INTRODUCTION
Molar Incisor Hypomineralization (MIH) is defined as a qualitative enamel defect, presumably multifactorial in origin, characterized by the presence of demarcated opacities in one to four of the first permanent molars, with or without the involvement of the permanent incisors. Weak and porous enamel rapidly evolves into posteruptive fracture and caries lesions.1-3
Ultrastructural, chemical composition and mechanical properties of MIH-enamel show significant differences with compared to healthy enamel. A reduction in mineral density has been reportedly associated with the color of the defect, containing a lower mineral density in brownish-brown opacities when compared with white-cream opacities. These findings guide clinicians to take therapeutic decisions, even though multiple factors are involved in determining the severity of MIH.4
Generally, permanent incisors are found less affected than first permanent molars. Patients with incisor involvement usually have aesthetic complaints leading to self-confidence problems, long dental treatments, especially in young patients with immature anterior teeth and extensive pulp tissue.2,5 Recently, a study has shown that management of aesthetics was considered by professionals as the second most challenging treatment (20%) in MIH patients, preceded only by the longevity of restorations.6 Additionally, opacities in anterior teeth are exposed during speaking and smiling, affecting self-image in a highly susceptible psychosocial period, such as puberty and adolescence. Microabrasion, dental vital bleaching (DVB), resin infiltration and composite restorations are the most frequent therapeutic options for MIH incisors.2,5,7-10
CASE SERIES PRESENTATION
A case series of five female MIH patients with aesthetic concerns is presented. All participants or their parents or legal representatives signed the informed consent form. Diagnose criteria (in at least one first permanent molar) established by the European Academy of Pediatric Dentistry for MIH were used and include: 1) Presence of demarcated opacities on the enamel surface that shows normal thickness, 2) Posteruptive enamel breakdown associated with a pre-existing opacity, 3) Presence of an atypical restoration with opaque enamel edges, 4) Absence of a permanent first molar due to extraction combined with the presence of opacities and / or atypical restoration in another first molar or permanent incisor and finally, 5) Delayed eruption of a first permanent molar.11 To determine severity of MIH, the classification proposed by Ghanim et al. was used; a tooth with opacities, regardless of its coloration, was considered as mild defect, while the posteruptive fracture, the atypical restoration or a tooth extracted due to MIH, was considered a severe defect.5 TF index described by Thylstrup and Fejerskov for the identification of dental fluorosis was used for case with combined defects (MIH and dental fluorosis).12
All clinical procedures were performed by the same clinician. Dental photographs were taken in first and consecutives dental visits following standardized procedure. All photographs were taken by one dentist using the following equipment: Canon® EOS 5D Mark IV body; Canon® 100mm f // 2,8 macro lens; Macro twin lite flash MT-26EX-RT Canon® Manual mode; Speed 1/100; Diaphragm 29; ISO 200.
Socio-demographic characteristics of the patients, clinical findings, diagnose criteria and procedures followed during dental treatment were tabulated (Table 1).
Table 1 Socio-demographic data, clinical findings, diagnose criteria and clinical procedures of all cases
| Case 1 | Case 2 | Case 3 | Case 4 | Case 5 | |
|---|---|---|---|---|---|
| Age (years) | 9 | 9 | 29 | 10 | 9 |
| Gender | Female | Female | Female | Female | Female |
| Resident endemic fluorosis area | No | No | No | No | No |
| Clinical findings (permanent incisors) | Demarcated opacity white-cream and posteruptive breakdown in incisal dental third #8. Lineal diffuse opacities in cervical third # 8 and #9. | Demarcated opacity cream-yellow #9. Mild discoloration #8 | Demarcated opacity cream/yellow. #9 Demarcated opacity (> 1 mm) white, incisal third #10 Enamel cracks post orthodontic brackets debonding (all incisors) | Remnant of orthodontic appliances (first visit) #8, #7, #9, #10, #24, #25. Brackets debonding was performed by colleague. Enamel cracks post orthodontic brackets debonding (second visit). Demarcated opacity yellow-brown #7 and white-cream # 9 | Posteruptive breakdown incisal third and opacity yellow- brownish #8 |
| Sensitivity before dental treatment | No | No | No | Yes | Yes |
| Diagnose and Defect Classification | Severe MIH + Dental Fluorosis TF 1 | Mild MIH | Mild MIH | Mild MIH | Severe MIH |
| Dental treatment and procedures described below. | Dental vital bleaching with 10% carbamide peroxide for 6 days/ 6 hours continuous per day. Continuous supervision by parents. Macroabrasion and microabrasion (same day) after DVB. | Dental vital bleaching with 10% carbamide peroxide for 5 days/ 6 hours continuous per day. Continuous supervision by parents. | Macroabrasion and microabrasion (same day). Control visit. Evaluation of tissue response. Dental vital bleaching with 20% carbamide peroxide for 8 days/ 2 hours continuous per day. | Resin infiltration (one session). | Macroabrasion and composite restoration. |
Source: by the authors
For DVB procedures, carbamide peroxide (Opalescence® - Ultradent Inc. Utah. USA), in concentrations of 10% or 20%, depending on the case, was used in an individual tray (0,39” Opalescence Kit®-Ultradent Inc. Utah. USA) with reservoirs (Block-Out Resin Ultradent Inc. Utah. USA) performed according to the manufacturer's instructions. Written directions were given to patients and parents, for optimal follow-up instructions. Specifications were done to apply gel only in maxillary permanent incisors in Cases 1 and 2. For Case 3, gel was applied in reservoirs from # 3 to #14. Patients were called every day to confirm correct use and treatment evolution.
