Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Revista colombiana de Gastroenterología
Print version ISSN 0120-9957
Rev Col Gastroenterol vol.29 no.2 Bogotá Apr./June 2014
Endometriosis in the Colon with Intestinal Obstruction: Case Report and Literature Review
Dumar Rodríguez Tello, MD. (1), William Otero Regino, MD. (2), Martín Gómez Zuleta, MD. (3)
(1) Emergency Medicine Physician at the Clínica Fundadores in Bogotá, Colombia.
(2) Professor of Medicine in the Gastroenterology Unit at the Universidad Nacional de Colombia and Gastroenterologist at the Clínica Fundadores in Bogotá, Colombia.
(3) Professor of Medicine in the Gastroenterology Unit at the Universidad Nacional de Colombia and Gastroenterologist at the Hospital El Tunal and Hospital de Kennedy in Bogota, Colombia.
Received: 27-08-13 Accepted: 08-15-14
Abstract
Endometriosis is a condition that primarily affects women of reproductive age since the intestinal tract is the most commonly affected extra-genital site. Its clinical presentation varies, but since it rarely presents together with intestinal obstruction, it is difficult to differentiate from malignancy prior to surgery. Colorectal compromises can mimic or coexist with different chronic gastrointestinal diseases thus hindering diagnosis. We report the case of a 48 -year-old patient with box intestinal obstruction secondary to endometriosis in the sigmoid colon. In addition, we present a literature review of intestinal endometriosis with emphasis on differential diagnosis and the involvement of bacterial infections in the etiology and reactivation of endometriosis.
Keywords
Endometriosis, intestinal obstruction, infection.
INTRODUCTION
Endometriosis (EMT) is defined as a chronic inflammatory condition characterized by the presence of endometrial glands and stroma outside the uterus (1). Its discovery is controversial, John Sampson is commonly considered to have made the first pathophysiology description, but his work would not have been possible without the contribution of Thomas Cullen (2). EMT is an estrogen dependent condition, commonly associated with chronic pelvic pain and infertility. It affects between 6% and 10% of reproductive age women, but its prevalence increases to between 30% and 50% in infertile women (1). It commonly manifests in the peritoneum, ovaries, rectovaginal septum, pulmonary system, central nervous system, skin and striated muscles (3, 4).
The intestinal tract is the most commonly affected extra genital area (3, 5). Prevalence varies from 5.3% to 12% (4, 6, 785 patients (5.4%). The average age at presentation is 39 years (5). The most frequent location is the rectosigmoid (71%), followed by the appendix (19%), terminal ileum (6.7%), cecum (5.5%) and the transverse colon (0.5%) (3, 4, 6-8).
When the intestines are involved, the main symptom is abdominal pain that worsens during the menstrual period (3, 7-9). 85 patients (5.4%Other symptoms include changes in intestinal habits, cyclical rectal bleeding, dyschezia, rectal tenesmus, abdominal distension, diarrhea, recurrent constipation and, occasionally, partial or complete intestinal obstruction and palpable abdominal masses (6, 885 patients (5.4%).
We present the case of a patient, and we review the literature. The patient was admitted to our institution with an intestinal obstruction due to endometriosis in the sigmoid colon.
CLINICAL CASE
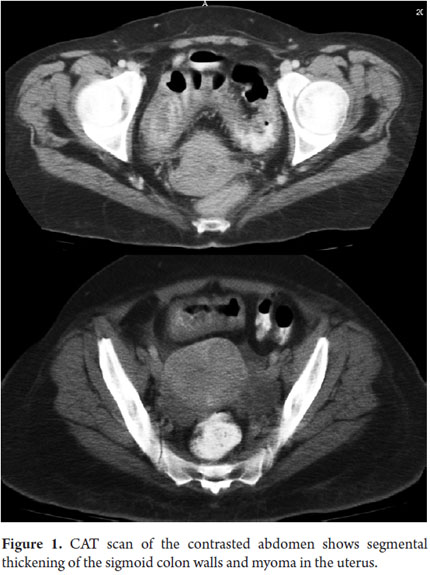
A 48 year old woman entered the intensive care unit at the Fundadores Clinic in Bogota. She had been suffering from persistently decreased caliber of her feces, diffuse posterior abdominal pain, vomiting and abdominal distension for 10 days. Her medical history included dysmenorrhea, uterine fibroids, iron deficiency anemia and left urolithiasis. A month and a half before admission to our clinic, she had been hospitalized for 12 days with E. coli pyelonephritis which had been treated with meropenem. After treatment, she developed colitis secondary to c. difficile and was treated with metrodinazole, but without improvement. She was switched to oral vancomycin for 10 days. This resolved the clinical presentation. While hospitalized the second time, a colonoscopy was performed. It found a sigmoid stenosis located 28cm from the rectum that could not be removed. Biopsies taken from that site showed no alterations. A double contrast enema with was performed, but it was not possible to visualize the whole colon. A complete abdominal CAT scan with contrast showed sigmoid thickening (Figure 1).
