Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Revista colombiana de Gastroenterología
versión impresa ISSN 0120-9957
Rev Col Gastroenterol vol.33 no.4 Bogotá oct./dic. 2018
https://doi.org/10.22516/25007440.315
Case report
Severe acute pancreatitis due to hypertriglyceridemia in adults: Clinical case presentation, diagnosis and treatment
1Médico cirujano, especialista en Medicina Crítica y Cuidado Intensivo. Fundación Santa Fe de Bogotá. Bogotá D. C., Colombia
2Médico cirujano, residente de Cirugía General III año Universidad Surcolombiana. Especialista en Epidemiología. Hospital Universitario Hernando Moncaleano Perdomo. Neiva, Colombia
3Médico cirujano, residente de Medicina Crítica y Cuidados Intensivos. Fundación Santa Fe de Bogotá. Bogotá D. C., Colombia
Pancreatitis is one of the most frequent gastrointestinal causes of hospital admission. In 2009, it accounted for more than 275,000 admissions to emergency departments in the United States. (1) Hypertriglyceridemia is the third most frequent cause of pancreatitis, and triglyceride levels over 1,000 mg/dl are considering to indicate high risk for its development. (2) This group of patients has a worse prognosis than those with pancreatitis of other etiologies, but to date, no clear standard definition of how the range of triglyceride levels is related to the severity of acute pancreatitis has been defined.
There are several pathophysiological mechanisms that explain the onset of pancreatitis in the context of hypertriglyceridemia. One of the best studied is the toxic role of free fatty acids on pancreatic tissue. (3) Another widely accepted mechanism is vascular obstruction mediated by chylomicrons given the decrease in the genetic expression of lipoprotein lipase (LPL). (4)
Successful treatment of this disease is based on lowering triglyceride levels below 500 mg/dl. One fast and effective tool for achieving this is plasmapheresis.
Keywords: Acute pancreatitis; triglycerides; plasmapheresis
La pancreatitis es una de las causas más frecuentes de admisión hospitalaria gastrointestinal; en 2009 representó más de 275 000 ingresos a urgencias en Estados Unidos (1). Por su parte, la hipertrigliceridemia es la tercera causa más frecuente, considerándose como de alto riesgo para el desarrollo de pancreatitis los valores superiores a 1000 mg/dL (2); este grupo de pacientes tiene peor pronóstico que quienes cursan con pancreatitis de otra etiología, aunque aún no se logra definir de forma clara y estandarizada un rango de triglicéridos (TAG) que se relacione con la gravedad de la pancreatitis aguda.
Existen varios mecanismos fisiopatológicos que explican la aparición de pancreatitis en el contexto de la hipertrigliceridemia, uno de los mejor estudiados es el papel tóxico directo de los ácidos grasos libres sobre el tejido pancreático (3) y otro mecanismo ampliamente acogido es la obstrucción vascular mediada por los quilomicrones, dada la disminución de la expresión genética de la lipoproteína lipasa (LPL) (4).
Por su parte, el éxito del tratamiento de esta enfermedad se basa en disminuir los niveles de TAG a menos de 500 mg/dL, teniendo para esto entre otras herramientas la plasmaféresis, tratamiento que ofrece rapidez y efectividad en la reducción de los niveles de TAG.
Palabras clave: Pancreatitis aguda; triglicéridos; plasmaféresis
Introduction
Acute pancreatitis is defined as an inflammatory response of the pancreas which can be secondary to various causes including gallstones, alcohol, and hypertriglyceridemia (HTG). It can produce a wide spectrum of local, regional or systemic complications. Local complications include necrosis, abscesses, pseudocysts and ascites while systemic complications include a wide manifestations ranging from the appearance of gastrointestinal hemorrhaging, hyperglycemia, hypercalcemia, development of insulin-dependent diabetes and diabetic ketoacidosis to the development of acute respiratory distress syndrome (ARDS), multi-organ dysfunction, disseminated intravascular coagulation and compartment syndrome.
It is interesting that diabetic ketoacidosis secondary to acute pancreatitis occurs infrequently in clinical practice, but that case reports and clinical studies reporting the occurrence of this complication note its association with HTG pancreatitis. 5,6 Occurrence of multiorgan failure in association with compartment syndrome is even more infrequent.
Clinical case
The patient was a 34-year-old woman patient with a history of polycystic ovary syndrome, type 2 diabetes mellitus and morbid obesity (body mass index [BMI]: 40 kg/m2). She came to the hospital following four days of nausea, vomiting and associated with epigastric pain irradiating in a band whose intensity had increased to 9/10. She had no fever or other symptoms. She had been in the process of doing the paperwork for bariatric surgery, and in the week prior to admission she had consumed more carbohydrates and fats than usual in order to achieve the minimum weight required for the procedure.
