INTRODUCTION
Barodontalgia is a rare dental pain caused by differences in barometric pressure on teeth during flights. This condition is characterized by an acute and/or throbbing pain as the aircraft ascends or descends. This phenomenon may occur in case of dental cavity, defective restoration, pulpitis, pulp necrosis, apical periodontitis, periodontal pockets, impacted teeth, root fracture, and residual cysts.1,2 A generally accepted classification of barodontalgia was developed by Ferjentsik and Aker (1982)3 and is primarily based on the underlying causes and clinical symptoms (Table 1).
Table 1 Barodontalgia classification by causes and symptoms.
| Class | Cause | Pain |
| I | Irreversible pulpitis | Sharp pain during ascent |
| II | Reversible pulpitis | Dull throbbing pain during ascent |
| III | Necrotic pulp | Dull throbbing pain during descent |
| IV | Periradicular pathology | Severe and persistent pain during both ascent and descent |
Military aviators, especially fighter pilots, who perform flights constantly alternating acceleration and atmospheric pressure, are the most susceptible to this phenomenon, and therefore maintaining dental health is important for them. Proper oral health reduces the occurrence of barodontalgia, since diseases such as dental cavity, apical periodontitis, root fracture, residual cysts, pulpitis, pulp necrosis and defective restoration are related to this etiology.2-6
Previous studies have documented the difficulty in obtaining a definitive diagnosis of barodontalgia.7 Flight-related toothaches must be carefully analyzed from a clinical and radiographic point of view, since barodontalgia presents facial barotrauma (related to facial cavities), barotitis media (traumatic inflammation of the middle ear area), barotitis externa (by the tympanic membrane’s external auditory canal mucosal lining), and barosinusitis (inflammation of one or more paranasal sinuses) as differential diagnoses.8
Even though planes are currently provided with pressurized cabins, that can help reduce pressure variations on the human system, quick ascents, such as in helicopters, may cause sudden sharp systemic circulatory changes that may be difficult for physiological mechanisms to balance, leading to barodontalgia in crew or passengers.9
Commercial aviation is a widely used means of transportation, and the knowledge of barodontalgia by dental surgeons is greatly valued in this regard, seeking proper diagnosis and treatment. The periodic oral evaluation of pilots is a key practice to prevent this phenomenon, as well as aircraft accidents, since this condition can lead to vertigo and physical disability and, consequently, to premature termination of flights. Both pilots and crew members must maintain preventive habits against dental diseases, in order to ensure flights within the normal standards, eliminating the possibility of being affected by barodontalgia.8
Preventive treatment includes periodic assessments and restorative treatment of decayed teeth, removal of defective restorations, and elimination of the causes of dental inflammation. Conclusive treatments should be performed, and direct pulp capping is not recommended, due to complications in the pulp regeneration process caused by atmospheric pressure variations.2,5,6
Further research is needed to demonstrate the incidence of barodontalgia, highlighting the importance of flying smooth flights and motivating all aircrew members to maintain perfect oral health. In this context, this article presents a clinical case report of an aircrew member assisted at the Santos Dumont Air Force Dental Clinic, who reported the occurrence of in-flight barodontalgia.
CASE REPORT
Patient M.J.M.F., a Brazilian Air Force Aviator Brigadier, aged 56, arrived at the Endodontics Department of the Santos Dumont Air Force Dental Clinic (OASD), Rio de Janeiro, complaining of intense sharp pain in the maxillary region while flying a C-95 Bandeirante Brazilian Air Force aircraft; the pain persisted while on the ground for some minutes. Immediately after landing, the patient went to the OASD in order to look into the strange incident. During the clinical examination, the military reported a dental trauma that occurred in the anterior region when he was about 30 years old. No tooth fractures, tooth decay or defective restorations were observed. The radiographic examinations showed an extensive periradicular lesion associated with tooth 12, and due to its size, the suggestive diagnostic was periradicular cyst (Figure 1).
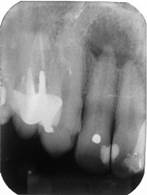
Figure 1 Representative periradicular radiograph of tooth 12 displaying an extensive periradicular lesion.
In order to confirm pulp necrosis, a sensitivity test was carried out and, upon confirmation, conventional endodontic treatment was indicated. During the first session, conventional access cavity and necropulpectomy were performed, as well as root canal preparation with a size R25 (#25.08 Reciproc VDW, Munich, Germany) endodontic instrument in reciprocating motion powered with an electric motor (Reciproc Silver VDW, Munich, Germany) using sodium hypochlorite as irrigation (Fórmula & Ação, São Paulo, Brazil). The intracanal dressing with calcium hydroxide-based paste (Calen + PMCC - camphorated parachlorophenol - SS White, Rio de Janeiro, Brazil) was applied for 30 days using a special syringe (Duflex - SS White, Rio de Janeiro, Brazil) and 27-gauge needle (Injecta Produtos Odontológicos, São Bernardo do Campo, Brazil). The temporary restoration was placed (Coltosol, Vigodent, Bonsucesso, Brazil) and, after the procedure, a periradicular radiograph was taken to confirm the proper dressing (Figure 2). During the inter-appointment period, the patient was instructed not to practice aerial activities or travel by plane, in order to prevent the possible recurrence of pain in the region.
