Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Revista colombiana de Gastroenterología
Print version ISSN 0120-9957
Rev Col Gastroenterol vol.31 no.1 Bogotá Jan./Mar. 2016
Impact on the Quality of Life of the Association between Sleep Disorders and Irritable Bowel Syndrome
Edward A. Cáceres Méndez MD. MSc. (1), Andrés J. Gómez MD. (2), Alberto Rodríguez Varón MD. (3), Jaime Alvarado Bestene MD. (3), Patricia Hidalgo MD. (4), Mauricio Medina (5)
(1) Third-year internal medicine resident at the Pontificia Universidad Javeriana in Bogotá, Colombia.
(2) Specialist in Internal Medicine at the Pontificia Universidad Javeriana in Bogotá, Colombia.
(3) Professor of Internal Medicine and Gastroenterology at the Pontificia Universidad Javeriana and the Hospital Universitario San Ignacio in Bogotá, Colombia.
(4) Associate Professor of Internal Medicine and Pneumology at the Pontificia Universidad Javeriana and the Hospital Universitario San Ignacio in Bogotá, Colombia.
(5) Medical student in the Semillero AOS program at the Pontificia Universidad Javeriana in Bogotá, Colombia.
Received: 27-08-15 Accepted: 26-01-16
Abstract
Objectives: The objectives of this study were to determine if sleep disorders in patients with irritable bowel syndrome (IBS) were associated with impaired quality of life as measured by the SF36 questionnaire.
Methods: This is cross-sectional study in which individuals with IBS according to the Rome III criteria were evaluated for sleep disorders with the Epworth Sleepiness Scale questionnaire and the Pittsburgh Sleep Quality Index (PSQI) questionnaire. They were also evaluated for restless legs syndrome (RLS) and, simultaneously, the Short Form (36) Health Survey was used to evaluate participants quality of life.
Results: Eighty patients with IBS, mostly women, were included in this study. 81% had some type of specific sleep disorder as measured by at least one of the questionnaires. Patients were groups into those who had sleep disorders, and those who did not. The group which had sleep disorders had statistically significantly more alterations in quality of life (OR 4.8125, 95% CI: 1.17 to 19.02, p <0.0076).
Conclusions: This study found that up to 81% of IBS patients have sleep disorders and that sleep disturbances in patients with IBS are associated with decreased quality of life according to the SF36 scale.
Keywords
Irritable bowel syndrome, sleep disorders, quality of life, SF36.
INTRODUCTION
Irritable bowel syndrome (IBS) is a common functional gastrointestinal disorder which generates high costs for health care systems. In the United States, these costs totaled $20 billion as the result of increased use of health care services. (1)
The main symptoms of IBS are chronic or recurrent abdominal pain and alterations in bowel habits. Currently, IBS is diagnosed on the basis of the 2006 Rome III criteria. (2) IBS is often associated with syndromes and symptoms that compromise other systems including headaches (34% to 50% of patients), fibromyalgia (32.5%), back pain (30%), chronic fatigue (51%), dyspareunia (52.3%) and changes in urinary frequency (50%). (3-5) It is believed that these associated disorders affect the quality of life of individuals and impose major limitations on performance of daily activities. (3, 6)
In recent years, the association between IBS and other disorders such as sleep disorders has been given more importance, and research has sought to establish whether these associations can condition further deterioration of the quality of life and eventually cause refractory or poor responses to treatment of IBS. (5, 7, 8). Taking into account the prevalence of IBS and current efforts to study of quality of life of patients with IBS and possible associations between IBS and sleep disorders, we decided to conduct this study to determine the frequency of sleep disturbances in patients with IBS and the impact on quality of life when this association is present.
