Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Revista colombiana de Gastroenterología
Print version ISSN 0120-9957
Rev Col Gastroenterol vol.33 no.2 Bogotá Apr./June 2018
https://doi.org/10.22516/25007440.258
Case report
A case of an unusual association of autoimmune hepatitis and colon cancer: report and literature review
1Médico, cirujano general, gastroenterólogo clínico-quirúrgico, coordinador del programa de Gastroenterología Clínico-Quirúrgica, Universidad de Caldas. Manizales, Colombia
2Médica, cirujana general, gastroenteróloga clínico-quirúrgica, docente del programa de Gastroenterología Clínico-Quirúrgica, Universidad de Caldas. Manizales, Colombia
3Médico, internista, gastroenterólogo clínico de la Universidad Nacional, docente del programa de Gastroenterología Clínico-Quirúrgica, Universidad de Caldas. Manizales, Colombia
4Médico, cirujano general, gastroenterólogo clínico-quirúrgico, Universidad de Caldas. Manizales, Colombia
5Médico, cirujano general, coloproctólogo, Universidad de Caldas. Manizales, Colombia
6Médica, cirujana general, gastroenteróloga clínico-quirúrgica, Universidad de Caldas. Manizales, Colombia
7Médico, cirujano general, residente de Gastroenterología Clínico-Quirúrgica, Universidad de Caldas. Manizales, Colombia
Introduction:
Idiopathic autoimmune hepatitis (IAH) is a chronic disease that occurs predominately in women, has episodic activity and remission, and favors hepatic fibrosis. Forty percent of patients have family histories of autoimmune diseases. It is apparently mediated by antigen-antibody interaction, but its causes are unknown. IAH is frequently associated with hepatobiliary cancer, less frequently with lymphomas, skin cancer and colon cancer and very rarely with hereditary colon cancer syndrome. This case debuted IAH and rectal bleeding caused by familial adenomatous polyposis (FAP) and adenocarcinoma of the sigmoid colon.
Clinical case:
The patient was a 51-year-old woman who had had IAH for one year which had been managed with prednisolone and azathioprine. A total colonoscopy, performed because of anemia, found multiple polyps that measured 5 and 10 mm and one ulcerated 30 mm sessile polyp in the sigmoid colon. A multiple endoscopic polypectomy revealed a tubulovillous adenoma with high and low grade dysplasia in several polyps and a low grade adenocarcinoma in the sigmoid polyp. Tests and examinations for metastasis were negative. Following presurgical nutritional repletion, a subtotal colectomy was performed and an ileal pouch-anal anastomosis with protective ileostomy was created. The pathology of the surgical specimen showed low grade adenocarcinoma of the colon and tubular and tubulovillous adenomas with high and low grade dysplasia.
Discussion and conclusions:
Association of IAH with familial adenomatous polyposis (FAP) and colorectal cancer (CC) occurs infrequently although associations of IAH with hepatobiliary cancer associated with cirrhosis, lymphomas, skin cancer and other autoimmune disorders are well-known. The prognosis is bad and no clear correlation with immune modulators can be established.
Keywords: Autoimmune hepatitis; malignancies; extra-hepatic neoplasms; adenomatous polyposis; colorectal carcinoma
Introducción:
la hepatitis autoinmune idiopática (HAI) es una enfermedad crónica que predomina en mujeres, con episodios de actividad y remisión, favoreciendo la fibrosis hepática. El 40% de los pacientes presenta historia familiar de enfermedades autoinmunes. Al parecer, es mediada por la interacción antígeno-anticuerpo; sin embargo, su causa es desconocida. Se conoce la asociación frecuente de HAI con cáncer hepatobiliar; menos frecuente con linfomas, cáncer de piel y cáncer de colon; y casi inexistente con síndromes hereditarios de cáncer de colon. Este caso debutó con HAI y sangrado rectal causado por poliposis adenomatosa familiar (PAF) y adenocarcinoma de colon sigmoide.
Caso clínico:
mujer de 51 años con HAI de 1 año de evolución manejada con prednisolona y azatioprina. Se realizó una colonoscopia total por anemia en la que se encontraron múltiples pólipos entre 5 y 10 mm y 1 de 30 mm sésil, ulcerado, en colon sigmoide. Se realizó una polipectomía endoscópica múltiple que reportó un adenoma tubulovelloso con displasia de alto y bajo grado en varios pólipos y un adenocarcinoma de bajo grado en el pólipo del sigmoide. Los estudios de extensión fueron negativos para metástasis. Se realizó una repleción nutricional prequirúrgica, luego una colectomía subtotal y una procto-ileoanastomosis con ileostomía de protección. La patología de pieza quirúrgica mostró un adenocarcinoma de colon de bajo grado y adenomas tubulares y tubulovellosos con displasias de alto y bajo grado.
