Introduction
Leclercia adecarboxylata is a member of the Enterobacteriaceae family, it is phenotypically similar to Escherichia coli, differentiated in 1986 by Tamura et al1,2. It is thought to be present widely in nature and it is a rare cause of disease in humans, with an antimicrobial susceptibility ranging from natural resistance to multiple antibiotics3, to multidrug resistance due to the production of several enzymes4-6. We report the first known case of infection by this microorganism related to trauma with plant material, a review of reported cases around the world with interesting clinical manifestations, natural antimicrobial susceptibility and acquired resistance patterns are also presented.
Case Report
A 69-year-old male patient, with medical history of Diabetes Mellitus type 2, presented to the emergency department of a hospital in Bogotá, Colombia, after losing his postural tone and hitting his head to the ground, with no consciousness loss, motor or sensitive alterations, vomiting or other relevant symptoms afterwards. At initial examination, the patient had a heart rate of 71 beats per minute, a respiratory rate of 19 breaths per minute, blood pressure of 169/97 mmHg, temperature of 36°C, blood glucose of 350 mg/dL, a hematoma on the right frontal zone of the head and a 4*4 cm erythematous, indurated, painful lesion with abundant purulent secretion, that limited the metatarsophalangeal flexion of the third, fourth and fifth fingers of the right hand, with no other relevant findings.
The patient was then asked about the injury on his right hand, and he referred that five days before consultation, he was at his country house (Carmen de Apicalá, Tolima, Colombia) carrying some wooden logs, when he stumbled and fell, hurting his right hand with the logs he was carrying, with subsequent abundant bleeding and edema; the patient grabbed his medic kit and cleaned the lesion with hydrogen peroxide (H2O2), he checked for foreign objects and applied a bandage on his hand. Three days before consultation, the patient noticed edema, pain, fetid smell and movement limitation of his right hand. After removing the bandages, he found blood stains and purulent secretion, he drained the lesion and massaged his hand with an ointment made of coke and marihuana leaves; on the day of consultation, although it was not the reason for his attendance to the hospital, the lesion had progressed, as described before.
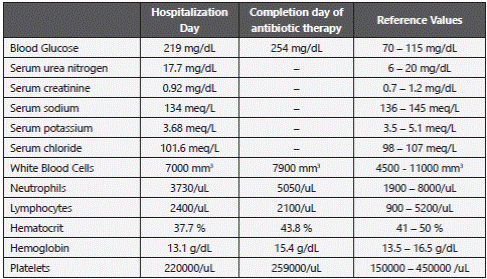
On the emergency room, they started intravenous Oxacillin, 2gr every four hours, in continuous infusion, received Tetanus prophylaxis (single IM dose) and requested an X-ray from his right hand, which had no abnormalities, a Computed Axial Tomography of the head, both with no abnormalities, and blood analysis (Table 1).
The patient was assessed by the orthopedist, who considered he was a candidate for surgical drainage and debridement, he suspended the infusion of oxacillin and started intravenous Ampicillin/Sulbactam, 1.5gr every 6 hours, and ordered his hospitalization. During the surgical procedure, an abscess of 8cc of purulent secretion was drained, a small foreign object (apparently vegetal) was extracted, samples for culture were taken and the wound was washed thoroughly with 1000cc of 0.9% saline solution and H2O2, finally the wound was sutured and covered with a nitrofurazone gauze and a bandage.
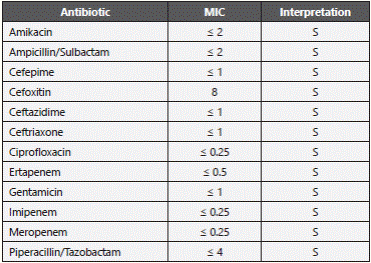
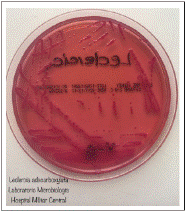
The patient had fluctuant glycemia, thus he was assessed by the internist, who started basal insulin therapy, with an adequate response. Five days after the surgical intervention, Leclercia adecarboxylata was identified using the VITEK® 2 system healthcare with a probability of 96% showing a natural antimicrobial resistance pattern (Table 2). We tested the isolated strain 4 times in our laboratory for certainty, all of which resulted positive for the same microorganism (Figure 1). The patient completed 10 days with intravenous Ampicillin/Sulbactam 1.5 grams IV every 6 hours, he had no need for a second surgical intervention, achieving clinical recovery and recovering full functionality of his hand.
