery are also higher than in Japan. Some countries such as South Korea have followed the example of Japan and have implemented mass screening programs for gastric cancer. This has brought the percentage of cases diagnosed early, and which are therefore treatable endoscopically, to over 40%. This in turn has to rapid spread of this technique in Korea (3).
Although other potentially malignant gastric diseases such as gastrointestinal stromal tumors (GIST) have been resected by DES, at present endoscopic management of these lesions has not proven clinic useful. Nevertheless, it has been shown that it is, at the least, technically possible. These procedures remain very controversial due to the risks of incompletely resected, and potentially malignant, lesions. This type of treatment is not accepted by the Japanese Society of Gastroenterology and most Japanese teachers who have experience in gastric DES do not practice it. The exceptions are a few centers which are currently performing these procedures within strict research protocols. Therefore, widespread routine subepithelial gastric resection of GIST by ESD cannot currently be recommended, even though it may eventually be possible.
EARLY GASTRIC CANCER DIAGNOSIS
Screening
Early-stage gastric cancer which is still curable by endoscopy can only be treated if it is diagnosed at this stage. This makes implementation of mass screening programs aimed primarily at high-risk populations mandatory. Japan, which has the highest rate of diagnosis of early stage cancer (over 50%), has a program to take double barium contrast radiographic images of every patient over 40 years of age. This technical achievement also requires standardized reading of these images. This is followed by endoscopic screening of symptomatic patients and any others who wish to have the procedure performed. It takes at least 20 minutes. The gastric mucosa is completely washed and the complete exanimation is performed with optical magnification video endoscopy equipment. Any irregularity found is carefully evaluated. In addition, electronic chromoendoscopy and chromoendoscopy with indigo carmine are routinely used, and biopsies of all suspicious lesions are taken. Between 40 and 100 photographs are taken during an endoscopy, and are stored in electronic files. The government subsidizes these screening programs.
Recently, South Korea has also implemented mass endoscopic screening programs and have already achieved rates of diagnosis of early stage cancer over 40%.
Western countries, especially Andean countries with high risks of gastric cancer, need to implement similar programs which would lead to early diagnosis of these lesions. This would need to be combined with better training in performance of endoscopies which can actually detect these lesions, and it would also require more widespread use of optical magnification video endoscopy equipment which is ideal for this purpose.
HISTOLOGICAL DIAGNOSIS
According to the Laurens classification (4), gastric cancer is histologically divided into:
1. Intestinal type (IT) gastric cancer, which includes:
- Well or moderately differentiated papillary adenocarcinoma
- Mucinous adenocarcinoma without signet ring cells
2. Diffuse type (DT) gastric cancer that includes:
- Signet ring cell carcinoma
- Poorly differentiated adenocarcinoma
3. Mixed type (MT) gastric cancer which has non-homogeneous mixtures of IT and DT.
MT and DT have more aggressive biological behaviors than does IT. These behaviors include tendencies to greater depths of invasion, lymphatic invasion and increased metastases to lymph nodes.
ENDOSCOPIC DIAGNOSIS
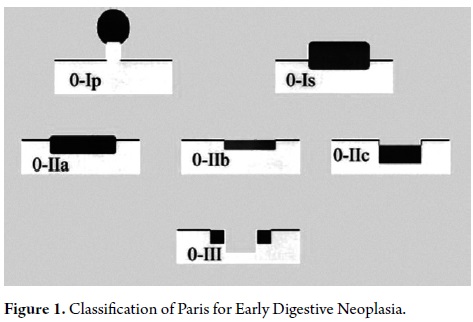
The Japanese attach great importance to the endoscopic appearance of these lesions for predicting the depth of invasion. When the endoscopic appearance suggests that the penetration depth of the tumor in the digestive wall does not extend beyond the submucosal layer, the lesion is called a "superficial injury." In other words, the chances that there is infiltration of the muscularis propria layer are negligible. A search for consensus with Western endoscopists led to the classification of Paris (5) (Figure 1) which classifies the early endoscopic appearance of these lesions as type 0, based on the classification of Bormann for advanced gastric tumors, as follows:
- Type 0-Ip (protruded pedunculated).
- Type 0-Is (protruded sessile).
- Type 0-IIa (superficial elevated).
- Type 0-IIb (superficial flat).
- Type 0-IIc (superficial depressed).
- Type 0-III (excavated).
In the stomach the limit for classification as sm1 has been set at up to 500 microns deep in the submucosa. Here the risk of metastasis to lymph nodes in well-differentiated adenocarcinoma is very low (less than 3%). This risk increases to more than 20% when the lesion has invaded more deeply into the submucosa (Table 1).
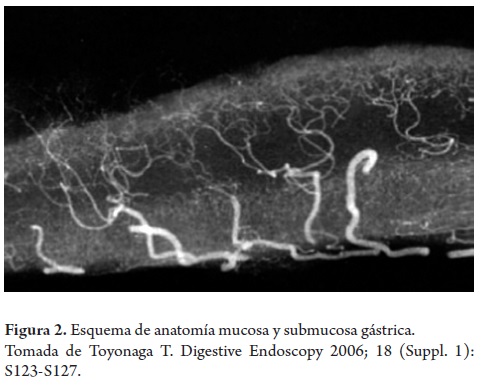
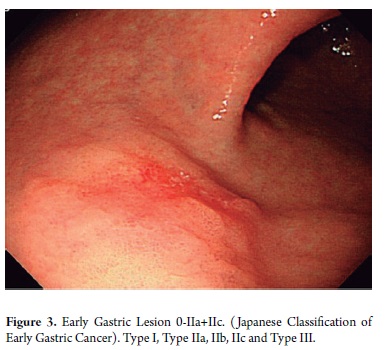
Most superficial neoplasias in stomach cancer are type 0-II (superficial), and most of these are depressed (type 0-IIc, 70%-80%). Types 0-I (polypoid) and 0-III (ulcerated) are rare. The overall risk of submucosal invasion in type 0-II is less than 40%. The risk is higher for type 0-I and for combined type 0-IIa + IIc. It is lowest for type 0-IIb. Initially, it was considered that non-depressed lesions (types 0-IIa and 0-IIb) with diameters less than 2 cm could be treated safely with endoscopy. For depressed lesions (type 0-IIc) a limit of 1 cm was established. However, these limits have been changed, and no final agreement has been reached as of this writing (Figures 2 and 3).
USEFULNESS OF TECHNOLOGICAL ADVANCES IN DIAGNOSTIC ENDOSCOPY
Technical advances in endoscopy such as electronic chromoendoscopy using Narrow Band Imaging (NBI) or Fujinon Intelligent Color Enhancement (FICE) that allow easy analysis of the vascular pattern in the transparency through uncolored translucent epithelium have allowed identification of abnormal vascular patterns which are closely related to certain types of neoplasias.
Sufficient technological support comes from a combination of advances. The high definition television technology of modern endoscopic monitors has up to 1,500,000 pixels from the camera at the tip of the endoscope while digital output (DVI) better integrates these systems without deterioration in the quality of image. These advances are used together with the total magnification of modern video endoscopes from 150X to 200X. (Total magnification is the sum of electronic magnification from modern 2X processors and the optical magnification of 150 times through the systems of microlenses at the end of the endoscope.) Combined with this technology, chemical chromoendoscopy (indigo carmine) and pit pattern analysis (analysis of the surface epithelium architecture) allow better classification of probable endoscopic tumor histology, the probable depth of tumor invasion, and lesion boundaries (6).
Optical magnification and electronic chromoendoscopy allow different depths of examination and therefore better assessment of the vasculature. This allows better determination of the surface structure of the tumor which, together with known micro vascular patterns, helps detect carcinoma in adenomatous lesions.
These technologies have been evaluated in Japan where they have been shown to better differentiate between neoplastic and non-neoplastic lesions (which do not require treatment) than other methods. This is true for all cancers and digestive tumors, particularly for pathology related to Barretts esophagus and neoplasia of the colon where the advantages, especially the optical magnification, are compelling.
Indigo carmine chromoscopy increases the recognition of tumor margins 67% to 84% over white light endoscopy: 68.5% to 89.8% for well-differentiated adenocarcinomas, and 62.8% to 70% for undifferentiated types. One study showed that by using optical magnification and electronic chromoendoscopy the possibility of proper recognition of the edges and after markings with ESD increases up to 97.4%. When optical magnification combined with chromoscopy with indigo carmine is used, recognition is 77.8%.
Adding confocal microscopy facilitates the differentiation of non-cancerous lesions from neoplastic gastric cancer lesions (high grade intraepithelial dysplasia). Studies of this technique are lacking, and it is expensive and time consuming. These factors make widespread use of this technique impractical in the near future.
USEFULNESS OF PREOPERATIVE ENDOSCOPIC ULTRASOUND AND OTHER STUDIES
Another important technology for preoperative evaluation of these patients is endoscopic ultrasound (EU). It is especially useful when high frequency mini-probes are used because it becomes possible to assess the degree of involvement of submucosal lesions scheduled for surgical endoscopy. However, it is not clear whether EU can differentiate exactly between mucosal gastric cancer and deeper gastric cancer. In different studies, the sensitivity of measurement of this difference varies from 18.2% to 100% (average 87.8%), specificity varies from 34.7% to 100% (average 80.2%), and accuracy is 89.24% (as measured by areas under ROC curves) (7). There is agreement that these cases should ideally be studied with mini-probes of 15 MHz or more since they make it possible to have endosonographic images of the muscularis mucosa layer.
The accuracy of EU is affected by histological differentiation and tumor size: greater error in staging is founded with large lesions and with undifferentiated lesions. To date, most ultrasound studies initially seek to define whether patients with advanced stages of cancer are candidates for surgery, so there are still too few studies that include patients with early stages, which are candidates for ESD.
EU is primarily used to define the possibility that suspicious lesions have invaded the submucosa, but even in Japan where it is widely available and physicians have experience using ultrasound in early gastric cancer, there is still no clarity about diagnosis with this technology and its usefulness for assessing theses patients. Studies have even been done that show no advantage of ultrasound-s accuracy over that of conventional endoscopic evaluation with modern video endoscopes. Fibrosis is another factor which can alter the accuracy of EU, but which has not yet been clearly evaluated, especially for recurrent lesions subjected to ESD.
