Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Revista colombiana de Gastroenterología
Print version ISSN 0120-9957
Rev Col Gastroenterol vol.33 no.3 Bogotá July/Sept. 2018
https://doi.org/10.22516/25007440.197
Original articles
Peroral endoscopic myotomy (POEM) for treatment of achalasia: our first experiences
1Especialista en cirugía gastrointestinal y endoscopia digestiva. Organización Clínica General del Norte, Barranquilla. Clínica Shaio, Bogotá D. C., Colombia.
2Especialista en cirugía general. Hospital Militar Central, Bogotá D. C., Colombia.
3Especialista en medicina interna, gastroenterología y epidemiología; profesor de la Universidad Nacional de Colombia, servicio de motilidad gastrointestinal; director científico del Instituto GutMédica. Bogotá D.C., Colombia.
4Especialista en cirugía general y endoscopia digestiva. Organización Clínica General del Norte. Barranquilla, Colombia.
5Cirujano general, Clínica MedSalud. Fusagasugá, Colombia.
6Especialista en medicina interna y gastroenterología; profesor de posgrado de la Universidad Nacional de Colombia; servicio de gastroenterología y endosonografía del Instituto GutMédica. Bogotá D. C., Colombia.
7Médico internista y gastroenterólogo. Profesor asociado de la Universidad Nacional de Colombia. Gastroenterólogo del Hospital Nacional Universitario. Bogotá D. C., Colombia.
8Cirujano general y gastroenterólogo. Clínica San José. Cúcuta, Colombia.
Introduction:
Peroral endoscopic myotomies (POEMs) were initially designed to manage achalasia, a chronic and progressive esophageal motility disorder with lower esophageal sphincter hypertension (LES). Until recently, standard treatment had been Heller’s surgery, but this new technique offers very promising pressure.
Materials and methods:
This is a retrospective review of the clinical histories of patients with achalasia who underwent POEM performed by one endoscopic surgeon at a Colombian institution.
Results:
Four patients with achalasia were found. All had Eckardt scores of ten or more and lower esophageal sphincter (LES) pressure of 30mm Hg or more. Surgical times ranged between 81 and 120 minutes. Follow-up examinations found that LES pressure had decreased by more than 50% in practically all patients. Eckardt scores were close to normal. This demonstrates success of POEM therapy after two months of evaluation. Complications were resolved intraoperatively without mortality.
Conclusions:
Management of achalasia by POEM has proven to be a safe and effective technique. Our first findings agree with the results described in the literature. This is the first step in the implementation of this novel approach for management of achalasia in our Colombian population.
Keywords: Achalasia; esophageal motility disorders; oral endoscopic myotomy; Heller myotomy
Introducción:
la miotomía endoscópica por vía oral (POEM) se diseñó inicialmente para el manejo de la acalasia, que es un trastorno crónico y progresivo de la motilidad esofágica con hipertensión del esfínter esofágico inferior (EEI), para la cual el manejo estándar, hasta ahora, ha sido la cirugía de Heller; sin embargo, esta nueva técnica ofrece resultados muy comparables y prometedores.
Materiales y métodos:
se realizó una revisión retrospectiva de las historias clínicas de los pacientes con acalasia operados por POEM en una institución de Colombia por un solo cirujano endoscopista.
Resultados:
se encontraron 4 pacientes con acalasia, todas con Eckardt ≥10 y presión EEI ≥30 mm Hg; el tiempo quirúrgico osciló entre 81-120 minutos; en el seguimiento, la reducción en la presión del EEI fue mayor al 50% prácticamente en todos los pacientes, encontrando valores cercanos a la normalidad y con resultados de Eckardt que demuestran éxito en la terapia POEM a los 2 meses de evaluación. Las complicaciones fueron resueltas en el intraoperatorio, con mortalidad de 0%.
Conclusiones:
El manejo de la acalasia mediante POEM ha demostrado ser una técnica eficaz y segura. Nuestros primeros hallazgos concuerdan con los resultados descritos en la literatura. Este es el primer paso para la implementación de este novedoso abordaje en el manejo de la acalasia en la población colombiana.
