INTRODUCTION
The main cause for the development of gingivitis in children is bacterial plaque, with clinical characteristics like gingival bleeding and changes in color, consistency, and surface texture of the gingiva.1 The severity of gingivitis is often related to plaque accumulation, which has been shown to vary with age.2 The most important local predisposing factor in children is poor oral hygiene.3 Other factors affecting the intensity and severity of gingivitis in children are of immunological, microbiological, and anatomical nature. Gingivitis develops in individuals after 7 to 21 days with no plaque removal, providing strong evidence to recommend teeth brushing at least once a day.2 Good oral hygiene is an important factor in maintaining optimal oral health.4
Gingivitis can be prevented by controlling bacterial plaque, by brushing teeth with the support of parents or guardians and visits to the dentist.5-7. In the absence of plaque control, there is a higher risk of suffering associated pathologies, and there might be complications once they appear.8 Many factors influence the adequate hygiene in patients, such as the parents’ socioeconomic status,9 their educational level, and the time devoted to their children due to occupations. The reviewed studies show that gingivitis prevalence is higher than 60%, related to bacterial plaque and age, with no gender preferences.10,11
In the first years of life, kids acquire healthy habits essential for personal life and relationships with others, like adequate nutrition, hygiene and personal order, and social coexistence. Therefore, preventive programs in these years are essential to children’s health.12
Since the year 2010, the State of Valle del Cauca (Colombia) has included in its oral health baseline the registration of caries, gingivitis, and bacterial plaque of users of the public health network. However, it is necessary to provide information on oral hygiene and the gingival health status of children from community homes in the state, as well as factors that may be related to gingivitis and its prevalence.
In consequence, the objective of this study was to evaluate the prevalence of gingivitis in preschoolers from community homes in 6 municipalities of Valle del Cauca and its associated factors.
METHODS
This was an analytical cross-sectional study in 982 children aged 2 to 5 years from community homes located in Florida, Pradera, Palmira, Yumbo, Jamundí, and Cali, as part of the baseline “Oral Health 2011, Project 0526 - Cartago Hospital”. The homes were selected by simple random sampling from a list of 31 homes. To run contract 0526 of 2010 between Cartago Hospital and the State Secretariat of Health, the project was approved by the Ethics Committee of Cartago Hospital, according to Affidavit # 010 of September 30th, 2010. The objectives of the study were explained to the mothers of the community homes and they were asked to provide an informed consent where parents authorized the participation of their children in the construction of this baseline; parents were told that the data and results of the study would be strictly confidential. Children with systemic medical conditions (leukemia, cancer, respiratory infections, and the like) or acute lesions in the oral cavity (like abscesses, dental pain, or herpes) were not included.
Community plaque index (CPI) and clinical evaluation of gingival inflammation were used to determine gingivitis. For caries assessment, the researchers used the clinical instrument provided by the Ministry of Health for baseline construction,13 used in the IV Estudio Nacional de Salud Bucal [IV National Survey on Oral Health]14 as caries experience, which refers to the proportion of people who, at the time of examination, showed evidence of having suffered caries (in either early or advanced stages), or its sequelae (filled or missing teeth due to caries) at some point in their lives. In reporting caries experience, the antecedents were recorded considering the number of teeth with advanced caries, as well as filled or missing teeth, and according to the kids’ age and deciduous dentition (def index).
Standardization was carried out in two phases: a theoretical phase in which the examiners were trained in clinical diagnosis and entering data on the forms provided, solving questions concerning evaluation criteria and the conditions required for the examination. The second phase was a practical session, in which the examiners and the study director took turns to evaluate five children. The degree of intra- and inter-examiner agreement was then assessed. The standardization yielded an 8% inter-examiner discrepancy for diagnosis of gingivitis, 9% for CPI and 10% for caries, among the five dental examiners. In CPI standardization,15 the concordance with Kappa values was 0.80. Entering bacterial plaque information on the appropriate forms was the last clinical examination activity and patients were asked to mouthwash using a disclosing solution for 30 seconds; the teeth surfaces were then observed as instructed for community plaque index.