Besides these problems, most endoscopy services do not have the necessary ultrasound mini-probes. Diagnosing higher stages of development than is actually present may occur in 20% of the cases in some series, which means that 10% to 20% of patients could become candidates for unnecessary ESD or surgery.
Currently in Japan, the gold standard for determining the proper treatment of early gastric cancer is detailed diagnostic endoscopy and estimation of lesion depth. This is achieved with +/-electronic optical magnification equipment (150X - 200X) plus electronic chromoendoscopy (FICE or NBI) and chromoendoscopy chemistry (indigo carmine). In current Japanese practice the use of ultrasound mini-probes for evaluation is rare. Endoscopic ultrasound with mini-probes prior to ESD of gastric lesions is carried out only when there is suspicion of massive invasion of the submucosa (which requires surgical treatment). If ultrasound does not show such a massive invasion, ESD is performed and the report from the histopathologic study report established the next steps (8).
Lymph node involvement is evaluated with several techniques including computerized tomography, conventional radial EU and ultrasound-guided cytological puncture (FNA-EUS). The latter is best for assessing lymph nodes in advanced lesions. For early lesions there are no studies comparing diagnostic accuracy for determining the presence or absence of lymph node involvement of histopathological evaluation and endoscopic ultrasound mini-probes. In some studies, the sensitivity of endoscopic ultrasound without puncture for assessing lymph node involvement in early lesions has only been 30% (9). In current Japanese practice, endoscopic ultrasound with mini-probes is not used for this purpose in preoperative evaluation for gastric ESD for early gastric cancer.
Evaluation of distant metastases should be performed with CT, although recently the use of positron emission tomography (PET) has increased for the evaluation of metastatic cancer in general. However, for these primary early lesions, it is very rarely indicated.
ENDOSCOPIC TREATMENT OF EARLY GASTRIC CANCER
Endoscopic mucosal resection (EMR)
The EMR was the first endoscopic treatment with curative intent that also attempts to preserve the tissue removed in one piece for histopathological staging. The three most common EMR techniques are the injection technique, the cap assisted technique and the ligature assisted technique (39). All EMRs should mark the boundaries of the lesion before resection.
Injection assisted EMR, also called saline assisted polypectomy, is often used to resect large flat polyps in the colon. There are actually two techniques which fall into this category: inject and cut, and inject-lift and cut. The inject and cut technique uses electrocauterization loop through a single-channel endoscope while the inject-lift and cut technique uses two separate channels of a double-channel endoscope. In this technique endoscopic grasping forceps clamp onto the lesion and raise it, and then the electrocauterization loop is used through the other channel of the endoscope. A variation of this technique applies counter-traction to the lesion with endoscopic grasping forceps through a percutaneous gastrostomy. The transparent caps used can be straight or oblique, and either hard or soft.
The principles of EMR-assisted ligation are similar to those for endoscopic variceal band ligation (EVL). Recently multiple band ligator accessories have become available in the market. They are equipped with hexagonal 1.5 x 5 cm handles and which have 5 to 7 Fr insertion sleeves.
The indications for an EMR in early gastric cancer, according to the classical Japanese guidelines from 2000, are:
1. When there is low risk of metastasis to lymph nodes and well-differentiated intramucosal adenocarcinoma the implications are:
- Resection of superficial or elevated mucosal lesions smaller than 2 cm when there is no ulceration, scarring, or venous or lymphatic involvement.
- Resection of flat or depressed mucosal lesions smaller than 1 cm when there is no ulceration, scarring, or venous or lymphatic involvement (Figure 4).
In these cases an EMR is a very good option as the risk of metastasis to lymph nodes is only 0.36%. This is also useful for some patients at high surgical risk and for those who refuse surgery. In Japan, the results of large series have shown a low incidence of complications and no deaths related to this treatment after 10 years of use. The survival rates at 5 and 10 years are similar to those obtained in patients with radical surgery (10, 11).
Reported local recurrences following EMRs vary between 2% and 35%. Normally neither EMRs nor ESDs should be attempted in cases in which lesions do not rise during submucosal injection. Failure to rise is a predictor of deep invasion which is unlikely to be successfully resected endoscopically (Table 2).
ENDOSCOPIC SUBMUCOSAL DISSECTION (ESD)
This technique removes the tumor by careful dissection completed in the deep submucosal layer beneath the lesion. The development of this technique and its accessories have enabled en bloc resection of much larger lesions than those resectable with EMRs.
Initially, ESD was used only to resect mucosal lesions in the stomach which were larger than 2 cm (the classical Japanese criteria). Subsequently, it was shown that outcomes and prognoses were just as good for well-differentiated adenocarcinomas under 30 mm in diameter that compromised the superficial submucosal layer (sm1: up to 500 microns). Outcomes and prognoses were even good for some lesions with ulceration (12).
The ideal patients for ESD are those whose previous endoscopic and endosonographic studies have reported the classic signs and therefore have very low risk of metastasis to lymph nodes. ESD is also ideal for patients who do not fully meet these criteria, but have high risks that contraindicate surgical management.
The Japanese series have shown that survival at 5 years specifically related to the disease has been 99% to 100% when the cancer is mucosal, and 96% when there is submucosal involvement. This must be taken into account in patients with borderline indications.
The results of monitoring these patients and their surgical specimens have shown that much of the surgery that has been performed has been unnecessary. The only results from this surgery have been additional morbidity and mortality for patients and additional costs for health systems. As a consequence, indications for ESD have been expanded. In a large series Gotoda found no lymph node involvement in the stomachs of patients with well differentiated intestinal mucosal gastric cancer without ulcers (no size limit), in patients with ulcers in lesions smaller than 30 mm, and in patients with well-differentiated submucosal cancer limited to sm1 of less than 30 mm in diameter. Based on this, Gotoda proposed to include these types of lesions within the usual indications for ESD and recommended the urgent need for adequate histopathologic evaluation of the resected lesions (Table 3) (13).
From this study arose the following expanded indications for ESD in cases of early gastric cancer:
- Differentiated gastric cancer: well or moderately differentiated tubular adenocarcinoma and papillary adenocarcinoma.
- Cancer without vascular lymph involvement correlated with minimal risk of metastasis to lymph nodes as defined by one of the following categories:
- Non-ulcerated mucosal cancer regardless of size.
- Ulcerated mucosal cancer of less than 30 mm in diameter.
- Minimally invasive cancer of the sub mucosa (sm1, less than 500 microns from the muscularis mucosa layer) of less than 30 mm in diameter.
Patients with cancer who do not meet these criteria require surgery. If the endoscopic evaluation suggests the possibility of mucosal invasion, it has been suggested that the patient undergo abdominal endoscopic ultrasound and a computed tomography (CT) scan before treatment (14). In some cases the utility of sentinel node navigation surgery has also been suggested (15). The criterion of ulceration has been much discussed, since antisecretory treatment can result in an ulcerated cancer without ulcers, and even fabric covered pseudo normal tissue can develop during re-epithelialization. Up to one third of malignant ulcers have been observed to change their appearances over time. The literature is not clear about the indications and prognoses of lesions for which no ulcers have been found, yet superficial scars or high fibrosis have been observed during dissection. In addition, differences exist among observers about the definition of what an ulcer is and about how to graduate the level of fibrosis encountered during dissection.
Recently, Gotoda published his personal experience following almost a decade of implementing the expanded criteria (16). He compared patients to whom he applied the classical unexpanded criteria to those to whom he had applied the expanded criteria. He found no differences in either overall performance or overall long term survival rates, but the expanded criteria resulted in avoidance of unnecessary radical surgery. Gotoda recommended annual endoscopic follow up for those who fulfilled the criteria. For those who did not, he recommended follow ups every six months with endoscopy plus endoscopic ultrasound or a CT scan.
In a series that used the expanded criteria, Goto et al. found that cancer recurred in 0.9% of the patients during 36 months of follow up. A recent large Korean series used histopathologic analysis and monitoring to evaluate the expanded indications. It found that 2.3% of patients who met the expanded indications for mucosal cancer, and 4% of those who met the expanded indications for submucosal cancer, had lymph node metastases. This series has shown flaws in these expanded indications. As a result they cannot be said to be definite, but rather require further studies and more evidence to define actual limits of these indications. Nevertheless, that series did not find a single patient with mucosal cancer without well-differentiated ulcers which had metastasized to the lymph nodes, regardless of lesion size. For now this might be considered to be the new limit for determining what to do with these patients. Indications for surgery for patients with any evidence of submucosal involvement (even sm1) must be better defined. Nevertheless, this is still very controversial (17).
The highest percentage of failures of the expanded criteria of Gotoda occurred among patients with poorly differentiated cancers. Another Korean study also found metastases to lymph nodes in 3.4% of patients with small poorly differentiated mucosal cancers. Indications for effective use of ESD in undifferentiated cancer in the long term are limited and have yet to be very clearly established (18).
A limitation of the currently available information about the results of ESD is related to the study of micro metastases to lymph nodes and to the possibility of iatrogenic spread by the devices used resulting in the possibility of late recurrences.
ESD PRINCIPLES AND TECHNIQUES
The principles for this endoscopic procedure are similar to those for any complex endoscopic procedure:
- Improve visualization of the gastric mucosa during the procedure by prior administration of pronase. Endoscopically wash mucosa with water and pronase to remove all the mucus around the lesion which improves vision and allows optical magnification and appropriate marking.
- Prevent embolism by use anti-embolism stockings for patients at risk.
- Prevent bronco-aspiration through use of a fixed nozzle with overtube. This allows frequent removal of equipment to clean the lens, place or remove caps, or even a change of equipment. It protects against bronco-aspiration especially in esophageal dissections which require the use of large quantities of fluids and dyes in the esophagus. Another necessary step is frequent aspiration of gastric contents, especially when the patient is placed in positions that favor the flow of fluids instilled.
