INTRODUCTION
Dental occlusion refers the relationship between antagonist teeth in contact at maximum intercuspation during mandibular closure to provide functionality to the stomatognathic system.1 Any alteration of occlusion and its functional demands is related to occlusal disharmony (malocclusion), dysfunction, or disorders in motor behavior, as in the case of sleep bruxism (SB), which is considered a parafunctional activity of the mandible and is defined by the ICSD-3 (International Classification of Sleep Disorders) as a stereotyped orofacial dental movement characterized by grinding or clenching teeth, associated with micro-awakenings and accompanied by dental, muscular and articular symptoms.2 On the other hand, the most used classification in determining dental occlusion type is that of Angle, which is based on the anteroposterior relationship of the first upper and lower permanent molars and has three variants: Class I, Class II and Class III.3,4
According to Angle’s classification, the intermaxillary relationship is expected to produce an occlusal configuration with diverse contacts and, consequently, characteristic occlusal patterns in each individual. However, since Angle’s molar classification is established in static relation, it is not possible to determine how it works in dynamic conditions during sleep (disocclusion guidance, occlusal working contacts, and/or interferences in balance), which are unconsciously performed.
Various occlusal patterns can be established during mandibular dynamics based on three concepts widely known and reported in the literature: canine guidance (CG),5 group function (GF)6 and balanced uni- or bilateral occlusion (BO).7 Of these, CG and GF are considered normal in natural or restored dentitions, while BO is used in rehabilitations with full prosthesis.8 Similarly, depending on occlusal configuration, pattern of reproduction, and the frequency of contacts produced during the mandibular activity in wake and sleep, long-term consequences can arise as adaptive (physiological) or non-adaptive (pathological) response of the stomatognathic system, according to each individual’s functional occlusal demands, which, if not supported, can lead to dental and musculoskeletal anomalies.9-12
Clinical examination with articulating paper is the most used method to assess the occlusal contacts produced during the centric and eccentric movements performed in while awake. However, this test is not entirely accurate since in most cases mandibular movements are indicated by the clinician (right and left lateral protrusive movements) in a given position (according to the chair’s inclination). On the other hand, being in an unconscious state and a specific position while sleeping, the patient fails to control the mandible’s position and movements, producing contacts that can be harmful to the organism.9-11 Various occlusal wear patterns have been reported in several studies using the Bruxchecker® (BC), a tool for detecting sleep-related contacts and occlusal wear. This is a recently developed easy-to-use device that does not induce muscle activity nor interfere with normal occlusion or mandibular movement.9,11,13-15
Identifying the occlusal wear pattern (resulting from SB activity) depending on the static dental relationship (according to Angle’s classification) is highly important for the diagnosis, management, and control of occlusal function. The aim of this study was to describe the sleep-related occlusal wear pattern in adolescents aged 12 to 17 years with full permanent dentition, grouped in Angle Class I, II and III.
MATERIALS AND METHODS
Prior approval of the Institutional Committee of Research Ethics of Universidad El Bosque (Act No. 004-2015) and once an informed consent was signed, a descriptive study was conducted in 45 adolescents aged 12 to 17 years from the city of Bogotá and the surrounding Western Plains.
The sample was selected for convenience using Angle’s molar classification and visual examination. The individuals were selected and classified according to Angle’s molar relationship until there were 15 in each group (I, II and III) (Table 1). The following selection criteria were taken into account: subjects with full dentition to the second molars in occlusion and with interocclusal anterior teeth contact; patients with no systemic involvement, caries or extensive fillings, as well as no shape and size anomalies, severe dental crowding, or previous or current orthodontic treatment; patients with no current medication with psychotropic agents that could alter the central nervous system, and who during the use of BC were not under the influence of alcohol or psychoactive substances.
