Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Revista de la Universidad Industrial de Santander. Salud
Print version ISSN 0121-0807
Rev. Univ. Ind. Santander. Salud vol.44 no.2 Bucaramanga May/Aug.. 2012
Internal antecubital fold line: A new
useful anatomical repair to identify the
medial epicondyle and avoid iatrogenic
ulnar nerve injury in patients with
supracondylar fracture of the humerus
Luis José Cespedes1, Camilo Turriago2, Jairo Goyeneche1
1. Pediatric Orthopaedic Surgeon. Centro Médico Carlos Ardila Lülle. Bucaramanga.
2. Pediatric Orthopaedic Surgeon. Hospital Infantil de San José de Bogotá.
Correspondencia: Luis José Céspedes. M.D, ljcespedes@intercable.net.co, Centro Médico Carlos Ardila Lülle, Torre A, Módulo 33.
Tel (7) 6383422, Fax: (7) 6384160, Bucaramanga, Colombia.
Recibido: 23 de Mayo de 2012 Aceptado: 16 de Julio de 2012
ABSTRACT
Introduction: The supracondylar fracture of the distal humerus is the most common pediatric fracture around the elbow. The currently accepted techniques of fixation are two lateral parallel wires , crosswiring technique from the lateral side, two divergent wires laterally and two retrograde crossed wires. The retrograde crossed wires provide the best mechanical stability. Many children with this fracture have swelling around the elbow, making difficult the feeling of the anatomic landmarks for percutaneous pinning, increasing the risk of ulnar nerve injury. Objective: To evaluate the correspondence of the internal antecubital fold line with the internal epicondyle in patients with supracondylar fracture and the incidence of iatrogenic ulnar nerve injuries . Methods: We conducted a series of clinical cases. In the first group we included 56 children with supracondylar fracture Gartland type III, from August 2000 to September 2007, who underwent closed reduction and crossed retrograde nail fixation. In the second group we included 241 (481 elbows) outpatients with no anatomic abnormality. We used the extension of antecubital fold line to find the internal epicondyle in both groups. Results: The prolongation of the antecubital fold line intersected the medial epicondyle in all participants of the first group. In 96.3% of the participants in the second group, the extension of antecubital fold line intersected the internal epicondyle. None patient had iatrogenic ulnar nerve injury. Conclusions: The use of the antecubital internal fold line may be useful to identify the internal epicondyle and thus avoid iatrogenic ulnar nerve injury. Salud UIS 2012; 44 (2): 9-14
Keywords: Supracondylar humerus fractures, internal antecubital fold line, iatrogenic ,nerve injury.
Línea del pliegue antecubital interno: Un nuevo reparo anatómico
útil para identificar la epitróclea y evitar lesiones iatrogénicas del
nervio ulnar en pacientes con fractura supracondílea del humero
RESUMEN
La fractura supracondílea del húmero distal es la más común alrededor del codo en niños. Las técnicas actualmente aceptadas de fijación son dos clavos laterales paralelos, dos clavos cruzados laterales, dos clavos laterales divergentes y dos clavos retrógrados cruzados. Los clavos retrógrados cruzados, proporcionan la mejor estabilidad mecánica. La mayoría de los niños con fractura supracondílea presentan inflamación alrededor del codo, haciendo difícil la palpación de la epítroclea, aumentando el riesgo de lesión del nervio cubital. Objetivo: evaluar la correspondencia de la línea del pliegue antecubital interno con la epitróclea en pacientes con fractura supracondílea y la incidencia de las lesiones iatrogénicas del nervio cubital. Metodología: Realizamos una serie de casos clínicos. El primer grupo incluyó 56 niños con fractura supracondílea tipo III de Gartland, entre agosto de 2000 a septiembre de 2007, tratados con reducción cerrada y fijación con clavos cruzados retrógrados. El segundo grupo incluyó 241 (481 codos) pacientes de consulta externa. En ambos grupos utilizamos la línea antecubital interna para identificar la epitróclea. Resultados: La prolongación de la línea del pliegue antecubital intersecó la epitróclea en todos los participantes del primer grupo. No hubo lesión iatrogénica del nervio cubital. En el segundo grupo la línea del pliegue antecubital intersecó la epitróclea en el 96.3% de los pacientes. Ningún paciente presentó lesión del nervio cubital. Conclusiones: La extensión de la línea de pliegue antecubital interno puede ser útil para la identificación de la epitróclea y así evitar lesiones iatrogénicas del nervio cubital. Salud UIS 2012; 44 (2): 9-14
Palabras Clave: Fracturas supracondíleas de húmero, Línea antecubital interna, Lesión iatrogénica del Nervio ulnar.