- Use optimal endoscopic technology. The endoscope should be thin and have high definition wide angle retroflexion equipment with optical magnification. It should also have electronic chromoendoscopy equipment for margin evaluation. Ideally, all of these features should be combined in one endoscope with a CO2 insufflation system.
- Avoid patient discomfort and improve patients tolerance to the procedure and facilitate proper implementation of operator technique through the use of moderate to deep sedation. Different schemes of moderate and deep sedation and administration can be used by the endoscopist with the assistance of nurses. In Japan, general anesthesia is rarely used (usually when the procedure is expected to last over 180 minutes). Currently, the most commonly used sedation schemes for gastric ESD in Japan, are the following:
.- Infusion of 3 mc/kg Dexmedetomidine hydrochloride (Precedex) for 5 minutes followed by continuous infusion of 0.4 mcg/kg/hour. An additional bolus of 1 mg of midazolam can be added as needed. This is a highly selective alpha 2 agonist that produces sedation and analgesia, maintains hemodynamic stability, but does not produce respiratory depression within the range of 0.2 to 0.7 mcg/kg per hour. In addition, it further reduces hormones response to stress. Dosages must be reduced in patients with significant liver damage. Recently, a study comparing this scheme with traditional sedation with propofol or midazolam for ESD treatment of early gastric cancer was published. It found that this scheme had no cases of patients who suffered clinically relevant oxygen desaturation, plus there was significantly lower percentage of patients with body movements, the effective rate of sedation was significantly higher, and the duration of the ESD was significantly lower than with the traditional scheme. These findings show that this scheme is effective and safe for these procedures (19).
.- 0.8 mg/kg propofol bolus followed by 3 mg/kg per hour parenteral infusion with or without additional1 mg boluses of midazolam.
.- 0.8 mg/kg propofol bolus followed by 3 mg/kg per hour parenteral infusion plus 15 mg pentazocine at baseline and then every hour (20).
.- 15 mg pentazocine initial plus 0.05 to 0.1 mg/kg bolus of midazolam plus 1 or 2 mg boluses of midazolam as needed.
- Facilitate submucosal dissection technique by having adequate quantities of injection agents for lifting the lesion and the accessories required for submucosal injection available (Figures 5 and 6). This will allow for safe dissection. The ideal agent for injection should be inexpensive, readily available, non-toxic, and easy to inject. These features provide adequate and easy lift of the sub mucosa and have long lasting effects. Long-acting solutions shown are hyaluronic acid, hydroxypropyl-methylcellulose (a semisynthetic ophthalmic solution), mannitol and fibrinogen solution. Hyaluronic acid is expensive, scarce, and requires special storage conditions. Hyaluronic acid and hydroxypropyl- methylcellulose are very viscous and should be diluted to facilitate injection. Tissue damage and local inflammatory reactions at mannitol and hydroxypropyl-methylcellulose injection sites have been reported. Fortunately, ESD management of gastric lesions using needle knives (Flush knife and flex knife) to allow permanent instillation of saline solution into the sub mucosa does not require any special solution other than normal saline solution (NSS). The needle knife can repeatedly instill the solution directly into the sub mucosa thus lifting the lesion prior to the electrical cut. This allows simultaneous continuation of dissection without changing accessories and without costly long-acting solutions. This accessory is very useful in places like Latin America where hyaluronic acid is not available in local markets and where a large proportion of lesions that may benefit from treatment with ESD are located in the stomach. This type of accessory (flush knife) enables the entire process of cutting edges, instillation of NSS in the sub mucosa, vascular dissection and coagulation. Its use simplifies, facilitates and shortens the whole process of the ESD. Use of long-acting solutions is essential for lesions of the colon and esophagus (The most commonly used are hyaluronic acid and mannitol).
- Have all additional accessories specifically needed for ESD (needle knives, injection needles, hemostats).
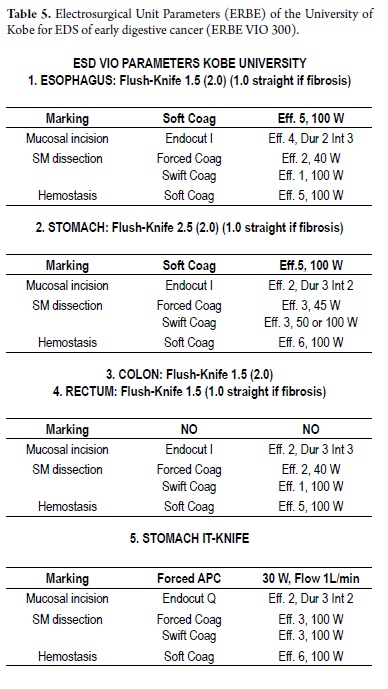
- Have an adequate electro-surgical unit (ESU) which includes support staff trained in the protocols of the specific parameters of ESD (Tables 4 and 5).
- Provide the operator with a convenient location which has with the screen in front of the operator. She or he should wear comfortable clothing to facilitate a procedure that may eventually be delayed for several hours and which may become tiring (Figures 7 and 8).

The ESD technique for managing early gastric cancer in the stomach is as follows:
Different types of needle knives need to be used. One of the most commonly used is the flush knife (plain or ball type). An adequate electro surgical unit ESU (ERBE ICC 200, VIO 200 or VIO 300) is needed. A 4 mm long cap should be placed at the tip of the endoscope for better vision in the operative field. Perform the following steps:
1. Marking: Small well defined marks are placed around the gastric lesion with a 1.5 to 2.5 mm flush knife (forced coagulation mode, effect 3, 20 W). In Japan, this is usually performed with optical magnification equipment. The mucosal lesion and the area around it should be well washed and free of mucus (prior cleaning with water and pronase). High definition optical magnification and electronic chromoendoscopy equipment (FICE, NBI) provide the actual location of the full edges of the lesion thus reducing the possibility of incorrect marking and resection which is not curative. Chemical chromoendoscopy with indigo carmine also helps identify the borders of the lesion, especially in places where there is no high definition optical magnification equipment with electronic chromoendoscopy. Usually the dots are marked at least 5 mm beyond the lesion with an additional proximal or distal mark according to the protocol of each hospital for the orientation of the lesion for histopathology.
2. Approach: In general, there are three types of approaches: front (for antral and pyloric lesions), rear (for personal, fundic and cardial lesions), and mixed (for complex lesions). According to the site of injury, the operator should plan what to use in advance and then make a list of all needed accessories.
Frontal approach used for antral lesions. First inject saline solution into the oral edge of the lesion. Make the mucosal incision at this level. If the lesion is very small, a larger area should be removed to facilitate handling. After the incision, cut frontally until there is a suitable flap. Then make a partial incision in the distal edge (anal). This will allow exertion of traction to help the distal (anal) and help lift the flap open to facilitate the entry of the endoscope with the cap on its tip into the area of exposed submucosa which will allow visualization and dissection. Dissection then continues from oral to anal. Prior to the end the missing segment of mucosa which exerted traction is isolated, and then dissection and resection of the lesion are completed. Depending on the location of the lesion, as the dissection progresses the surgeon can always try to use the force of gravity to help remove the flap of the gastric wall. This may require changes in the patients position. Always verify proper lifting before cutting the edge of the mucosa. Repeated injections of submucosal saline may be necessary. A circumferential incision can be made for some small antral lesions with very low probability of fibrosis. Dissect sufficiently to expand the edges, and complete the procedure to resection the submucosa with a sufficiently large polypectomy snare (forced coagulation mode, effect 4, 45 W).
Rear approach used in personal, cardial or subcardial lesions. First, make a distal (anal) edge incision from the rear approach. This incision must be wide for small lesions. It continues in the same direction, from oral to anal, as the initial dissection (l) until the flap is created. In this case the proximal segment of uncut mucosa helps exert traction in the oral direction which facilitates entry through the rear approach of the capped tip of the endoscope for further dissection. Then resection the mucosa to the sides and continue dissection along these lateral segments. Segmenting remaining uncut traction facilitates mucosal dissection. Shortly before finishing, isolate missing segment of mucosa for exerting traction. Complete dissection and resection of the lesion. Cardial lesions usually require a frontal approach of the cutting edge to the oral edge. Depending on the location of the lesion, as dissection progresses the force of gravity may help remove the flaps of the gastric wall facilitating dissection. This approach requires the use of high capacity retroflexion equipment made especially for cardial lesions. Always make sure that during entry of the endoscope the cap and needle knife are as parallel as possible to the muscularis propria layer. This will facilitate the procedure and avoid complications.
To dissect the oral segment of lesions located in the incision through the rear approach, it is usually helpful to move the endoscope away from the gastric wall. This enables the tip to enter the dissection window more easily allowing better dissection. This is accomplished by using the endoscope to place a balloon on the most proximal segment (oral) of the lesser curvature of the corpus, and then inflating the balloon with air. This holds the endoscope in a stable position which is separated from the gastric wall by the balloon.
Some large or complex lesions, or those located distally from the lesser curvature, usually require mixed approaches (frontal approaches for some segments and rear approaches for others). An example of a lesion requiring this mixed approach is the pylorus lesion which requires a rear approach in the duodenal bulb to mark and cut the anal edge of the lesion followed by performance of dissection and resectioning of the most oral edge. Finally, frontal dissection of the full lesion is performed.
3. Mucosal incision of the entire circumference is performed using a 2.5 mm flush knife (ERBE VIO 300, Endo-Cut mode I, 80 W, effect 2, duration 3, interval 2). The tip of the sheath of the needle acts as a protector and allows continuous handling. You can also use a pre-cut needle, but this requires changing the accessory before starting dissection, a step which is not necessary when using the knife flush.
After making the cut, dissect the mucosal side of the cut to the depth of the adjacent submucosa. This will not be extracted. Then perform appropriate coagulation of blood vessels in the sub mucosa adjacent to this margin. The vessels at the edge of the lesion to be extracted will not need additional hemostatic measures. This dissection depth in the vicinity of the cut makes it easy to complete homeostasis and dissection, especially in its final portion. In addition this avoids dissection beyond the defined margin.