Table 1 Sample classification by age, according to Angle malocclusion
| n = 45 | Angle malocclusion | ||
|---|---|---|---|
| Age (years) | Class I n = 15 | Class II n = 15 | Class III n = 15 |
| 12 | 0 | 1 | 1 |
| 13 | 4 | 1 | 4 |
| 14 | 2 | 6 | 2 |
| 15 | 5 | 3 | 4 |
| 16 | 1 | 2 | 3 |
| 17 | 3 | 2 | 1 |
A Bruxchecker® mouthguard (Scheu Dental Technology, Iserlohn, Germany) was used to identify the occlusal wear pattern in sleep. This device was created and developed in Japan and consists of a 0.1 mm thick polyvinyl chloride sheet that does not interfere with normal occlusion and does not cause muscular or articular alterations. The mouthguard records occlusal patterns as wear markings in the red dye on its surface produced by dental contact; it can be easily and safely used during sleep.14,16
Each subject underwent the following protocol to obtain the BC and to identify the occlusal wear pattern during sleep:
An impression of the upper arch was made in alginate, obtaining a type III plaster working model (Orthoprofessional Dental Ltda., Bogotá, Colombia), thermomoulding two Bruxchecker® mouthguards in a Biostar machine at 230 °C for 15 seconds and 2.5 bar pressure (Scheu Dental Technology, Iserlohn, Germany). The mouthguards were trimmed 2 mm from the gingival margin and handed in to patients under the supervision of their parents, giving them instructions on how to use them for 2 nights. The mouthguards were collected, observing the presence of dental wear patterns (by reduced red dye) in both mouthguards and using articulating paper to verify the occlusal contacts at maximum intercuspation, which correspond to contacts in normal occlusion and can be produced by swallowing in sleep.
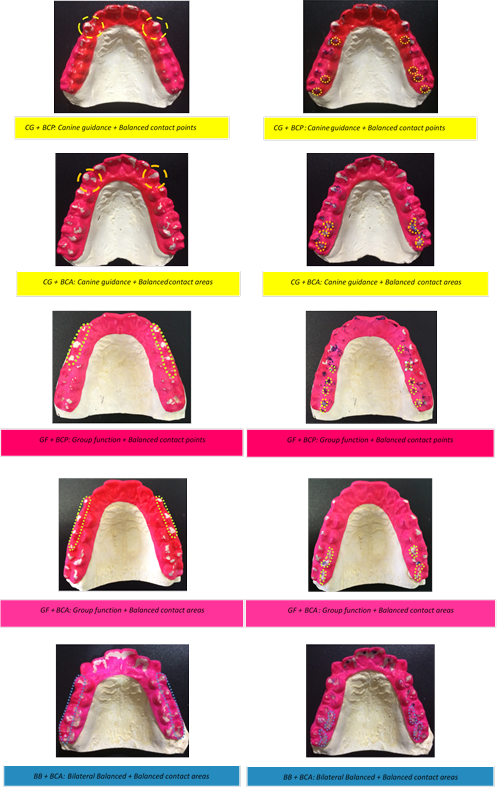
Finally, in order to determine occlusal wear pattern, the contact markings (either points or areas) resulting from mandibular dynamics in SB were identified and analyzed by visual inspection, taking into account their location and extension in the working side (WS) and balancing side (BS) (Table 2).
Table 2 Occlusal wear pattern classification per working side (WS) and balancing side (BS)
| Occlusal wear patterns | |
| WS + BS | Working side + Balancing side |
| CG + BCP | Canine guidance + Balanced contact points |
| CG + BCA | Canine guidance + Balanced contact areas |
| GF + BCP | Group function + Balanced contact points |
| GF + BCA | Group function + Balanced contact areas |
| BB + BCP | Bilateral Balanced + Balanced contact points |
| BB + BCA | Bilateral Balanced + Balanced contact areas |
On the working side, the occlusal wear pattern was classified into canine guidance (CG), group function (GF) and bilateral balanced occlusion (BB).8 On the balancing side, balanced contact points (BCP) and balanced contact areas (BCA) could be identified.
This evaluation was performed by an expert, with 0% intra-operator error (Dahlberg test). The data collected for the 3 molar classification groups were entered in an Excel® database (Microsoft Office Professional Plus 2013, Microsoft Corporation® Santa Rosa, California) and analyzed in the Minitab® 17 Statistical Software (Pennsylvania State University, USA). Exploratory data analysis and descriptive statistics were carried out by means of frequency tables and bar charts to describe the findings in the study population.
