Introduction
Continuous comprehensive care with patients requires a common language between nursing healthcare. In this context, the use of NANDA International Inc. (NANDA-I) taxonomy stands out internationally. The Nursing Diagnoses of NANDA-I are based on the diagnosis of human responses through clinical reasoning in which needs are identified and treatment and prevention strategies proposed. These answers can be based on potential or real problems 1.
As for the care of patients with susceptibility to decreased cardiac tissue perfusion (DCTP), we identify the nursing diagnosis risk for decreased cardiac tissue perfusion (00200) in the taxonomy. To assist in the development of NANDA-I Taxonomy II, two recent surveys have proposed and validated 2,3 the ND of DCTP, presenting acute coronary syndromes (ACS) as the most common associated condition. These works also discuss the relationship of DCTP with other diagnoses concerning Domain 4 - Activity/Rest, Class 4 - Cardiovascular/Pulmonary responses, such as decreased cardiac output and activity intolerance.
Rethinking care with a focus on NDS is still a major challenge for nurses, where we highlight two points. First, because the focus on the disease is the prevailing approach. Second, because we find it difficult to think both of care as a continuum and on the interrelationships among NDS, especially when we think of risky and real NDS.
Several studies focusing on nursing diagnosis have been developed 4-6, especially when we think about real NDS. Thus, the mains objectives of this research were to identify the nursing diagnoses of risk for decreased cardiac tissue perfusion (RDCTP) [code: 00200] and risk for activity intolerance (RAI) [code: 00094] and to establish the relationship between the components of these diagnoses and the signs and symptoms of DCTP. As a specific objective, we seek to characterize the sociodemographic and clinical profile of the studied population. NDS were chosen for this research since they are frequent in the clinical practice of nurses and because they remain little studied subjects that could contribute to better subsidize health care planning.
Materials and methods
Design
This is an observational, associative, quantitative, and cross-sectional study derived from a clinical construction validation study based on accuracy test models 3. The research scenario comprised the emergency, hospitalization, intensive care, and hemodynamic units in Brazil.
Participants and sample
The inclusion criteria for the study established the selection of patients aged 18 or older with a medical diagnosis of ACS and who were in the acute phase of the disease. Patients who did not present the clinical condition (signs and symptoms) at the time of admission or who had undergone reperfusion therapy before admission to the service were excluded from the study. Eligible patients were informed before discharge and enrolled in the study.
As the present study is derived from primary research to verify the accuracy of the nursing diagnosis regarding DCTP in patients with ACS 3, sample size calculation considered the clinical construct validation methodology for the latent class analysis 7.
The latent class analysis is used to calculate accuracy measures (sensitivity and specificity) of clinical indicators when there is no perfect reference standard. For this reason, the sample size may vary from 5 to 30 individuals for each defining characteristic 7. Therefore, considering that the ND of DCTP has 15 defining characteristics, a total of 5 patients were considered per each defining characteristic, totaling 75 patients 3.
Data collection
Data collection with patients and medical records occurred from August 2018 to February 2019. This process was carried out by a nurse and a nursing senior student.
In order to standardize data collection, conceptual and operational definitions for each component of the NDS under study were developed as a protocol. This construction was submitted to the appreciation of three judges through a focus group. These were nurses, teachers, and researchers in the area of Standardized Language System or cardiology and with experience in caring for patients with ACS. The protocol was adjusted according to the consensus of the discussion group and was used by the research team to reduce the evaluation and instrument bias. In addition, to decrease the evaluation bias related to measurement accuracy, the research team carried out a theoretical-practical training of eight hours to apply the instrument built for the collection of data and to carry out the physical examination in a standardized way. After a pre-test with five patients, who were not included in the final version, it was possible to verify the adequacy of the data recording instrument to start data collection.
Interviews included questions about patients' baseline sociodemographic characteristics and social background: sex, age, marital status, education, employment status, family income, and number of inhabitants per household. Data regarding the presence of risk factors for ACS (arterial hypertension, diabetes mellitus, smoking, dyslipidemia, and obesity) and others risk factors were also collected, following the protocol previously defined. In this case, for example, an open-ended question about the factors that could lead to ACS was formulated, so the examiner could check which risk factor(s) were known to patients and thus minimize bias in the instrument. Data regarding the associated conditions and whether patients fit into risk populations for the NDS under study were investigated in medical records.
