Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Vitae
Print version ISSN 0121-4004
Vitae vol.22 no.1 Medellín Jan./Apr. 2015
https://doi.org/10.17533/udea.vitae.v22n1a05
PHARMACEUTICAL CARE
DOI: 10.17533/udea.vitae.v22n1a05
SMOKING CESSATION IN A COMMUNITY PHARMACY: PRELIMINARY RESULTS OF A PHARMACEUTICAL CARE PROGRAMME
CESACIÓN TABÁQUICA EN FARMACIA COMUNITARIA: RESULTADOS PRELIMINARES DE UN PROGRAMA DE ATENCIÓN FARMACÉUTICA
Mónica CONDINHO MsC.1,2, Fernando FERNÁNDEZ-LLIMOS Ph.D.3, Isabel V. FIGUEIREDO Ph.D.1,4, Carlos SINOGAS Ph.D.5,5,*
1 Pharmacology and Pharmaceutical Care, Faculty of Pharmacy, University of Coimbra. Coimbra, Portugal
2 ACF - Acompanhamento Farmacoterapêutico, Lda. Pavia, Portugal
3 Research Institute for Medicines (iMed.ULisboa), Department of Social Pharmacy, Faculty of Pharmacy, University of Lisbon. Lisbon, Portugal
4 Institute for Biomedical Imaging and Life Sciences (IBILI) - University of Coimbra. Coimbra, Portugal
5 Department of Biology, School of Science and Technology, University of Évora. Évora, Portugal
* Correspondig author: sinogas@uevora.pt.
Recibido: Febrero 05 de 2015.
Aceptado: Mayo 05 de 2015
ABSTRACT
Background: According to the World Health Organisation, tobacco use is one of the most widespread public health threats in the world, making it particularly urgent to promote smoking cessation. The effectiveness of pharmacist interventions in smoking cessation has been documented in the international literature, but not sufficiently in Portugal. Objective: To report the preliminary results of study to assess the effectiveness of a smoking cessation programme delivered in Portuguese community pharmacies using an outsorcing-based regimen. Methods: Within the scope of a pharmaceutical care programme implemented in seven community pharmacies by an outsourced pharmacist, a specific consultation for smoking cessation was developed, in accordance with Portugal's General Directorate of Health's recommendations and instruments. The smokers were identified and invited to join the programme by the pharmacy staff during their daily activities. Patients that accepted signed an informed consent. Through several face-to-face and phone consultations and based on a comprehensive patient approach, personalised plans to quit tobacco were defined with the patients' agreement. The effectiveness of the service was assessed through the evaluation of quit rates at 1, 6 and 12 months. The continuous variables were expressed as mean ± standard error of the mean. Results: During approximately 5 years (between January 2009 and July 2014), 69 smokers joined the programme. Of these, 17 desisted during the first consultation. Of the remaining 52 patients, the mean age was 47.4 ± 2.11 years old and 55.8% were male. A total of 264 pharmaceutical consultations were delivered and, on average, each patient received 7.7 ± 0.81 interventions. Most interventions (60.1%) were pharmacological (e.g. nicotine replacement products), while non-pharmacological measures (e.g. motivational interviewing) represented 39.9%. Five patients were referred to a physician. At 1 month after the quit date, 37 patients were abstinent (53.6%); 6 months later the number reduced to 24 (34.8%) and, 1 year later, 16 patients remained abstinent (23.2%). Conclusions: The implementation of a smoking cessation programme in community pharmacies using an external pharmacist may contribute effectively to tobacco cessation in Portugal.