RESULTS
Once the three groups of this study were distributed according to Angle’s molar classification (n = 15 per group), the Bruxchecker® was used to determine the different occlusal wear patterns resulting from the mandibular dynamics in sleep (taking into account disocclusion guidance, occlusal working contacts, and/or interferences in balance) and classify them according to location (tooth) and extension (points or areas) of the markings observed on both the working side (laterotrusion) and balancing side (mediotrusion) (Figure 1).
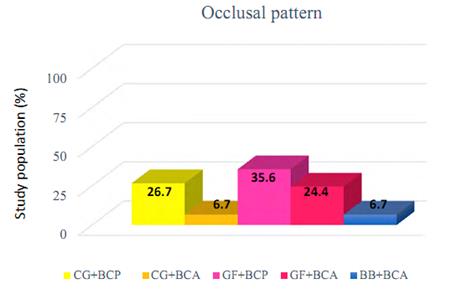
Overall occlusal wear pattern distribution in the total sample (n = 45) is shown in Figure 2. The most predominant patterns were group function (60%) with balanced contact points (GF + BCP: 35.6%) and balanced contact areas (GF + BCA: 24.4%), followed by canine guidance (33.3%) with balanced contact points (CG + BCP: 26.66%) and balanced contact areas (CG + BCA: 6.7%). Finally, there was a lower percentage of balanced bilateral occlusion with balanced contact areas (BB + BCA: 6.7%); there were no cases of bilateral balanced occlusion with balanced contact points (BB + BCP).
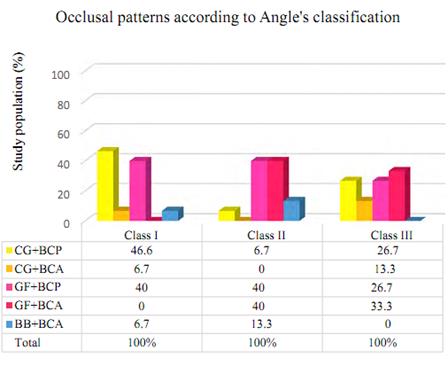
Figure 3 shows the occlusal wear pattern percentage distribution according to Angle’s molar classification. A higher prevalence of group function is generally observed in all three groups, followed by canine guidance, with predominance in Classes I and III. The balanced bilateral occlusion pattern was seen exclusively in Classes I and II and showed less frequency. The distribution of occlusal patterns in Class I shows predominance of canine guidance with balanced areas and points (CG + BCA and CG + BCP: 53.3%), followed by group function with balanced areas and points (GF + BCA and GF + BCP: 40%) and balanced bilateral occlusion with balanced contact areas (BB + BCA: 6.7%). In Class II, the predominant pattern was group function with balanced areas and points (GF + BCA and GF + BCP: 80%), followed by balanced bilateral occlusion (BB + BCA: 13.3%) and canine guidance with balanced points (CG + BCP: 6.7%). In Class III, the predominant pattern was group function with balanced contact areas and points (GF + BCA and GF + BCP: 60%), followed by canine guidance with balanced contact areas and points (CG + BCA and CG + BCP: 40%), with no presence of the balanced bilateral occlusion pattern.
Other findings of this study are related to the presence of dental arch malpositions plus overjet and overbite (horizontal and vertical), which were reported per percentage distribution in the different occlusion types (Classes I, II and III) according to Angle’s molar classification, in order to be subsequently contrasted with the occlusal wear pattern (Tables 3, 4 and 5).