Palabras clave: Acalasia; desórdenes de la motilidad esofágica; miotomía endoscópica por vía oral; miotomía de Heller
Introduction
Peroral endoscopic myotomy (POEM) is a true surgical technique performed via a natural orifice (natural orifice transluminal endoscopic surgery -NOTES-) for management of achalasia, a chronic esophageal motility disorder in which the muscle tone of the lower esophageal sphincter (LES) progressively increases. The current treatment of choice is a laparoscopic Heller myotomy (LHM) in which the circular musculature of the lower esophageal sphincter is cut. Although it is demonstrably effective, 1 in 2007 Dr. J. Pasricha et al. described POEM in pigs. 2 This laid the foundations for the procedure which was performed in humans for the first time in 2008 by Dr. Haruhiro Inoue who published his first series of cases in 2010. 3 Use of this endoscopic technique is growing, and its results in terms of clinical improvement have been similar to those of LHM. 4 Moreover, POEM has the important advantage of being a purely endoscopic approach which offers rapid recovery with very short hospital stays. In addition, a zero percent mortality rate has been reported in one of the largest series which covered 500 patients. 5
This led us to think that this novel and promising endoscopic approach can positively contribute to the evolution and recovery of patients with achalasia. This is the first series of cases from Colombia that has been published. All procedures were performed by a single endoscopic surgeon. Our results are analyzed.
Materials and methods
We performed a retrospective review of the clinical records of patients diagnosed with esophageal achalasia who were treated with POEM at the Organización Clínica General del Norte, in Barranquilla, Colombia between June 2015 and November 2017. This procedure was performed by an endoscopic surgeon with therapeutic experience. Intravenous antibiotic prophylaxis with single 1 g dose of Cefazolin was administered 30 minutes before surgery in all interventions.
Equipment used included an Olympus Excera 2 CV-180 with carbon dioxide unit (CO2), a Fujinom VP-4450 HD with a Fujifilm GW100 CO2 unit, an ERBE VIO 200 S and a VIO 300 D unit with an ERBEJET 2 hydrodissection unit.
Surgical technique
Step 1: General anesthesia with patient in dorsal decubitus and nasotracheal intubation.
Step 2: Esophageal lavage performed with 500 cc of 0.9% normal saline solution with endoscope with therapeutic channel.
Step 3: Identification of anatomical location of UES, aortic arch, left bronchus, LES and silhouette of the spine which in turn can be corroborated by instilling 30 mL water in the esophageal lumen and observing the area of decline (Figure 1).
Step 4: Papule formed by submucosal injection with 10 mL of dextrose in distilled water 5% in normal saline solution mixed with indigo carmine or methylene blue together with 80 mg of gentamicin at a location immediately inferior to the anatomical repair of the aortic arch and left bronchus at the 5 o’clock position (Figure 2 A).
Step 5: A 1.5 cm longitudinal mucosotomy is cut with a Triangle Tip Electrosurgical Knife or ERBE Hybrid electrocautery knife including into the submucosal cellular tissue at the most distal vertex of the mucosotomy. This allows easy introduction of the distal plastic cup of the endoscope. Application of the dye mixture can be repeated during dissection of submucosal tissue to facilitate progression of dissection (Figure 2 B).
Step 6: Submucosal tunnel created with the electrocautery knife in spray coagulation mode. Tunnel should be extended until beyond 3 cm distal to the cardia along the 5 o’clock axis. The cut should be made very close to the circular layer of muscle which must be viewed completely horizontal and inferior to the axis of the endoscope taking maximum care not to injure the esophageal mucosa (Figure 2 C). It is useful to remove the endoscope several times from the submucosal tunnel and reintroduce it into the esophageal lumen to verify that the dissection is being performed on the 5 o’clock axis and also to confirm when the dissection exceeds the LES. This can be complemented by observing the cardia in retroflexion and following the column of indigo carmine.
Step 7: Myotomy starts 2 cm lower than mucosotomy at 5 o’clock and continues up to 3 cm below the cardia. It cuts only the circular (internal) muscular layer of the esophagus until the external longitudinal muscle fibers can be seen (Figure 2 D).
Step 8: Review and closure of mucosotomy: Exhaustively check hemostasis in the tunnel, washing residuals with normal saline solution followed by gentle suction and closure of the mucosotomy with blue Olympus clips. Placing the first 0.5 cm distal to the lower vertex of the mucosotomy to allow the formation of a fold to facilitate placement of the second clip. Continue in this manner with 6 to 8 clips until the mucosotomy is closed. Sealing of both sides of the row of clips should be corroborated at the end of the surgery (Figure 2 E).