The incision is made not only with the ball tip flush knife but also with the straight portion of the metal tip. Generally, the initial incision is nearly straight and is most often in the anal margin through the rear approach. As the process progresses the incision is extended, the cut takes the form of the letter C. This will ultimately be a circumferential incision. For this extension of the incision in the stomach, replacing the flush knife with the injection needle is not necessary for submucosal injection to lift the cutting edge safely. The flush knife can instill saline solution directly into the submucosa at the cutting angle which will permit continuation of the cut to continue extending the incision until the C becomes an O (an island). Making a C incision and then going deeper into the dissection cutting sites also has the advantage that it avoids going beyond the limits established for dissection by marking. In some places, you have to help by exerting pressure with the cap on the tip of the endoscope. This serves to separate the edges of the cut and to expand the window, thus facilitating the completion of the cut as it is deepened and facilitating coagulation of the border.
4. Submucosal dissection is performed with a 2.5 mm flush knife in the stomach or a 1.5 mm flush knife in technically difficult sites. The manipulation of the needle knife should be kept as parallel as possible to the muscularis propria while making the passage of electricity forced coagulation (effect 3, 45 watts). This should adequately control bleeding and prevent excessive burning. With this attachment, the tip of the needle knife is not visible, so the operator must use the tip of the sheath as a reference point to direct movement. The tip also acts as a protector of the muscularis propria when the needle knife is parallel to it. During dissection this needle can always be kept parallel to the wall by rotating movements of the endoscope. This avoids injury to the muscularis propria or middle submucosal layer which is rich in vessels. This flush knife keeps dissection almost uniform in the ideal area of the deep submucosal segment closest to the muscularis propria which has less vasculature. When this nearly parallel approach reaches the muscle layer, you can use the same knife for both dissection and cutting. If parallel positioning of the accessory is impossible, shorter needle accessories should be used to reduce the possibility of injury to the muscle layer and to increase the safety of the procedure.
Dissecting in deep submucosal tissue which is not very fibrous should be done by traction and tension maneuvers of the connective tissue fibers with the tip of the needle scalpel. With this method it is not necessary to move the attachment when applying coagulation current and the tension of the fibers helps in the process of cutting. In very fibrous regions the physician must make moves similar to needle punctures with the scalpel in order to dissect. Since there is no way to tighten these fibers, small lateral movements of the tip should be used to help dissect the tissue.
A flush knife connected to a water pump, preferably a manual syringe, can inject needed saline solution into the deep submucosa to thicken this layer which will facilitate visualization and dissection. This makes the procedure faster, easier and safer which enables clear identification of the architecture of the muscle layer and the submucosal vascular tree. The sheath on the tip of the flush knife protects the muscle layer against coagulation and against the cutting current while simultaneously allowing for a fairly deep dissection of the submucosal layer. By instilling saline solution into the submucosa the lesion is lifted and the middle submucosal layer can be separated from the muscularis propria layer. This creates what some authors call a dissection window which is both ideal and necessary for accomplishing dissection.
Water jet pressure and water volume can be easily controlled under the appropriate conditions. The jet helps keep the tip of the needle knife free from tissue adherence which could impair its cutting ability. In addition, if it becomes dry during the procedure it could be very difficult to remove, so frequent applications of the water jet are also necessary for removal. The water jet also keeps the operating field of vision clear when there is any soiling or bleeding. In case of bleeding, this accessory can be used to determine the exact point of bleeding and wash that point to allow for immediate homeostasis. If bleeding cannot be stopped after 2 or 3 attempts (coagulation effect forced mode 3, 45 W), the attachment must be replaced with a hemostat (coagulasper forceps -Olympus, or hot biopsy -Boston-) (soft coagulation mode effect 6, 100 W) to avoid perforation from excessive coagulation. If there is severe fibrosis, the needle knife will not be to inject saline solution into the submucosa in some segments to lift very fibrous injury. In these cases lifting of the lesion will require a conventional thin injection needle.
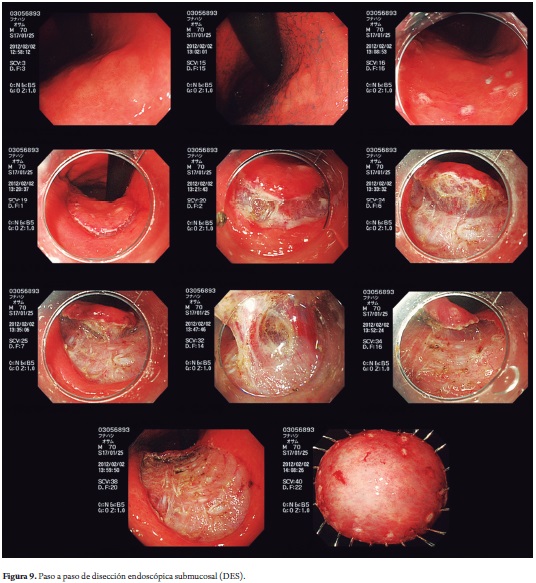
It is often impossible to complete this process with coagulation when dissection is in areas of severe fibrosis (e.g., ulcer scar areas). In these cases it may become necessary to carefully cut some segments fibrous areas with a scalpel with cutting current rather than drilling. When this happens, use of a short 1.5 mm flush knife with cutting current (Endocut I, 50 W, effect 1, length 2 and interval 2) is recommended (Figure 9).
5. Prevention of intraoperative bleeding: Coagulation efficiency increases when the current density decreases which results in improved homeostasis. In contrast, at high current density incision and cutting efficiency increase which results in less effective homeostasis.
The large blood vessels usually exit the muscularis propria and penetrate the submucosal layer vertically perpendicular to the muscularis propria. They then branch out horizontally. Most of them form a network in the middle submucosal layer. Therefore, the layer containing the fewest vessels is the deep submucosal layer that is closest to the muscularis propria. The key to minimizing intraoperative bleeding is dissection at this level. Preferably it should be parallel to the muscularis propria. Preventive treatment of large vessels should be done prior to coagulation at this level.
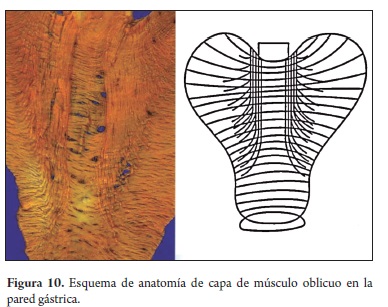
It should be kept in mind that the antrum has a lower density of vessels and less fibrous tissue while the lesser curvature of the corpus has more vessels, but little fibrosis. The anterior and posterior regions of the corpus have an additional layer of oblique muscle which increases the amount of perivascular fibrous tissue. This abundance of vessels and fibrous tissue at the site form an additional facade like layer over the submucosal layer which makes dissection difficult and increases bleeding. On the other hand it also exerts an additional protective effect on the inner circular muscle layer which is the layer in which coagulation increases the risk of perforation (Figure 10).
Some additional technical tips for prevention of bleeding include: The mucosal incision should be superficial and involve only the thickness of the mucosal layer. This avoids initial cutting of the submucosal layer, especially the middle submucosal layer, and avoids cutting blood vessels.
For submucosal dissection "arm cut" technique is one of the safest. Prior to electric dissection of tissue and vessels the arm of the needle knife is used to lift them away from the muscularis propria to prevent damage to it. Although hooked needle knives have been designed for this purpose, this procedure can be performed with other needle knives such as a flush knife. The ball at the tip of the ball variety of knife provides traction on the vessels towards the endoscope and away from the muscle wall which facilitates coagulation and cutting.
Additional cutting of the mucosal surface can be done with the same flush needle knife, thus minimizing contact with the middle submucosal layer and submucosal vessel damage.
Frequent additional injections of normal saline solution (NSS) into the deep submucosal layer are useful for clarifying the area of dissection and sites of vessel penetration. If a large vessel is identified, precoagulation with hemostatic forceps in soft coagulation mode (effect 6, 100 W) needs to be done prior to dissection to prevent bleeding. Precoagulation can also be done with the flush knife with the same coagulation current: precoagulation is done first on one side of the vessel and then on the other. This gentle coagulation aims for vessel to become white (coagulated) (forced coagulation effect 3, 45 W) before proceeding to cut it. Thanks to this, most of the time the necessity of changing accessories can be avoided. (21, 22, 23, 24, 25, 26).
The most appropriate technique is to cut from left to right because the device exits the endoscope channel in the lower left visual field. If counterclockwise cuts are required, it is best to rotate the scope until you find a place which allows an easier visual approach. Then perform the usual dissection. This keeps the area of dissection between the 7 oclock and 9 oclock positions where it exits the fixture through the working channel of the endoscope. When the vertical approach is used perpendicular to the muscle layer a hook knife (Olympus) must be used.
Finally, use Coagulasper clamp forceps or hot tweezers to coagulate all visible vessels leading from the gastric ulcer thus preventing late bleeding (coagulation smooth mode, effect 6, 100 W). It takes only a slight pull to remove the remaining vessels from the muscularis propria and avoid injuring it (this is only done in the esophagus or colorectal region, if there are visible pulsating vessels).
When dissecting very fibrous areas or areas which are under water in a place where dissection would not otherwise be possible, we recommend the use of the Swift coagulation mode (effect 3 for stomach, 80 W).
The needle knife is the perfect dissection accessory for ESD because it is easy to use, makes incisions efficiently, has a low risk of perforation and has minimal effect on coagulation in tissues at the edge of the resected specimen. The advantages of the flush knife (Fusion) are that it allows more precise dissection which protects the muscle layer and the lesion with the tip of the sheath thereby more easily controlling bleeding. The ball type is especially good for vascular coagulation and has a faster rate of dissection than does the traditional variety. The traditional short variety (1.0 or 1.5 mm) remains the most useful variety for dissection of highly fibrous areas.