Macroabrasion technique was used in Cases 1 and 3 to treat dental fluorosis (Case 1) and enamel cracks caused by brackets debonding (Case 3), following this procedure: with a conical diamond bur, round end tip type (DFS- Diamon® # 531516, Riedenburg, German) medium grit and a high-speed handpiece. No pressure was applied into the vestibular face of each affected tooth when activating the handpiece, placing the bur parallel to its long axis and making mesial-distal movements, avoiding proximal zones and keeping the anatomy of the vestibular face. Then, a second procedure was necessary when it was observed that remnant affected enamel in the cervical zone, which was removed with diamond bur, needle end tip type fine grit (DFS® # 531304, Riedenburg, German).
Microabrasion was performed using 6,6% hydrochloric acid and silicon carbide micro particles product (Opalustre®-Ultradent Inc. Utah. USA) following manufacturer's instructions: after rubber dam (Elasti-dam®, Coltene, Altstätten, Switzerland), a layer of product was applied to the vestibular area of superior incisors, and then using a cup (OpalCups Bristle®- Ultradent Inc. Utah. USA) and slow revolutions per minute (approximately 500 RPM) a medium pressure was applied for each tooth for 60 seconds. Then, the clinician rinsed the teeth with a solution of sodium bicarbonate 1:1 and after the rubber dam was removed, the operator applied neutral sodium fluoride gel, using a tray for 4 minutes. Outcomes after procedures in Cases 1 to 3 are shown in Figures 1, 2 and 3.
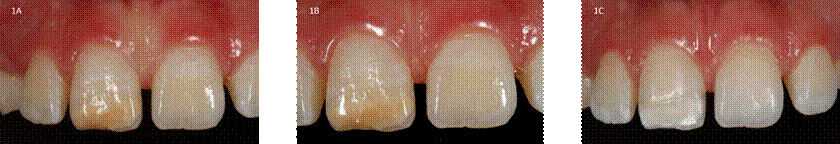
Source: by the authors
Figure 1 Pre and post-treatment dental photographs of all cases. 1A-1B. Case 1: pre-treatment image posteruptive enamel breakdown #11. 1C. Case 1: image after macroabrasion, microabrasion and DVB
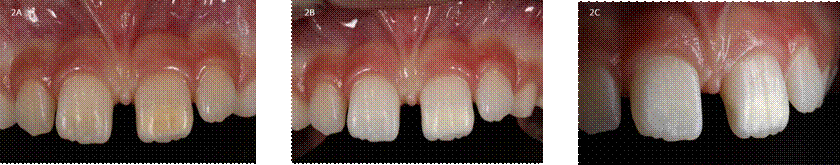
Source: by the authors
Figure 2 Pre and post-treatment dental photographs of all cases. 2A. Case 2: cream/yellow opacity #21. 2B. Case 2: frontal photo #21 and # 11 after DVB. 2C. Case 2: lateral photo #21 after DVB
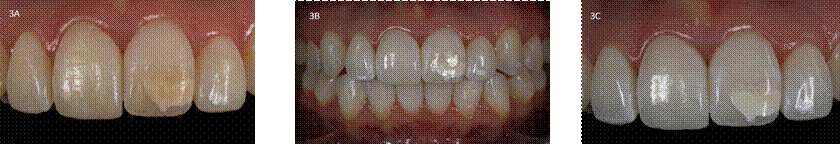
Source: by the authors
Figure 3 Pre and post-treatment dental photographs of all cases. 3A. Case 3: enamel cracks due to brackets debonding, cream/yellow opacity #21. 3B -3C. Case 3: photo after macroabrasion, microabrasion and DVB
Resin infiltration (Case 4) was performance with absolute isolation and using Icon® products (DMG Company, Hamburgo, Germany): Icon-etch: Hydrochloric acid, pyrogenic silicic acid, surface-active substances; Icon-Dry: 99% ethanol and Icon-Infiltrant: Methacrylate-based resin matrix, initiators, and additives, following these instructions: Icon-etch was applied for 2 minutes, rinsed for 30 seconds, and dried 3 times. Icon-dry was applied and allowed to rest for 30 seconds, and the operator then proceeded to dry again until the area was completely desiccated in order to use Icon-Infiltrant, allowing the penetration for 3 minutes. Excess material was removed with the use of cotton wads and dental floss, and the remaining material was polymerized for 40 seconds. Polish cup was used for surface finish. The outcome after resin infiltration is shown in Figure 4.