Table 3 Dental malpositions in the study population distributed according to Angle’s classification
| n = 45 | ANT | ANT-MOL | ANT-PRE | ANT-PRE-MOL | N/A |
|---|---|---|---|---|---|
| Class I (15) | 33.3 | 13.3 | 13.3 | 20.0 | 20.0 |
| Class II (15) | 33.3 | 6.7 | 33.3 | 20.0 | 6.7 |
| Class III (15) | 53.3 | 0 | 33.3 | 6.7 | 6.7 |
Table 4 Arch types in the study population distributed according to Angle’s classification
| Arch type | |||
|---|---|---|---|
| n = 45 | Upper arch (%) | ||
| Square | Ovoid | Triangular | |
| Class I (15) | 20.0 | 60.0 | 20.0 |
| Class II (15) | 53.3 | 33.3 | 13.3 |
| Class III (15) | 20.0 | 46.6 | 33.3 |
| n = 45 | Lower arch (%) | ||
| Square | Ovoid | Triangular | |
| Class I (15) | 26.7 | 66.7 | 6.7 |
| Class II (15) | 26.7 | 60.0 | 13.3 |
| Class III (15) | 26.7 | 60.0 | 13.3 |
Table 5 Overjet and overbite in the study population distributed according to Angle’s classification
| Mean | Standard deviation | Minimum | Maximum | |
|---|---|---|---|---|
| n = 45 | Overbite (%) | |||
| Class I (15) | 37.5 | 15.3 | 20.0 | 60.0 |
| Class II (15) | 34.7 | 34.4 | -30.0 | 90.0 |
| Class III (15) | 24.2 | 20.8 | 0.0 | 60.0 |
| n = 45 | Overjet (mm) | |||
| Class I (15) | 2.3 | 0.8 | 1.0 | 4.0 |
| Class II (15) | 5.1 | 2.4 | 2.0 | 10.0 |
| Class III (15) | 2.4 | 1.724 | 0 | 7 |
DISCUSSION
The literature includes several studies that demonstrate the importance of dental wear patterns and allow to identify contacts or interferences originating in the mandibular dynamics in sleep, directly relating them to the activity of bruxism.2,9,11,14-17
The results of the present study are consistent with those of Panek et al18 in 2008, who performed a clinical assessment of 834 subjects, reporting a frequency of 41.5% and 26.4% for group function and occlusion with bilateral canine guidance, respectively. It should be kept in mind, however, that their study was conducted in adult subjects (aged 20 to 63 years), suggesting that, once the occlusal wear pattern has been established in full dentition, it can be maintained, regardless of age.18
Park et al,9 also in 2008, used the Bruxchecker® to identify the dental wear pattern in a Japanese population of 50 patients, reporting a higher frequency of two patterns: incisor-canine-premolar (ICP: 59%) and incisor-canine-premolar with areas on the balancing side (ICP + GM: 33%), which correspond to the most frequent patterns in the present study, GF + BCP and GF + BCA (with 60%). Also, the results of both studies were similar in terms of canine incisor pattern (CI: 24%), which is similar to the canine guidance with balanced contact points (CG + BCP: 26.7%) in the present study. The pattern of canine-incisor with balanced areas (CI + BCA) was found in 8%, compared to 6.7% for the canine guidance with balanced contact areas (CG + BCA). In terms of bilateral balanced occlusion with balanced contact areas (BB + BCA), the present study showed a frequency of 6.7%, differing from the study by Park et al, who reported a frequency of 59%, probably due to the age difference in the studied samples (ranging from 23 to 74 years),9 taking into account the physiological attrition that occurs in aging subjects.15
In 2006, Onodera et al, in a sample of 86 subjects with and without temporomandibular joint (TMJ) symptoms, and with the help of Bruxchecker®, reported that the dental wear patterns in SB that were most frequently presented in laterotrusion were the incisor-canine-premolar (ICP: 38.9%) with mediotrusive wear or balanced areas (63.9%) in patients without joint symptoms, and the incisor-canine-premolar-molar (ICPM: 94%) with mediotrusive wear (84%) in patients with articular symptoms.16 This agrees with the present study, where group function with balanced contacts areas (GF + BCA: 60%) was the pattern with the highest prevalence. In particular, Angle molar classes II and III showed a higher frequency of GF + BCA, in 40% and 33.33%, respectively, suggesting that these patients could be more susceptible to disorders or dysfunction of the TMJ.19
Considering that this is the first study that takes into account the description of dental wear patterns with respect to Angles’ molar classification, the occlusal wear pattern with the highest prevalence in Angle Class I was CG + BCP in a 46.6%, followed by GF + BCP in 40%, and to a lesser extent but with the same frequency, CG + BCA and BB + BCA in 6.7%; the GF + BCA occlusal wear pattern was not reported. It can be inferred that the percentage distribution of occlusal patterns is due to the position and proper relationship of the first molars in contact, which provide good occlusal support, achieving a pattern that meets the requirements for an optimal functional occlusion and obtaining the posterior disocclusion (presence of contacts and less wear due to interference) when performing the lateral movements (lateroprotusion and lateroretrusion) of the mandible during sleep. During the eccentric movements, the canine is the most appropriate tooth in these cases because it shows lower muscular activity compared to the contact between the posterior teeth; however, as reported by Belser and Hannam in 1985, the presence of CG does not reduce muscle activity during mastication, but it does during tightening.20 Nevertheless, in some cases the canines do not have an appropriate position to support these forces, or their crown-radicular length is not acceptable.1,21