The flex knife is a similar needle knife, but unlike the flush knife it cannot instill NSS into the submucosa. Its disadvantage is that it requires frequent changes of needle length, and cannot dissect areas of severe fibrosis. IT-1 and IT-2 needles (Olympus) do not allow full control of the dissection site and are not useful in narrow places with large amounts of fibrosis. Furthermore, the initial incision requires the use of a different accessory (for example a precut needle).
6. Extraction and preparation of the surgical specimen for histopathologic analysis: The piece is removed after being resected, grasped by foreign body forceps, and drawn into the cap on the tip of the endoscope. The piece is removed and placed in saline solution. The endoscope without its cap is reintroduced for preventive coagulation of late bleeding and for the eventual placement of clips at sites of suspected damage to the circumferential muscularis propria in order to prevent late perforations. The piece is then stretched and fixed and anatomical orientation is indicated. It is photographed with and without indigo carmine and is then introduced in to formaldehyde and sent to the pathology service.
7. Postoperative treatment: Proton pump inhibitors are administered parenterally to patients who are without complications for two days. They begin receiving a liquid diet 24 hours following the procedure. 80 mg of omeprazole or esomeprazole plus 3 g of sucralfate are then taken daily for 8 weeks. If helicobacter pylori has not already been be eradicated, it must be eradicated. 300 mg/day of rebamipida are prescribed for 8 weeks to patients with severe atrophic gastritis. This significantly increases the rate of healing of gastric ulcers induced by ESD (27, 28).
ESD COMPLICATIONS
Major complications of gastric ESD are bleeding and perforations. Other less common complications are transient bacteremia, aspiration pneumonia and prepyloric and pyloric stenosis.
ESD bleeding: Acute bleeding that occurs during ESD is almost always easily controlled. It is mild and causes no problems for patients, so it is not considered to be a complication of DES. It is prevented by careful maintenance of the dissection level to the submucosal layer depth (since most of the vessels are in the middle layer of the submucosa). Bleeding can also be avoided by maintaining a clear field of operation that allows recognition and meticulous coagulation of vessels before cutting them with a scalpel. Bleeding is controlled by coagulation. If it is severe, it can be controlled with hot biopsy forceps or grasper forceps. In theory, such bleeding can be also controlled by using argon coagulator during or after the procedure (flow 1.8 L and 45 Watts). However, this treatment produces smoke which is disadvantageous and requires vacuuming and which is not useful for pulsating bleeding.
Late hemorrhaging is a symptom associated with DES which occurs in 5.2% of cases. It is usually managed with endoscopic coagulation or clips, but 1.7% of patients require transfusions. Clips are not used for management of acute bleeding because they interfere with the procedure, but the can be eventually used to prevent bleeding from large vessels visible in the ulcer after ESD has been performed.
This late bleeding usually occurs within the first 24 hours, but can occur up to 8 weeks following the procedure as a complication of the ulcer is left by the resection. A Korean series reported late bleeding in 15.6% of cases. Of those, 0.6% were significant and required transfusions. In that series, the proportion of proximal bleeding was more than twice that in distal gastric resections.
Perforations caused by ESD: The reported incidence of gastric perforations during ESD is 0.5% in different series. A recent meta-analysis showed that 11.67% of these perforations required surgery and the other 88.33% were managed with conservative treatment consisting of endoscopic measures such as clips and general measures such as fasting, nasogastric tube feeding and broad spectrum antibiotics.
Perforation, particularly in fibrous areas, is avoided by careful technique which uses sufficient injection of solution to keep the submucosa layer edematous long enough so that the display can always be adjusted before each cut with the scalpel. Perforation is also prevented by rapid recognition and management by the physician during the procedure when there is evidence of fiber coagulation in the circular layer of the gastric wall, such as when it turns white, or if there is evidence of the "sign of muscle contraction" which consists of a secondary contraction of healthy muscle fibers around the injured muscle area (evident only in the colon). Endoscopic treatment involves the application of clips close enough to join the edges of the mucosa around the dissected area. Clips can eventually be used before completion of dissection to close suspicious areas of muscle damage in places where these clips do not impede the full en bloc dissection of the lesion.
Since no perforation during ESD has ever produced mortality, it is not considered to be a life threatening complication. Operator experience is inversely related to the occurrence of perforations. Perforations occur more frequently in colonic ESD than during ESDs elsewhere. They may occur in 7% of upper stomach resections, in 1% of those in the distal stomach, in 6% of lesions with ulceration and fibrosis, and in 3% of those with no ulcer fibrosis. They can be partially prevented with the use of shorter needle knives.
Endoscopic treatment of these perforations has a 98.3% success rate. Using CO2 for inflation during the procedure instead of air has clear advantages in cases in which perforation occurs. Its rapid absorption in the splanchnic vessels causes the patients symptoms to be more tolerable, and helps stabilize vital signs. ESD patients undergoing this type of inflation have less bloating and less pain following the procedure (29).
Other large series have reported ESD perforation rates from 0% to 3.5% most of which were managed with endoscopic clips and conservative management. In the largest series only 1 of 34 patients required surgery. Patients with microperforations and localized peritonitis may improve with conservative treatment, fasting, and intravenous antibiotics for 2 days and nasogastric LEV for 12 to 24 hours. Patients can begin eating two to four days following improvement of signs of peritoneal irritation, resolution of intraperitoneal air or improvement of white blood cell count.
Surgical management is reserved for large perforations that cannot be sutured with clips and for patients who appear to have severe peritonitis or unstable vital signs. A CT scan which shows large amounts of free abdominal fluid is an absolute indication for surgery because this suggests intraperitoneal infection caused by gastric contents. Late perforations caused by excessive coagulation compromising the muscularis propria may appear hours or days after ESD. They are manifested by abrupt onset of abdominal pain and fever and can progress to disseminated peritonitis. Every patient who develops any symptom after undergoing colonic or gastric ESD undergoes routine abdominal radiography in the standing position the day after the procedure as screening for late perforation. If late perforation is found, the patient requires surgery.
Other complications of ESD: Other complications include prepyloric and pyloric stenosis due to resection of lesions of the distal antrum. This occurs most commonly when the lesion has invaded the pylorus and when it covers more than two thirds of the luminal area. Severe stenosis of the antrum can be dilated with a balloon although some require surgical management.
Transient bacteremia is caused by bacterial translocation. It manifests as fever and discomfort after the procedure. Most patients improve with conservative treatment and the use of empirical antibiotics.
Aspiration pneumonia occurs primarily among the elderly. It can be prevented by placement of an overtube, frequent suction of gastric fluid to avoid accumulation, and by any changes in position conducive to reducing gastric fluid reflux into the esophagus that might accumulate during dissection (30).
HISTOPATHOLOGICAL EVALUATION OF THE SURGICAL SPECIMEN AFTER ESD RESECTION
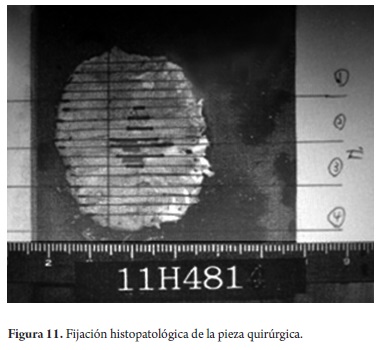
En bloc resection is ideal from the pathologists point of view. The endoscopist sends the lesion to pathology where it is fixed in paraffin and subjected to longitudinal cuts every two millimeters for pathological evaluation (Figure 11).
Due to the large discrepancy between the criteria of Japanese and western pathologists (31), an agreement on histopathologic staging of neoplastic gastrointestinal lesions was proposed in Vienna in 2000 (32) (Table 6). This agreement is in current use and divides the different stages of tumor progression into progressive categories classified p-TNM ("p" for pathology). When there is no invasion of the lamina propria the lesion is called a tumor in situ (p-Tis). When there is invasion of the lamina propria, the lesion is called a micro invasive carcinoma (p-T1M). If it invades the submucosa, the lesion is called an invasive neoplasia (p-T1sm).
The categories are defined as:
Category 1: Negative for cancer or dysplasia
Category 2: Indefinite for neoplasia or dysplasia
Category 3: Low-grade non invasive neoplasia: low grade adenoma or low grade dysplasia
Category 4: High grade non-invasive neoplasia:
- High-grade adenoma or high-grade dysplasia
- Non invasive carcinoma
- Suspicion of invasive carcinoma
Category 5: Invasive neoplasia:
- Mucosal carcinoma with invasion of the lamina propria or muscularis mucosa
- Carcinoma with invasion to submucosal or greater depth.
The pathologists report should include
1. Histological type. According to Vienna classification reports are frequently:
- Low-grade adenoma.
- High-grade adenoma.
- Differentiated early gastric carcinoma.
- Undifferentiated early gastric carcinoma.
2. Depth of tumor invasion. If the lesion involves the sub mucosa, the micrometer measurement of the depth of involvement must be reported.
3. Size.
4. Location.
5. Macroscopic appearance (including presence or absence of ulceration).
6. Lymphatic involvement.
7. Venous involvement.
8. Detailed description of involvement of lateral and vertical tumor resection margins which defines curability.
There are publications that show discrepancies between diagnoses made from preoperative endoscopic biopsies and subsequent histopathologic diagnoses from the whole piece of up to one third of cases. These discrepancies occur most frequently in non-intestinal cancer cases and often indicate unnecessary treatment.
RESULTS OF ENDOSCOPIC GASTRIC SUB MUCOSA DISSECTION FOR EARLY GASTRIC CANCER
Definitions
The following definitions are presented for evaluating results and establishing prognoses after ESDs.
1. Procedure time: time between entry of the endoscope and complete resection.
2. Operating time: time between marking and cutting lesions.
3. Speed of the procedure: procedure time divided by the area of the resected specimen.
4. Differentiated gastric cancer: well or moderately differentiated tubular adenocarcinoma and papillary adenocarcinoma.
5. Undifferentiated gastric cancer: poorly differentiated adenocarcinoma or carcinoma with signet ring cells.
6. Complete resection: en bloc resection of the tumor with horizontal and vertical margins free of neoplasia.
7. Positive lateral margin: Tumor cells are found in the lateral margin or lateral margin assessment is difficult because of burn effect due to excess coagulation or due to insufficient reconstruction of fragments in the case of piecemeal resection. There must always be a resection safety margin of at least 2 mm between the lesion and the edge of the cut around the surgical specimen.