INTRODUCTION
Supracondylar fractures are very common in children, account for 60% of fractures around the elbow. They occur mostly in children between 5 and 10 years, due to lower relative thickness of this zone and ligamentous laxity, characteristic of the age that allows hyperextension of the elbow. They are classified into three types according to Gartland: Type I: nondisplaced, Type II: angled with intact posterior cortex, and Type III: with a full displacement.1
There are different options for fixing these fractures: external parallel nails, side cross-nails, cross-wiring technique performed from the lateral side (Dorgan's technique) nails crossed retrograde via the internal and external. The setting that provides the best stability, with less risk of loss of reduction and residual deformity, is what is done with crossed retrograde nails , but with more risk of producing iatrogenic ulnar nerve injury, compared with lateral nail fixation; complication that is especially associated with the presence of edema characteristic of these fractures.2-9 Some authors, based on biomechanical tests suggest that the lateral retrograde divergent nail fixation provides good stability but when non anatomic reduction is achieved, they recommend the use of an internal pin.10
The incidence of iatrogenic ulnar nerve injury is about 2% to 6%. Although most injuries are classified as type neuropraxia and resolved by removing the locking pin, is a matter of concern to the surgeon and the family, because in some cases, the injury may be permanent11-13.
One option described to identify the ulnar nerve and avoid injury when performing fracture reduction is the use of a peripheral nerve stimulator, but their usefulness is limited because this equipment is not available in all medical centers. Another strategy used with good results, is conducting a mini-incision over the medial epicondyle to avoid ulnar nerve injury, however this involves making a surgical incision. 14,15
In the literature we did not found surface landmarks to identify the medial epicondyle in order to facilitate the fixation of supracondylar humeral fractures. In this study, and as a result of our clinical observation, we describe the use and results of the prolongation of the antecubital fold line, as a surface landmark to identify the internal epicondyle and thus choose a safe entry point preventing dangerous inputs with risk of ulnar nerve injury.
MATERIAL AND METHODS
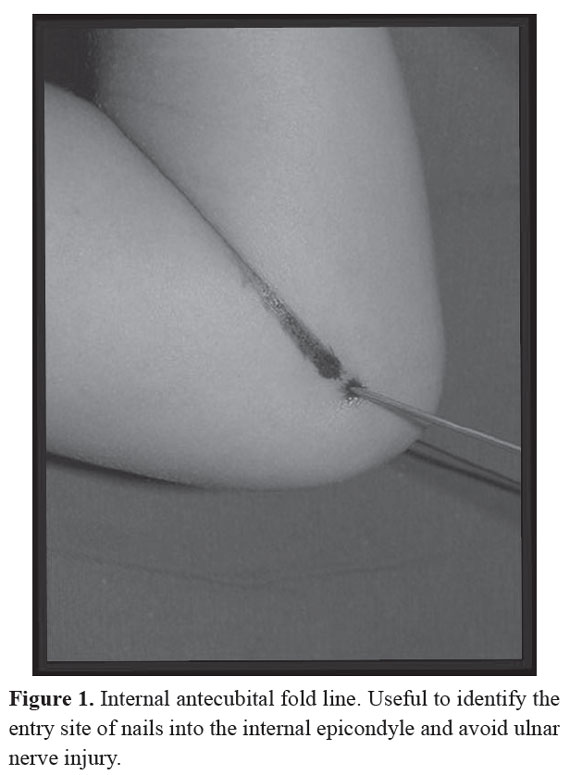
We conducted a descriptive study of clinical case series. The study population consisted of patients with humeral supracondylar fracture Gartland III treated in the emergency department of the Carlos Ardila Lülle clinic, Bucaramanga, Colombia, Southamerica, in the period between August 2000 and September 2006. The inclusion criterion was established for absence of anatomical abnormality of the elbow prior to fracture. We excluded patients with neurological disorders, bone dysplasias, history of infection or fracture in the elbow committed and syndromes associated with musculoskeletal disorders. The senior author performed in all patients retrograde crossed nail fixation, using the distal extension of the antecubital fold line for the identification of the internal epicondyle. The first step was to perform closed reduction and verification of complete reduction with the use of fluoroscopy. With a metal ruler and methylene blue, he drew a line extending the antecubital fold, which intersected the internal epicondyle in all cases, then by palpation he chose the entry site of nails as shown in Figure 1.