Keywords: Pharmacist; Smoking Cessation; Community Pharmacy; Pharmaceutical care
RESUMEN
Antecedentes: Según la Organización Mundial de la Salud, el tabaco es una de las mayores amenazas del mundo, siendo urgente promover el abandono tabáquico. La efectividad de las intervenciones farmacéuticas en cesación tabáquica ha sido documentada en la literatura, pero no en Portugal. Objetivo: Comunicar los resultados preliminares de un estudio para evaluar la efectividad de un programa de cesación tabáquica desarrollado en farmacias comunitarias portuguesas usando un régimen de out-sourcing. Métodos: En el ámbito de un programa de atención farmacéutica implantado en siete farmacias por un farmacéutico externalizado, se desarrolló una consulta de cesación tabáquica siguiendo las recomendaciones e instrumentos de la Dirección General de Salud de Portugal. Se identificó a los fumadores y el personal de la farmacia durante sus actividades rutinarias les invitó a unirse al programa. Los que aceptaban firmaban un consentimiento informado. Mediante consultas presenciales y telefónicas y a través de un abordaje global del paciente, se definieron en acuerdo con el paciente planes personalizados de abandono del tabaquismo. La efectividad del servicio se midió mediante las tasas de cesación a 1, 6 y 12 meses. Las variables continuas se expresaron como media ± error estándar de la media. Resultados: Durante aproximadamente 5 años (entre enero 2009 y julio 2014), 69 fumadores se unieron al programa. De estos, 17 desistieron durante la primera consulta. Entre los restantes 52 pacientes, tenían 47.4 ± 2.11 años y el 55,8% eran hombres. Se realizaron 264 consultas farmacéuticas y, en media cada paciente recibió 7.7 ± 0.81 intervenciones. La mayoría de las intervenciones (60,1%) eran farmacológicas (p.e. productos de substitución de nicotina), y el restante 39,9% fueron medidas no farmacológicas (p.e. entrevista motivacional). Cinco pacientes fueron remitidos al médico. Después de 1 mes de la fecha convenida para el inicio de la cesación, 37 pacientes (53,6%) estaban en abstinencia; 6 meses más tarde el número se reducía a 24 (34,8%) y un año más tarde 16 pacientes (23,2%) permanecían abstinentes.Conclusión: La implantación de un programa de casación tabáquica en farmacias comunitarias, utilizando un farmacéutico externo, puede contribuir efectivamente a la cesación tabáquica en Portugal.
Palabras clave: Farmacéutico; Cesación tabáquica; Farmacia comunitaria; Atención farmacéutica.
INTRODUCTION
According to the World Health Organisation, the tobacco epidemic is one of the greatest public health threats the world has ever faced, killing nearly six million people a year (1). Additionally, it is estimated that if effective measures are not urgently taken, tobacco could kill over 1 billion people in the 21st century. In Portugal, tobacco use may be responsible for 1 in 10 deaths of adult smokers and 1 in 4 for people aged 45-59 years old (2). Approximately half of the Portuguese smokers never made any attempt to stop smoking (3).
The effectiveness of pharmacist interventions in smoking cessation is recognised in the international literature (4-6), but, in Portugal, the data are scarce. This paper reports the preliminary results of a study aiming to assess the effectiveness of a smoking cessation programme delivered in Portuguese community pharmacies using an outsorcing-based regimen.
METHODS
A retrospective and longitudinal study on the preliminary results of a pharmaceutical care programme for smoking cessation is reported. An outsourced (external) pharmacist, specifically trained in smoking cessation, implemented the pharmaceutical care programme in seven community pharmacies (mainly in the Algarve and Alentejo Portuguese regions), following Portugal's General Directorate of Health's recommendations (through several consultations and phone contacts) (7). The patients were identified during the daily pharmacy activities with no specific sampling method other than having smoking habits and wish to quit smoking. They were invited to join the programme by the pharmacy staff (pharmacists or technicians) and were informed about the structure of the service and the price of the consultations. All patients that joined the service signed an informed consent form.