With a diagnosis of stenosis and partial intestinal obstruction, laparoscopic en-bloc resection of the sigmoid colon and a Hartmann colostomy were performed. The surgery uncovered an inflammatory process and fibrosis in the pelvis. Consequently, the gynecologist performed a hysterectomy and a bilateral salpingo-oophorectomy. The results from pathology were, " endometriosis in the sigmoid colon. The muscularis is infiltrated by stroma and endometrial glands, and there is edema and vascular congestion in the mucosa. Tumor processes were not identified. The ovaries and left fallopian tube have endometriosis."
INTESTINAL OBSTRUCTION RESULTING FROM ENDOMETRIOSIS
Intestinal obstruction secondary to EMT is an infrequent pathology, occurring in less than 1% of all cases (10). In a study with 163 patients with intestinal EMT, ten patients presented partial intestinal obstructions (11). In most cases, obstruction was not initially diagnosed but was discovered in the pathology results. Intestinal obstruction may occur in patients with intestinal EMT who may concomitantly presently colonic neoplasia (12). In a study with 16 cases of intestinal obstruction due to endometriosis, microscopic findings showed a greater concentration of glands and stroma in the serosa and the external muscular layers when the ileum was compromised while obstructions in the sigmoid have greater implications for the inner circular muscle and the submucosa (13).
Intestinal EMT manifests as superficial or profound lesions. The most frequently affected intestinal layer is the serosa, followed by the muscularis propria (12, 14). The superficial lesions endanger the serosa and are generally the size of the head of a pin and surrounded by scarce fibrotic tissue (5). The deepest lesions endanger the muscularis propria or even the submucosa and mucosa in patients with gastrointestinal symptoms (4, 15). This involvement produces secondary fibrosis which provokes thickening of the wall and decreases the intestinal lumen. When endometrial lesions affect the rectum and/or sigmoid colon beyond the internal muscular layer and more than 40% of the circumference of these organs is compromised, the recommendation is segmented intestinal resection (16).
Endometriosis affected the sigmoid muscular layer in the case described above.
DIFFERENTIAL DIAGNOSIS
Colorectal EMT can imitate or coexist with various other gastrointestinal diseases such as Crohn's disease, ulcerative colitis, ischemic colitis, diverticulitis, irritable bowel syndrome, and even colon and rectum tumors when intraluminal endometriomas are present. This can complicate diagnosis which can lead to aggressive surgical treatment associated with high morbidity and mortality (6, 17, 18and evaluated them for a variety of gross and histologic changes. Cases with preneoplastic or neoplastic changes were excluded specifically because they were the subject of a previous study. The patients ranged in age from 28 to 56 years (mean age, 44 years). In a case and control study of 5,540 women with endometriosis, there was a higher probability of being diagnosed with irritable bowel syndrome among women with endometriosis than among women in the control group (OR 3.5 CI 95%, 3.13.9). There was also a higher probability of being treated for inflammatory pelvic disease before (OR 5.9 CI 95%, 5.16.9) and after (OR 3.8 CI 95%, 3.14.6) being diagnosed with endometriosis (19). In another study of 7,025 women with endometriosis, 65% were misdiagnosed with another condition and 46% were seen by five doctors or more before the diagnosis (20). When the ileum is compromised, the differential diagnosis must check for Crohn's disease, since both diseases may produce inflammation, hardening, thickening and stenosis in the small intestine (21). A study of a cohort of 37,661 women with endometriosis showed a 50% increase in the risk of inflammatory intestinal disease. This risk persisted after 20 years of monitoring (21).