In the second group, using the described technique, two pediatric orthopedic surgeons evaluated the extent of internal antecubital fold line in 241 patients with no anatomic abnormality of the elbow (481 elbows), and that met the inclusion and exclusion criteria.
We performed characterization of the study population taking into account variables such as age, sex, elbow evaluated (left or right), matching the line with the medial epicondyle, preoperative and postoperative nerve injury, using measures of central tendency and dispersion, according with the nature and distribution of the variables of interest.
RESULTS
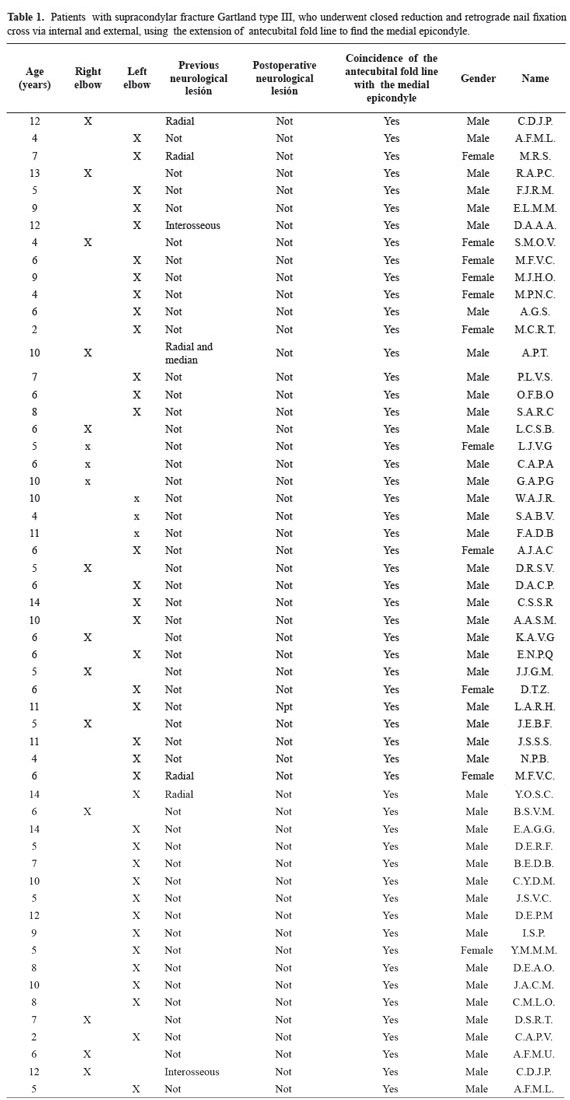
In total, 56 patients with type III fracture Gardland, 80.4% male, with an average age of 7.3 ± 3.3 years (minimum 2 and maximum of 16). 71% of patients (n = 40) had fracture in his left elbow, 12.5% (n = 7) patients had nerve injury prior to the surgical procedure(radial nerve, interosseous nerve , median nerve). In all patients, the extension of antecubital fold line intersected the internal epicondyle. None patient had iatrogenic ulnar nerve injury (Table 1).