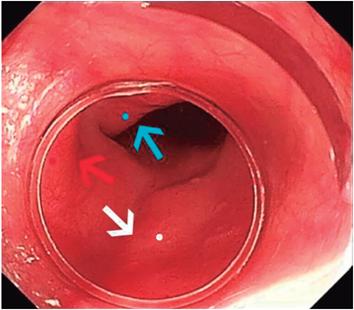
Figure 1 Anatomical repairs: aortic arch (red arrow and dot), left source bronchus (arrow and blue dot) and silhouette of the spine (arrow and white dot) (6).
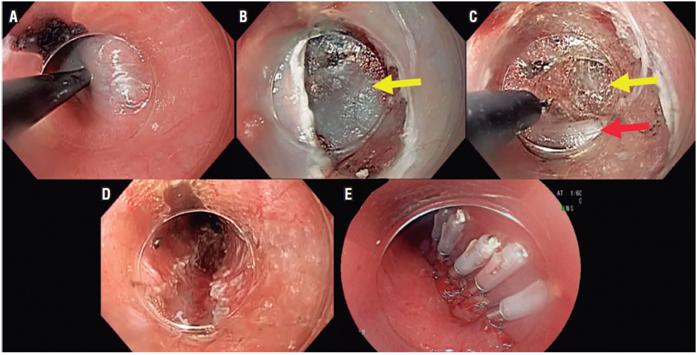
Figure 2 Steps of a POEM. A. Papule. B. Mucosotomy (yellow arrow: submucosal space). C. Submucosal tunnel (yellow arrow: submucosal space, red arrow: circular muscle layer). D. Myotomy. E. Mucosotomy closure.
When the procedure is finished, all patients undergo a chest X-ray primarily to rule out pneumothorax. Twenty-four hours later, an esophagogram is performed with water-soluble medium. If there are no leaks, a liquid diet is started. It is maintained for one week, followed by a diet of soft foods the second week, and a return to the normal diet by the third week.
Results
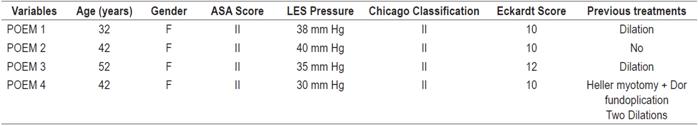
We found four female patients who had undergone POEM to treat achalasia between June 2015 and November 2017. Their preoperative characteristics are specified in Table 1. The patients had LES pressure measurements greater than 30 mm Hg, one had previously undergone a laparoscopic Heller myotomy, and two had previously undergone pneumatic dilatations.
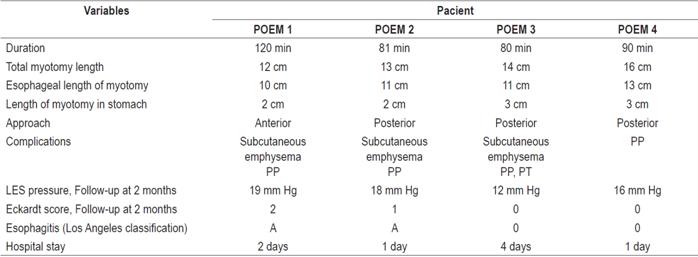
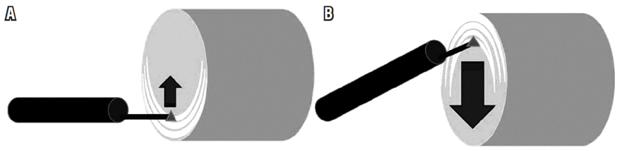
Postoperative results are shown in Table 2. The posterior route was used for three of the four patients because it was considered more practical at the time of the myotomy since the output of the electrocautery knife is located on the 6 o’clock axis of the equipment. This places the camera at 12 o’clock which allows better visualization of the muscular plane to be sectioned (Figure 3). Only POEM 1 was performed anteriorly, towards 2 o’clock, which resulted in longer procedure time and greater degree of difficulty than in the other three procedures (POEM 2-4). Events derived from myotomy and CO2 pressure occurred in all four patients. The most common, detection of pneumoperitoneum by the capnography, was managed intraoperatively without complications by inserting a Jelco 14G catheter connected to a water trap into the right flank. One of the patients developed left pneumothorax, which was managed by creating a closed drainage system with a 28 Fr thoracostomy tube that was removed 24 hours later after a chest x-ray showed e resolution of the pneumothorax. This was the reason the patient (POEM 3) had a longer hospital stay than did the other patients. Subcutaneous emphysema does not require additional management because it is self-limiting.