Source: by the authors
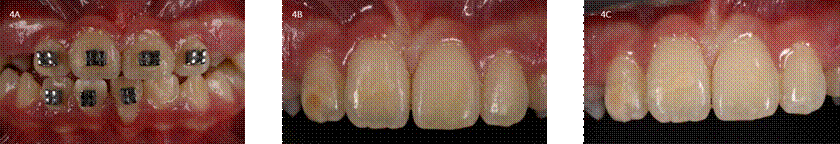
Figure 4 Pre and post-treatment dental photographs of all cases. 4A. Case 4: pretreatment photo, first visit. 4B. Case 4: dental photo after bracket debonding by a colleague. 4C. Case 4: dental photo after resin infiltration
Composite restoration (Case 5) was performed following this sequence: Local anesthesia (Newcaina®, New Stetic, Colombia) and rubber dam (Elasti-dam®, Coltene, Altstätten, Switzerland) of upper incisors. The next step was a prophylaxis with pumice-stone and water, then prophylaxis with only the brush. A #4 round fine grit diamond bur (DFS®, Riedenburg, German) was used for tooth preparation. Macroreduction of hypomineralized tissue was carried out with a conservative approach; some porous enamel was kept in preparation margins. Pre-aciding deproteinization technique was performed with 5,25% sodium hypochlorite solution applied to MIH-enamel for 60 seconds. Cavity was etched with 37% orthophosphoric acid for 15 seconds using selective technique, and then rinsed for 15 seconds. Excess water was removed using a foam pellet (Pele Tim® Voco, Cuxhaven, Germany). One-bottled adhesive was applied (Ultradent Peak®-Ultradent Inc. Utah. USA), then gently dried and polymerized. Nano-hybrid composite enamel and dentine (Forma®- Ultradent Inc. Utah. USA), color A2, was placed in incremental layers. The restoration was finished off using composites polishers and brushes (Jiffy Original Composite System ®- Ultradent Inc. Utah. USA). The outcome after composite restoration is shown in Figure 5.
POTENTIAL PROBLEMS
No problems or complications were perceived. None of the patients referred dental sensitivity after clinical procedures. Although this case series has limitations due a low number of patients and the range of ages between them, it may be used to evaluate outcomes after different clinical approaches in patients with MIH. There are few publications in this area, and there should be more reports to highlight the advantages and disadvantages of clinical procedures.
SUMMARY OF ADVANTAGES AND DISADVANTAGES
MIH is a condition that significantly affects the aesthetics of patients when incisors present opacities. Although some clinicians consider that MIH-opacities in anterior teeth often improve in the long term and most of them prefer to postpone aesthetic treatment, young patients with affection of self-esteem and self-image require appropriate and timely dental intervention.
Advantages
DVB with low concentration (10%) of carbamide peroxide is considered the first-choice treatment for opacities in adolescent patients since it has a reduced possibility of diffusing through enamel and dentin, preventing adverse effects on extensive pulp tissue13,14.
Microabrasion, in combination with macroabrasion, produces significant changes in dental fluorosis and enamel cracks.
Resin infiltration seems to be an appropriate conservative alternative since it may reduce (or correct, depending on the opacity color) the aesthetic complaint and sensitivity, and may also create a more appropriate substrate for bonding of orthodontic brackets.
Macroreduction and composite restoration solve aesthetic complaints in MIH patients.