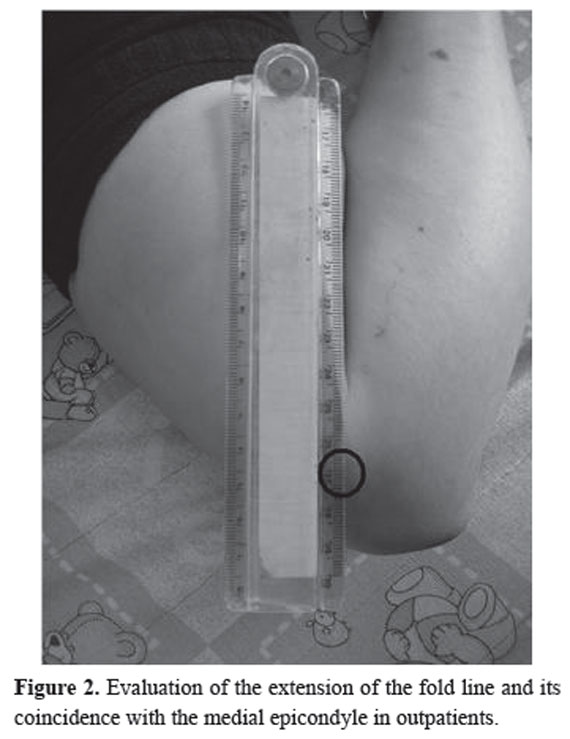
In the second group we included 241 (481 elbows) children with no anatomic abnormality of the elbow, 53.8% were female, with an average age of 6.16 ± 3.2 years (minimum 1, maximum 15). In 96.3% of the participants, the extension of antecubital fold line intersected the medial epicondyle. Figure 2.
DISCUSSION
The currently accepted techniques to make fixation in supracondylar fractures in children are two parallel wires inserted through the lateral condyle across the fracture, cross-wiring technique performed from the lateral side, two divergent wires inserted laterally, two crossed nails, one inserted laterally and one through the medial condyle. The nails crossed, provide the best mechanical stability. The pin that is inserted through medial epicondyle carries a risk of injury to the ulnar nerve. The iatrogenic injuries of the ulnar nerve after closed reduction and percutaneous fixation, produce temporary disability and could be a matter of concern because in some cases the sequelae could be permanent.
The location of the internal epicondyle could be facilitated if there is onen anatomical landmark. According to our clinical experience reported in this study, one line extended from the internal antecubital fold, intersects the medial epicondyle in any degree of flexion, both in patients with supracondylar fractures of the humerus and children without any anatomical abnormality of the elbow. Although, the actual trend is to use lateral wires to avoid ulnar nerve injury, in fractures with medial comminution, oblique fractures, and more proximal fractures, is necessary make an internal fixation to achieve an stable fixation16. In this cases, the internal antecubital fold line could be useful to locate the internal epicondyle. Using this technique, none of the 56 patients who underwent cross retrograde nail fixation and reported in this study presented ulnar nerve injury.
The authors recommend the use of this simple strategy to identificate the internal epicondyle, which facilitate the surgical technique and also is particularly useful to prevent ulnar nerve injury, when we used crossed retrograde nails to stabilize supracondylar humerus fractures. We do not pretend that this review will replace the strategies recommended in the literature to avoid iatrogenic ulnar nerve injuries, however, we want to show another useful way to avoid this injury in the treatment of supracondylar fractures.
ETHICS CONSIDERATIONS
All patients were informed about the procedure that was perfomed. I want to thanks the co-authors for their help making this paper. There are not economic sponsors to make this article.