EMT is usually a benign disease, yet it is estimated that 1% of the cases are associated with cancer, especially when both conditions are present in the ovary. This mainly affects postmenopausal woman (21). The frequency of endometriosis and cancer in the sigmoid colon was calculated at 1:156 (5). Malignant tumors should be suspected in patients with abdominal pain or rectal bleeding and a previous history of quiescent endometriosis, especially when the patient has received estrogen treatment (12). Primary colon carcinomas always involve the mucosa and are often associated with adenomatous changes or a neoplastic polyp in the adjacent epithelium. They extend from the mucosa through the intestinal wall until the serous surface or to the adjacent fat (12). In contrast, endometriosis, and the cancers it may harbor, most frequently involve the outermost layers of the intestine wall (occasionally associated with adhesions): the serous, sub-serous and muscularis propria, occasionally extending into the sub-mucosa (12). Generally useful characteristics that help distinguish neoplasia from intestinal endometriosis include the characteristic location within the intestinal wall with extensive mural involvement and less prominent changes in the mucosa, association with serositis or post-operational adhesions and the presence of small mural cysts or hemorrhaging (6).
ETIOLOGY
The etiology of EMT is complex and multifactorial. Several theories try to explain its physiopathology. The theory of retrograde menstruation proposed by Sampson in the 1920's states that fragments of the endometrium disseminate. This is supported by the discovery of menstrual blood in the peritoneal liquid in 90% of healthy women with permeable fallopian tubes who receive laparoscopies during their premenstrual cycle (23).
The theory of coelomic metaplasia involves a transformation of the peritoneal tissue to ectopic endometrial tissue induced by hormonal or endogenous immunological stimulus (23). Another consideration is that the embryonic remains of the paramesonephric ducts migrate and have the capacity of developing endometrial lesions under the influence of estrogens beginning in puberty (23). This theory is supported by a study that found that women whose uteruses were exposed to diethylstilbestrol had a relative risk of 1.8 (CI 95%, 1.22.8) of developing endometriosis (24). A more recent possibility suggests that extra uterine stem cells from bone marrow can be differentiated into endometrial tissue (23). The support for this theory is derived from cases of histologically confirmed endometriosis in patients without menstrual endometrium such as people with the Mayer-Rokitansky-Küster-Hauser syndrome (MRKH) and men with prostate cancer who receive high dose estrogen treatments (23).
EMT is a chronic inflammatory disease that involves secondary inflammatory mediators. Primary inflammatory mediators like endotoxins or lipopolysaccharides (LPS) of gram-negative bacteria can be the triggers of secondary inflammatory mediators such as cytokines, chemokines, maturation growth factors or macrophage activation in the pelvis (25, 26). The bacterial hypothesis suggests that Shigella or similar bacteria can detonate immunological changes in the pelvic peritoneum which initiate etiopathogenesis of the endometriosis (25). Some patients with intestinal EMT present bacterial overgrowth which is speculated to be secondary to the neuromuscular alteration produced by the entity (26). EMT in Rhesus monkeys is associated with alterations in intestinal microflora in which there is a low concentration of lactobacilli and a high concentration of Gram-negative bacteria (27). Khan et al. performed a study which proved for the first time that women's menstrual blood with endometriosis is more contaminated with Escherichia coli than the blood of women in a control group. They also showed that women with EMT had higher levels of endotoxins in their menstrual blood and therefore in the peritoneal liquid due to the reflux of menstrual blood in the pelvis (28). This can promote the growth of Toll-4 receptor (TRL4) mediated by EMT as evidenced by increased endometrial cell growth in response to LPS and the suppression of these effects mediated by the anti-TLR4 antibody (28). In contrast, an experimental endometriosis study in mice showed no significant difference in the total bacterial load or in the number of lactobacilli in experimental animal colons when compared to controls (29). The patient mentioned in this study presented pyelonephritis from E. Coli and pseudomembranous colitis from C. difficile before the intestinal obstruction from EMT. It is possible that the inflammatory response from these infectious entities could reactivate EMT causing an increase in lesions and triggering intestinal obstruction.