The preschoolers’ socio-demographic variables included in the form filled by the examiners were age, population group, type of social security, sex, and geographical area; in addition, it explored the community mothers’ knowledge in oral health. Variables with p value less than 0.05 in the bivariate analysis were considered factors associated with gingivitis.
The univariate statistical analysis involved evaluation of frequencies and measures of central tendency. For statistical analysis of the analytical variables, bacterial plaque indices lower than or equal to 25% were considered acceptable CPI. The exploratory statistical analysis used the sociodemographic variables (with a p value < 0.05), which were correlated to the bacterial plaque level, in order to suggest hypotheses related to the main result, using the chi squared test for the bivariate analysis, and logistic regression for the multivariate analysis through version 18 of the SPSS software.
RESULTS
This study assessed 982 children from 11 community houses in six municipalities of Valle del Cauca during the year 2010-2011. Of the total study population, 55.7% were male and most were 3 to 4 years old. Regarding social security, the highest percentage was covered by the contributory system, with 51.2%, followed by the subsidized system, with 36.6%. Concerning population groups, 62% of mothers did not identify the kids with any ethnicity, while 30.4% were considered mestizo, 7.0% Afro-Colombian and 0.5% indigenous.
This study found that 30.8% of the assessed population had gingivitis (32.4% boys and 28.7% girls, without significant differences). The prevalence of gingivitis was higher in the following situations: Afro-descendant preschoolers, those who had a bacterial plaque level greater than 25%, the ones who lived in rural areas, those covered by the contributory or special systems, and the ones who were under the supervision of a community mother with little knowledge on oral health (Table 1).
Table 1 Factors associated with gingivitis in preschoolers from community homes in 6 municipalities. Oral Health Baseline, Valle del Cauca (Colombia), 2012
| Associated factors | Gingivitis (%) | Unadjusted OR | Adjusted OR | |||
|---|---|---|---|---|---|---|
| Yes | Value | CI95% | Value | CI95% | ||
| Afro-descendant | 75.4 | 8.1 | 4.6-14.3* | 3.6 | 1.6-8.1* | |
| Rest of population | 27.4 | 1.0 | - | 1.0 | - | |
| Bacterial plaque ≤ 25% | 1.4 | 1.0 | - | 1.0 | - | |
| Bacterial plaque > 25% | 35.5 | 17.0 | 9.2-152* | 62.5 | 14.1-250.0* | |
| Jamundí resident | 67.5 | 6.8 | 4.8-9.8* | N.S. | - | |
| Resident in other municipalities | 23.1 | 1.0 | - | |||
| Rural resident | 80.4 | 10.5 | 5.2-21.3* | N.S. | - | |
| Urban resident | 28.0 | 1.0 | - | |||
| Contributory or special system | 34.2 | 1.4 | 1.1-1.9* | 2.4 | 1.7-3.5* | |
| Subsidized system and uninsured poor population | 27.0 | 1.0 | - | |||
| Community mothers’ acceptable knowledge on oral health | 25.0 | 2.9 | 2.1-3.9* | N.S. | - | |
| Community mothers’ inadequate knowledge on oral health | 49.4 | 1.0 | - | - | - | |
| High caries level (def > 2) | 54.2 | 4.7 | 3.5-6.3 | 4.3 | 3.1-6.2* | |
| Low caries level (def ≤ 2) | 20.0 | 1.0 | - | 1.0 | - | |
* p < 0.01; variables included: rural area vs urban area, municipality of Jamundí vs. other municipalities, community mothers’ knowledge on oral health promotion, age 2-3 years vs. 4-5 years, acceptable CPI contributory system vs. other types of coverage, Afro-descendant population vs. other populations, sex (N. S.: not significant)
A bacterial plaque score of 41.3% (CI95% 40.4-42.5) was found. A score of 2.2% of plaque was considered acceptable (Figure 1) and plaque scores higher than 25% were found in preschoolers from rural areas, in those who were covered by the contributory or special system and in those who had a high level of decayed, missing and filled teeth (DMF, and def for deciduous dentition) (Table 2). The level of oral hygiene did not show significant differences with sex, ethnicity, age, or dental malocclusions, nor with the community mothers’ health knowledge.