In all four of our cases, symptoms derived from achalasia clearly decreased as shown by Eckardt scores. This indicates that the surgery was successful in 100% of the patients. High resolution esophageal manometry showed decreases in LES pressure that were practically 50% less than the measurements prior to performance of POEM. Slight esophagitis after procedures was managed with proton pump inhibitors (PPI), to provide even more evident clinical improvement and better quality of life for these patients. There were no deaths in this series of cases.
Discussion
Achalasia is a progressive, medically irreversible disease is idiopathic in most cases but can also be secondary as in Chagas disease and herpes virus. 1,7 It is more common in people from the third to the fifth decade of life, as in the cases of our patients. Its incidence is from 0.4 per 100,000 inhabitants to 1.2 per 100,000 inhabitants, and its prevalence ranges from 7 to 13 per 100,000 inhabitants. 8 It has been treated pharmacologically and with botulinum toxin, but long term success rates have been low and there have been poorly tolerated side/effects. 7,9 The guidelines of the American College of Gastroenterology (ACG) and the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) recommend pneumatic dilation which has had a four-year success rate of 93%. 7,10,11 Nevertheless, this methods’ results for five year dysphagia-free time ranges from 40% to -78% while LHM has an average success rate of 89% (77% -100%) including one report of 75% at 15.8 years of follow-up. 12,13,14
With Dr. Inoue’s 2008 introduction of POEM, a new horizon in the management of this pathology has opened up. As of now, there have been more than 5,000 POEM procedures performed with good results worldwide. This makes the procedure the most successful version of NOTES. 3,15 It has also been used for difficult-to-manage motor disorders such as diffuse esophageal spasms and nutcracker/jackhammer esophagus 16,17,18.
The success of POEM for management of achalasia has been measured primarily by two parameters: LES pressure of the LES and the Eckardt score. 19 A success rates of 93% with a very low incidence of major complications has been found. 20 This efficacy has been demonstrated in studies published such as that of Haruhiro Inoue et al. of 500 patients who were treated with POEM after being diagnosed diagnosed with achalasia. Both the anterior and posterior routes were used in these patients, and high resolution esophageal manometry and Eckardt scores were evaluated two months after the procedues. 5 Preoperative measurements were 25.4 ± 17.1 and 6.0 ± 3.0 while and postoperative measures were 13.4 ± 5.9 mm Hg, p <0.0001 and 1.0 ± 2.0, p <0.0001. These results show clear reductions in LES pressure and in occurrence of patients’ symptoms. Similar data were obtained by Rupjyoti Talukdar et al. in a meta-analysis covering 1,045 patients in 19 studies. 21
Despite the small sample size, our results coincide with the aforementioned literature and show evident improvement of Eckardt scores and LES pressure. In our study population, one patient had undergone a LHM before and after dilations. This added greater degree of difficulty to the procedure due to the fibrotic process. Nevertheless, this is the circumstance in which a posterior myotomy is most useful because the plane of dissection can be seen more clearly (Figure 4). 5,22
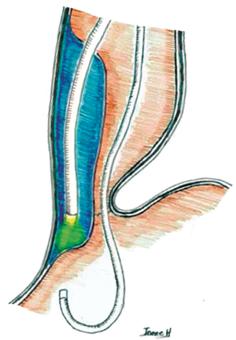
Figure 4 Double endoscope technique shown with endoscope in gastric chamber at retroflexion with transillumination of the endoscope via the submucosal tunnel and the myotomy. 23
Several studies have compared the results of POEMs and LHMs. One metaanalysis published in 2015 found the odds ratio (OR) for the risk of complications to be 1.17 with a 95% confidence interval of 0.53 to 2.56 (p = 0.70) while the OR for gastroesophageal reflux was 1.00 with a 95% CI of 0.38 to 2.61 (p = 1.00). (24) In 2015, Vivek Kumbhari et al. published a retrospective multicenter study that compared POEM to LHM in patients with type III achalasia. POEM’s results were superior for clinical improvement, shorter operating times, and greater myotomy length: (98.0% vs. 80.8%, p = 0.01), (102 min vs. 264 min, p <0.01) (16 cm vs. 8 cm, p <0.01). All of these differences are statistically significant. 4 One implication is that POEM can be used to successfully treat Type III achalasia which requires a longer myotomy which is not possible through LHM.