The present study shows that the occlusal wear patterns with the highest prevalence according to Angle’s molar classification Class II are GF + BCP and GF + BCA in 80%, followed by BB + BCA in 13.3% and, less frequently, CG + BCP in 6.7%. It also shows that the CG + BCA occlusal wear pattern is not present in this group. It can be inferred that there is a marked tendency towards group function in Class II subjects, possibly due to a mesial disposition of the first maxillary molar and therefore of the anterior and premolar teeth, with presence of dental malpositions in 33.3% in the anterior area (ANT) and 33.3% in anterior and premolar teeth (ANT and PRE). This results in an interarch relationship between the upper premolars and the lower canines and/or premolars during the eccentric movements of the mandible, producing an occlusal wear pattern with predominance of group function and compromising the balancing side (interference)-a situation that poses a risk for the emergence of temporomandibular disorders (TMD)-.22,23
Another related aspect was arch form, because arches are affected by both the dimensional position of teeth within the alveolar ridge and as the interdental relationships (in this case with the canine, one of the most important teeth). Thus, the most frequent upper and lower arch type was the ovoid (60% and 66.7%) in Class I, which is compatible with the predominance of canine guidance in this group. In contrast, the most frequent upper arch type in Class II was the square (53.3%) and the ovoid in the lower arch (60%), showing a more vestibular spatial position of the canine and, in turn, a posterior position of premolars and molars, determining a greater predisposition for group function.
In addition, a significant increase in average overjet in Class II patients (5.1 +/- 2.4 mm distance between the vestibular side of the lower teeth with respect to the incisal edge of the upper teeth) hinders the canine guidance occlusal wear pattern since contact between the upper and lower canines becomes impossible due to the discrepancy between both jaws.
Concerning the findings in Class III, this study found out that the occlusal wear pattern with the highest prevalence was GF + BCA in 33.3%, followed by GF + BCP and CG + BC in 26.7% in both patterns, with CG + BCA being less frequent (in 13.3%). No presence of the BB + BCA occlusal wear pattern was identified in this classification. While the most prevalent upper and lower arch type in Class III was the ovoid (46.7% and 60%), the interdental relationship implies the presence of a varied occlusal wear pattern distribution depending on the intermaxillary relationship, which requires a broader sample and a more specific study on this classification, considering that no subject in the selected sample had anterior crossbite and only some had unilateral or bilateral posterior crossbite, which, according to the literature, can be associated with a high prevalence of signs and symptoms of TMD.24,25
Moreover, Goldstein et al, in 1984, stated that there is a relationship between the position of the head and an unstable occlusion due to an upward and backward mandibular displacement, producing unnecessary muscular activity and altering the elastic properties of the jaw; this causes a retruded and elevated position, decreasing the physiological inocclusion space between the jaws, resulting in more posterior contacts that can behave as interferences in the case of crossbites. This finding can explain the higher frequency of GF + BCA (33.3%) and GF + BCP (26.7%) occlusal wear patterns in Class III subjects.26,27
The only occlusal wear pattern that was not present in the study population was BB + BCP-with the BB + BCA pattern showing a very low frequency-. This may be explained because this type of occlusion is typical of the occlusal function in patients with full prosthesis (occlusion with flat morphology), where bilateral contacts are crucial to keep the prosthesis in place, and therefore it is unlikely for this to occur in subjects with definite dental morphology and with no loss in vertical dimension or dental pieces. The population in the present study was aged 12 to 17 years, with a short time of permanent dentition in mouth because of the recent completion of teeth eruption and occlusal coupling, and a probability of dental loss of 0.03% at the age of 12 years, according to the IV National Oral Health Survey (ENSAB IV).28 If these occlusal patterns were the most frequent in adolescents, any contact during the mandible’s eccentric movement posterior to the mesial cusp of the first upper and lower molars, especially on the balancing side, would exert greater force on the temporomandibular joint, resulting in the emergence of TMD.1,29