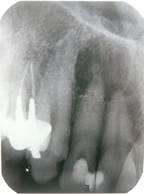
Figure 2 Representative periradicular radiograph of tooth 12, to evidence the total filling of the canal with Calen + PMCC.
On the follow up appointment after 30 days, the dressing was removed using sodium hypochlorite as irrigation and a size R25 instrument; as the patient was asymptomatic, the filling procedure was performed using R25 gutta-percha points (Reciproc VDW, Munich, Germany) and AH-Plus (Dentsply, Tulsa, United States) as endodontic sealer. The periradicular radiograph of tooth 12 after root canal filling is shown in Figure 3.
Considering that the patient was a military aviator, a rapid clinical resolution was required, so the apical surgery was chosen, as there was extensive damage to the maxillary bone that could cause another barodontalgia incident. The surgical procedure was done on the tooth with the root canal treatment the following day, and included the removal of the inflammatory lesion, an apicoectomy with MiniEndo Ultrasonics Unit and inserts (Kerr, Orange, United States), an apical filling with MTA (Angelus Indústria de Produtos Odontológicos, Londrina, Brazil) and placing of a bone hydroxyapatite-based graft (Alobone Poros, Osseocon Biomateriais, Rio de Janeiro, Brazil) in the surgical cavity. The representative periradicular radiograph of tooth 12 after periradicular surgery is shown in Figure 4.
In addition, the removed inflammatory lesion was submitted to histopathological examination at the Brazilian Air Force Central Hospital (HCA), which confirmed the early diagnosis of a periradicular cyst. The patient returned 12 months after surgery and no clinical or radiographic evidences of periradicular inflammatory recurrence were observed. In addition, radiographic signs of bone healing and proper graft integration were verified (Figure 5).
DISCUSSION
According to the relevant literature, irreversible pulpitis, with or without apical periodontitis, accounts for 18.5% of barodontalgia cases. Facial pain may be induced by increased atmospheric pressure of the air trapped under defective restorations, which compresses the pulpal nerve endings. When there is increased pressure in the pulp cavity, the pulp is unable to expand as the teeth walls are made of hard tissue, which can lead to ischemia, hence pain and necrosis. After pulp necrosis, the chemicals released by cell decomposition can be extruded through the apex, due to in-flight pressure variations, and trigger inflammatory and immunological processes in the periradicular area.1,2,5,8
Those processes are extremely painful and cause significant discomfort to the patient. They are even more complex in aircrew members and pilots in particular, as the safety of the flight, as well as that of the aircraft and passengers, becomes compromised.6,8 Thus, the literature recommends an extreme endodontic treatment for civil and military aircrew in case of invasion to the radicular pulp, in order to prevent subacute pulpitis or silent pulp necrosis.10-12
In the clinical case report presented herein, the patient, an Aviator Brigadier, was a passenger on an official flight in a pressurized cabin at the time of the incident. The patient reported painful symptoms during the flight, which lasted for a few minutes after landing. According to Zadik (2006),13 pain usually ceases when returning to onset level or ground atmospheric level but can last longer if caused by periradicular disease or facial barotrauma.
During the clinical examination, the pulp tissue was observed to be necrotic, probably due to the trauma suffered at an earlier time. The radiographic examination showed a large periradicular lesion that may have caused the acute pain experienced during the flight, due to the difference in atmospheric pressure.8,9 According to the literature, as an aircraft height increases, the atmospheric pressure decreases, leading to expansion of constricted air and compressing of the neural structures causing acute pain.1,2,5,14
After diagnosis, a conventional endodontic treatment was carried out using intracanal medication with a calcium hydroxide-based paste for 30 days, in order to eliminate the microorganisms that survived the chemo-mechanical preparation. To provide the patient with greater comfort and to prevent additional barodontalgia incidents, the patient was advised to suspend flying activities until completion of the endodontic treatment.1,2
As the patient was a military aviator, a rapid clinical resolution of the case was required, so the periradicular surgery procedure was chosen in order to seal the large lesion in the maxillary bone and to prevent a new incident of barodontalgia.8,9,15 The periradicular surgery was performed with a minimally invasive technique to remove the apical periodontitis and to perform a rapid regression of an apical bone lesion. In addition, the surgical cavity was filled with osteoconductive material, in order to minimize the possibility of a new barodontalgia episode by osteogenesis incentive, since the patient would not stop flying, as recommended by the literature, because this is his job.15 The tissue removed by biopsy was sent for histopathological examination at the Central Hospital of Brazil Air Force and the diagnosis was of a periradicular cyst.
The literature suggests that military aircrew are more vulnerable to the occurrence of barodontalgia due to their extreme working conditions.1-5 Therefore, a periodic assessment of the oral condition of aircrew members should be performed as a means to prevent barodontalgia incidents. For this purpose, a yearly meticulous clinical and radiographic dental examination is required, in order to attest the conditions of restorative, endodontic or surgical treatments previously performed, or to identify the need for new procedures to promote wellness of aircrew members.1,2,15,16) Periradicular and panoramic X-rays are valuable examinations during periodical assessments, as well as after one, three, six, and twelve months following the dental procedures, and in cases of extensive lesions extended over two to three years.2,5,8,17,18 In the reported case, the radiographic follow-up was performed after 12 months.











 text in
text in