8. Positive vertical margin: Tumor cells involve the vertical submucosal margin (Some consider this to occur when there is more than sm1 level which is equivalent to a depth of invasion greater than 500 microns, but this is currently in dispute).
9. Curative resection: Vertical and lateral margins are negative, submucosal invasion is not greater than 500 microns from the muscularis mucosa layer, and no vascular or lymphatic involvement or nests of undifferentiated cell type are found (Also called R0 en bloc resection).
10. No curative resection: Resection does not meet the above criteria, or there is one or more of the following findings:
- A component of undifferentiated carcinoma.
- Slight (minute) invasion of the sub mucosa within 500 microns in a lesion over 30 mm in diameter.
- The tumor is ulcerated with intramucosal cancer and is greater than 30 mm in diameter.
11. Local recurrence of tumor: histological diagnosis of cancer at the site of resection.
12. Perforation: free air in cavity immediately after resection as evidenced by x-ray, CT or physical examination.
Curability with ESD
An important series that specifically evaluated the curability of early gastric cancer with ESD was recently published. It showed that ESD treatment of early gastric tumors achieved resection en bloc in 98.9% of case and curative resection in 88.1%. Large lesions, lesions in the upper stomach and ulcerated lesions were related to non curative resection. The best chance for cure was achieved in distal gastric lesions, non ulcerated lesions, and lesions of less than 20 mm. The lowest probability of cure was found among ulcerated gastric tumors of over 30 mm located in the upper stomach. The failure rate ranged as high as 40% for these lesions. The average reported resection time was 64.8 minutes while average hospital stay was 8.1 days. Follow up times of up to 36 months for patients with curative resections found no local recurrences, but 5.97% died as a result of other causes.
This study determined overall survival rates of 95.7% at 3 years and 92.3% at 5 years. However, since none died of gastric cancer, the survival at 3 and 5 years specifically related to the disease was 100%. The comparable survival rate for surgery was 98%. The exceptional deaths from gastric cancer which did occur in the 10-year follow-up of patients who had undergone ESD were caused by metachronous tumors which were diagnosed late. No deaths have been reported from local recurrences, or from ESD or its complications anywhere in the world. Preliminary results published in the West do not achieve cure rates as high as those achieved in Japan (33, 34).
It is clear that hospital costs for these patients are lower than those for patients undergoing surgery. However, there are no comparative studies on this issue, nor are there studies that reflect either the costs of endoscopic follow up that these patients need or costs adjusted for quality of life.
For best rates of curability, the most experienced endoscopists should take the most difficult cases. These include local recurrences, very large lesions with large amounts of expected fibrosis, and ulcerated lesions of the proximal stomach especially in the gastroesophageal junction. Less difficult sites are the distal stomach and rectum which are ideal resection sites for operators that are just beginning their experience (35).
Of the patients whose ESD resections were not curative, 43.9% were referred for surgery, 7.0% were cured with a second ESD or an EMR after positive lateral margins were found following the first ESD, and 49.1% had no residual tumor apparent at endoscopy and were supervised with frequent monitoring.
An important recent Korean series reported results similar to those in Japan. ESD resections were complete in 95.3% of cases, and there were no deaths. Submucosal invasion was found in 7.4% of cases and vascular lymph invasion was found in 3% (36).
Another Korean series which evaluated curative resections which followed the extended criteria found curative resections in 88.7% of intestinal type lesions smaller than 2 cm, in 73.3% of intestinal-type lesions larger than 2 cm, and 37.9% of non-intestinal type lesions. This study also found that tumor size greater than 3 cm, presence of ulceration, histological type not intestinal and piecemeal resection were independent unfavorable factors not curative resection. In addition, reported that the fibrosis associated with ulcers increased the difficulty of resection. This study also found that lesion size was directly correlated with the depth of invasion, and recommended that the ESD with intent to cure stomach should be attempted in early gastric cancer of intestinal type well or moderately differentiated, less than 3 cm and ulcerated. It also found that considerable variations may occur in the accuracy of pathologic staging between hospitals of high and low volume.
ESD reports for early gastric cancer in the West, which are currently small case series, complete resections show a lesser proportion of cases (78% to 92%).
Indications for surgery after ESD: Surgery can be indicated for management of complications, but more often is indicated for management of disease rather than for curative resections which account for only 2.8% of cases. Only 0.2% of ESD cases suffer complications requiring surgery. This is usually treatment of significant perforation without localized peritonitis. Rather than early intestinal cancer, the primary indication for surgery after ESD heals is massive submucosal cancer (sm2 commitment or greater). (37) These tumors compromise the vertical margins or are lymphovascular invasions. Surgical specimens of these patients show residual cancer in 30.7% of patients, and 7.6% are positive for cancer in the lymph nodes. When the only cause for suspicion is positive margins, patients should be managed as if they really had positive margins because of the high risk of residual cancer. There is still controversy about the indication for surgery in these patients.
Indications for endoscopic retreatment after ESD: For all other patients whose ESDs were not curative, but who had no previous indications for surgery, a second endoscopic treatment using ESD, EMR or argon is recommended. If there is no endoscopic evidence of any residual lesion, more frequent endoscopic monitoring is required.
Local recurrence, the reappearance of tumor at the site of a resection, is Bly associated with incomplete resections. The risk of lymph node involvement in local recurrence is very low. Surgical management of a large number these patients found that all local recurrences were only mucosal and had no lymph node involvement. It is estimated that local recurrence occurs in 15% of non-curative resections and in 0% of curative ones. The largest proportion of recurrences occurs in resections of the upper two thirds of the stomach which is difficult to access and where recognition of lesion edges is more difficult in tangential assessments. In addition, in the upper two thirds of the stomach has greater fibrosis and vasculature. The latter results in increased bleeding during the procedure which makes procedures difficult and reduces the proportion of curative resections.
We must differentiate between local recurrences and appearance of new metachronous tumors. This series reported 4.8% of these tumors at 5 years. (38) It has been suggested that the eradication of Helicobacter pylori may decrease the incidence of metachronous tumors. At follow up, the range of metachronous gastric cancer incidence should be studied to define the relevant range of endoscopic monitoring.
Annual endoscopic follow up, and thereafter follow ups every three years, should be done for patients who have had curative resections. Monitoring should be more frequent for patients whose resections were not curative but who do not undergo surgery. These patients should have endoscopic checkups every 2, 6, and 12 months and then annual checkups. Routine chromoendoscopy of the scar should be performed and a biopsy should be taken whenever there is any suspicion of recurrence of a lesion.
Other data show local recurrence rates from 0% to 7.7%, although in most studies it is less than 1%. Most local recurrences can be cured endoscopically. When resection is piecemeal, reported local recurrence rates increase to between 2.3% and 36.5%. This is similar to reported local recurrence rates following EMRs.
Because local recurrences have abundant fibrosis, they are technically more difficult to remove through a second ESD. For these cases ESDs should be performed by experienced operators. Studies are needed to show the real impact of different levels of experience of the operator performing the task.
COMPARISON OF ESD RESULTS WITH RESULTS FROM EMR FOR EARLY GASTRIC CANCER
A large recent meta-analysis comparing the EMR with the ESD found that:
ESD requires smaller sizes of resection than does EMR.
ESD is more effective than EMR for:
- En bloc resection for both primary and recurrent cancer (OR 8.43, 95% CI 5.20 to 13.67).
- Complete resection (OR 14.11, 95% CI 10.85 to 18.35) for all locations, regardless of tumor size (even for lesions less than 10 mm in diameter where OR 3.58, 95% CI 1.84 -7.02). Korean series found en bloc resection for lesions less than 20 mm 95.3% with ESD vs. 76% with EMR (39).
- Curative resection (OR 3.28, 95% CI 1.95 to 5.54) for all locations, regardless of tumor size (even for lesions less than 10 mm in diameter where OR 3.53, 95% CI 2.57 - 4.84).
- Local recurrences up to 4 years (RR 0.13, 95% CI 0.04 to 0.41). The difference occurs in lesions larger than 10 mm; for less than 10 mm there was no difference in the meta-analysis.
ESD produces more of the following than EMR:
- Intraoperative bleeding (RR 2.16, 95% CI 1.14 to 4.09), although this bleeding is always easy to control. POP bleeding occurred more frequently in EMRs, but the difference was not statistically significant.
- Risk of perforation (RR 3.58, 95% CI 1.95 to 6.55). Most cases can be managed medically without mortality.
- Operative time (standardized mean difference, EMD 1.55, 95% CI 0.74 to 2.37). The difference was for lesions greater than 20 mm; for minor lesions there is no difference in operative time.
There are no differences between ESD and EMR in terms of overall risk of bleeding (RR 1.22, 95% CI 0.76 to 1.98) or all-cause mortality (RR 0.65, 95% CI 0.08 - 5.38).
EMR is easier and requires less skill than does ESD, but indications for EMR are more limited. ESD provides greater endoscopic therapy options than does EMR including the possibility of resecting some ulcerated lesions.
All the above comparison data are from metaanalysis of large case series. The only controlled comparison study conducted in Japan, by Dr. Nakamoto (40), found statistically significant differences:
En bloc resection: 53.8% in EMR vs. 94.3% in ESD (p <0.001)
Curative resection: 37.5% in EMR vs. 92.6% in ESD (p <0.001)
Recurrence at 5 years: 17.5% in EMR vs. 0% in ESD (p <0.001)
This study found no differences between ESD and EMR in en bloc resection and curative resection for early gastric cancer lesions of 5 mm or less, or for recurrence at 5 years in lesions of 10 mm or less. Therefore, according to this controlled study, EMR should be indicated for lesions smaller than 5 mm. This contradicts previous studies such as that by Dr. Watanabe which set the limit at 10 mm (41), and that by Dr. Yamaguchi which set the limit at 15 mm (42).