In the first consultation, and using a specific form, the pharmacist recorded tobacco habits, a clinical history and the medication profile. All consultations included an assessment of the body mass index, waist circumference, blood pressure and respiratory parameters, such as spirometric tests and carbon monoxide and carboxihaemoglobin in exhaled air. The two later were considered as tobacco biomarkers. The Richmond (8), and Fagerström (9) scales were used to evaluate quit motivation and nicotine dependence, respectively. Based on a comprehensive patient approach, the pharmacist suggested a therapeutic plan to quit tobacco (pharmacological and non-pharmacological interventions). Nicotine replacement products, medication adherence and induction of prescription medicinal products were the main pharmacological interventions. Non-pharmacological interventions were motivational interviewing, and the promotion of strategies to reduce the number of cigarettes and to avoid concomitant risk factors. The interventions were directed both to patients or physicians. Referral to a physician occurred when diagnosis of a medical condition was required or when:
- Treatment with nicotine replacement products was inadequate.
- Spirometry was outside the normal values, without positive evolution from smoking cessation.
- An uncontrolled mental disease and/or another addiction were present.
- Strategies involving non-prescription medicines were exhausted.
In follow-up consultations and phone calls, all the pharmacist's interventions were evaluated and the therapeutic plan adjusted (if needed) until to achieve tobacco abstinence. Patients could leave the programme at any time and return later if a relapse occurred.
The effectiveness of pharmacist interventions was assessed by smoking cessation at endpoints: 1, 6 and 12 months after the patient's quit date. Mean values were expressed as mean ± standard error of the mean.
RESULTS
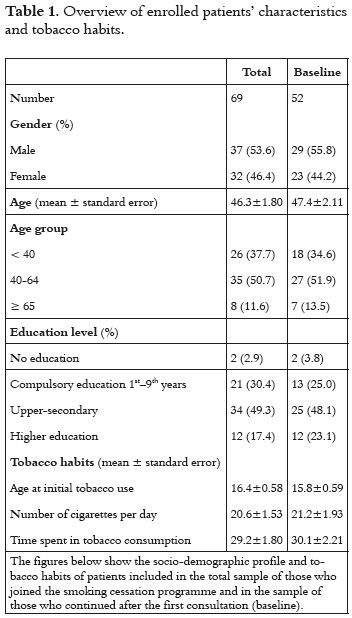
Between January 2009 and July 2014, 69 smokers joined the smoking cessation programme in the seven community pharmacies enrolled. Thirtyseven (53.6%) of these were male. The mean age was 46.3 ± 1.80 years old and the majority (50.7%) of smokers belonged to the age group between 40 and 64 years old. The upper-secondary school was the most prevalent educational level (49.3%). Almost 70.0% of the patients declared an active working situation. Table 1 shows an overview of patients' characteristics and tobacco habits. During the first consultation, 24.6% of the patients abandoned the programme. Of the remaining 52 smokers, 29 (55.8%) were male, with a mean age of 47.4 ± 2.11 years old. Among the patients, 48.1% had an upper-secondary education level, and 67.3% were actively employed. Dyslipidaemia (71.2%), overweight (61.5%) and anxiety (44.2%) were the most prevalent comorbidities (Table 1).
During the study period, 264 pharmaceutical consultations were performed, 5.2 ± 0.51 on average per patient, with a mean time for face-to-face follow-up consultations of 5.5 ± 0.76 months. According with the information registered at the first pharmaceutical consultation, in average, each patient initiated tobacco use very early (at 15.8 ± 0.59 years old) and consumed about 21.2 ± 1.93 cigarettes per day. A mean smoking time of 30.1 ± 2.21 years was registered (Table 1). Previous attempts to quit smoking were reported by 35 smokers (67.3%). More than 40% of the patients showed moderate motivation, and their nicotine dependence was classified as primarily low or medium (63.5%).