Upon admission, grade II dehydration and blood glucose of 315 mg/dL were found. Laboratory tests (Table 1) showed metabolic acidemia associated with amylase of 643 and lipase of 1,281. With these findings, a diagnosis of moderately severe pancreatitis of unknown origin was made.
Table 1 Laboratory report
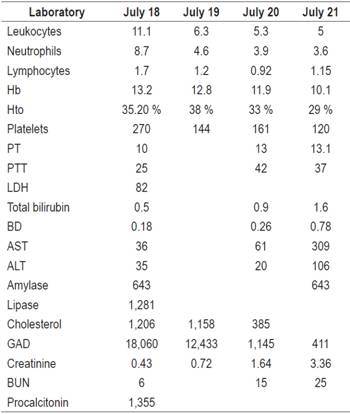
ALT: alanine aminotransferase; AST: aspartate aminotransferase; BUN: blood urea nitrogen; GAD: glutamic acid decarboxylase Hb: hemoglobin; Hto: hematocrit; LDH: lactate dehydrogenase; PT: prothrombin time; PTT: partial thromboplastin time.
Subsequently, a CT scan (Figures 1 and 2) showed Balthazar D pancreatitis. She was staged with Marshall 1, Balthazar D, and APACHE-II: 20 pancreatitis with a 35% probability of death. Given her severe pancreatitis, she was transferred to the intensive care unit (ICU). A metabolic profile to clarify the ethology showed 18,060 mg/dL of glutamic acid decarboxylase (GAD) and hemoglobin A1c (HbA1c) at 9.87%.
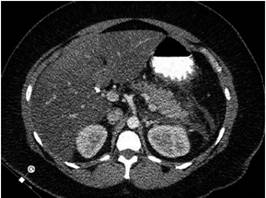
Figure 1 Double abdominal CAT scan abdomen showing definite collection of liquid around the pancreas especially towards the tail of the pancreas compatible with a Balthazar E score.

Figure 2 Double abdominal CAT scan showing definite collection of liquid around the pancreas. especially towards the tail of the pancreas compatible with a Balthazar D score.
Twelve hours after admission, progressive hemodynamic deterioration required staggered doses of dual vasopressor and metabolic support with insulin infusion (20 -30 IU/h but patient had poor glucose control 235-350 mg/dL). Finally, daily plasmapheresis was ordered by a multidisciplinary meeting (Figure 3).

Figure 3 Process and result of initial plasmapheresis of this patient who had severe pancreatitis due to hypertriglyceridemia.
During the second day of hospitalization, refractory distributive shock developed and early monitoring of intra-abdominal pressure (IAP) found an increase from 18 to 25 mm Hg. Medical measures to reduce IAP including neuromuscular relaxation were taken, but IAP continued to increase until it was over 29 mm Hg, a level associated with oligoanuria and worsening oxygenation parameters. She was diagnosed with abdominal compartment syndrome refractory to medical management. A laparotomy drained 700 mL of serous peritoneal fluid but found no evidence of signs of steatonecrosis. During the procedure, the omentum was not examined. The abdomen was left open with a negative pressure system.
After 3 cycles of plasmapheresis, her levels of GAD progressively decreased from 18,060 to 12,433 to 2,670 to 1,145 and to 411 mg/dL. In addition her blood glucose improved.
Nevertheless, progressive hemodynamic deterioration persisted and multi-organ dysfunction and refractory hypoxemia developed. She finally died 72 hours after admission.
Discussion
Pancreatitis is defined as an inflammatory process located in the viscera which is secondary to enzymatic activation (trypsin) within the pancreatic parenchyma in most cases.
The causes are subject to demographic characteristics and dietary habits of patients. Currently, alcohol and gallstones are recognized as the main causes and accounting for 80% of all cases. HTG accounts for 2% to 4% of all cases, and other causes including drugs and trauma account for smaller percentages.
