Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Revista colombiana de Gastroenterología
Print version ISSN 0120-9957
Rev Col Gastroenterol vol.32 no.1 Bogotá Jan./Mar. 2017
https://doi.org/https://doi.org/10.22516/25007440.127
Virtual Chromoendoscopy with I-Scan and its Application for Detection and Characterization of Colon Polyps
Henry Royero G. MD.(1)
(1) Internist and Gastroenterologist at the Emiro Quintero Cañizares Hospital in Ocaña, Colombia and international member of the ACP, AGA and ASGE. Mail: royerogastro@hotmail.com
Received:Â Â Â 05-05-16Â Accepted:Â Â Â 16-12-16
Abstract
The limitations of white light colonoscopy result in missing 6% of advanced neoplasias in 6% and up to 25% of adenomas. This has motivated the development of techniques such as virtual chromoendoscopy including the i-Scan system to detect larger numbers of polyps as a strategy for preventing colon cancer. This review summarizes the current application of this technique for detection and characterization of adenomas. The new system is a possible alternative in our environment to the better known NBI and FICE which are already being used here.
Key words
i-Scan, colonoscopy, polyp.
INTRODUCTION
Performance of polypectomy to remove adenomas detected during colonoscopy has reduced the incidence of colorectal cancer, (1-3) but it has been found that up to 6% of neoplasias and 25% of polyps cannot be seen during colonoscopy. (4, 5) This has led to several diagnostic modalities including chromoendoscopy with vital stains which can detect greater numbers of polyps and can be used to characterize them with the Kudo classification. (6-8) Nevertheless, routine use of this technique is not recommended because of its expense and because it can prolong the exploration time. These disadvantages make new techniques of virtual chromoendoscopy more attractive. (9) They have the advantages of being reversible, fast, clean and without any adverse effects due to dyes. (10) There are currently five virtual chromoendoscopy programs: Narrow Band (Olympus), the composite band imaging system (CBI) (Ahuoa), Fujifilm Intelligent Color Enhancement (FICE), the iScan system (Illumina), and the SPIES (Storz) system which was just recently introduced. (11, 12)
This is the first review of the iScan system in Colombia. Our objectives are to learn about this technology and to provide an additional point of view about high definition colonoscopy and virtual chromoendoscopy. When we searched Pubmed until January 2016 using the keywords iScan and endoscopy, we found 68 articles. We did not include those designed for applications other than the detection and characterization of colon neoplasms. We also reviewed the references of the selected papers and have included the most relevant in our bibliography.
What Is the IScan System?
The high-definition iScan, developed by Pentax (HOYA, Japan), is based on processing of the image taken by the CCD (charge coupled device) of the endoscope to increase the contrast of the vascular structures and the patterns of the mucosa of the digestive tract. (13, 14) It can produce optical resolutions up to 1,300,000 pixels. (15-18)
The iScan consists has three modes based on several algorithms: surface enhancement (SE), contrast enhancement (CE) and tone enhancement (TE). The first two have three levels: low, medium and high. Three objectives can be obtained with TE: the esophagus, the stomach and the colon. The three modes (SE, CE and TE) are arranged in series so that two or more can be applied consecutively in real time, without delays and at the touch of a button. (11, 19-21)
How is iScan used?
Various authors recommend iScan modes for the scenarios listed below. (15, 21, 22)
- iScan 1 (SE) should be used for detection of lesions. It refines the image of subtle surface abnormalities without alterating the brilliance of the endoscopic image.
- iScan 2 (TE plus SE) should be used for characterization of lesions. It combines surface and tone enhancement and enhances minute changes of the mucosa and vascular structures.
- iScan 3 (TE plus CE) should be used for demarcating lesions. It digitally adds blue color and darkens the edges of the endoscopic image.
Use of iScan for Colon Polyp Detection
The first prospective randomized study that compared detection of polyps with the iScan methodology standard white-light endoscopy has shown that iScan found significantly more colorectal neoplasias than did traditional endoscopy (38% versus 13%, p <0.001). (23) Another prospective randomized study compared the detection of adenomas of iScan with tone enhancement against detection with high definition white light colonoscopy. (24) iScan with tone enhancement found more adenomas (20 versus 6, p = 0.006) and identified a greater number of polyps omitted per subject (0.5 versus 0.15, p = 0.006). It was concluded that iScan with tone omitted fewer adenomas than did white light. Bowman found significantly similar findings with a larger number of patients. (25)
Another prospective study of 389 asymptomatic patients sought to determine percentages of adenomas detected. (26), Based on multivariate analysis, it concluded that iScan failed to document a significant performance in the detection of omitted adenomas which is contrary to the studies already mentioned. Nevertheless, it reported that The SE/TE-CE modes of iScan tended to outperform high-definition white light endoscopy in the detection of adenomas. This study's limitation is that it was performed in a single center with only a few endoscopists.
