INTRODUCTION
The orthodontic movement aimed at closing posterior edentulous gaps is a clever idea but often difficult to perform due to a decrease in residual alveolar ridge width and the common collapse of the vestibular and lingual tables at the extraction site, especially if it has been done long ago.1
Premature loss of the first permanent molar is very common because it appears in the oral cavity at an early age, with more chances to experience cavities and to require early extraction.2,3 This causes the mesial inclination of the second and third molars, distalization of premolars, extrusion of the antagonist molar, alteration of the gingival margin to the inclined molar, uneven marginal ridges, food impaction and finally bite collapse, producing occlusal interferences, periodontal diseases, bruxism, decreased chewing effectiveness and alterations at the temporomandibular joint.4-6 Therefore, one of the possible treatments is the orthodontic closure of these edentulous spaces.
The loss or extraction of a tooth affects the alveolar bone by approximately 40% to 60%, in both height and thickness between the second and third years after extraction.7 This causes collapse of vestibular and lingual tables, decreasing the normal width of the bone passage.1
Orthodontic movement depends on multiple factors, the most important being the jaws’ bone composition. Movements in the maxillary bone can be achieved more quickly than in the mandible, because the maxillary bone has relatively thin corticals interconnected by a network of trabeculae and a spongy bone. The mandible, on the other hand, has more compact corticals in a more radial direction, connected by relatively thick trabeculae that hinder the movement of the molars.8
Patient’s age is another important factor since orthodontics in adults implies several aspects that must be considered, such as the state of health of periodontium and alveolar bone, which is more compact due to greater bone condensation. There is also reduction of the spongy bone and decrease in bone volume, with decreased cellular response; this results in slowed and limited orthodontic treatment.9-12
All this makes orthodontic movement difficult, forcing the orthodontist to apply more mechanical force to move the affected tooth, resulting in problems such as necrotic sites or hyalinization of the periodontal ligament, loss of marginal bone, dehiscence, fenestration and root resorption due to excessive force.
In view of the consequences of losing a tooth unit, this study proposes a technique to achieve the closure of space, reducing orthodontic treatment time and avoiding unnecessary or overly complex dental movements, as well as the possible side effects during closure.
It is also important to bear in mind the physiology of the alveolar bone, which has a cortical layer formed by compact bone-difficult to remodel- and another layer of spongy or trabecular bone-which is the area where orthodontic movement mainly occurs-.13,14 Thus, the rate of dental movement is the catabolic activity mediated by osteoclasts, which perform remodeling and bone destruction functions when required by the body.9,13,15,16
The theoretical linear rate of osteoclasts reabsorption during cortical bone remodeling is estimated at 0.6 mm/month through the cortical bone. However, a clinical study in adults showed that the linear reabsorption rate at the interface of the lower molars periodontal ligament was significantly lower.17-24
This is why the present study particularly recommends the technique used by Mejía (1994), called flexicorticotomy, which by cutting the cortical bone layer separates its lingual/palatal portion from its vestibular portion, creating a corridor or sulcus that allows the movement of a tooth or group of teeth to large distances through the bone, thus minimizing treatment time in cases with atrophied bone corridors or narrow residual ridges.1,11,12
It is then understood that this new surgical gap created by strapping the residual ridge tables would behave like a simple exodontia that allows the formation of blood clot and then transform itself into spongy bone that facilitates teeth displacement.1,11,25,26 In turn, this technique induces a response in the alveolar bone that can demineralize bone tissue around the dental roots, producing a transient osteopenia. Once this has happened, there is the so-called “window” of 3 to 4 months to quickly move the teeth through the demineralized bone matrix. This bone response is known as regional acceleratory phenomenon or RAP.27
Thus, the term regional in demineralization of both the cutting side and the adjacent bone, and the term acceleratory both refer to an exaggerated or intensified bone response of osteoclasts and osteoblasts, which increase in number by multicellular mediator mechanisms containing precursors, helper cells, blood capillaries, and lymphocytes, extending to the spongy bone, without greatly affecting the intramedullary vessels, which is beneficial for optimal bone regeneration thanks to accelerated bone remodeling.3,16,21,28,29
In the flexicorticotomy technique, no suture is done to avoid confronting the edges of the incision and to maintain gained width. Below is a description of the surgical procedure:1,25,26
Infiltratory anesthesia in the corresponding area
Incision on the edentulous edge
Intracrevicular incisions
Full-thickness flap lift
Consecutive perforations on the cortical from mesial to distal, in an apical direction to the spongy bone
Longitudinal fracture lines are done on the bone adjacent to the neighboring vestibular or lingual teeth in the mid-proximal area towards the toothless space
Bone girdles are separated from adjacent teeth following the axes of teeth
Bone tables are separated by slowly strapping them towards vestibular or lingual until the desired expansion of the bone passage
The surgical alveolus fills with blood and forms the clot needed for bone neoformation. Dental movement can be performed immediately if the apparatus is already in place or else wait 8 days to place the apparatus.