DIAGNOSIS
Currently, the "gold standard" for a definitive EMT diagnosis is visual laparoscopic inspection with histological confirmation. This also allows ablative and corrective treatment in the same surgical treatment (30). Colonoscopy with histology is rarely used to diagnose intestinal endometriosis, unless there are intraluminal lesions. It has low sensitivity except when there is evident compromise of the mucosa (31). However, it is the exam of choice for every patient with rectal bleeding, especially if bleeding is cyclical. It is the first exam performed on patients with rectal bleeding since it can exclude malignancies and other causes of bleeding, but it has a low sensitivity for diagnosing colorectal endometriosis (32). The most common finding is eccentric thickening of the wall followed by polypoid lesions. The histological diagnostic performance of endoscopic biopsies is high when lesions are accompanied by superficial nodules, and low when they are not present. This is probably due to the fact that involvement of the colon's mucosa is rare (31). The colonoscopy and the biopsy performed on our patient showed no evidence of EMT. This correlates with what is described in the literature. Barium enemas with double contrast have been used to diagnose intestinal endometriosis (32, 33). The main limitation is the difficulty in differentiating intestinal endometriosis from other pathologies. Other limitations include the use of ionizing radiation in women during reproductive ages, the impossibility of estimating the degree of infiltration of the intestinal wall, and identification of extension to other pelvic organs (33). Endoscopic rectosigmoid ultrasonography is used to establish the depth of the EMT's infiltration into the intestinal wall when performed prior to surgery. It is possible to distinguish between patients for whom intestinal resection is indicated and those that may be treated with laparoscopic surgery without entering the intestine (32). Preoperative magnetic resonance (MR), after cleaning the intestines allows a clear and anatomical delimitation of lesions in the sigmoidal colon and the rectum (33). The depth of infiltration of endometrial nodules in the intestinal wall cannot be precisely determined by an MRI (33). CAT scans and MRIs can reveal thickening of the intestinal wall, but they cannot provide a diagnosis of the tissue unless a directed biopsy is requested (30). Transvaginal echography has no value for diagnosing peritoneal endometriosis, but it is a useful tool for diagnosing and, excluding a diagnosis of, ovarian endometriosis (30). A multivariate analysis of four biomarkers (annexin V, vascular endothelial growth factor (VEGF), CA-125 and cell adhesion molecule I (sICAM-1) or glycodelin) in plasma samples obtained during the menstrual phase can diagnose endometriosis which is undetectable through ultrasound. The sensitivity of this test is 81% to 90% and its specificity is 63% to 81%. (20)
TREATMENT
Treatment options consist primarily of medical therapy and surgical therapy (34, 35). Segmented laparoscopic resection of the rectum and sigmoid colon improve symptoms related to pain and meet the essential objective of treating intestinal endometriosis. Consequently, they significantly improve the patients´ quality of life (34, 35). The hormonal treatment for suppressing the ovarian function lasts 6 months and decreases the pain associated with endometriosis. The most frequently used hormonal medications are oral contraceptives, danazol, gestrinone, medroxyprogesterone acetate and agonists of gonadotropin-releasing hormone. They are equally efficient, but their secondary effects and cost profiles differ (30). Patients with obstructive symptoms from intestinal EMT should undergo surgical resection (4). Conservative surgery has shown benefits in women who wish to preserve their reproductive organs: out of 54 women who underwent conservative surgery, 23 became pregnant (11). When comparing laparoscopic colonic resection with laparotomy in patients with intestinal EMT, both options lead to similar symptomatic improvement after surgery, but those who underwent laparoscopic treatment had significantly lower rates of surgical complications and also had the highest rates of spontaneous pregnancy (7, 36).
CONCLUSIONS
Intestinal EMT is a pathology that should be clinically suspected in women at reproductive ages as a possible cause of diffuse abdominal pain, rectal bleeding and intestinal obstruction. Also, intestinal EMT can imitate or coexist with various gastrointestinal pathologies such as neoplasia, inflammatory intestinal disease and irritable bowel syndrome. Additional research needs to be done in order to determine the role that bacterial infections might have in this pathophysiology since the theoretical possibility exists that they might be related to the etiology itself or to reactivation of the inflammatory process that leads to EMT.