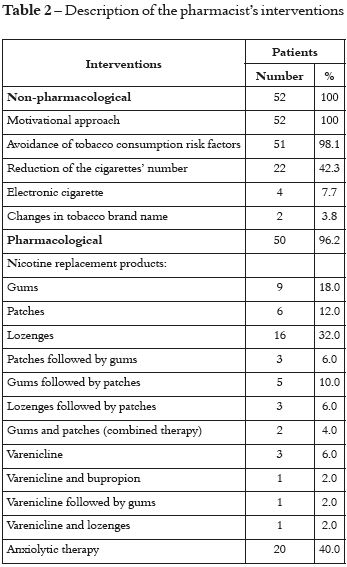
A total of 401 interventions were provided (7.7 ± 0.81 on average per patient), 395 (98.8%) were addressed to patients and 5 (1.3%) addressed to physicians. Pharmacological interventions represented 60.1% (n=241) of the total provided. Fifty patients (96.2%) decided to quit tobacco with the support of pharmacological methods. Nicotine replacement products were recommended in 92.0% of the cases. Oral pharmaceutical forms were the most utilised forms, while 13 patients used a combination therapy with transdermal delivery. Varenicline and Buproprion were prescribed to 6 patients, 1 before the patient joined the programme and the others after the pharmacist's referral. Anxiolytic therapy was required for 20 patients (40.0%), including prescribed medication or phytotherapy (non-prescription medicines). The most frequent non-pharmacological interventions were motivational interviewing used with all the patients, promoting the avoidance of risk factors (98.1%) and the reduction of daily cigarettes (42.3%). Table 2 summarized the pharmacist's interventions.
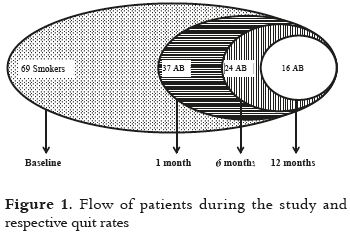
One month after patient's quit date, 37 of the initial 69 smokers had stopped smoking (53.6%). The quit rate decreased to 34.8% after 6 months and to 23.2% after 1 year. Figure 1 shows the flow of patients during the study and respective quit smoking rates.
At baseline, 69 smokers joined the smoking cessation programme (stippled area). Of these, 17 abandoned the programme during the first consultation. Of the 52 patients continuing in the programme, 13 reduced their number of cigarettes per day but dropped out before recording a quit date. Thirty-nine smokers recorded their quit date, with 2 relapsing before 1 month. Thus, 37 patients from the initial sample achieved abstinence 1 month after the quit date or 53.6% (vertical lines). Of these, 8 dropped out. Of the 29 remaining patients, 3 relapsed, and 2 patients had only 4 months of follow-up sessions. This means that 24 patients were still abstinent 6 months after their quit date or 34.8% (horizontal lines). Seven of these dropped out. Of the 17 patients that continued in the service, 16 patients remained abstinent for twelve months after their quit date or 23.2% (white area). Note: AB = abstinent patients.
DISCUSSION
Our study demonstrated that there is room to implement effective smoking cessation programs in Portuguese community pharmacies. The relative small number of smokers in our study may be due to lack of awareness of smoking cessation programmes assisted by a pharmacist, allied with a weak involvement of the pharmacies in tobacco control policies in Portugal.
The prevalence of tobacco use in Portugal and, in particular, in the Algarve and Alentejo regions is higher among males than females, showing a trend towards decreasing among men (10). This may explain the higher percentage of male patients in our sample, in spite of females being found to be more receptive to asking for help to quit smoking (11). The most prevalent age group in our sample matches the distribution of smokers in Portugal (10).
Our programme presented better cessation effectiveness rates than reported in the literature ( 4-6,12,13). Our quit rate of 53.6% after 1 month compares favourably with quit rates ranging from 22% (12) to 26% (5), and our quit rate of 34.8% after 6 months of abstinence is still higher than the previously reported quit rates of 25% (13) and 28% (6). Disappointing quit rates of 3.6% by 1 year after the quit date in other studies(12) contrast with our 23.2% quit rate. Our high success rates may be due to the close relationship established between the patients and the pharmacist and his easy availability (pharmacy and phone contacts). In addition, the measurement of several health parameters during consultations, namely spirometry and carbon monoxide tests, may have contributed also to additional motivation. However, we believe that a highly trained pharmacist who was focused on providing this service, as the specialized outsourced pharmacist, could result in substantial improvements in smoking cessation rates, also explaining our better outcomes.