REFERENCES
1. Kasser JR, Beaty JH. Rockwood and Wilkins' fractures in children. Supracondylar fractures of the distal humerus. 6 edition. Philadelphia, USA: Lippincott Williams & Wilkins, 2006 p. 577-624. [ Links ]
2. Brauer CA, Minsuk BL, Bae DS, Waters PM, Mininder S Kocher. A Systematic Review of Medial and Lateral Entry Pinning Versus Lateral Entry Pinning for supracondylar Fractures of the Humerus. J Pediatr Orthop 2007;27:181-186 [ Links ]
3. Shannon FJ, Mohan P, Chacko J, D'Souza LG. "Dorgan's" Percutaneous Lateral Cross-Wiring of Supracondylar Fractures of the Humerus in Children. J Pediatr Orthop. 2004; 24:376-379. [ Links ]
4. Zeni M, Ramachandran M, Milne B, Little D, Smith N. Intraoperative Stability Testing of Lateral- Entry Pin Fixation of Pediatric Fractures Humeral supracondylar. J Pediatr Orthop. 2007; 27:695-702. [ Links ]
5. Larson L, Firoozbakhsh K, Passarelli R, Bosch P. Biomechanical Analysis of Pinning Techniques for Pediatric supracondylar Humerus Fractures. J Pediatr Orthop 2006; 26:573-578 [ Links ]
6. Amre H, Poitras P, Louati Hakim. Simon Dagenais. Masquijo July Javier. Ken Kontio. Biomechanical Analysis of Lateral Pin Placements for Pediatric supracondylar Humerus Fractures. J Pediatr Orthop. 2010; 30:135-139. [ Links ]
7. Bloom T, Robertson C, Mahar AT. Newton P. Biomechanical Analysis of supracondylar Humerus Fracture Pinning for Slightly Malreduced Fractures. J Pediatr Orthop. 2008; 28:766-772. [ Links ]
8. Lee SS, Mahar AT, Mieses D, Newton PO. Displaced supracondylar Pediatric Humerus Fractures: Biomechanical Analysis of Percutaneous Pinning Techniques. J Pediatr Ortho. 2002; 22:440-443. [ Links ]
9. Gordon AT, Patton CM, Luhmann SJ, Bassett GS, Schoenecker PL. Fracture Stability After Pinning of Displaced Distal Humerus supracondylar Fractures in Children. Journal of Pediatric Orthopaedics. 2001; 21:313-318. [ Links ]
10. Gottschalk HP, Sagoo D, Glaser D. Doan J, Edmonds EW, Schlechter J. Biomechanical Analysis of Pin Placement for Pediatric Supracondylar Humerus Fractures: Does Starting Point, Pin Size, and Number Matter? J Pediatr Orthop. 2012; 32: 445-451 [ Links ]
11. Lyons, JP, Ashley E, Hoffer MM. Ulnar Nerve palsy After Percutaneous Cross-Pinning of supracondylar Fractures in Children's Elbows. J. Pediatr Orthop. 1998; 18: 43-45. [ Links ]
12. Ponce BA, Hedequist DJ, Zurakowski D, Atkinson CC, Waters PM. Complications and Timing of Follow-up After Closed Reduction and Percutaneous Pinning of Fractures Humerus supracondylar Follow-up After Percutaneous Pinning Fractures of Humerus supracondylar. J Pediatr Orthop. 2004; 24:610-614. [ Links ]
13. Babal JC, Mehlman CT, Klein G. Nerve Injuries Associated Pediatric supracondylar With Humeral Fractures: A Meta-analysis. J Pediatr Orthop. 2010; 30: 253 - 263. [ Links ]
14. Wind WM, Schwend RM, Armstrong DG. Predicting Ulnar Nerve Location in Pinning of supracondylar Humerus Fractures. J Pediatr Orthop. 2002; 22:444-447. [ Links ]
15. Ramachandran M, Birch R, Eastwood DM. Clinical outcome of nerve Associated Injuries with supracondylar fractures of the humerus in children. J Bone Joint Surg [Br]. 2006; 88-B: 90-94. [ Links ]
16. Edmonds EW, Roocroft JH, Mubarak SJ. Treatment of Displaced Pediatric Supracondylar Humerus Fracture Patterns Requiring Medial Fixation: A Reliable and Safer Cross-pinning Technique. J Pediatr Orthop. 2012; 32:346-351. [ Links ]