MATERIALS AND METHODS
In order to determine the frequency of sleep disturbances in a group of patients with IBS and to determine whether the association between the two disorders causes greater alterations to patient quality of life, an observational descriptive cross-sectional study was designed. Patients older than 18 and younger than 65 years with IBS, as defined by the Rome III criteria, were included. They were scored according to the Epworth sleepiness scale validated for Colombia, the Pittsburgh sleep quality index, and criteria for restless legs. If the Epworth scale score is greater than ten, daytime sleepiness is established, scores over five on Pittsburgh index and scores of two to four for restless leg criteria indicate poor quality sleep. All patients filled out the Short Form (36) Health Survey for determination of quality of life.
We excluded patients with Alzheimers disease, frontal-temporal dementia and those who consumed sleep inducing drugs, benzodiazepines and antidepressants.
The study defined a sleep disorder as an abnormal result on one or more of the scales used.
RESULTS
A total of 80 patients with IBS were included. Most were women. Average patient age was 35 years old.
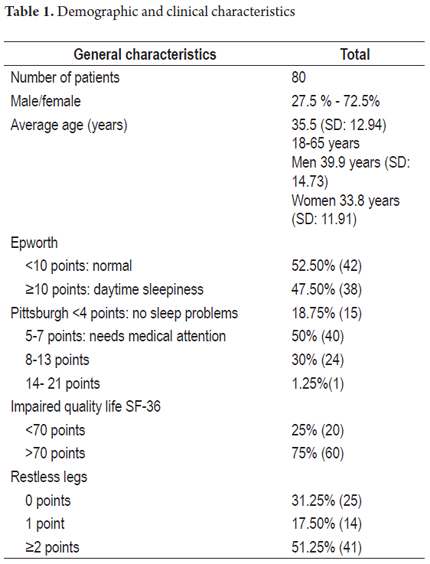
According to the criteria and scoring systems used, 38 patients (47.5%) suffered from daytime sleepiness defined as more than 10 points on the Epworth scale. Sixty-five patients (81%) showed some degree of alteration sleep quality measured with the Pittsburgh questionnaire, 25 patients (31%) presented scores compatible with moderate and severe impairment, and 41 patients (51%) had restless leg syndrome.
Of the total sample, 60 patients (75%) had impaired quality of life. Demographic and clinical characteristics of the sample are shown in Table 1.
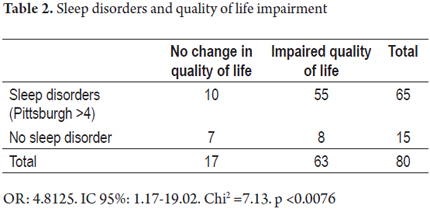
When outcomes were compared, it was found that the proportion of patients with sleep disorders as defined by an alteration in one or more of the scales used that also had some degree of impairment of quality of life according to the results of the SF-36 scale was statistically significant (OR: 4.8125, 95% CI: 1.17 to 19.02, p <0.0076) (Table 2).
DISCUSSION
Irritable bowel syndrome is a very common disease in the general population: its prevalence is between 10% and 20%, (9, 10) and it is one of the main reasons for consultation at all levels of care. Morbidity depends on the severity of gastrointestinal symptoms as well as on important social and cultural implications that lead patients to limit their daily activities and modify their daily performance. This is a phenomenon that can be accentuated with other diseases which may accompany IBS such as fibromyalgia and sleep disorders. (5, 7, 11)
Although an association has been described between IBS and sleep disorders that have been detected with polysomnography, (12) there had been no relevant information about this phenomenon in Colombia to establish whether manifested clinically sleep disturbances (prolonged sleep latency, frequent nocturnal awakenings and daytime sleepiness) produce additional deterioration in the quality of life of patients with IBS. (11).
Among the tools for assessment of sleep disorders are the Epworth scale sleepiness, which evaluates the propensity to fall asleep in 8 sedentary situations, and the Berlin Questionnaire, which assesses snoring, cessation of breathing and daytime sleepiness. Two other resources are the Pittsburgh Quality of Sleep Index and measurements of restless leg syndrome. Although full polysomnography is better at detecting the characteristics of sleep disorders, we decided to use clinical scales that were readily reproducible in any clinical setting.