Pathophysiology
At present, the pathophysiological mechanism of acute pancreatitis due to hypertriglyceridemia (AP-HTG) is not fully understood. The most widely accepted theories argue that fatty acids directly harm pancreatic tissue leading to compromised acinar activity, inhibition of mitochondrial function of complexes I and V, and release of calcium causing cell necrosis. 3 Another recent theory proposes that HTG episodes occur when albumin, a GAD transport protein, becomes saturated. This increases the free concentration of GAD that, after degradation by endothelial lipase and lysophosphatidylcholine, generates cellular toxicity and triggers an inflammatory response mediated by tumor necrosis factor alpha (TNF-α) and interleukin 6 [IL-6]) in the pancreas. This can even lead to multisystem compromise due to inflammation. 3,7
It has been argued that gene expression of lipoprotein lipase (LPL), an enzyme produced in muscles and adipocytes, decreases. This enzyme is transported to the capillary endothelium where it is responsible for hydrolyzing chylomicrons and rich lipoproteins in GAD fatty acids and glycerol which are finally carried to the liver, skeletal muscle, myocardium and adipocytes for use. LPL deficiency causes abnormal degradation of chylomicrons. 8 Similarly, following high concentrations of chylomicrons, obstruction of the distal pancreatic circulation occurs causing ischemia due to alteration of blood rheology. This generates structural damage of the pancreatic tissue exposing it to the GAD and leading to the production of a local acidic medium that facilitates activation of lipase and trypsinogen.
The existence of diffuse destruction of β cells of the pancreas has also been demonstrated. Its main effect is to cause concomitant diabetic ketoacidosis. This adds to the high levels of production of counter regulatory hormones, increases blood glucose levels and decreases circulating functional insulin. 9
Diagnosis
AP-HTG occurs in patients with a history of HTG defined as a fasting serum GAD level above the 95th percentile for age and sex. 10 A high concentration of serum GAD results from increased production or decreased catabolism of lipid products and is usually caused by genetic and environmental factors. Among environmental factors are alcohol consumption, 11 obesity, diabetes mellitus, pregnancy and the use of drugs that cause secondary HTG.
Serum GAD levels for diagnosis of AP-HTG picture have not been established, but the most common definition of AP-HTG reported in the literature is GAD>1,000 mg/dL associated levels of amylase or lipase three times the base level. Recently, reports have used GAD levels greater than 500 mg/dL to diagnose HTG. It has also been found that the average serum concentration of GAD of all patients with AP-HTG is over 2,654 mg/dL which is remarkably high. 12,13
Treatment
No standard treatment for management of this disease has been described, and literature on the subject is scarce. Most published articles are case reports, and there are few guidelines available given that this is not a frequent pathology. Treatment revolves around adequate water resuscitation, conventional analgesic management, stabilization of serum glucose levels with goals of 140-180 mg/dL) and decreasing levels of GAD.
Fasting usually plays an important role in treatment of these patients since it favors rapid metabolism of chylomicrons and GAD. In addition, goal-directed water resuscitation and vasopressor or inotropic support are of vital importance for reducing morbidity and mortality in this group of patients.
Various integral management options for HTG have been proposed. They include
1. Insulin or heparin infusions: These drugs increase activity of plasma LPL linked to the endothelium, and insulin favors the degradation of chylomicrons. In the clinical case described, insulin infusion was used empirically in order to achieve blood glucose goals in the face of pancreatitis. This treatment was maintained throughout the hospitalization period, due to the difficultly of control blood glucose levels.
2. Plasmapheresis has been described in numerous articles as one of the most useful tools for reduction of GAD levels. At the same time, it helps clear proinflammatory cytokines and reduces plasma viscosity which improves blood rheology.
At present, it is not clear which patients benefit from plasmapheresis, but some studies suggest better results in patients with severely elevated GAD (GAD> 2000 mg/dL) associated with severe pancreatitis according to the Revised Atlanta Classification. 14,15 A systematic review found that patients with AP-HTG required more than two cycles of plasmapheresis, especially for initial levels over 4,425 mg/dL. 14 In the clinical case presented here, the patient initially has a very high initial level of GAD which was reduced by 97% from 18,060 to 411 mg/dL after 3 cycles of plasmapheresis. This result matches those reported in the literature which show reductions of over 84% after 2 cycles of plasmapheresis. Decreases in mortality rates have been reported, and reduced APACHE-II scores have been reported in 42% of patients receiving plasmapheresis.
Severe pancreatitis also entails increased risk of acute coronary syndrome (ACS) which makes it necessary to recognize risk factors of obesity, vigorous water resuscitation and pancreatic collections to begin early monitoring of IAP. Using conventional medical strategies, its incidence can be reduced. 15 In the clinical case presented, the patient’s serious clinical deterioration and the poor response to medical management of compartment syndrome led to our decision to use laparotomy for decompression in order to decrease IAP and pressures on the compromised compartments. Finally, it was decided not to explore the cavity of the omentum in the first and only surgery performed due to the characteristics of the peritoneal fluid seen during surgical exploration and in order to decrease the duration of surgery.