When the collapse length is longer than the mesio-distal distance of a tooth, it is recommended to fill the new surgical alveolus with collagen sponges, freeze-dried bone, or resorbable hydroxyapatite, to avoid collapsing the tables, keep them separated to avoid pressure from surrounding soft tissues, and avoid bony defects by the time treatment is completed.1
Also, with this surgical technique it is possible to move the teeth immediately after surgery.1 This is why the mesialization of molars with the help of flexicorticotomy allows to make the most of cellular activity to accelerate orthodontic movement. Especially when this mesialization is performed with the help of an absolute anchorage with miniscrews which help maintain the anterior coupling and perform the dental movements without losing anchorage, which offers advantages to both patient and orthodontist.
CASE DESCRIPTION
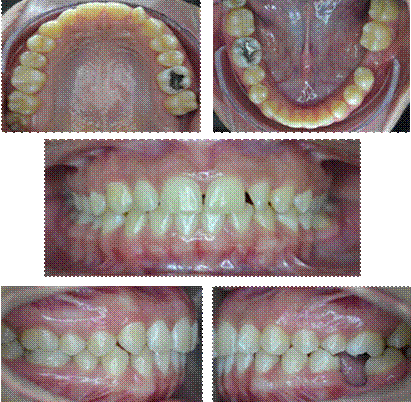
This is the case of a 22-year-old female patient who consulted the Universidad de Carabobo’s Dentofacial Orthopedics and Orthodontics Graduate Program for assessment and orthodontic treatment. Medical history was done upon obtaining her informed consent, showing that the patient does not have personal or family history of medical conditions. The extraoral clinical examination showed that the patient has an oval face with mild facial asymmetry and convex profile.
The oral clinical examination shows moderate upper crowding, 2.5 mm horizontal overbite and 2.5 mm vertical overbite. She also has Class I molar relationship in the right side and non-registerable relationship in the left side due to the absence of dental piece 36, and Class I canine relationship in both sides. Spee’s Curve: 2mm right, 3.5 mm left, multiple tooth rotations and absence of tooth 36 causing depression of vestibular bone table (Figure 1).
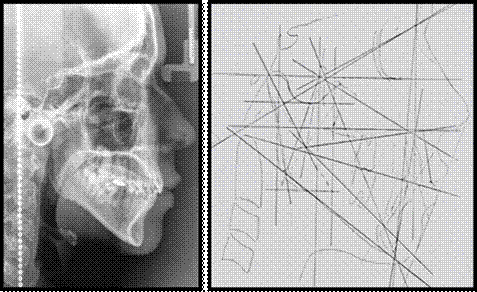
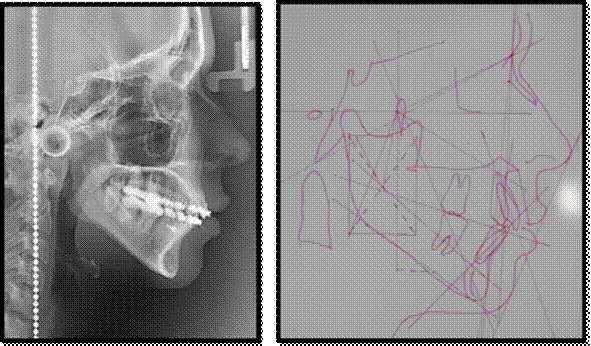
Radiographic evaluation
Conventional studies were conducted, including panoramic and lateral cephalic radiography (Figure 2).
Distance between teeth 35 and 37
The distance between the vestibular cusp of tooth 35 and the mesiobuccal cusp of tooth 37 pre-treatment was measured as 14 mm.
Treatment plan
Roth slot 0.022” orthodontic apparatus was placed, performing the following actions: alignment and leveling, placement of orthodontic implant between teeth 35 and 34, flexicorticotomy for the mesialization of teeth 37 and 38, completion and containment, placing upper and lower circumferential retainer.