Discusión y conclusiones:
La asociación de HAI con PAF y cáncer colorrectal (CC) es infrecuente. Es conocida la correlación de HAI con cáncer hepatobiliar (asociado con cirrosis), linfomas, cáncer de piel y otros desórdenes autoinmunes. El pronóstico es malo y no puede establecerse una correlación clara con moduladores inmunes.
Palabras clave: Hepatitis autoinmune; malignidades; neoplasias extrahepáticas; poliposis adenomatosa; carcinoma colorrectal
Introduction
Idiopathic autoimmune hepatitis (AIH) is associated with several pathologies. It predisposes those who have it to development of liver cirrhosis which in turn is an established factor for hepatocellular cancer (HCC) whose annual incidence among those with cirrhosis is between 3% and 9%. It is especially induced by chronic viral hepatitis B and C. 1 At the time of diagnosis, up to one third of AIH patients have already developed cirrhosis. 2
It is well established that AIH can be associated with several autoimmune diseases, so the risk of malignancy associated with immunosuppressive treatment is a fundamental concern. 3 Because association of AIH with either familial adenomatous polyposis (FAP) or colorectal cancer (CC) is rare, we have described this clinical case and reviewed the scant literature available.
Clinical case
The patient is a 51-year-old woman who had suffered jaundice, pruritus, choluria and rectorrhagia intermittently for 18 months. She had no other relevant medical history and did not mention taking any hepatotoxic drugs. A clinical examination showed jaundice, a normal abdomen, and no musculoskeletal pain or weight loss. Blood tests showed carcinoembryonic antigen level of 1.57 ng/mL (0-10), no signs of hepatitis B or C negative, Gamma-glutamyltransferase (GGT) level at r60 IU/L, total bilirubin of 3.7 mg/dL, glutamic oxalacetic transaminase (GOT) at 116, glutamic pyruvic transaminase (TGP) at 119, albumin at 3.8 mg/dL, hemoglobin (Hb) at 9.6 mg/dL, hematocrit at 32%. She also tested positive for antinuclear antibodies (ANA) and smooth muscle antibodies (SMA) but negative for anti-mitochondrial antibodies (AMA). Abdominal ultrasonography showed no signs of liver lesions or cholelithiasis and a normal bile duct. A liver biopsy showed interface hepatitis of moderate activity, without lobular hepatitis or necrosis and without granulomas.
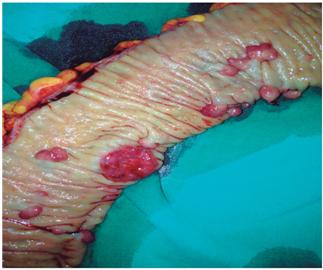
A diagnosis of AIH was made and immunomodulatory therapy with prednisolone and azathioprine was initiated. Due to the patient’s anemia endoscopy was ordered. It reported Los Angeles scale grade B esophagitis and antral erosive gastritis. A colonoscopy showed 25 to 30 polyps with diameters between 0.5 and 1.0 cm throughout the entire colon. Random biopsies of numerous polyps were performed. They showed two right colon polyps with tubulovillous adenoma and high grade dysplasia, two polyps of the transverse and descending colon with tubulovillous adenoma and low grade dysplasia, and an ulcerated 3 cm polypoid lesion in the sigmoid colon at 30 cm from the anal margin which tested positive for low-grade colon adenocarcinoma. A chest x-ray and a CAT scan of the abdomen were normal. Presurgical nutritional intervention was performed. Subsequently a laparotomy showed that the liver had no nodules, ascites or peritoneal seeding. A subtotal colectomy was performed together with ileal-anal anastomosis (IPAA) surgery and creation of a protective ileostomy (Figure 1).
The pathology report showed multiple sessile polypoid formations throughout the colon. They tested positive for tubulovillous adenomas with low and high grade dysplasia and measured from 0.8 x 0.5 cm to 2.0 x 1.5 cm. In the sigmoid colon, there was an ulcerated polypoid lesion with infiltration of the muscularis propria and lymphovascular invasion, but tumor-free serosa. It tested positive for low-grade, well-differentiated adenocarcinoma of the colon. We also observed a 1.3 x 0.3 cm polyp in the superior rectus and a tubular adenoma with high grade dysplasia which were not malignant. Three out of thirteen positive nodes had resection edges free from tumors and were staged T3N1bM0.