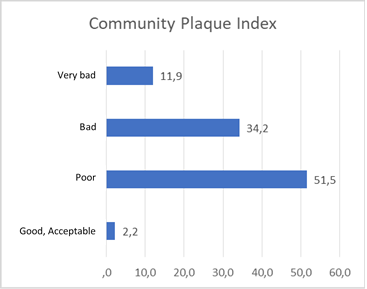
Figure 1 Community plaque index of evaluated preschoolers from community houses in 6 municipalities. Oral Health Baseline, Valle del Cauca (Colombia), 2012
Table 2 Factors associated with bacterial plaque in preschoolers from community homes in 6 municipalities. Oral Health Baseline, Valle del Cauca (Colombia), 2012
| Associated factors | Bacterial plaque | Unadjusted OR | Adjusted OR | |||
|---|---|---|---|---|---|---|
| > 25% | Value | CI95% | Value | CI95% | ||
| Rural resident | 96.1 | 4.1 | 1.0-17.5** | 5.8 | 1.3-26,8** | |
| Urban resident | 85.4 | 1.0 | - | 1.0 | - | |
| Contributory or special system | 90.0 | 1.9 | 1.3-2.8* | N.S** | - | |
| Subsidized system and poor uninsured population | 82.2 | 1.0 | - | - | - | |
| High caries level (def > 2) | 98.7 | 18.8 | 6.9-51.4 | 19.8 | 7.2-54.7 | |
| Low caries level (def ≤ 2) | 80.1 | 1.0 | - | 1.0 | - | |
| Jamundí resident | 81.7 | 1.4 | 0.96-2.0 ** | 6.9 | 1.9-24.6* | |
| Resident in other municipalities | 86.8 | 1.0 | - | 1.0 | - | |
* p < 0.01; ** p > 0.05. Variables included: community mothers’ knowledge on oral health, rural vs urban population, sex, age 2-3 years vs. 4-5 years, caries level, residents of Jamundí vs other municipalities, Afro-descendant population vs other populations, social security coverage (contributory system) vs. poor population (subsidized system and uninsured population)
In exploring possible associations in search of hypotheses about the factors most likely related to the presence of gingivitis, it was found that belonging to a given ethnic group (like the Afro-descendant), having poor oral hygiene, being covered by the contributory system, and having a high level of caries experience are related to a greater likelihood of having gingivitis (Table 1). It was also observed that the odds ratio (OR) for bacterial plaque increases while the OR for ethnicity decreases when the model includes other sociodemographic variables, such as place of residence, type of social security, and community mothers’ knowledge on oral health (Table 1). In evaluating which factors are related to higher levels of bacterial plaque, it was found that the variables that most affect OR were the place of residence and the caries level measured by DMF index (Table 2).
The place of residence was associated to oral hygiene by the multivariate analysis but not by the bivariate one. When relationships are stratified, it can be observed that belonging to the subsidized system and residing in Jamundí increase poor hygiene (OR = 2.3; CI95% 1.3-3.9). The Afro-descendant population from the municipality of Jamundí showed a higher percentage of poor hygiene compared to the Afro-descendant population from other municipalities (OR = 6.8; CI95% 1.2-40.0). The Afro-descendant population of the subsidized system had better oral hygiene than the Afro-descendant population of the contributory system, but these differences were not significant; it was also found that 75.9% of Afro-descendants from Jamundí were covered by the contributory system.
