Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Revista colombiana de Gastroenterología
Print version ISSN 0120-9957
Rev Col Gastroenterol vol.29 no.2 Bogotá Apr./June 2014
Two Case Reports of Boerhaave's Syndrome
Martín Alonso Gómez Zuleta, MD. (1), David Andrés Viveros Carreño, MD. (2), Melissa Buitrago, MD. (3)
(1) Gastroenterology Unit at the Universidad Nacional de Colombia and Gastroenterologist at Hospital El Tunal in Bogotá, Colombia.
(2) Hospital El Tunal in Bogotá, Colombia.
(3) Surgeon at the Universidad Nacional de Colombia in Bogotá, Colombia.
Received: 16-11-13 Accepted: 08-05-14
Abstract
Boerhaave's syndrome is a type of esophageal rupture caused by a rapid increase in intraluminal pressure in a previously healthy esophagus. The rupture usually occurs in the distal third of the esophagus. This condition has a high mortality rate and is very rare with very few cases reported in the literature. Estimates of mortality rates range as high as 40%, but management by experienced physicians combined with early diagnosis early has been shown to positively impact patients' prognoses. Unfortunately due to the condition´s low frequency, no clear consensus exists regarding the best therapeutic approach. Here we present the clinical features of two patients who were diagnosed at our institution, present diagnostic images, and review the topic.
Keywords
Boerhaave's syndrome, esophageal perforation.
INTRODUCTION
Boerhaave's syndrome is a rare clinical condition first described by the Danish Medical Hermann Boerhaave in 1724 (1). It represents 10-20% of esophageal ruptures and is defined as the spontaneous rupture of the total thickness of the esophageal wall due to a barogenic trauma induced by uncoordinated presence of emesis associated with pyloric closure and diaphragmatic contraction against a closed cricopharyngeus muscle (2).
Negative intrathoracic pressure and ventilatory movements lead to the passage of gastrointestinal content to the mediastinum and pleura which eventually results in the development of mediastinitis and septic compromise as well as cardiopulmonary compromise due to collection (2). It usually occurs in the distal third of the esophagus, towards the left side, two to three inches from the esophagogastric junction which is considered to be the weakest area of the organ (1, 3). In general the size of the perforation varies greatly, but can measure up to 10 cm (4).
CLINICAL CASE 1
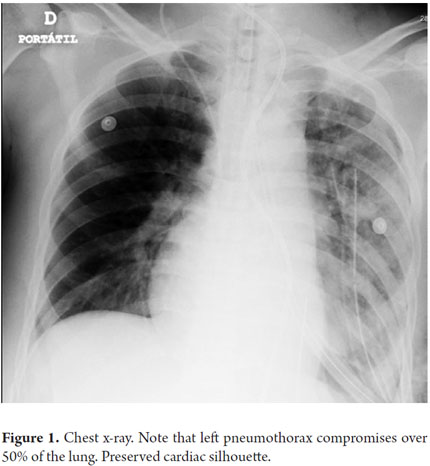
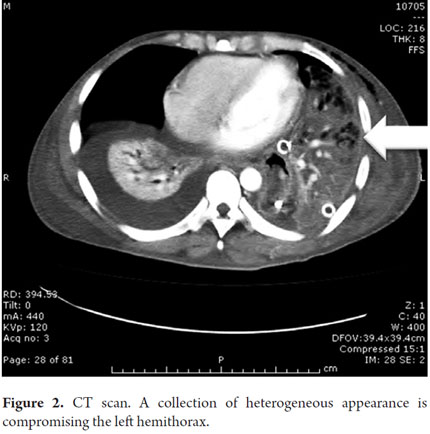
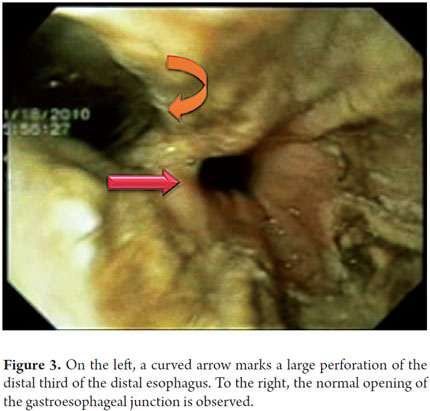
A 34 year old indigent man was brought to the hospital by the police in an altered state of consciousness and in respiratory distress. During the short interview period the patient described eight hours of multiple emetic episodes with hematemesis and some chest pain. A chest x-ray showed a large left pleural effusion (Figure 1) which led to a thoracostomy that obtained cloudy material. Given this finding, a CAT scan was performed. It showed a collapsed lung with a collection of material of heterogeneous appearance (Figure 2). The patient's general condition was progressively deteriorating, so he was taken to surgery. Since the patient had hematemesis, an upper gastrointestinal endoscopy was performed before surgery. It showed large hole in the left wall of the distal esophagus (Figure 3). During preparation for an open thoracotomy, it was decided to enter through the perforation. A collapsed left lung was found with large amounts of contaminated material occupying the left hemithorax and pericardium. Even traces of food (Figure 4) could be seen.