Another finding related to the identification of occlusal patterns, in addition to the working side (WS), was the presence of points (BCP) or areas (BCA) on the balancing side (BS), since one of the most common characteristics related to the etiology of temporomandibular disorders in previous reports were the contacts on the balancing side considered as interferences.29,30 However, the authors of subsequent investigations, carried out since the late 1980s and to the present, refer to studies in which contacts on the balancing side can possibly have a protective role on the temporomandibular joint of the same side, especially during clenching bruxism. This is because concentric wear can be observed around a point (instead of wear or interferences) at the support cusps during clenching, which is considered physiological and provides posterior support in the presence of occlusal forces, preventing from compressive ipsilateral joint displacements.20,30-35
Some studies suggest that the mediotrusive contacts (BCPs) are perceived by the neuromuscular system in a different way from occlusal contacts, which tend to reduce or inhibit muscle activity because the proprioceptors and nociceptors of the periodontal ligament create inhibitory responses;36 however, other studies suggest that the presence of mediotrusive contacts in posterior teeth increase muscle activity, which can be associated to the subjects who presented areas on the balancing side (BCA) in this study.37
However, the literature is not conclusive on whether the presence of occlusal interferences (BCP and BCA) causes TMD. It should be considered that there is no single etiologic factor in the development of TMD, and perhaps other factors (either psychological or genetic, for instance) can play an important role in the relationship between the subject’s individual response to interferences with balancing side wear and the development of symptoms in the craniomandibular system.38
Improvements in research designs should be made, including other variables to obtain new relevant information that allows for a different interpretation of the actual role of occlusal interferences and how these affect individuals. This would improve the predictions on the need and effectiveness of specific treatments aimed at eliminating occlusal interferences to implement protocols meeting the requirements for optimal functional occlusion.38 Since this is a descriptive study with a limited sample size for each Angle classification group (I, II and III) and a complex diverse universe of individuals, it is necessary to carry out more structured studies leading to more conclusive analyses.
However, the identification of different occlusal wear patterns according to Angle’s molar classification suggests the need to individualize the occlusal management of patients according to their functional demands, because, depending on the interarch relationship, there may be patters compatible with canine guidance, group function, and bilateral balanced occlusion-with balanced contacts and areas-like the ones reported in the present study.
It is important to recognize the role of SB as a parafunction that can alter the homeostasis of the stomatognathic system; however, recent studies claim that this activity favors stress release, acting as a protective factor to avoid the emergence of alterations in other organs (like gastric ulcers or suprarenal disorders), as reported by Sato and Slavicek.10 This study is therefore relevant because, by establishing occlusal wear patterns by means of a Bruxchecker® (in wake or sleep) as a starting point, the dental treatment can be individualized, identifying each patient’s needs and integrating the different specialties to achieve an adequate occlusion that can withstand the loads produced in the activity of bruxism, especially in sleep (when this activity is not controlled), in order to achieve functional stability, depending on each individual’s physiological tolerance, and thus avoid systemic alterations that put the human beings’ quality of life at risk.
CONCLUSIONS
The most frequent occlusal wear pattern in SB in this sample was group function with balanced contacts, followed by canine guidance with balanced contacts. The presence of the balanced bilateral occlusion pattern with balanced contacts could not be observed in the study population. The canine guidance with balanced areas and contacts was the predominant wear pattern for Angle Class I molar relationship. Concerning Class II molar relationship, the most predominant wear pattern was group function with balanced areas and contacts, and results were mixed regarding Class III molar relationship, showing group function with balanced areas and contacts, and canine guidance with balanced areas and contacts. Finally, it should be noted that the presence or absence of contacts on the balancing side could be an important factor to consider due to its protective (points) or favoring (areas) role in the emergence of TMD.