In our patients, myotomy cuts were 12 cm or longer, and operating times decreased each time including for the performance of the most complex case, the patient in POEM 4.
The use of a hybrid knife significantly reduced both surgical time and bleeding from those common with a conventional triangle knife. This is because it offers the possibility of making injections to raise the submucosal plane and at the same time as performing electrocautery. 25 This device was used in two procedures and proved to be more practical because it decreased the times of introduction and removal of tools through the working channel of the endoscope.
For difficult cases such as patients whose which LES anatomy has been distorted by previous Heller myotomy, dilations, and/or administration of botulinum toxin, a second pediatric diameter endoscope can be used (Figure 3). In our cases there was no need for this technique, but it can be used to achieve a longer gastric myotomy (3.2 cm versus 2.5 cm, p = 0.013) and lower the risk of perforation of the gastric mucosa. Nevertheless, use of the technique has had no significant impact on the success rate. 23
Grades B and C esophagitis can occur in up to 16% of patients especially when the integrated relaxation pressure (IRP) is low (≈9.5 mm Hg) at the postoperative follow-up. 26 In our cases, half of the patients developed mild esophagitis which responded to PPI therapy.
Complication rates vary. One metaanalysis by K. Patel et al. has covered 22 studies with 1,122 patients who underwent POEM. It reported that 392 patients who had previously been treated for achalasia suffered the following complications: subcutaneous emphysema in 31.6%, pneumoperitoneum in 30.6 %, pneumothorax in 11%, pneumoperitoneum requiring decompression in 8%, pneumothorax requiring decompression in 2.7%, postoperative bleeding in 1.1%, esophageal perforation/mediastinal leakage in 0.3% and mortality in 0.09% of the cases. The aforementioned series of 500 patients with achalasia managed with POEM that was published by Haruhiro Inoue et al. found that 195 had previously been treated (Ten had undergone laparoscopic Heller myotomies). The overall rate of complications was 3.2% (16 patients). One case of pneumothorax with pneumomediastinum, one case of bleeding, one case of perforation of the mucosa, eight cases of postoperative hematomas in the tunnel, three cases of inflammation in the lesser omentum, and one case of pleural effusion. There were no deaths. 5 Our findings correlate well with those observed in the literature although all of our patients developed pneumoperitoneum that resolved with a Jelco catheter and a water trap without resulting in any major complication or mortality.
In cases in which symptoms persist after the first POEM, the procedure can be repeated on another axis with safe results and significant clinical improvement. This has been demonstrated by Amy Tyberg-Stefan Seewald and her colleagues in a study of 46 patients published in 2017. 27
A prospective series that analyzed the learning curve for POEM has concluded that at least 40 cases are required to master the technique. Variables used included surgical time and the number of perforations in the mucosa with these two variables becoming more constant with performance of more procedures. 28
In conclusion, POEM is a safe and effective technique according to the current literature. A posterior myotomy is technically easier than the previous route, has a low morbidity rate, and does not require more complex equipment than that used in a therapeutic endoscopy unit. Our results are limited by the small sample size and, therefore, cannot be judged with high statistical power, but they are the first step for implementation of, and expansion of the use of, POEM in our population.