During surgery, the defect was corrected, the pleural compromised cavity was cleaned and drained, a protective gastrostomy was inserted, and the patient was moved to the ICU where he was treated with broad spectrum antibiotics. Unfortunately given the level of compromise at admission, the patient did not survive.
CLINICAL CASE 2
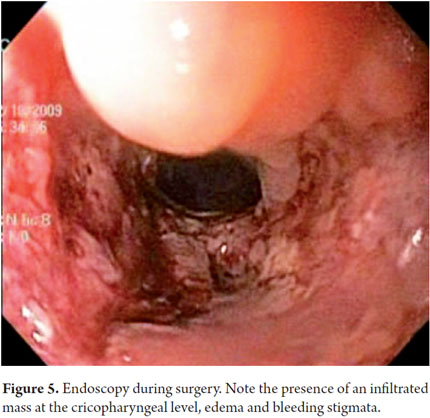
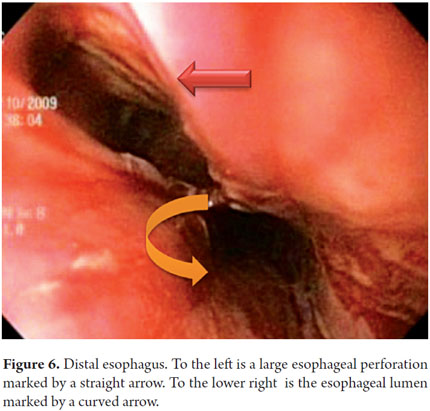
An 82 year old female outpatient who had clinical symptoms of dysphagia when trying to swallow solid food and weight loss underwent upper endoscopy. It showed an upper esophageal lesion which compromised 50% of the passage. Biopsies showed that the middle and distal esophagus were normal with an intact Z line. Following the procedure, the patient complained of odynophagia and an hour later presented multiple episodes of gagging and hematemesis with evidence of mild respiratory distress. A chest X-ray showed left pneumothorax. The patient was sent to surgery. An endoscopy prior to surgery showed the presence of a lesion and bleeding stigmata due to the biopsies (Figure 5). We advanced 27 cm in until the endoscope reached a large perforation in the left wall (Figure 6). The perforation probably occurred because the patient could not expel air from the first endoscopy as the edema produced by biopsies prevented adequate cricopharyngeal relaxation. The primary wound was closed, and then radiation therapy was used to treat the original lesion which was squamous cell carcinoma. The outcome was satisfactory.
DISCUSSION
Boerhaave's syndrome is most often seen in elderly adults in the sixth and seventh decades of life without regard to race, although it occurs more frequently in men than in women (4, 5). Some series show that it occurs more frequently among patients with a history of chronic alcohol consumption.
Its clinical presentation is nonspecific, but, as in our first patient, the main finding is often epigastric-chest pain which varies depending upon whether emesis is present (3, 4). Mackler's triad consisting of emesis, pain and subcutaneous emphysema is documented in a minority of patients (2, 5).
The diagnosis requires a high degree of clinical suspicion supported by images. It is very important to note that upon admission virtually all patients show an abnormality in a simple chest x-ray as was evident in our cases. This should be the first consideration in the initial evaluation of patients in whom we suspect this diagnosis. We are then able to find widened mediastinum, mediastinal and subcutaneous emphysema, hydropneumothorax and atelectasis (2, 3, 4). Using contrast medium and/or a CAT scan makes use of most diagnostic algorithms and has a false negative rate of only about 10% (3, 4). Since the chief complaint is chest pain, major differential diagnoses include acute myocardial infarction, pericarditis, spontaneous pneumothorax and pneumonia (2).