Disadvantages
DVB procedures don´t correct visible defects on the tooth surface by themselves, thus having the necessity to be combined with other techniques such as micro-abrasion, resin infiltration or composites restorations to reach the desirable effect
Microabrasion and macroabrasion seem to have limited results in MIH demarcated opacities. Additionally, clinicians need to develop appropriate skills in these procedures to avoid inadequate loss of enamel
Resin infiltration in hypomineralized enamel has unpredictable results
DISCUSSION
Dental vital bleaching (DVB), microabrasion, macroreduction resin infiltration and composite restorations are the most frequent therapeutic options for MIH incisors and has been usefully in the cases presented.
Early diagnosis should be within the reach of all clinicians and is essential for improving the treatment outcome and quality of life of affected patients. Therefore, to prevent damage to the teeth with structure anomalies, early visits and close follow-ups are necessary. In children, the first dental visit is recommended at the age of 3-4 years, yet in the presence of important dental abnormalities of the deciduous dentition, the pediatrician or the parents should request a visit at an even younger age.15 The high prevalence of MIH indicates the need for research to clarify etiological factors and improve the durability of restorations in affected teeth.16
There is a growing body of evidence related to the etiology, presentation, and clinical management of MIH. Current knowledge appears to be focused on potential genetic aspects, as well as the development and validation of indices for the diagnosis and management of MIH. There has also been increasing recognition of the global and individual burden of this common condition. Dental health professionals should regularly appraise the basic science and clinical MIH literature to ensure that they provide the best possible short- and long-term care for their young patients.17
Most publications in MIH are done in clinical management of molars; incisors affected are less studied and reported. Although these patients suffer from many discomforts, there is evidence of better levels of self-esteem after intervention.
Simple, non-invasive dental treatment can have a positive effect on appearance-related satisfaction. The use of child-centered approaches offer an invaluable insight into patient perspectives.18
Also, there are problems in HIM like tooth hypersensitivity which is a common symptom in these patients. MIH-related tooth hypersensitivity seems to be present in disintegrated molars immediately after tooth eruption.19
Despite clear assessment criteria, studies of MIH and hypomineralised second primary molars (HSPM) are marked by inconsistency in outcome measurements. The use of a standardised protocol, diagnostic and grading criteria will greatly enhance the quality of epidemiological studies of MIH.5
Facial and dental appearance influences how individuals are perceived by others. Young people may make negative psychosocial judgements on the basis of enamel appearance.20 In a research carried out in a group of children with enamel dental defects, the results revealed that the group had negative emotions about how they perceived themselves and were dissatisfied with their body image. This would likely indicate that children are having difficulty forming their values and components related to self-esteem in an inappropriate way.21
The EAPD (European Academy of Pediatric Dentistry) strongly supports the use of all available treatment tools for the treatment of HIM teeth, keeping in mind the need for a pain-free and effective treatment plan and the well-being of the pediatric patient through dental, oral, medical, and social level.22
This series of cases has some limitations which are important to highlight. There is a need for more cases to show the scope of these treatments. The indication of dental whitening within the concept of "minimum intervention" has been an obstacle due to the poor acceptance that it has as an alternative of great value to preserve dental tissue, both due to the multiple failures reported by patients on previous occasions, as well as due to the side effects, presumably due to bad experiences and poorly controlled treatment.
Adherence remains uncertain despite the outcome of a case presented in this article, but alternative methods should be studied to optimize this important reconstruction step for post-eruptive fractures and to recover aesthetics that are so valuable in self-esteem and self-image of juvenile infant patients.
Studies should be carried out with different adhesive systems to ensure a greater longevity of the restorations. More literature is required to support or deny deproteinization of enamel. There is a lack of studies on adhesion to different substrates due the limited possibility of obtaining study specimens.
Finally, there is still a need to improve knowledge to identify, diagnose and treat enamel development defects.
CONCLUSIONS
MIH is a dental defect that modifies aesthetics, self-image, and self-esteem in patients with incisors affected. Therapeutic options range from very conservative procedures to those considered more invasive.
Better changes are observed in the stratification with resin, total or partial aesthetic change is appreciated depending on the case. It is advisable to take into consideration the available treatments according to each patient's need.
Clinicians must select the appropriate approach according to an individualized evaluation of each case, considering the patient's expectations, dental age, psychosocial period, oncoming orthodontic treatment, the severity of the condition, presence of sensitivity and the presumed aesthetic result of the selected treatment. Patients and parents should receive adequate information of procedures’ limitations and possible outcomes. More longitudinal studies are still required to determine the long-term results in treatments for aesthetic affectation.