iScan Characterization of Polyps
A group from Mainz, Germany was the first to study detection and characterization of tiny polyps smaller than 5 mm. They used comparisons with histology to demonstrate that adenomas can be predicted with the iScan technique with a sensitivity of 9/11 (82%) and a specificity of 52/54 (96%). (27)
Another prospective study predicted histological outcome with a high degree of certainty (96.85%) through Kudo classification. (23) Successful studies in which this was the primary or secondary objective have demonstrated the high level of iScan's accuracy for classification adenomatous and non-adenomatous polyps. (16, 28, 29, 30)
A meta-analysis that included NBI, iScan , FICE, confocal endomicroscopy and autofluorescence imaging found that iScan had a sensitivity of 89.3% (83.3-93.3) and a specificity of 88.2% (80.3-93.2) for predicting polyps with a negative real-time predictive value of 86.5% (78-92.1). (31) These data were similar to those of other modalities, so it was concluded that these methods, including iScan, could be used routinely.
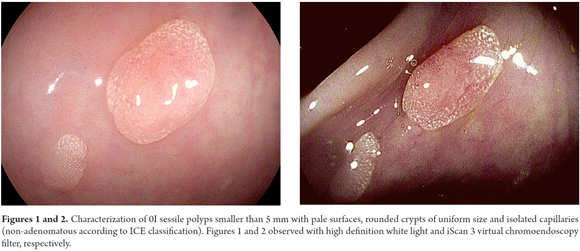
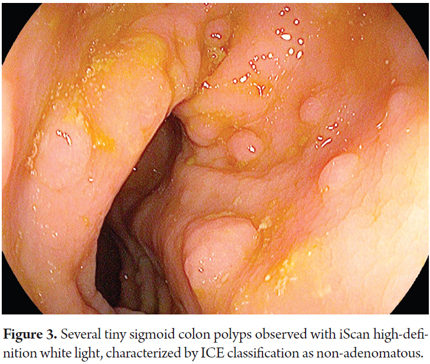
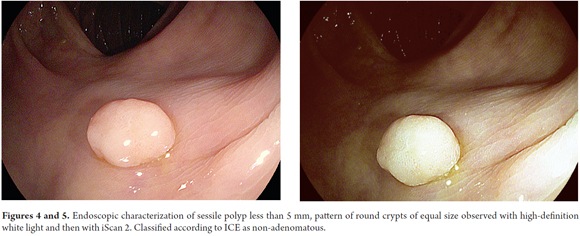
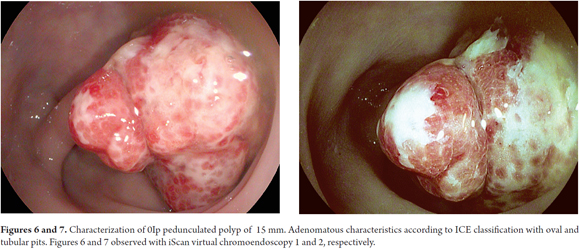
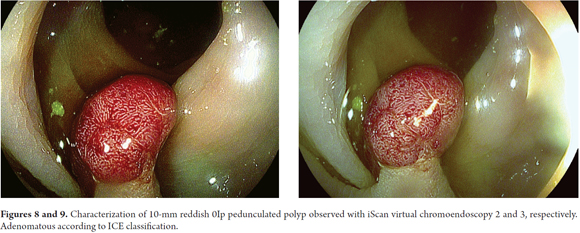
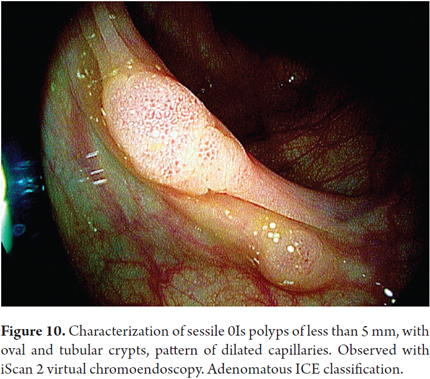
A comparison of iScan with NBI, another virtual chromoendoscopy technique, showed no obvious differences between the two for real-time prediction of polyps of less than 5 mm (sensitivity of 88.8% versus 94.6%; Specificity of 86.8% versus 86.4%; certainty of 87.8% versus 90.7%, respectively). (29) On the other hand, Bouwens has proposed a simple classification (ICE classification) for characterization of polyps that provides certainty 84% (Table 1 and Figures 1-2, 3, 4-5, 6-7, 8-9 and 10). (32) In addition, Lee has proposed a unified classification for NBI and iScan which combines the vascular pattern with the description of the mucosal surface of a polyp. Both classifications constitute practical tools for real-time optical diagnosis and characterization of adenomatous polyps. (29)
Learning Curve for Characterization of Polyps
According to the findings of a prospective study, after brief instruction eleven endoscopists with various levels of experience were able to predict the histological results with an accuracy of 84%. (30) Similarly, Neuman found that an accuracy of 94.3% could be obtained and that the learning curve can be quickly assimilated. (33) Routine use of iScan would allow less skilled examiners to achieve results comparable to those achieved by experienced endoscopists.