Discussion
The frequency of extrahepatic malignancy in cases of AIH is 5% with an estimated incidence of 1 case per 194 patients/year. The probability of extrahepatic tumors after 10 years is 3% with a risk that is 1.4 times higher than that in the general population. The pathogenic mechanisms that promote the development of extrahepatic neoplasms in AIH are unknown but are not associated with cirrhosis. 4
Extrahepatic malignancies that develop before or after diagnosis of AIH can originate in the bladder, blood, breast, cervix, lymphoid tissue, skin, thymus, soft tissues and stomach. 5
Werner et al. evaluated 473 patients in the national cancer registry of Sweden who had AIH between 1990 and 2003. They found 108 tumors, 39 of which were benign and 69 of which were malignant. Twenty-five were prevalent (existing before diagnosis of AIH) and 44 were incidental (developing after diagnosis). They analyzed the risk for hepatobiliary cancer, skin, non-Hodgkin’s lymphoma, colon cancer, and rectal cancer in this cohort. Four patients were found to have with CC with slightly elevated risk indicated by a standardized incidence ratio (SIR) of 4.23 with a 95% confidence interval (CI) of 1.1 to 10.8. None had histories of inflammatory bowel disease. This contrasts with the high risks for hepatobiliary cancer, lymphoma and skin cancer (SIR: 8.4, 95% CI: 2.66-19.2, SIR: 5.91, 95% CI: 1.9-13.7 and SIR: 6.1, 95% CI: 2.47-12.7, respectively).
AIH is a rare and progressive disease that can induce cirrhosis and HCC. However, their relationships are less obvious and are underestimated compared to the well-known relation of liver cirrhosis and HCC with hepatitis B and C. The risk of cancer after diagnosis of AIH is high, but only 4 of 473 patients with AIH from the Swedish national cancer registry had CC. 6
Tumors associated with chronic immunosuppression after organ transplantation (e.g. skin cancer) are correlated with drug-induced effects on immune mechanisms involved in tumor and infection control. A Swedish study of 634 patients with AIH showed the known association of HCC and recognized non-melanoma skin cancer as the most frequent extrahepatic tumor presentations (23 cases), followed by non-Hodgkin’s lymphoma. 7 In AIH, the duration and degree of immunosuppressant therapy cannot be ruled out as risk factors for tumors. 8
Suppression of lymphocyte functioning and mechanisms of tumor control mediated by cytokines, alteration of apoptosis and tumor growth through cellular signaling pathways, 9 direct damage of DNA and its repair mechanisms, low levels of expression of tumor suppressor genes, poor regulation of the cell cycle, 10 severity of autoimmune disease and the type and dosage of drugs administered are all objects of speculation about effects of drugs that might lead to development of cancer in patients with AIH. 6
It is interesting to compare the risks of PAF and CC with other autoimmune biliary and hepatic diseases. In a Swedish cohort of 604 patients who had primary sclerosing cholangitis between 1970 and 1998, HCC was observed in 12 patients with inflammatory bowel disease with an SIR of 10.3 (95% CI: 5.3-18.1). (11
A Scottish study of 85 patients with primary biliary cirrhosis found 10 patients who presented extrahepatic malignancies. Only one presented CC. 12. A metaanalysis by Liang et al. that covered 16,300 patients with primary sclerosing cholangitis found that the general risk of cancer and the risk of HCC were higher than those of the general population but they did not find this to be true for other types of cancer. Fifty cases of colon cancer with a SIR of 1.13 (95% CI: -0.26 to -2.52). Twenty-three cases of rectal cancer were recorded with a SIR of 1.0 (95% CI: 0.56 to 1.43). 13
After comparing other autoimmune liver diseases, it can be concluded that there are similar increases in the risks of liver and extrahepatic cancer. This suggests a need to create strict surveillance programs. Despite the fact that the association of AIH and CC is not statistically significant, studies are needed to evaluate this relationship.
The evidence available from patients with AIH and extrahepatic tumors is based mostly on tumors outside of the gastrointestinal tract. Among the gastrointestinal tumors, CC is the most frequent. Treatment must be appropriate to the particular pathology and may include resection, radiation therapy and/or chemotherapy. 8 Immunosuppression should be adjusted and, although these responses have not been documented with AIH, the dose of medication should be reduced as much as possible or the immunosuppressant should be replaced by an alternative drug. The appropriate action is to suspend azathioprine and other non-standard immunosuppressants (calcineurin inhibitors and mycophenolate mofetil) and to control hepatic inflammatory activity with an increase in the dose of corticosteroids. 6 Even in post-transplant patients there is an increase in the appearance of CC for those who have immunomodulatory therapy with thiopurine plus steroids. These patients also experience increased incidence of lymphoma and sarcoma. Patients treated with cyclosporine do not have increased risks. 14
Despite surgical resection of colon adenocarcinoma, as in the case presented here, patients have a high risk of additional neoplasms. For this reason, endoscopic follow-up plus imaging and monitoring of tumor markers are very important. Improvement in diagnostic methods, increasing number of reports of AIH and extrahepatic malignancies, new molecular pharmacological treatments, cellular intervention that can damage immune response against cancer, and increased survival in cases of AIH, cirrhosis and extrahepatic cancer all justify a change of mentality and awareness of this type of pathologies.