To complement data collection, we sought medical records information on clinical indicators of DCTP on admission, as recommended by Santos et al.2 and validated by Gonçalves et al.3, namely: angina, pain score higher than seven, electrocardiographic changes, arrhythmia, altered cardiac enzymes, dyspnea, irradiation of pain to shoulder and jaw, pain duration for less than ten hours, nausea, altered blood pressure, dizziness, vomiting, pulmonary rales, altered heart rate, and third heart sound.
The diagnostic inference was carried out independently by a nursing student, a nurse specialized in cardiology, who is also enrolled in a master's degree, and a nurse doctor and researcher in the study area, all of them with broad knowledge of nursing taxonomies. This helped to limit the spectrum bias, referring the researcher to determine which patient has a diagnosis through their perception of patient impairment. Each evaluator received the clinical information of all patients in an Excel software spreadsheet. Afterwards, the agreement reached by the three evaluators was used as the gold standard for the presence of NDS, as in the study by Oliveira et al.8.
Data analysis
All statistical analyses were performed in SAS, version 9.4. Descriptive analysis was presented using means, standard deviation (SD), median, and range for continuous variables. Categorical variables were expressed as numbers and percentages. The Shapiro-Wilk test was used to verify the normality of the data. Pearson's Chi-square test or Fisher's exact test was used for associative measures of categorical data.
Multiple Poisson regression models were constructed with robust variance, considering the two NDS studied as dependent variables. In these models, prevalence ratios and their confidence intervals and p-values were presented 9. A significance level of 5% was adopted for all tests.
Results
Patients' sociodemographic characteristics are shown in Table 1.
Table 1 Patients' baseline demographic characteristics
Source: authors, based on research data.
The study included 75 patients with ACS, with an average age of 60.2 years (SD = 10.4), in age ranges from 36 to 86 years, and who in most cases were married (65.3%). There was a prevalence of men among the sample (72%). About 54.2% of patients did not complete elementary school, the average monthly family income was 2.7 minimum wages (SD = 1.5), and the number of inhabitants/household was in mean 1.9 (SD = 1.7), with a range from 1 to 9. Besides, 30.7% of the sample was aged 65 years or over, and 84% had a history of cardiovascular disease.
As for ACS risk factors, we highlight that 72% of participants reported living with arterial hypertension, 54.7% were active or passive smokers, 45.3% had diabetes mellitus, 40% dyslipidemia, and 12% were obese. This way, all the indicators of DCTP were evidenced in this sample. The NDS and their elements are shown in Table 2.
Table 2 Frequency of nursing diagnosis of risk for activity intolerance and risk for decreased cardiac tissue perfusion
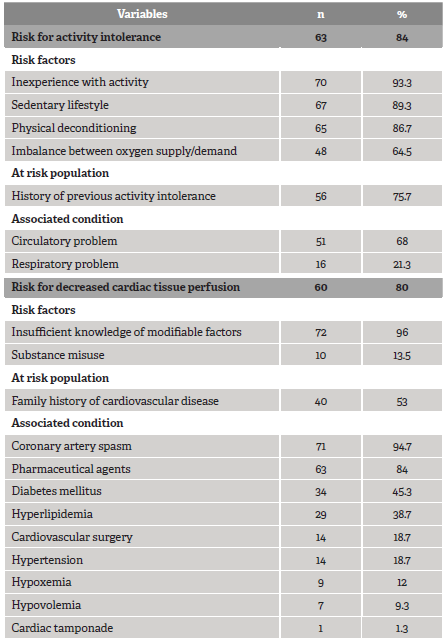
Source: authors, based on research data.
Related to RAI diagnosis, all the risk factors of this condition were present in more than 50% of the individuals in the sample, except for the immobility risk factor, which was not identified in any of the participants. As for the risk of DCTP, 96% of the participants had insufficient knowledge about modifiable risk factors (e.g., smoking, sedentary lifestyle, obesity) and 94.7% had artery spasms associated with this coronary ND.
Table 3 shows the significant diagnostic inferences between risk factors, associated conditions, population at risk, and the presence or absence of the corresponding nursing diagnosis. Table 4, in turn, presents the multiple Poisson regression models.