Acknowledgements
This study was made possible by the collaboration and support of the Clínica General del Norte in Barranquilla, Colombia which contributed its human resources, facilities, equipment and support
REFERENCES
1. Pandolfino JE, Gawron AJ. Achalasia: a systematic review. JAMA. 2015;313(18):1841-52. doi: 10.1001/jama.2015.2996. [ Links ]
2. Pasricha PJ, Hawari R, Ahmed I, Chen J, Cotton PB, Hawes RH, et al. Submucosal endoscopic esophageal myotomy: a novel experimental approach for the treatment of achalasia. Endoscopy. 2007;39(9):761-4. doi: 10.1055/s-2007-966764. [ Links ]
3. Inoue H, Minami H, Kobayashi Y, Sato Y, Kaga M, Suzuki M, et al. Peroral endoscopic myotomy (POEM) for esophageal achalasia. Endoscopy. 2010;42(4):265-71. doi: 10.1055/s-0029-1244080. [ Links ]
4. Kumbhari V, Tieu A, Onimaru M, El Zein MH, Modayil RJ, Teitelbaum EN, et al. 730 PerOral Endoscopic Myotomy (POEM) Versus Laparoscopic Heller Myotomy (Lhm) for the Treatment of Type III Achalasia in 75 Patients: an International Multicenter Experience. Gastrointest Endosc. 2014;79(5):AB166. doi: 10.1016/j.gie.2014.02.167. [ Links ]
5. Inoue H, Sato H, Ikeda H, Onimaru M, Sato C, Minami H, et al. Per-Oral Endoscopic Myotomy: A Series of 500 Patients. J Am Coll Surg. 2015;221(2):256-64. doi: 10.1016/j.jamcollsurg.2015.03.057. [ Links ]
6. Bechara R, Onimaru M, Ikeda H, Inoue H. Per-oral endoscopic myotomy, 1000 cases later: pearls, pitfalls, and practical considerations. Gastrointest Endosc. 2016;84(2):330-8. doi: 10.1016/j.gie.2016.03.1469. [ Links ]
7. Vaezi MF, Pandolfino JE, Vela MF. ACG clinical guideline: diagnosis and management of achalasia. Am J Gastroenterol. 2013 Aug;108(8):1238-49. doi: 10.1038/ajg.2013.196. [ Links ]
8. O’Connor JB, Singer ME, Imperiale TF, Vaezi MF, Richter JE. The cost-effectiveness of treatment strategies for achalasia. Dig Dis Sci. 2002;47(7):1516-25. [ Links ]
9. Martínek J, Siroký M, Plottová Z, Bures J, Hep A, Spicák J. Treatment of patients with achalasia with botulinum toxin: a multicenter prospective cohort study. Dis Esophagus. 2003;16(3):204-9. [ Links ]
10. Stefanidis D, Richardson W, Farrell TM, Kohn GP, Augenstein V, Fanelli RD, et al. SAGES guidelines for the surgical treatment of esophageal achalasia. Surg Endosc. 2012;26(2):296-311. doi: 10.1007/s00464-011-2017-2. [ Links ]
11. Kadakia SC, Wong RK. Pneumatic balloon dilation for esophageal achalasia. Gastrointest Endosc Clin N Am. 2001;11(2):325-46, vii. [ Links ]
12. Zerbib F, Thétiot V, Richy F, Benajah DA, Message L, Lamouliatte H. Repeated pneumatic dilations as long-term maintenance therapy for esophageal achalasia. Am J Gastroenterol. 2006;101(4):692-7. doi: 10.1111/j.1572-0241.2006.00385.x. [ Links ]
13. Campos GM, Vittinghoff E, Rabl C, Takata M, Gadenstätter M, Lin F, et al. Endoscopic and surgical treatments for achalasia: a systematic review and meta-analysis. Ann Surg. 2009;249(1):45-57. doi: 10.1097/SLA.0b013e31818e43ab. [ Links ]
14. Csendes A, Braghetto I, Burdiles P, Korn O, Csendes P, Henríquez A. Very late results of esophagomyotomy for patients with achalasia: clinical, endoscopic, histologic, manometric, and acid reflux studies in 67 patients for a mean follow-up of 190 months. Ann Surg. 2006;243(2):196-203. doi: 10.1097/01.sla.0000197469.12632.e0. [ Links ]