REFERENCES
1. Rogers PAW, D'Hooghe TM, Fazleabas A, Giudice LC, Montgomery GW, Petraglia F, et al. Defining future directions for endometriosis research: workshop report from the 2011 World Congress of Endometriosis In Montpellier, France. Reprod Sci Thousand Oaks Calif. 2013;20(5):483-99. [ Links ]
2. Benagiano G, Brosens I. Who identified endometriosis? Fertil Steril. 2011;95(1):13-6. [ Links ]
3. Veeraswamy A, Lewis M, Mann A, Kotikela S, Hajhosseini B, Nezhat C. Extragenital endometriosis. Clin Obstet Gynecol. 2010;53(2):449-66. [ Links ]
4. Prystowsky JB, Stryker SJ, Ujiki GT, Poticha SM. Gastrointestinal endometriosis. Incidence and indications for resection. Arch Surg Chic Ill 1960. 1988;123(7):855-8. [ Links ]
5. Bergqvist A. Different types of extragenital endometriosis: a review. Gynecol Endocrinol Off J Int Soc Gynecol Endocrinol. 1993;7(3):207-21. [ Links ]
6. Yantiss RK, Clement PB, Young RH. Endometriosis of the intestinal tract: a study of 44 cases of a disease that may cause diverse challenges in clinical and pathologic evaluation. Am J Surg Pathol. 2001;25(4):445-54. [ Links ]
7. Wills HJ, Reid GD, Cooper MJW, Tsaltas J, Morgan M, Woods RJ. Bowel resection for severe endometriosis: an Australian series of 177 cases. Aust N Z J Obstet Gynaecol. 2009;49(4):415-8. [ Links ]
8. Cameron IC, Rogers S, Collins MC, Reed MW. Intestinal endometriosis: presentation, investigation, and surgical management. Int J Colorectal Dis. 1995;10(2):83-6. [ Links ]
9. Kaufman LC, Smyrk TC, Levy MJ, Enders FT, Oxentenko AS. Symptomatic intestinal endometriosis requiring surgical resection: clinical presentation and preoperative diagnosis. Am J Gastroenterol. 2011;106(7):1325-32. [ Links ]
10. De Jong MJH, Mijatovic V, van Waesberghe JHTM, Cuesta MA, Hompes PGA. Surgical outcome and long-term follow-up after segmental colorectal resection in women with a complete obstruction of the rectosigmoid due to endometriosis. Dig Surg. 2009;26(1):50-5. [ Links ]
11. Weed JC, Ray JE. Endometriosis of the bowel. Obstet Gynecol.;69(5):727-30. [ Links ]
12. Yantiss RK, Clement PB, Young RH. Neoplastic and pre-neoplastic changes in gastrointestinal endometriosis: a study of 17 cases. Am J Surg Pathol. 2000;24(4):513-24. [ Links ]
13. Macafee CH, Greer HL. Intestinal endometriosis. A report of 29 cases and a survey of the literature. J Obstet Gynaecol Br Emp. 1960;67:539-55. [ Links ]
14. Kavallaris A, Köhler C, Kühne-Heid R, Schneider A. Histopathological extent of rectal invasion by rectovaginal endometriosis. Hum Reprod Oxf Engl. 2003;18(6):1323-7. [ Links ]
15. naf V, El Nakadi I, Simon P, Van de Stadt J, Fayt I, Simonart T, et al. Preferential infiltration of large bowel endometriosis along the nerves of the colon. Hum Reprod Oxf Engl. 2004;19(4):996-1002. [ Links ]
16. Abrão MS, Podgaec S, Dias JA Jr, Averbach M, Silva LFF, Marino de Carvalho F. Endometriosis lesions that compromise the rectum deeper than the inner muscularis layer have more than 40% of the circumference of the rectum affected by the disease. J Minim Invasive Gynecol. 2008;15(3):280-5. [ Links ]
17. Ong SY, Sim SY, Johnston M, Crowley P, Froomes P. Education and imaging. Gastrointestinal: refractory ulcerative colitis complicated by colonic stricturing endometriosis. J Gastroenterol Hepatol. 2012;27(1):181. [ Links ]
18. Samet JD, Horton KM, Fishman EK, Hruban RH. Colonic endometriosis mimicking colon cancer on a virtual colonoscopy study: a potential pitfall in diagnosis. Case Rep Med. 2009;2009:379578. [ Links ]