IBS patients usually report changes in the quality of their lives comparable to those that occur in other chronic diseases such as diabetes, hypertension and chronic kidney disease. (1) Among the scales that assess quality of life are the SF-36 questionnaire, IBS-QOL, IBS-HRQOL, and the BEST scale. The last three are aimed at patients with IBS and can allow quick estimations of the quality of life of these patients. (1, 8) All of these scales have advantages and disadvantages, but, given our previous experience with the SF-36 plus its accessibility and validation in Spanish, and considering that it has no major differences with the other scales, we decided to use this scale.
This study identified a high prevalence of sleep disorders in the IBS patient population (81%). This could be explained by our use of various scales that assess different outcomes and that have good sensitivity for detection of sleep abnormalities, albeit with limited specificity. Even though these instruments have relatively low specificity, their advantage lies in simplicity of application and interpretation in any clinical setting.
According to the SF-36, quality of life was impaired in 75% of these patients with IBS. This is recognized as a high frequency that is plausible within the perceived quality of life of this group of patients who seek medical care because of moderate to severe clinical pictures.
From the results obtained in this study, it can be concluded that the association between IBS and sleep disorders is close to 81%. There is a high frequency (75%) of perceptions of impaired quality of life (SF-36) in this group of patients with IBS. It was also found that the association between IBS and sleep disorders is associated with additional impairment in patients quality of life.
These results should alert the medical community to the importance of exploring sleep disturbances in patients with IBS and the importance of following-up on these patients so that detection and management of sleep disorders can produce favorable results for patient quality of life.
REFERENCES
1. Agarwal N, Spiegel BM. The effect of irritable bowel syndrome on health-related quality of life and health care expenditures. Gastroenterol Clin North Am. 2011 Mar;40(1):11-19. [ Links ]
2. Videlock EJ, Chang L. Irritable bowel syndrome: Current approach to symptoms, evaluation, and treatment. Gastroenterol Clin North Am. 2007 Sep;36(3):665-85. [ Links ]
3. Luscombe F. Health-related quality of life and associated psychosocial factors in irritable bowel syndrome: A review. Qual Life Res. 2000;9:161-176. [ Links ]
4. Poitras P, Gougeon A, et al. Extra digestive manifestations of irritable bowel syndrome: Intolerance to drugs. Dig Dis Sci. 2008 Aug;53(8):2168-76. [ Links ]
5. Riedl A, Schmidtmann M, et al. Somatic comorbidities of irritable bowel syndrome: A systematic analysis. J Psychosom Res. 2008 Jun;64(6):573-82. Epub 2008 Apr 28. [ Links ]
6. Amouretti M, Le Pen C, et al. Impact of irritable bowel syndrome (IBS) on health-related quality of life (HRQOL). Gastroenterol Clin Biol. 2006;30:241-246. [ Links ]
7. Orr WC. Sleep and gastrointestinal disease: A new horizon in sleep medicine. Sleep Med. 2009 Jun;10(6):595-6. [ Links ]
8. Galdón Castillo A, Galera Mendoza L, et al. Disorders affecting the digestive system during sleep. Rev Neurol. 2004 Apr 16-30;38(8):757-65. [ Links ]
9. Spiller R, Aziz Q, et al. Guidelines on the irritable bowel syndrome: Mechanisms and practical management. Gut. 2007;56:1770–1798. [ Links ]
10. Quigley EM, Bytzer P, et al. Irritable bowel syndrome: The burden and unmet needs in Europe. Dig Liver Dis. 2006 Oct;38(10):717-23. [ Links ]
11. Kanaly T, Shaheen NJ, et al. Gastrointestinal physiology and digestive disorders in sleep. Curr Opin Pulm Med. 15:571–577. [ Links ]
12. Tibbits GM. Sleep Disorders: Causes, Effects, and Solutions. Prim Care. 2008 Dec;35(4):817-37. [ Links ]











 text in
text in