A potential limitation of our study is the reduced number of patients and locations, what precluded generalization of the results. However, these preliminary results encourage us to proceed towards the main study with an increase in the number of patients and locations.
CONCLUSION
Based on these preliminary results, the implementation of an outsourced smoking cessation programme in community pharmacies using a highly-trained external pharmacist may contribute effectively to tobacco cessation in Portugal..
REFERENCES
1. World Health Organisation. Tobacco - Fact sheet nº 339. Updated May 2014. Available on http://www.who.int/mediacentre/factsheets/fs339/en/ (Accessed 4 October 2014). [ Links ]
2. World Health Organisation. WHO global report: mortality attributable to tobacco. 2012. Available on http://whqlibdoc.who.int/publications/2012/9789241564434_eng.pdf?ua=1 (Accessed 4 October 2014). [ Links ]
3. Direção-Geral da Saúde. Portugal: Prevenção e Controlo do Tabagismo em Números - 2013. Programa Nacional para a Prevenção e Controlo do Tabagismo. 2013. Available on http://www.dgs.pt/estatisticas-de-saude/estatisticas-de-saude/publicacoes/portugal-prevencao-e-controlo-do-tabagismo-emnumeros-2013.aspx (Accessed 5 October 2014). [ Links ]
4. Saba M, Diep J, Saini B, Dhippayom T. Meta-analysis of the effectiveness of smoking cessation interventions in community pharmacy. J Clin Pharm Ther 2014; 39(3):240-7. [ Links ]
5. Costello M, Sproule B, Victor J, Leatherdale S, Zawertailo L, Selby P. Effectiveness of pharmacist counselling combined with nicotine replacement therapy: a pragmatic randomised trial with 6,987 smokers. Cancer Causes Control 2011; 22(2):167-80. [ Links ]
6. Dent L, Harris K, Noonan C. Randomized trial assessing the effectiveness of a pharmacist-delivered programme for smoking cessation. Ann Pharmacother 2009; 43(2):194-201. [ Links ]
7. Direção-Geral da Saúde. Cessação tabágica. Programa-tipo de actuação. Gradiva. 2007. Available on http://www.dgs.pt/upload/membro.id/ficheiros/i009774.pdf (Accessed 28 November 2014). [ Links ]
8. Richmond RI, Kehoe LA, Webster IW. Multivariate models for predicting abstention following intervention to stop smoking by general practitioners. Addiction. 1993; 88(8):1127-35. [ Links ]
9. Ferreira PL, Quintal C, Lopes I, Taveira N. Teste de dependência à nicotina: validação linguística e psicométrica do teste de Fagerström. Rev Port Saúde Pública. 2009;27(2):37-56. [ Links ]
10. Machado A, Nicolau R, Dias C. Consumo de tabaco na população portuguesa retratado pelo Inquérito Nacional de Saúde (2005/2006). Rev Port Pneumol 2009; XV(6):1005-27. [ Links ]
11. Aguiar M, Todo-Bom F, Felizardo M, Caeiro F, Sotto-Mayor R, Bugalho de Almeida A. Casuística de quatro anos de um consulta de apoio ao fumador. Rev Port Pneumol 2009; XV:179-97. [ Links ]
12. Bauld L, Boyd K, Briggs A, Chesterman J, Ferguson J, Judge K, et al. One-year outcomes and a cost-effectiveness analysis for smokers accessing group-based and pharmacy-led cessation services. Nicotine Tob Res 2011; 13(2):135-45. [ Links ]
13. Khan N, Anderson J, Du J, Tinker D, Bachyrycz A, Namdar R. Smoking cessation and its predictors: results from a communitybased pharmacy tobacco cessation programme in New Mexico. Ann Pharmacother 2012; 46(9):1198-204. [ Links ]