Table 3 Analysis of associations of nursing diagnoses of risk for activity intolerance and risk for decreased cardiac tissue perfusion with risk factors, associated conditions, and at-risk population
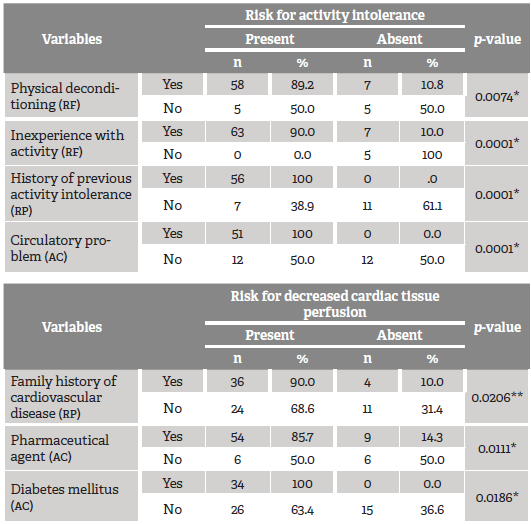
*Fisher test. **Chi-square test. RF = Risk factor; AC = Associated conditions; RP = At-risk population.
Source: authors, based on research data.
Table 4 Multiple Poisson regression models

* PR = Prevalence ratio, the probability of presenting the result "Yes" was estimated. ** In relation to the set of variables, the evaluation of the multiple Poisson regression models only considered the male sex as the reference for the variable, since there is a higher prevalence of ACS among the participating male population. CI = Confidence interval; LL = Lower limit; UL = Upper limit. Bold indicates the significance at p <0.05.
Source: authors, based on research data.
It was observed that patients admitted at RAI and dyspnea were 1.32 times more likely to develop a diagnosis of activity intolerance. For the risk of decreased cardiac perfusion, those who did not have dyspnea and pain duration for less than ten hours were more likely to develop such diagnosis. Finally, in those who did not report pain irradiation the probability of having this diagnosis decreased by 47%, compared to those who had this symptom.
Discussion
Population aging and the increase in chronic diseases are important factors in the growing prevalence of ACS, as reflected in the sociodemographic characteristics collected by this study 10-12. Corroborating the findings of other studies, participating patients showed hypertension, diabetes mellitus, dyslipidemia, and other cardiovascular diseases. We also found that smoking and obesity are associated risk factors 13-16. Due to the absence of studies that analyzed the elements of the two NDS studied in the population chosen for this study, we made comparisons with studies that performed an analysis in patients with a phenomenon often installed, which demands the importance of early assessment.
Research with stable heart disease patients identified 13 NDS, where lifestyle (00168) and activity intolerance (00092) stand out. However, RDCTP (00200) and RAI (00094) presented less agreement between specialist nurses 15, which shows the difference between NDS of the acute, subacute and chronic faces. The evidence of activity intolerance (00092) shows that the presence of dyspnea on exertion, fatigue, the imbalance between oxygen supply and demand, stress discomfort, and the presence of angina is a common feature 15.
The insufficient knowledge of modifiable factors was identified in a more significant percentage of the patients in this sample who were diagnosed with RDCTP. The correct adherence to treatment and the rapid conduction in emergency cases are affected by the lack of knowledge about ACS risk factors, as well as by failure in identifying the signs of the ischemic event in heart diseases 17,18.
In this context, knowledge about risk factors needs to be addressed in primary and secondary care services. The prioritization of the approach to drug therapy in consultations results in a lack of knowledge about heart disease as a whole by the population, a fact observed in a study with patients with ACS 18.
In nursing appointments, RDTP increases when there is a family history of cardiovascular disease or diabetes mellitus, accompanied by the use of drugs that act on the heart pump. Concomitant with these factors, early non-adherence to treatment and lack of therapeutic continuity increases the chances of the patient developing again DCTP.
In this study, the defining characteristics of DCTP were observed in patients at the time of admission to the emergency department, showing a relationship with the determination of risk diagnoses. In other words, the accurate and precise identification of clinical parameters is essential for making diagnostic and therapeutic decisions with potential impacts on the evolution of the patient.
As previously stated 3, patients with ACS showed angina (100%), pain score higher than seven (81.3%), electrocardiographic changes (82.4%), arrhythmia (78%), altered cardiac enzymes (76.4%), dyspnea (61.6 %), radiation to shoulder and jaw (55.4%), pain for less than ten hours (53.3%), nausea (45.3%), altered blood pressure (30.7%), dizziness (29.3%), vomiting (26.7%), pulmonary rales (18.9%), altered heart rate (14.7%), and third heart sound (4%).