DISCUSSION
This study measured the presence of bacterial plaque as an indicator of oral hygiene in a sample of preschoolers, in relation to the presence of gingivitis-a disease characterized by inflammatory changes in shape, size, color, and consistency of the gingiva, with no pain at probing. The absence of pain may be one of the reasons why this pathology is not usually consulted in health services. This is the first published study from the Oral Health Baseline for Valle del Cauca aiming to describe the situation of gingivitis associated with bacterial plaque in preschoolers from community homes in six municipalities, finding out a plaque index similar to that reported in the National Oral Health Survey (ENSAB III),16 in which the soft plaque index at the age of 5 was 43.3%. The present study found a similar result to a study conducted in the city Medellín, which found an index of 45.3% in children aged 3 to 5 years.17
The statistical analysis shows that, the better the child’s oral hygiene and the better the community mothers’ knowledge on oral health, the lower the prevalence of gingivitis, agreeing with findings by recent studies.2,7,11,18 The presence of gingivitis in one third of the study population was similar to that reported in other studies.19,20 Therefore, it should be taken into account when analyzing the effectiveness of educational programs aimed at improving oral hygiene as a risk factor.
The prevalence of gingivitis was higher in the population covered by the contributory system (who usually have better purchasing power) than those covered by the subsidized system and the uninsured poor population. This situation is not consistent with the findings showing that children of better socioeconomic levels have better gingival health conditions,9,19,21 but it may indicate that, despite having better socioeconomic conditions than the subsidized population, the parents or guardians fail to bring preschool-age children to the dental services offered by the insurance system, and may also point to other sociocultural factors influencing the attendance to growth and development programs.22
The high prevalence of gingivitis in the Afro-descendant population may be related to other social factors influencing health care access, as reported by studies that associate social variables (such as ethnicity and type of health insurance) with access to prenatal control and dental care services,23,24 as well as ethnicity with habits, like good oral health practices, positive health beliefs, and adequate oral health knowledge.25
If bacterial plaque index is considered the most relevant factor in children with gingivitis and considering that 97.8% had poor to bad oral hygiene (Figure 1), it follows that all preschoolers are at risk of suffering from gingivitis. This clinically significant risk was found by Taboada and Talavera in their study.26 The factors associated with a bacterial plaque index greater than 25% in preschoolers from the studied community houses were place of residence, type of insurance, and a high level of caries, measured with a caries experience index greater than 2, which shows that the determinants of oral hygiene are not only biological but also social factors. The high indexes of bacterial plaque that have been found at early ages should lead those responsible for the health insurance administration, governmental and non-governmental bodies, health-care providers, and educators of oral health professionals to strengthen health promotion actions involving caregivers (parents, family members, community mothers, teachers, etc.), promoting the acquisition of healthy habits, such as good oral hygiene in the early stages of life, and fostering learning processes to help control risk factors, as recommended by other studies.27
The present study found that gingivitis prevalence is not related to age, disagreeing with the findings by Rocha et al,11 but in agreement with other reports claiming that there is not a relationship with preschoolers’ gender.10,11
One limitation of the present study is the number of assessed community homes, as not all the community homes in the region were included, and therefore it was not possible to stratify by municipality. In addition, information related to close caregivers’ knowledge in oral health was obtained only from community mothers instead of parents. In our opinion, one strength is that the study design helped explore associations of social factors with biological aspects like gingivitis in preschoolers and formulate hypotheses to guide decision makers in oral health policies.
This study concludes that gingivitis prevalence is high, and the exploration of associated factors suggests the hypothesis that there is a greater likelihood of gingivitis according to ethnicity, as shown by the results of the Afro-descendant population. Other associated factors are: having poor oral hygiene, the type of social security coverage and the level of community mothers’ knowledge on oral health.
Considering the importance of hygiene (measured by bacterial plaque index) and secondary findings, which suggest that plaque increases according to caries level, it is recommended to improve the health services response to preschoolers’ oral problems.
Strategies should be sought to assess the effectiveness of programs offered by health insurers and their network of providers to control preventable risk factors like bacterial plaque, which is a common risk factor for both caries and problems affecting the gingiva. Health policy makers should consider the unequal distribution of gingivitis in population groups and include the children’s caregivers, like parents and community mothers, so that they play a more active role in monitoring and controlling risks, through easy-to-achieve strategies, such as improving oral hygiene. It is also important to implement programs aimed at parents, in order to improve the hygienic and dietary habits of families.
Social vulnerability of early childhood is also observed in the evaluated community homes; therefore, the authors recommend to carefully exploring the determinants affecting children’s oral health care.











 text in
text in 