Treatment phases
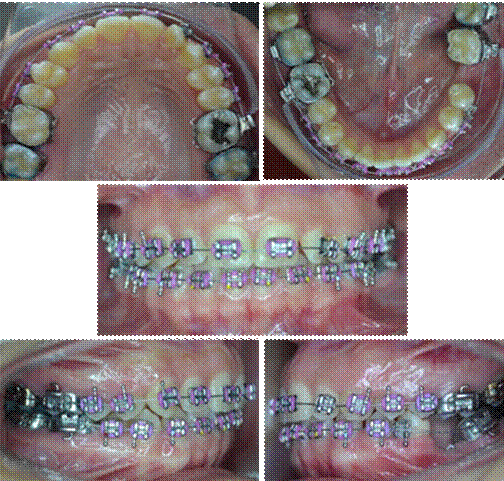
Phase 1. Alignment and planing
The following sequence of archwires was used during a 5-month period (Figure 3):
0.012” NiTi archwhire. Super Elastic
0.014” NiTi archwhire. Super Elastic
0.018” NiTi archwhire. Super Elastic
0.017” x 0.025” NiTi. Super Elastic
0.018” x 0.025” NiTi. Super Elastic
Phase 2. Work
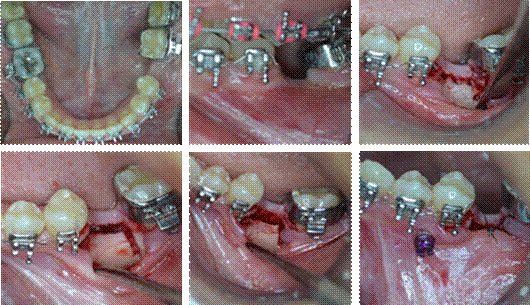
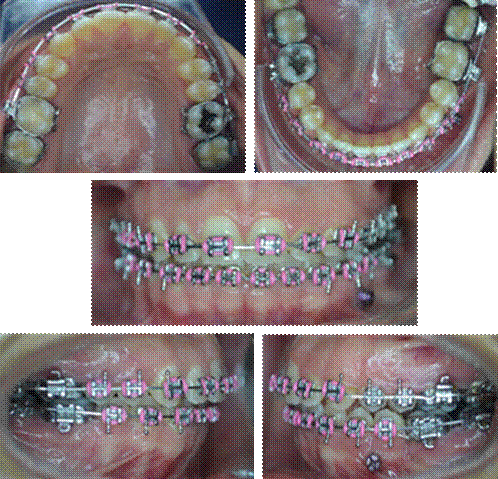
At this stage, anterior upper interproximal stripping was performed to correct the mild crowding and improve overjet. Flexicorticotomy was performed to achieve the displacement of teeth 37 and 38 in less time. Absolute anchorage was placed with ortho implant of 8 x 1.7 mm and .022” slot between teeth 34 and 35, conducting mesialization with orthoimplant chain to the power-arm of teeth 37, achieving a mass movement. Stainless steel 0.018” x 0.025” archwire was used (Figure 4).
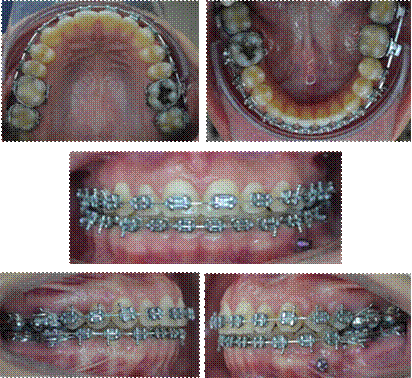
Lower impressions and photographs were also taken one, three, six, nine months and one year later to observe and quantify the mesialization of tooth units (Figure 5 and 6).
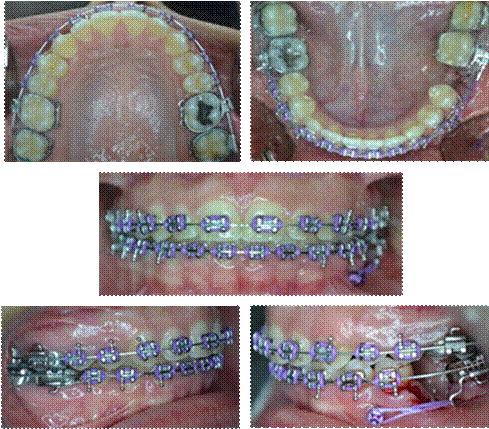
Source: by the authors
Figure 5 Intraoral photographs, flexicorticotomy, and placement of orthoimplant and power arm
Phase 3. Completion
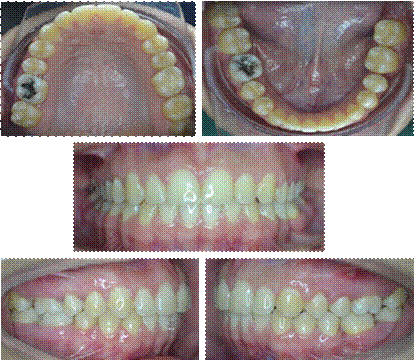
Coordinated stainless steel archwires of 0.017” x 0.025” mm were placed. Upper Gingivoplasty. Replacement of brackets in teeth 24 and 25 (Figure 7).