In summary, the comparison of ESD with EMR shows that perforations are not life threatening when they occur during either procedure, and rates of the occurrence of bleeding are the same for both procedures. The comparison shows that the benefits of ESD are markedly greater than those of EMR since ESD, especially in expert hands, can be used to treat a broader range of patients and has a much lower recurrence rate.
TRAINING RECOMMENDED FOR GASTRIC ESD
Training recommended by Japanese experts in the art of ESD includes:
1. Acquire basic knowledge of the disease, the instruments, and the use of the electrosurgical unit. Become familiar with indications, limitations, risks and outcomes of ESD.
2. Visit experts in Japan to observe the technique as performed by them (ideally for a month to see about 50 cases).
3. During training assist in procedures with patients.
4. Training with animal models (isolated pig stomachs or live pigs). Ideally, a student should perform about 30 resections on animal models.
5. Perform procedures on patients. Start with low-risk cases which are not difficulty or complicated. Most experts in Japan believe that to reach a proficient level of experience a physician must have performed 50 procedures in which the proportion of curative resections increased over time.
6. Lifetime continued training through books, magazines, DVDs, lectures, live demonstrations and occasional return visits to centers of expertise.
Ideally, starting the practice of this procedure requires a high-definition video endoscope with optical magnification equipment, data storage management system and high quality imaging. In addition, an experienced histopathologist who is knowledgeable about the advantages and limitations of this technique should be available. Additional requirements for practicing this procedure include careful endoscopic monitoring of patients; an ongoing training program to update practitioners, performance of at least 10 to 20 cases per year and maintenance of a prospective registry of all cases completed. En bloc resection should always be the aim, and piece meal resections should be avoided if it is at all possible.
THE FUTURE OF ENDOSCOPIC MANAGEMENT OF EARLY GASTRIC CANCER
Although use of ESD to resect gastric lesions has been going on for a fairly long period of time, the accessories available are continuously changing. Today, the types of needle knives used most often by the experts are the flush knife (regular and ball type) (43), and the insulation tipped knife (IT knife). Experts also continue to use smaller precut needle knives, flex knives and hook knives. However, since they are constantly creating and evaluating new models such as the swan blade, ERBE Hybridknife, dual knife, fork knife and scissors-type grasping forceps, only the future will tell which are really are the best for a particular type of injury.
Although today EMR and ESD can be used as definitive therapies for premalignant and early stage malignant lesions (T1M-N0) of the digestive tract, perhaps someday some of the stages are currently indicated for handling surgically will be handled with a combination of endoscopic management and either regional laparoscopic lymph node dissection or by procedures such as NOTES (Natural Orifice Transluminal Endoscopy Surgery). This could possibly include partial resectioning and suturing of the muscular layer (44, 45).
REFERENCES
1. Retana A. An update in endoscopic management of gastric cancer. Curr Opin Gastroenterol 2011; 27: 576-582.
2. Gotoda T. Endoscopic resection of early gastric cancer. Gastric Cancer 2007; 10: 1-11.
3. Song KY, Hyung WJ, Kim HH, Han SU, Cho GS, Ryu SW, Lee HJ, Kim MC; Korean Laparoscopic Gastrointestinal Surgery Study (KLASS) Group. Is gastrectomy mandatory for all residual or recurrent gastric cancer following endoscopic resection? A large-scale Korean multi-center study. J Surg Oncol 2008; 98(1): 6-10.
4. Lee TH. Appropriate indications for endoscopic submucosal dissection of early gastric cancer according to tumor size and histopathological type. Gastrointest Endosc 2010; 71: 920-6.
5. The Paris endoscopic classification of superficial neoplastic lesions: esophagus, stomach and colon. Gastrointest Endosc 2003; 58: S3-S43.
6. Lee WS. Technical issues and new devices of ESD of early gastric cancer. World J Gastroenterol 2011; 17(31): 3585-3590.
7. Kwee RM, Kwee TC. The accuracy of endoscopic ultrasonography in differentiating mucosal from deeper gastric cancer. Am J Gastroenterol 2008; 103(7): 1801-9. Epub 2008 Jun 28.
8. Conlin A, Kaltenbach T, Kusano C, Matsuda T, Oda I, Gotoda T. Endoscopic resection of gastrointestinal lesions: advancement in the application of endoscopic submucosal dissection. J Gastroenterol Hepatol 2010; 25(8): 1348-57.
9. Forero EA. Tratado de ultrasonografía endoscópica. Ultrasonido endoscópico en cáncer gástrico temprano. Editorial Atheneu; 2006.
10. Bennett C, Wang Y, Pan T. Endoscopic mucosal resection for early gastric cancer. Cochrane Database Syst Rev 2009; (4): CD004276.
11. Othman MO, Wallace MB. Endoscopic mucosal resection (EMR) and endoscopic submucosal dissection (ESD) in 2011, a Western perspective. Clin Res Hepatol Gastroenterol 2011; 35(4): 288-94.
12. Deprez PH. Current practice with endoscopic submucosal dissection in Europe: position statement from a panel of experts. Endoscopy 2010; 42(10): 853-8.
13. Gotoda T. Incidence of lymph node metastasis from early gastric cancer: estimation with a large number of cases at two large centers. Gastric Cancer 2000; 3: 219-25.
14. Hirasawa K. Risk assessment chart for curability of early gastric cancer with endoscopic submucosal dissection. Gastrointest Endosc 2011; 74: 1268-75.
15. Koeda K. Minimally invasive surgery for gastric cancer: the future standard of care. World J Surg 2011; 35(7): 1469-77.
16. Gotoda T. Endoscopic resection of early gastric cancer treated by guideline and expanded national cancer centre criteria. British Journal of Surgery 2010; 97: 868-871.
17. Lee H. Do we have enough evidence for expanding the indications of ESD for EGC? World J Gastroenterol 2011; 17(21): 2597-2601.
18. Park YM. The effectiveness and safety of endoscopic submucosal dissection compared with endoscopic mucosal resection for early gastric cancer: a systematic review and meta-analysis. Surg Endosc 2011; 25(8): 2666-77.
19. Takimoto K, Toyonaga T. Sedation with dexmedetomidine hydrochloride during endoscopic submucosal dissection of gastric cancer. Dig Endosc 2011; 23(2): 176-81.
20. Kiriyama S. Safe and effective sedation in endoscopic submucosal dissection for early gastric cancer: a randomized comparison between propofol continuous infusion and intermittent midazolam injection. J Gastroenterol 2010; 45(8): 831-7.
21. Toyonaga T. Retrospective study of technical aspects and complications of endoscopic sub mucosal dissection for laterally spreading tumors of the colorectum. Endoscopy 2010; 42: 714-722.
22. Toyonaga T. The performance of a novel ball-tipped Flush knife for endoscopic submucosal dissection: a casecontrol study. Aliment Pharmacol Ther 2010; 32: 908-915.
23. Toyonaga T. Invention of water jet short needle knives for endoscopic submucosal dissection. Endoscopy 2005; 37: A19.
24. Toyonaga T. Use of short needle knife for esophageal endoscopic submucosal dissection. Dig Endosc 2005; 17: 246-52.
25. Toyonaga T. Intraoperative bleeding in endoscopic submucosal dissection in the stomach and strategy for prevention and treatment. Dig Endosc 2006; 18: S1237.
26. Toyonaga T. Management to prevent bleeding during endoscopic submucosal dissection using the flush knife for gastric tumors. Dig Endosc 2007; 19: S14-8.
27. Fujiwara S, Toyonaga T. A randomized controlled trial of rebamipide plus rabeprazole for the healing of artificial ulcers after endoscopic submucosal dissection. J Gastroenterol 2011; 46(5): 595-602.
28. Kato T. Clinical trial: rebamipide promotes gastric ulcer healing by proton pump inhibitor after endoscopic submucosal dissection--a randomized controlled study. J Gastroenterol 2010; 45(3): 285-90.
29. Nonaka S. Safety of carbon dioxide insufflation for upper gastrointestinal tract endoscopic treatment of patients under deep sedation. Surg Endosc 2010; 24(7):1638-45.
30. Kim SH. Management of the complications of endoscopic submucosal dissection. World J Gastroenterol 2011; 17(31): 3575-9.
31. Japanese Gastric Cancer Association. Japanese classification of Gastric carcinoma: 2nd English edition. Gastric Cancer 1998; 1: 10-24.
32. Schlemper RJ. The Vienna classification of gastrointestinal epithelial neoplasia. Gut 2000; 47: 251-5.
33. Catalano F. The modern treatment of early gastric cancer: our experience in an Italian cohort. Surg Endosc 2009; 23: 1581-6.
34. Dinis-Ribeiro M. A European case series of endoscopic submucosal dissection for gastric superficial lesions. Gastrointes Endosc 2009; 69: 350-5.
35. Kim K. Do you have what it takes for challenging endoscopic submucosal dissection cases? World J Gastroenterol 2011; 17(31): 3580-3584.
36. Chung IK. Therapeutic outcomes in 1000 cases of endoscopic submucosal dissection for early gastric neoplasms: Korean ESD study Group multicenter study. Gastrointest Endosc 2009; 69: 1228-35.
37. Cho W. Endoscopic submucosal dissection for early gastric cancer: Quo vadis? World J Gastroenterol 2011; 17(21): 2623-2625.
38. Takenaka R. Risk factors associated with local recurrence of early gastric cancers after endoscopic submucosal dissection. Gastrointest Endosc 2008; 68: 887-94.
39. Cao Y. Metaanalysis of endoscopic submucosal dissection versus endoscopic mucosal resection for tumors of the gastrointestinal tract. Endoscopy 2009; 41(9): 751-7.
40. Nakamoto S. Indications for the use of endoscopic mucosal resection for early gastric cancer in Japan: a comparative study with endoscopic submucosal dissection. Endoscopy 2009; 41: 746-50.
41. Watanabe K. Clinical outcomes of EMR for gastric tumors: historical pilot evaluation between endoscopis submucosal dissection and conventional mucosal resection. Gastrointest Endosc. 2006; 63: 776-82.