Conclusion
Patients with AIH are known to be at increased risk of HCC and extrahepatic neoplasms. The pathogenic mechanism is not completely known. There is little literature available that links AIH to CC, and none that relates AIH to FAP. There is a need to create more stringent evaluation and surveillance programs to enable prediction of biological behavior, to manage these tumors, and to improve patient survival in these cases.
Referencias
1. Velázquez RF, Rodríguez M, Navascués CA, et al. Prospective analysis of risk factors for hepatocellular carcinoma in patients with liver cirrhosis. Hepatology. 2003;37(3):520-7. doi: 10.1053/jhep.2003.50093. [ Links ]
2. European Association for the Study of the Liver. EASL Clinical Practice Guidelines: Autoimmune hepatitis. J Hepatology. 2015;63(4):971-1004. doi: 10.1016/j.jhep.2015.06.030. [ Links ]
3. Smedby KE, Baecklund E, Askling J. Malignant lymphomas in autoimmunity and inflammation: a review of risks, risk factors, and lymphoma characteristics. Cancer Epidemiol Biomarkers Prev. 2006;15(11):2069-77. doi: 10.1158/1055-9965.EPI-06-0300. [ Links ]
4. Wang KK, Czaja AJ, Beaver SJ, et al. Extrahepatic malignancy following long-term immunosuppressive therapy of severe hepatitis B surface antigen-negative chronic active hepatitis. Hepatology. 1989;10(1):39-43. doi: 10.1002/hep.1840100110. [ Links ]
5. Czaja AJ. Hepatocellular carcinoma and other malignancies in autoimmune hepatitis. Dig Dis Sci. 2013;58(6):1459-76. doi: 10.1007/s10620-012-2525-5. [ Links ]
6. Werner M, Almer S, Prytz H, et al. Hepatic and extrahepatic malignancies in autoimmune hepatitis. A long-term follow-up in 473 Swedish patients. J Hepatol. 2009;50(2):388-9. doi: 10.1016/j.jhep.2008.08.022. [ Links ]
7. Komaki Y, Komaki F, Micic D, et al. Risk of colorectal cancer in chronic liver diseases: a systematic review and meta-analysis. Gastrointest Endosc. 2017;86(1):93-104.e5. doi: 10.1016/j.gie.2016.12.009. [ Links ]
8. Penn I. Post-transplant malignancy: the role of immunosuppression. Drug Saf. 2000;23(2):101-13. doi: 10.2165/00002018-200023020-00002. [ Links ]
9. Han W, Soltani K, Ming M, et al. Deregulation of XPC and CypA by cyclosporin A: an immunosuppression-independent mechanism of skin carcinogenesis. Cancer Prev Res (Phila). 2012;5(9):1155-62. doi: 10.1158/1940-6207.CAPR-12-0185-T. [ Links ]
10. Strickland FM, Kripke ML. Immune response associated with nonmelanoma skin cancer. Clin Plast Surg. 1997;24(4):637-47. [ Links ]
11. Bergquist A, Ekbom A, Olsson R, et al. Hepatic and extrahepatic malignancies in primary sclerosing cholangitis. J Hepatol. 2002;36(3):321-7. doi: 10.1016/S0168-8278(01)00288-4 [ Links ]
12. Mills PR, Boyle P, Quigley EM, et al. Primary biliary cirrhosis: an increased incidence of extrahepatic malignancies? J Clin Pathol. 1982;35(5):541-3. doi: 10.1136/jcp.35.5.541. [ Links ]
13. Liang Y, Yang Z, Zhong R. Primary biliary cirrhosis and cancer risk: a systematic review and meta-analysis. Hepatology. 2012;56(4):1409-17. doi: 10.1002/hep.25788. [ Links ]
14. Danielsson Borssén Å, Almer S, Prytz H, et al. Hepatocellular and extrahepatic cancer in patients with autoimmune hepatitis - a long-term follow-up study in 634 Swedish patients. Scand J Gastroenterol. 2015;50(2):217-23. doi: 10.3109/00365521.2014.983154. [ Links ]
Received: August 14, 2017; Accepted: April 13, 2018











 text in
text in