RESULTS
The mesialization of second and third lower molars was monitored for a year, taking the distance between the vestibular cusp of tooth 35 and the mesio-vestibular cusp of tooth 37-which was 14 mm-as an initial measurement. In the first month after flexicorticotomy, there was a 1 mm closure; at 3 months it was 3 mm, at 6 months it was 5 mm, at 9 months it was 6 mm, and one year after the procedure the closure between dental pieces reached 8 mm.
DISCUSSION
Orthodontic movement is influenced by increased alveolar bone metabolism and decreased bone density. Therefore, the bone turnover rate determines the quantity and quality of movements. High bone turnover significantly increases the rate of dental movement.13,22-24,27,28 For this reason, flexicorticotomy seeks to modify the cortical layer of alveolar bone with minimal alteration of the spongy or spinal bone, influencing the bone turnover rate, significantly increasing the number of osteoclasts, which are known to be responsible for the removal of bone on the pressure side of the applied force, and thus accelerate the orthodontic movement.1,3,25,29-31
The regional acceleratory phenomenon described by several authors (Hiaji, 2000, Frost, 1989 and Wilcko, 2009) has been proven over the years, offering insights into bone histology and physiology of the orthodontic movement. Lee (2006) found that this surgical technique works well due to induction of a transient osteopenia at the lesion site, which triggers exaggerated celular activity, intensifying the transformation of macrophages into osteoclasts, and thus healing occurs 2 to 10 times faster than a physiological healing, offering a time window to accelerate orthodontic movement, which begins within a few days of the injury, with typical peaks at 1 to 2 months, and usually lasts up to 4 months, but may take up to 6 to 24 months to decrease.8,10,11,32,33,34 However, according to Saad’s study (2010), RAP remains while the orthodontic movement continues, and once it stops, the same will occur with osteopenia.11,12,33,34
Mejía (1994) and Martínez (2010) reported similar results in their cases, obtaining full mesialization of second and third molars for the edentulous space of the former in 18 months-an orthodontic movement that normally takes 24 to 36 months to complete.
Flexicorticotomy is thus a technique that opens new windows to orthodontics, expanding the range of movements to be performed especially in adult patients, reducing periods of time to half the conventional total lapse, achieving movements that were limited in the past, and reaching treatment goals more effectively by combining orthodontics with surgical treatment to solve all patients’ needs.26,32,34,35
Finally, the periodontium is preserved during flexicorticotomy because no moderate or advanced resorptions are produced. This shows that a systematized orthodontic therapy after the surgical act provides rapid movement and support for relocated teeth. The presence of normal bone repair and X-ray evidence of bone formation are extensive evidence of the remarkable restorative properties and versatility of the involved connective tissue.26,32,35,36,37
CONCLUSIONS
The flexicorticotomy approach helped accelerate dental movement, with added benefits to patient as it reduces treatment time. This technique makes difficult movements possible, as it successfully mesializes lower molars, thus eliminating the use of prosthetics.
Similarly, the use of flexicorticotomy did not produce root resorptions, nor gingival dehiscences, achieving the full closure of edentulous space in a short period of time.
RECOMMENDATIONS
The findings of the present study suggest that flexicorticotomy is a particularly useful tool for orthodontists after an adequate diagnosis of the clinical case; however, it is recommended to use it only when it is really necessary. It is also essential to analyze the following aspects:
Always evaluate the ridge section because the outcome would be unpredictable in the presence of a large disto-mesial amount of edentulous ridge.
Evaluate ridge type because it is contraindicated in knife-edged ridges due to risk of bony table fracture.3
Assess bone quality to reduce fracture risk.
Dental movement can be performed immediately if the appliance is already in place, or else wait 8 days to install the apparatus and start closing.36
It is recommended to activate orthodontic appliance every fortnight to make the most of the surgical procedure, especially in the weeks of greatest osteopenia, namely weeks 4th to 6th, which according to the literature is when the most movement occurs.33
In all cases, the start of orthodontic force should not be delayed more than 2 weeks after surgery. A longer delay could cause failure or decrease the advantages offered by the shorter period when RAP occurs.33
A permanent orthodontic-periodontal assessment, follow-up, and maintenance is recommended while dental movement is being performed.
Collagen sponges, freeze-dried bone, resorbable hydroxyapatite, or autologous bone should be used to fill the surgical alveolus when the collapse length is longer than the mesio-distal distance of a tooth.
Antibiotics and pain medications should be given. However, the administration of anti-inflammatory agents is not recommended because it can theoretically interfere with the regional acceleratory process. It is also recommended to apply ice packs to the affected areas to decrease the severity of any possible edema or postoperative inflammation.