Position of the ASGE regarding the Characterization of Colonic Polyps and Virtual Chromoendoscopy
Preservation and Incorporation of Valuable endoscopic Innovations (PIVI) is an American Society of Gastrointestinal Endoscopy (ASGE) program that, in this particular case, addresses real-time assessment of diminutive polyps (less than 5 mm). It recommends two different strategies depending on the location of the polyps. For diminutive polyps that are not located in the rectum or sigmoid colon, and that can be characterized by virtual chromoendoscopy with high reliability, the ASGE recommends that they be predicted, resected and discarded. For diminutive polyps that are located in the rectum or sigmoid colon, and that can be characterized by virtual chromoendoscopy with high reliability, the ASGE recommends that they be predicted, but not resected. To use these strategies, it is necessary to emphasize the reliability of optical diagnosis and reduction of interobserver variation. (35, 36) A recent review and meta-analysis by the ASGE, similar to the HISCOPE study, suggests that the thresholds proposed by PIVI can potentially be reached by the iScan system, but large randomized studies are necessary to test it. (37, 38) In addition, training and accreditation are needed that guarantee the quality of optical diagnosis. (39)
However, it is important to note that the iScan colonoscopy system is a tool that is complementary to good technique and quality indicators in colonoscopy: cecal intubation, adequate withdrawal time, percentage of adenomas detected and optimal colon cleansing. (40 , 41)
Position of the ESGE regarding Characterization of Colonic Polyps and Chromoendoscopy
The recent European Society of Gastrointestinal Endoscopy (ESGE) guidelines for the use of new technologies for detection and characterization of colon neoplasias has several recommendations. (42)
- Routine use of high magnification endoscopy with white light to detect colorectal neoplasms in the average population
- Routine use of high definition systems and conventional or virtual pan-chromoendoscopy (NBI, iScan ) in patients known or suspected to have Lynch syndrome
- Conventional or virtual chromoendoscopy (NBI, FICE or iScan ) should be strictly controlled for real-time diagnosis of polyps less than or equal to 5 mm in order to replace the histopathological diagnosis. In addition, photo documentation should be done by properly trained experienced endoscopists.
Future Research Areas
A consensus of the current classification systems of gastrointestinal mucosal lesions found with high definition endoscopes is needed for easy use in clinical settings. In addition, the relative value of digital chromoendoscopy compared to the histology of polyps raised by ASGE's PIVI should be studied in order to develop training certification modules. (43, 44)
CONCLUSIONS
The high definition iScan system can be considered as an alternative to the known virtual chromoendoscopy systems for detection of colon neoplasias.
With iScan technology, the histological prediction of adenomatous or hyperplastic polyps in real time during colonoscopy is safe. The learning curve can be quickly acquired which could lead to routine use outside of referral centers.
Conflict of Interests
The author states that he has no conflicts of interest.