42. Yamaguchi Y, Katusmi N, Aoki K, et al. Resection area of 15mm as dividing line for choosing strip biopsy or endoscopic submucosal dissection for mucosal gastric neoplasm. J Clin Gastroenterol 2007; 41: 472-476.
43. Toyonaga T. Endoscopic submucosal dissection using the Flush Knife and the Flush knife BT. Techniques in Gastrointestinal Endoscopy 2011; 13: 84-90.
44. Asakuma M. Ancillary N.O.T.E.S. procedures for early stage gastric cancer. Surg Oncol 2009; 18(2): 157-61.
45. ASGE Technology Committee, Kantsevoy SV, Adler DG, Conway JD, Diehl DL, Farraye FA, Kwon R, Mamula P, Rodríguez S, Shah RJ, Wong Kee Song LM, Tierney WM. Endoscopic mucosal resection and endoscopic submucosal dissection. Gastrointest Endosc 2008; 68(1): 11-8.
1. Retana A. An update in endoscopic management of gastric cancer. Curr Opin Gastroenterol 2011; 27: 576-582. [ Links ]
2. Gotoda T. Endoscopic resection of early gastric cancer. Gastric Cancer 2007; 10: 1-11. [ Links ]
3. Song KY, Hyung WJ, Kim HH, Han SU, Cho GS, Ryu SW, Lee HJ, Kim MC; Korean Laparoscopic Gastrointestinal Surgery Study (KLASS) Group. Is gastrectomy mandatory for all residual or recurrent gastric cancer following endoscopic resection? A large-scale Korean multi-center study. J Surg Oncol 2008; 98(1): 6-10. [ Links ]
4. Lee TH. Appropriate indications for endoscopic submucosal dissection of early gastric cancer according to tumor size and histopathological type. Gastrointest Endosc 2010; 71: 920-6. [ Links ]
5. The Paris endoscopic classification of superficial neoplastic lesions: esophagus, stomach and colon. Gastrointest Endosc 2003; 58: S3-S43. [ Links ]
6. Lee WS. Technical issues and new devices of ESD of early gastric cancer. World J Gastroenterol 2011; 17(31): 3585-3590. [ Links ]
7. Kwee RM, Kwee TC. The accuracy of endoscopic ultrasonography in differentiating mucosal from deeper gastric cancer. Am J Gastroenterol 2008; 103(7): 1801-9. Epub 2008 Jun 28. [ Links ]
8. Conlin A, Kaltenbach T, Kusano C, Matsuda T, Oda I, Gotoda T. Endoscopic resection of gastrointestinal lesions: advancement in the application of endoscopic submucosal dissection. J Gastroenterol Hepatol 2010; 25(8): 1348-57. [ Links ]
9. Forero EA. Tratado de ultrasonografía endoscópica. Ultrasonido endoscópico en cáncer gástrico temprano. Editorial Atheneu; 2006. [ Links ]
10. Bennett C, Wang Y, Pan T. Endoscopic mucosal resection for early gastric cancer. Cochrane Database Syst Rev 2009; (4): CD004276. [ Links ]
11. Othman MO, Wallace MB. Endoscopic mucosal resection (EMR) and endoscopic submucosal dissection (ESD) in 2011, a Western perspective. Clin Res Hepatol Gastroenterol 2011; 35(4): 288-94. [ Links ]
12. Deprez PH. Current practice with endoscopic submucosal dissection in Europe: position statement from a panel of experts. Endoscopy 2010; 42(10): 853-8. [ Links ]
13. Gotoda T. Incidence of lymph node metastasis from early gastric cancer: estimation with a large number of cases at two large centers. Gastric Cancer 2000; 3: 219-25. [ Links ]
14. Hirasawa K. Risk assessment chart for curability of early gastric cancer with endoscopic submucosal dissection. Gastrointest Endosc 2011; 74: 1268-75. [ Links ]
15. Koeda K. Minimally invasive surgery for gastric cancer: the future standard of care. World J Surg 2011; 35(7): 1469-77. [ Links ]
16. Gotoda T. Endoscopic resection of early gastric cancer treated by guideline and expanded national cancer centre criteria. British Journal of Surgery 2010; 97: 868-871. [ Links ]
17. Lee H. Do we have enough evidence for expanding the indications of ESD for EGC? World J Gastroenterol 2011; 17(21): 2597-2601. [ Links ]
18. Park YM. The effectiveness and safety of endoscopic submucosal dissection compared with endoscopic mucosal resection for early gastric cancer: a systematic review and meta-analysis. Surg Endosc 2011; 25(8): 2666-77. [ Links ]
19. Takimoto K, Toyonaga T. Sedation with dexmedetomidine hydrochloride during endoscopic submucosal dissection of gastric cancer. Dig Endosc 2011; 23(2): 176-81. [ Links ]
20. Kiriyama S. Safe and effective sedation in endoscopic submucosal dissection for early gastric cancer: a randomized comparison between propofol continuous infusion and intermittent midazolam injection. J Gastroenterol 2010; 45(8): 831-7. [ Links ]
21. Toyonaga T. Retrospective study of technical aspects and complications of endoscopic sub mucosal dissection for laterally spreading tumors of the colorectum. Endoscopy 2010; 42: 714-722. [ Links ]
22. Toyonaga T. The performance of a novel ball-tipped Flush knife for endoscopic submucosal dissection: a case–control study. Aliment Pharmacol Ther 2010; 32: 908-915. [ Links ]
23. Toyonaga T. Invention of water jet short needle knives for endoscopic submucosal dissection. Endoscopy 2005; 37: A19. [ Links ]
24. Toyonaga T. Use of short needle knife for esophageal endoscopic submucosal dissection. Dig Endosc 2005; 17: 246-52. [ Links ]
25. Toyonaga T. Intraoperative bleeding in endoscopic submucosal dissection in the stomach and strategy for prevention and treatment. Dig Endosc 2006; 18: S123–7. [ Links ]
26. Toyonaga T. Management to prevent bleeding during endoscopic submucosal dissection using the flush knife for gastric tumors. Dig Endosc 2007; 19: S14-8. [ Links ]
27. Fujiwara S, Toyonaga T. A randomized controlled trial of rebamipide plus rabeprazole for the healing of artificial ulcers after endoscopic submucosal dissection. J Gastroenterol 2011; 46(5): 595-602. [ Links ]
28. Kato T. Clinical trial: rebamipide promotes gastric ulcer healing by proton pump inhibitor after endoscopic submucosal dissection--a randomized controlled study. J Gastroenterol 2010; 45(3): 285-90. [ Links ]
29. Nonaka S. Safety of carbon dioxide insufflation for upper gastrointestinal tract endoscopic treatment of patients under deep sedation. Surg Endosc 2010; 24(7):1638-45. [ Links ]
30. Kim SH. Management of the complications of endoscopic submucosal dissection. World J Gastroenterol 2011; 17(31): 3575-9. [ Links ]
31. Japanese Gastric Cancer Association. Japanese classification of Gastric carcinoma: 2nd English edition. Gastric Cancer 1998; 1: 10-24. [ Links ]
32. Schlemper RJ. The Vienna classification of gastrointestinal epithelial neoplasia. Gut 2000; 47: 251-5. [ Links ]
33. Catalano F. The modern treatment of early gastric cancer: our experience in an Italian cohort. Surg Endosc 2009; 23: 1581-6. [ Links ]
34. Dinis-Ribeiro M. A European case series of endoscopic submucosal dissection for gastric superficial lesions. Gastrointes Endosc 2009; 69: 350-5. [ Links ]
35. Kim K. Do you have what it takes for challenging endoscopic submucosal dissection cases? World J Gastroenterol 2011; 17(31): 3580-3584. [ Links ]
36. Chung IK. Therapeutic outcomes in 1000 cases of endoscopic submucosal dissection for early gastric neoplasms: Korean ESD study Group multicenter study. Gastrointest Endosc 2009; 69: 1228-35. [ Links ]
37. Cho W. Endoscopic submucosal dissection for early gastric cancer: Quo vadis? World J Gastroenterol 2011; 17(21): 2623-2625. [ Links ]
38. Takenaka R. Risk factors associated with local recurrence of early gastric cancers after endoscopic submucosal dissection. Gastrointest Endosc 2008; 68: 887-94. [ Links ]
39. Cao Y. Metaanalysis of endoscopic submucosal dissection versus endoscopic mucosal resection for tumors of the gastrointestinal tract. Endoscopy 2009; 41(9): 751-7. [ Links ]
40. Nakamoto S. Indications for the use of endoscopic mucosal resection for early gastric cancer in Japan: a comparative study with endoscopic submucosal dissection. Endoscopy 2009; 41: 746-50. [ Links ]
41. Watanabe K. Clinical outcomes of EMR for gastric tumors: historical pilot evaluation between endoscopis submucosal dissection and conventional mucosal resection. Gastrointest Endosc. 2006; 63: 776-82. [ Links ]
42. Yamaguchi Y, Katusmi N, Aoki K, et al. Resection area of 15mm as dividing line for choosing strip biopsy or endoscopic submucosal dissection for mucosal gastric neoplasm. J Clin Gastroenterol 2007; 41: 472-476. [ Links ]
43. Toyonaga T. Endoscopic submucosal dissection using the Flush Knife and the Flush knife BT. Techniques in Gastrointestinal Endoscopy 2011; 13: 84-90. [ Links ]
44. Asakuma M. Ancillary N.O.T.E.S. procedures for early stage gastric cancer. Surg Oncol 2009; 18(2): 157-61. [ Links ]
45. ASGE Technology Committee, Kantsevoy SV, Adler DG, Conway JD, Diehl DL, Farraye FA, Kwon R, Mamula P, Rodríguez S, Shah RJ, Wong Kee Song LM, Tierney WM. Endoscopic mucosal resection and endoscopic submucosal dissection. Gastrointest Endosc 2008; 68(1): 11-8. [ Links ]











 text in
text in