Since this event occurs very infrequently, there is no consensus regarding its treatment. The most conservative treatment consists of broad spectrum antibiotics with percutaneous drainage of abscesses or collections. This is classically indicated for cases that meet certain characteristics such as diagnosis more than 48 hours after occurrence, small lesions, absence of systemic inflammatory response, and absence of contamination in the pleural space (1). Although conservative treatment has shown a good survival rate it is now considered that most patients can safely undergo surgery with a positive impacting on results.
Endoscopic treatment includes the use of clips, sutures and self-expanding metallic stents. This type of treatment is indicated for patients whose compromised is too great to undergo surgery or for those who have lesions without septic compromise and a maximum size of 2.5 cm per perforation (4, 6). It has shown good results although most experience is in cases of iatrogenic esophageal ruptures which have characteristics that are different from those of the Boerhaave syndrome when it is detected early. Surgical treatment is normally reserved for patients who are diagnosed within 24 hours of occurrence because it is possible to perform an esophagectomy or to create an esophago-cutaneous fistula during surgery and to repair the lesion. The main purpose is always to drain the pleural cavity and to use of gastrostomy or jejunostomies to reduce pressure on the damaged area and reduce gastroesophageal reflux (2, 4, 5). Recent studies have shown that patients with late diagnoses also benefit from attempting primary closure. This decision should be based on the characteristics of each case leaving aside evolution time as the sole deciding factor for conduct (3, 5). Primary correction has been shown to have the best results with shorter stays in the Intensive Care Unit and in the hospital and with lower mortality and reintervention rates (5). The main factors that impact on mortality are evolution time until treatment, comorbidities, general health status, perforation site and type of treatment used. Patients who are diagnosed during the first 24 hours have the best results (3, 4, 7).
There is no information about long-term survival rates, but some studies show good results with surgically treated patients achieving three year survival rates of up to 90% (3).
CONCLUSION
The challenge with Boerhaave syndrome is to establish diagnosis early enough for adequate treatment. One of our cases was detected late as indicated by contamination and the outcome was fatal. Surgery is key for most patients. The literature shows that it is a first-line treatment that repairs the defect, drains collections and creates a gastrointestinal bypass to achieve a rapid return to food consumption. In cases that are diagnosed late, but have no systemic compromise, endoscopic treatment can be attempted.
REFERENCES
1. De Schipper JP, Pull ter Gunne AF, Oostvogel HJM, van Laarhoven CJHM. Spontaneous rupture of the oesophagus: Boerhaave's syndrome in 2008. Literature review and treatment algorithm. Dig Surg. 2009;26(1):1-6. [ Links ]
2. Jeganathan R, Jones M, Graham AN. Re: Khan AZ, Strauss D, Mason RC. Boerhaave's syndrome: diagnosis and surgical management. Surgeon 2007; 5:39-44. Surg J R Coll Surg Edinb Irel. 2009;7(1):61; author reply 61. [ Links ]
3. Shaker H, Elsayed H, Whittle I, Hussein S, Shackcloth M. The influence of the «golden 24-h rule» on the prognosis of oesophageal perforation in the modern era. Eur J Cardio-Thorac Surg Off J Eur Assoc Cardio-Thorac Surg. 2010;38(2):216-22. [ Links ]
4. Lázár G Jr, Paszt A, Simonka Z, Bársony A, Abrahám S, Horváth G. A successful strategy for surgical treatment of Boerhaave's syndrome. Surg Endosc. 2011;25(11):3613-9. [ Links ]
5. Sulpice L, Dileon S, Rayar M, Badic B, Boudjema K, Bail JP, et al. Conservative surgical management of Boerhaave's syndrome: experience of two tertiary referral centers. Int J Surg Lond Engl. 2013;11(1):64-7. [ Links ]
6. Gomez-Esquivel R, Raju GS. Endoscopic closure of acute esophageal perforations. Curr Gastroenterol Rep. 2013;15(5):321. [ Links ]
7. Gupta NM, Kaman L. Personal management of 57 consecutive patients with esophageal perforation. Am J Surg. 2004;187(1):58-63. [ Links ]











 text in
text in