REFERENCES
1. Winawer SJ, Zauber AG, Ho MN, et al. Prevention of colorectal cancer by colonoscopy polypectomy. The National Polyp Study Workgroup. N Engl J Med. 1993;329:1977-81. [ Links ]
2. Winawer SJ, Zauber AG, OBrien MJ, et al. Randomized comparison of surveillance intervals after colonoscopic removal of newly diagnosed adenomatous polyps. N Engl J Med. 1993;328:901-6. [ Links ]
3. Bressler B, Paszat LF, Chen Z, et al. Rates of new or missed colorectal cancers after colonoscopy and their risk factors: a population-based analysis. Gastroenterology. 2007;132:96-112. [ Links ]
4. Van Rijn JC, Eitsma JB, Stoker J, et al. Polyp miss rate determined by tandem colonoscopy: a systematic review. Am J Gastroenterol. 2006;101:343-50. [ Links ]
5. Rex DK, Cutler CS, Lemmel GT, et al. Colonoscopic miss rates of adenomas determined by back to back colonoscopies. Gastroenterology. 2007;132:96-102. [ Links ]
6. Devuni D, Vaziri H, Anderson J. Chromocolonoscopy. Gastroenterol Clin N Am. 2013;42:521-45. [ Links ]
7. Kudo S, Hirota S, Nakajima T, et al. Colorectal tumours and Pit Pattern. J Clin Pathol. 1994;47:880-5. [ Links ]
8. Tischendorf J, Wasmuth HE, Koch A, et al. Value of magnifying chromoendoscopy and narrow band imaging (NBI) in classifying colorectal polyps a prospective controlled study. Endoscopy. 2007;39:1092-6. [ Links ]
9. Huang Q, Fukami N, Kashida H, et al. Interobserver and Intraobserver consistency in the endoscopic assessment of colon pit patterns. Gastrointest Endosc. 2001;60:520-6. [ Links ]
10. Lopez- Cerón L, Sanabria E, Pellise M. Colonic polyps is it useful to characterize them with advance endoscopy? World J Gastroenterol. 2014;26:8449-57. [ Links ]
11. Neuman H, Fujishro M, Wilcox M, et al. Present and future perspectives of virtual chromoendoscopy with i-scan and optical enhancement technology. Dig Endosc. 2014;26(Suppl 1):43-51. [ Links ]
12. Neuman H, Nagel A, Buda A. Advance endoscopic imaging to improve adenoma detection. World J Gastrointest Endosc. 2015;7:224-9. [ Links ]
13. Reyes-Dorantes A. Nuevas técnicas de imagen (i-Scan, NBI, FICE). Rev Gastroenterol Mex. 2011;76:(Suppl 1):134-6. [ Links ]
14. Yeung TM, Mortesen NJ. Advances in endoscopic visualization of colorectal polyps. Colorectal Dis. 2011;13:352-9. [ Links ]
15. Galloro G. High technology imaging in digestive endoscopy. World J Gastrointest Endosc. 2012;16;4(2):22-7. [ Links ]
16. Masci E, Mangiavillano B, Costa C, et al. Interobserver agreement among endoscopists on evaluation of polypoid colorectal lesions visualized with Pentax i-Scan Technique. Dig Liver Dis. 2013;45:207-10. [ Links ]
17. Banks M, Haidry R, Butt M, et al. High resolution colonoscopy in a bowel cancer screening program improves polyp detection. World J Gastroenterol. 2011;17:4308-13. [ Links ]
18. Kwon RS, Adler DG, Chand B, et al. High-resolution and High-magnification endoscopes. Gastrointetinal Endosc. 2009;69:399-407. [ Links ]
19. Ventakaraman S, Ragunath K. Advance endoscopic imaging: a review of commercially aviable technologies. Clin Gastroenterol Hepatol. 2014;12:368-76. [ Links ]
20. Hancock S, Bowman E, Prabakaran J, et al. Use of i-scan endoscopic image enhancement technology and therapeutic endoscopy: a case series and review of the literature. Diagn Ther Endosc. 2012;2012:193570. [ Links ]
21. Kodashima S, Fujishiro M. Novel image-enhanced endoscopy with i-scan technology. World J Gastroenterol. 2010;16:1043-9. [ Links ]
22. Cho JH. Advanced imaging technology other than narrow band imaging. Clin Endosc. 2015:48:503-10. [ Links ]
23. Hoffman A, Sar F, Goetz M, et al. High definition colonoscopy combined with i-scan is superior in the detection of colorectal neoplasias compared with standard videocolonoscopy: a prospective randomized controlled trial. Endoscopy. 2010;47:827-33. [ Links ]
24. Hoffman A, Loth L, Rey JW, et al. High definition plus colonoscopy combined with i-scan tone enhancement vs. high definition colonoscopy for colorectal neoplasia: A randomized trial. Dig Liver Dis. 2014;46:991-6. [ Links ]