19. Seaman HE, Ballard KD, Wright JT, de Vries CS. Endometriosis and its coexistence with irritable bowel syndrome and pelvic inflammatory disease: findings from a national case-control study--Part 2. BJOG Int J Obstet Gynaecol. 2008;115(11):1392-6. [ Links ]
20. Vodolazkaia A, El-Aalamat Y, Popovic D, Mihalyi A, Bossuyt X, Kyama CM, et al. Evaluation of a panel of 28 biomarkers for the non-invasive diagnosis of endometriosis. Hum Reprod Oxf Engl. 2012;27(9):2698-711. [ Links ]
21. Jess T, Frisch M, Jørgensen KT, Pedersen BV, Nielsen NM. Increased risk of inflammatory bowel disease in women with endometriosis: a nationwide Danish cohort study. Gut. 2012;61(9):1279-83. [ Links ]
22. Sampson JA. Metastatic or Embolic Endometriosis, due to the Menstrual Dissemination of Endometrial Tissue into the Venous Circulation. Am J Pathol. 1927;3(2):93-110.43. [ Links ]
23. Burney RO, Giudice LC. Pathogenesis and pathophysiology of endometriosis. Fertil Steril. 2012;98(3):511-9. [ Links ]
24. Missmer SA, Hankinson SE, Spiegelman D, Barbieri RL, Michels KB, Hunter DJ. In utero exposures and the incidence of endometriosis. Fertil Steril. 2004;82(6):1501-8. [ Links ]
25. Kodati VL, Govindan S, Movva S, Ponnala S, Hasan Q. Role of Shigella infection in endometriosis: a novel hypothesis. Med Hypotheses. 2008;70(2):239-43. [ Links ]
26. Mathias JR, Franklin R, Quast DC, Fraga N, Loftin CA, Yates L, et al. Relation of endometriosis and neuromuscular disease of the gastrointestinal tract: new insights. Fertil Steril. 1998;70(1):81-8. [ Links ]
27. Bailey MT, Coe CL. Endometriosis is associated with an altered profile of intestinal microflora in female rhesus monkeys. Hum Reprod Oxf Engl. 2002;17(7):1704-8. [ Links ]
28. Khan KN, Kitajima M, Hiraki K, Yamaguchi N, Katamine S, Matsuyama T, et al. Escherichia coli contamination of menstrual blood and effect of bacterial endotoxin on endometriosis. Fertil Steril. 2010;94(7):2860-2863.e1-3. [ Links ]
29. Appleyard CB, Cruz ML, Rivera E, Hernández GA, Flores I. Experimental endometriosis in the rat is correlated with colonic motor function alterations but not with bacterial load. Reprod Sci Thousand Oaks Calif. 2007;14(8):815-24. [ Links ]
30. Kennedy S, Bergqvist A, Chapron C, D'Hooghe T, Dunselman G, Greb R, et al. ESHRE guideline for the diagnosis and treatment of endometriosis. Hum Reprod Oxf Engl. 2005;20(10):2698-704. [ Links ]
31. Kim K-J, Jung S-S, Yang S-K, Yoon SM, Yang D-H, Ye BD, et al. Colonoscopic findings and histologic diagnostic yield of colorectal endometriosis. J Clin Gastroenterol. 2011;45(6):536-41. [ Links ]
32. Roseau G, Dumontier I, Palazzo L, Chapron C, Dousset B, Chaussade S, et al. Rectosigmoid endometriosis: endoscopic ultrasound features and clinical implications. Endoscopy. 2000;32(7):525-30. [ Links ]
33. Loubeyre P, Copercini M, Frossard JL, Wenger JM, Petignat P. Pictorial review: rectosigmoid endometriosis on MRI with gel opacification after rectosigmoid colon cleansing. Clin Imaging. 2012;36(4):295-300. [ Links ]
34. Keckstein J, Wiesinger H. Deep endometriosis, including intestinal involvement--the interdisciplinary approach. Minim Invasive Ther Allied Technol MITAT Off J Soc Minim Invasive Ther. 2005;14(3):160-6. [ Links ]
35. Bassi MA, Podgaec S, Dias JA Jr, D'Amico Filho N, Petta CA, Abrao MS. Quality of life after segmental resection of the rectosigmoid by laparoscopy in patients with deep infiltrating endometriosis with bowel involvement. J Minim Invasive Gynecol. 2011;18(6):730-3. [ Links ]
36. Ruffo G, Scopelliti F, Scioscia M, Ceccaroni M, Mainardi P, Minelli L. Laparoscopic colorectal resection for deep infiltrating endometriosis: analysis of 436 cases. Surg Endosc. 2010;24(1):63-7. [ Links ]











 text in
text in