Conclusions
Pancreatitis occurs frequently in the general population, but when it is caused by HTG it is more difficult to characterize, there is still no standardized treatment, and its possible impact on the prognosis for morbidity and mortality is unknown. Studies and guidelines are needed to clarify the panorama of physiopathology and management of this entity
Referencias
1. Peery AF, Dellon ES, Lund J, Crockett SD, McGowan CE, Bulsiewicz WJ, et al. Burden of gastrointestinal disease in the United States: 2012 update. Gastroenterology. 2012;143(5):1179-87.e3. doi: 10.1053/j.gastro.2012.08.002. [ Links ]
2. Berglund L, Brunzell JD, Goldberg AC, Goldberg IJ, Sacks F, Murad MH, et al. Evaluation and treatment of hypertriglyceridemia: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2012;97(9):2969-89. doi: 10.1210/jc.2011-3213. [ Links ]
3. Navina S, Acharya C, DeLany JP, Orlichenko LS, Baty CJ, Shiva SS, et al. Lipotoxicity causes multisystem organ failure and exacerbates acute pancreatitis in obesity. Sci Transl Med. 2011;3(107):107ra110. doi: 10.1126/scitranslmed.3002573. [ Links ]
4. Gan SI, Edwards AL, Symonds CJ, Beck PL. Hypertriglyceridemia- induced pancreatitis: A case-based review. World J Gastroenterol. 2006;12(44):7197-202. doi: 10.3748/wjg.v12.i44.7197. [ Links ]
5. Aboulhosn K, Arnason T. Acute pancreatitis and severe hypertriglyceridaemia masking unsuspected underlying diabetic ketoacidosis. BMJ Case Rep. 2013;2013. pii: bcr2013200431. doi: 10.1136/bcr-2013-200431. [ Links ]
6. Quintanilla-Flores DL, Rendón-Ramírez EJ, Colunga-Pedraza PR, Gallardo-Escamilla J, Corral-Benavides SA, González-González JG, et al. Clinical course of diabetic ketoacidosis in hyper- triglyceridemic pancreatitis. Pancreas. 2015;44:615-8. doi: 10.1097/MPA.0000000000000300. [ Links ]
7. Pierre N, Deldicque L, Barb!e C, et al. Toll-like receptor 4 knockout mice are protected against endoplasmic reticulum stress induced by a high-fat diet. PLoS One. 2013 May 31;8(5):e65061. doi: 10.1371/journal.pone.0065061. Print 2013. [ Links ]
8. Nair S, Yadav D, Pitchumoni CS. Association of diabetic ketoaci- dosis and acute pancreatitis: observations in 100 consecutive episodes of DKA. Am J Gastroenterol. 2000;95:2795-2800. doi: 10.1111/j.1572-0241.2000.03188.x. [ Links ]
9. Click B, Ketchum AM, Turner R, Whitcomb DC, Papachristou GI, Yadav D. The role of apheresis in hypertriglyceridemia-induced acute pancreatitis: a systematic review. Pancreatology. 2015;15(4):313-20. doi: 10.1016/j.pan.2015.02.010. [ Links ]
10. Yuan G, Al-Shali KZ, Hegele RA. Hypertriglyceridemia: its etiology, effects and treatment. CMAJ. 2007;176:1113-20. doi: 10.1503/cmaj.060963. [ Links ]
11. Bessembinders K, Wielders J, van de Wiel A. Severe hypertriglyceridemia influenced by alcohol (SHIBA). Alcohol Alcohol. 2011;46(2):113-6. doi: 10.1093/alcalc/agq088. [ Links ]
12. Yadav D, Pitchumoni CS. Issues in hyperlipidemic pancreatitis. J Clin Gastroenterol. 2003;36:54-62. doi: 10.1097/00004836-200301000-00016. [ Links ]
13. Ewald N, Hardt PD, Kloer HU. Severe hypertriglyceridemia and pancreatitis: presentation and management. Curr Opin Lipidol. 2009;20:497-504. doi: 10.1097/MOL.0b013e3283319a1d. [ Links ]
14. Banks PA, Bollen TL, Dervenis C, Gooszen HG, Johnson CD, Sarr MG, et al. Classification of acute pancreatitis-2012: revision of the Atlanta classification and definitions by international consensus. Gut. 2013;62(1):102-11. doi: 10.1136/gutjnl-2012-302779. [ Links ]
15. Bhandari V, Jaipuria J, Singh M, Chawla AS. Intra-abdominal pressure in the early phase of severe acute pancreatitis: canary in a coal mine? Results from a rigorous validation protocol. Gut Liver. 2013;7:731-8. doi: 10.5009/gnl.2013.7.6.731. [ Links ]
Received: October 24, 2017; Accepted: June 05, 2018











 texto en
texto en 