15. Mejía R, Donoso A, Manríquez E, Sáez J, Crovari F, Gabrielli M, et al. Miotomía endoscópica por vía oral (POEM) para el tratamiento de la acalasia. Experiencia clínica inicial y resultados a corto plazo. Rev Chil Cirugía. 2017;69(5):429-34. doi: 10.1016/j.rchic.2017.03.004. [ Links ]
16. Khashab MA, Messallam AA, Onimaru M, Teitelbaum EN, Ujiki MB, Gitelis ME, et al. International multicenter experience with peroral endoscopic myotomy for the treatment of spastic esophageal disorders refractory to medical therapy (with video). Gastrointest Endosc. 2015 May;81(5):1170-7. doi: 10.1016/j.gie.2014.10.011. [ Links ]
17. Paterson WG, Beck IT, Da Costa LR. Transition from nutcracker esophagus to achalasia. A case report. J Clin Gastroenterol. 1991;13(5):554-8. [ Links ]
18. Khan MA, Kumbhari V, Ngamruengphong S, Ismail A, Chen YI, Chavez YH, et al. Is POEM the Answer for Management of Spastic Esophageal Disorders? A Systematic Review and Meta-Analysis. Dig Dis Sci. 2017;62(1):35-44. doi: 10.1007/s10620-016-4373-1. [ Links ]
19. Eckardt AJ, Eckardt VF. Treatment and surveillance strategies in achalasia: an update. Nat Rev Gastroenterol Hepatol. 2011;8(6):311-9. doi: 10.1038/nrgastro.2011.68. [ Links ]
20. Barbieri LA, Hassan C, Rosati R, Romario UF, Correale L, Repici A. Systematic review and meta-analysis: Efficacy and safety of POEM for achalasia. United European Gastroenterol J. 2015;3(4):325-34. doi: 10.1177/2050640615581732. [ Links ]
21. Talukdar R, Inoue H, Nageshwar Reddy D. Efficacy of peroral endoscopic myotomy (POEM) in the treatment of achalasia: a systematic review and meta-analysis. Surg Endosc. 2015;29(11):3030-46. doi: 10.1007/s00464-014-4040-6. [ Links ]
22. Nabi Z, Ramchandani M, Chavan R, Kalapala R, Darisetty S, Rao GV, et al. Per-oral endoscopic myotomy for achalasia cardia: outcomes in over 400 consecutive patients. Endosc Int Open. 2017;5(5):E331-E339. doi: 10.1055/s-0043-105517. [ Links ]
23. Grimes KL, Inoue H, Onimaru M, Ikeda H, Tansawet A, Bechara R, et al. Double-scope per oral endoscopic myotomy (POEM): a prospective randomized controlled trial. Surg Endosc. 2016;30(4):1344-51. doi: 10.1007/s00464-015-4396-2. [ Links ]
24. Wei M, Yang T, Yang X, Wang Z, Zhou Z. Peroral esophageal myotomy versus laparoscopic Heller’s myotomy for achalasia: a meta-analysis. J Laparoendosc Adv Surg Tech A. 2015;25(2):123-9. doi: 10.1089/lap.2014.0454. [ Links ]
25. Cai MY, Zhou PH, Yao LQ, Xu MD, Zhong YS, Li QL, et al. Peroral endoscopic myotomy for idiopathic achalasia: randomized comparison of water-jet assisted versus conventional dissection technique. Surg Endosc. 2014;28(4):1158-65. doi: 10.1007/s00464-013-3300-1. [ Links ]
26. Shiwaku H, Inoue H, Sasaki T, Yamashita K, Ohmiya T, Takeno S, et al. A prospective analysis of GERD after POEM on anterior myotomy. Surg Endosc. 2016;30(6):2496-504. doi: 10.1007/s00464-015-4507-0. [ Links ]
27. Tyberg A, Seewald S, Sharaiha RZ, Martinez G, Desai AP, Kumta NA, et al. A multicenter international registry of redo per-oral endoscopic myotomy (POEM) after failed POEM. Gastrointest Endosc. 2017;85(6):1208-1211. doi: 10.1016/j.gie.2016.10.015. [ Links ]
28. Kurian AA, Dunst CM, Sharata A, Bhayani NH, Reavis KM, Swanström LL. Peroral endoscopic esophageal myotomy: defining the learning curve. Gastrointest Endosc. 2013;77(5):719-25. doi: 10.1016/j.gie.2012.12.006. [ Links ]
Received: December 19, 2017; Accepted: March 08, 2018











 text in
text in