25. Bowman E, Pfau P, Mitra A, et al. High definition colonoscopy combined with i-SCAN imaging technology is superior in the detection of adenomas and advanced lessions compared to high definition colonoscopy alone. Diagn Ther Endosc. 2015;2015:167406. [ Links ]
26. Hong SN, Choe WH, Lee JH, et al. Prospective, randomized, back-to-back trial evaluating the usefulness of i-SCAN in screening colonoscopy. Gastrointest Endosc. 2012;75(5):1011-21. [ Links ]
27. Hoffman A, Kagel C, Goetz M, et al. Recognition and characterization of small colonic neoplasia with-definition colonoscopy using i-scan as precise chromoendoscopy. Dig Liver Dis. 2009;42;45-50. [ Links ]
28. Pigo F, Bertani H, Barbera C, et al. I-Scan high-definition white light endoscopy and colorectal polyps: prediction of histology interobserver and intraobserver agreement. Int J Colorectal Dis. 2013;28:399-406. [ Links ]
29. Lee Ch, Lee SH, Hwagbo Y. Narrow-band imaging versus I-Scan for the real time histological prediction of diminutive colonic polyps: a prospective comparative study by using the simple unified endoscopic classification. Gastrointest Endosc. 2011;74:603-9. [ Links ]
30. Hong SN, Choe WC, Lee JH, et al. Prospective, randomized, back-to-back trial evaluating the usefulness of i-SCAN screening colonoscopy. Gastrointest Endosc. 2012;75:1011-21. [ Links ]
31. Wanders L, East J, Uitentius S, et al. Diagnostic performance of narrowed a spectrum endoscopy autofluorescense imaging, and confocal laser endomicroscopy for optical diagnosis of colonic polyps: a meta-analysis. Lancet. 2013;14:1337-47. [ Links ]
32. Bouwens M, Ridder R, Masclee A, et al. Optical diagnosis of colorectal polyps using high-definition i-scan: an educational experience. World J Gastroenterol. 2013;19:4334-43. [ Links ]
33. Neuman H, Vieth M, Fry L, et al. Learning curve of virtual chromo endoscopy for the prediction of hyperplastic and adenomatous colorectal lesions: a prospective 2-center study. Gastrointest Endosc. 2013;78:115-20. [ Links ]
34. Rex DK, Kahi C, O´Brien M, et al. The American Society for Gastrointestinal Endoscopy PIVI (Preservation and Incorporation of Valuable Endoscopic Innovations) on real-time endoscopic assessment of the histology of diminute colorectal polyps. Gastrointest Endosc. 2011;73:419-22. [ Links ]
35. Kaltenbach T, Rex D, Wilson A, et al. Implementation of optical diagnosis for colorectal polyps: standardization of studies is needed. Clin Gastroenterol Hepatol. 2015;13:6-10. [ Links ]
36. Hassan C, Repici A, Zullo A, et al. New paradigms for colonoscopic management of diminutive colorectal polyps: predict, resect, and discard or do not resect? Clin Endosc. 2013;48:130-7. [ Links ]
37. Abu Dayyeh BK, Thosani N, Konda V, et al. ASGE Technology Committee systematic review and meta-analysis assessing the ASGE PIVI thresholds for adopting real-time endoscopic assessment of the histology of diminutive colorectal polyps. Gastrointest Endosc. 2015;81:502-16. [ Links ]
38. Basford P, Longcroft-Wheaton G, Higgins B, et al. High-definition endoscopy with i-Scan for evaluation of small colon polyps: the HisCOPE study. Gastrointest Endosc. 2014;79:111-8. [ Links ]
39. Wilson BA. Optical diagnosis of small colorectal polyps during colonoscopy: When to resect and during colonoscopy: When to resect and discard? Best Pract Res Clin Gastroenterol. 2015;29:639-49. [ Links ]
40. Gomez V, Wallace M. Advances in diagnostic and therapeutic colonoscopy. Curr Opin Gastroenterol. 2014;30:63-8. [ Links ]
41. Kiesslich R. Novel colonoscopic imaging techniques. Gastroenterol Hepatol. 2013;9:241-4. [ Links ]
42. Kaminski M, Hassan C, Bisschops R, et al. Advance imaging for detection and differentiation of colorectal neoplasia: European Society of Gastrointestinal Endoscopy (ESGE) Guideline. Endoscopy. 2014:46;435-49. [ Links ]
43. Bath Y, Abu Dayyeh B, Chauhan S, et al. High-definition and high-magnification endoscopes. Gastrointest Endosc. 2014;80:919-27. [ Links ]
44. Jang JY. The past, present, and future of image- enhanced. Endoscopy Clin Endosc. 2015;48:466-75. [ Links ]











 text in
text in