Another point to be explored is the relationship between the presence of ACS and increased risk of functional decline, which leads to an increased chance of hospital readmissions and death in elderly patients, as well as impacts on their quality of life 19,20. Thus, it is evident the gap that needs to be addressed during early stages, through intervention studies aimed at promotion, disease prevention, and rehabilitation of patients at risk, thus favoring the non-development of problem-focused NDS 15.
In the context of hospital discharge of patients with RDCTP and RAI diagnoses, it is necessary to continue with rehabilitation mediated by a multidisciplinary team in patients' home environment. Therefore, the complete evaluation, with the introduction of elements of the measure of functionality, should be prioritized, especially when considering individuals with multiple morbidities and the elderly 20. Based on the data collected, the importance of investigating the patient's previous and current functional status during hospitalization is a remarkable finding that will contribute to reducing the impacts on rehabilitation.
Linked to the elements of physical deconditioning and inexperience with activity, the ability to walk is a crucial point to be evaluated.
A possible explanation for this fact would be the relationship between the loss of microvascular perfusion after ACS, which is responsible for the supply of oxygen and nutrients to the tissues, and the continuity of ischemia and the development of adverse clinical results 21.
In another study, it was observed that the limitations in performing basic activities of daily living started eight years before the acute event 22. That is the period in which interventions for RDCTP and RAI could have started, considering the presence of risk factors, thus corroborating the findings of our study regarding the association of NDS and the RAI and the history of previous activity intolerance element.
However, faced with the evidence of low adherence to health promotion and disease prevention activities, the possibility of a decline that may affect the area of cardiac rehabilitation becomes a concern. At home and in the primary care setting, cardiac rehabilitation could contribute to improving and maintaining physical activity habits and increasing cardiorespiratory fitness and survival, thus reducing the risk of mortality 23.
It should be noted that in the current study sample all risk factors for RAI were identified, although only in association with inexperience with activity, and imbalance between oxygen supply/demand. On this regard, a study whose objective was to verify the prevalence of ND sedentary lifestyle and the defining characteristic of physical deconditioning in patients with ACS reported a frequency of 56.1 and 46.8%, respectively 24.
In the case of appearance of these two elements, there is a higher chance of systemic, muscular, respiratory, cardiovascular, and articular changes, and, consequently, activity intolerance, which might cause a new episode of DCTP 15. As for RDCTP, all the constituent elements of NDS were identified in the sample studied. According to the research study by Moreira et al.25, in which 1,542 adult patients were monitored for seven years after percutaneous coronary intervention, 12.1% of the sample developed DCTP, listing advanced age, multivessel disease, and complications of the intra-procedure injury as predictor of such a condition. These outcomes reinforce the need for continuous monitoring of the population at risk.
The care of patients with DCTP should be focused on health promotion and risk prevention in light of their basic psychosocial and psychobiological human needs. The results found in this study reinforce this claim. The importance of early identification of risk diagnosis and risk factors was also observed though this research. Therefore, diagnosing these risk factors significantly contributes to the care and prevention of ACS complications.
We should mention as a limitation of this research that it is a cross-sectional study, leading to the observation of some characteristics only in a single moment, which could compromise the reading of the phenomenon. Besides, due to the use of a sample for convenience in a single hospital, our findings may not be generalized.
Conclusion
The nursing diagnoses of RAI and RDCTP were present in 84 and 80% of patients with DCTP, respectively.
When verifying the relationship between the risk factors and the NDS studied, we found an association of the use of pharmacological agents, the presence of diabetes mellitus, and family history of coronary disease with RPCD. In the case of RAI, this reports an association with lack of physical conditioning, previous history of activity intolerance, inexperience with activity, and circulatory problems. Finally, RPCP is associated with pharmacological agents and dyslipidemia.
The absence of evidence of DCTP such as dyspnea, radiation to shoulder andjaw, and arterial pressure, and pain for less than ten hours acted as protective factors for the development of the studied risk diagnoses.
To conclude, considering the high cardiovascular vulnerability of patients with ACS to nursing diagnoses through the NANDA-I domain Class 4, we recommend further studies to determine the predictive power of the risk diagnoses evaluated by ND from a problem-centered approach.