The strain was sent for extra institutional confirmation to bioMérieux in Bogotá, Colombia, where they used a Matrix Assisted Laser Desorption/Ionization-Time of Flight (MALDITOF) mass spectrometer (MALDI TOFVITEK® MS) to confirm the results yielding a trust percentage 99.6% and thus confirming the identification of L. adecarboxylata.
Discussion
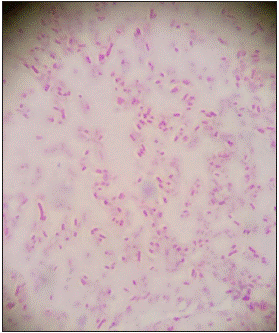
Leclercia adecarboxylata, described by Leclerc in 1962 and first designated as “Enteric group 41” or “Escherichia adecarboxylata”, is a Gram-negative, oxidase-negative, indole-positive, facultative-anaerobic, motile bacillus, member of the Enterobacteriaceae family, that is phenotypically similar to Escherichia coli1,3,7; it was differentiated in 1986 by Tamura et al. through DNA hybridization, biochemical and computer identification tests, resulting in a new genus1,2. L. adecarboxylata is thought to be distributed widely in nature, present in food, water sources, egg shells, milk, industrial fat and oil reservoirs and as a commensal of the gut flora of some animals1,3,7-9; it has also been recovered, uncommonly, from human samples like blood, bone10, cardiac valve, wounds, bronchial wash11, peritoneal fluid, urine, gall bladder, synovial fluid, abscesses and epididymo-orchitis, from immunocompromised and immunocompetent patients, being the former the most relevant and frequent scenario, as the case of our patient, and the later generally but not always associated to polymicrobial infections, suggesting the dependence of this bacteria on other microorganisms to infect immunocompetent hosts1,7.
Zapor et al.7 reported the case of a 25-year-old soldier who was wounded in Afghanistan by an improvised explosive device, with a subsequent prolonged hospital stay and multiple surgical interventions; after being discharged the patient consulted again due to limited right hip range of motion, during surgical intervention they found a focal collection in the right buttock with the isolation of L. adecarboxylata by BD Phoenix Automated Microbiology System and confirmed by 16s ribosomal sequencing, due to in-vitro resistance of the strain to Amoxicillin/Clavulanic acid, Ampicillin/Sulbactam and Cefazolin, the patient was successfully treated with orally Ciprofloxacin, 750 mg twice daily, for 10 days. Keren et al.12 reported the case of a 46-year-old male patient who suffered a laceration at the dorsum of his left foot with a surfboard fin while surfing, developing a soft-tissue infection, with the identification, using VITEK® 2 systems as in our case, of L. adecarboxylata and Enterobacter cloacae, successfully treated with oral Ciprofloxacin for 14 days. Sanchez Porto et al.2 reported the case of a 56-year-old female with Metabolic Syndrome and Diabetes Mellitus type 2, with a burn wound located in the left pre-tibia extremity with an open ulcer and signs of infection, with the identification in three sets of blood culture and a swab culture of the exudate of L. adecarboxylata by Microscan Automatic identification System, confirmed by API 20E System (bio-Mérieux, Marcy l’Etoile, France), successfully treated with Amoxacillin/Clavulanic acid 1 gram IV every 8 hours for seven days, then orally 875/125 mg every 8 hours for 7 additional days. Corti et al.13 reported the case of a 37-year-old male patient that was involved in a major motor vehicle accident with multiple injuries, including Gustillo-Anderson type II open fracture of the left distal femur, type IIIB open fracture of the left distal tibia with bone loss and mangled left foot with multiple fractures and extensive soft-tissue involvement, no farm contamination expected as he was rescued on the road, with the isolation from several surgical samples of the wounds of L. adecarboxylata and Enterobacter amnigenus, successfully treated with Piperacillin/Tazobactam 4.5 grams three times a day. To our knowledge, our patient is the first report of infection by Leclercia adecarboxylata after a trauma with plant material (logs), in an immunocompromised patient (Diabetes Mellitus type 2), not associated to other microorganisms, successfully treated with a course of 10 days of Ampicillin/Sulbactam 1.5 grams IV every 6 hours for 10 days. (Figure 2)
L. adecarboxylata has natural resistance to fosfomycin3. Natural resistance of L. adecarboxylata to fosfomycin may represent an additional parameter for its reliable phenotypic separation from E. coli.15,16In the case of our patient, we isolated a strain with a usual susceptibility pattern, however there are reports in the literature of L. adecarboxylata strains expressing diverse acquired resistance mechanisms. Sun et al.6 describe the production of plasmid-encoded NDM-1 from a L. adecarboxylata strain (P10164) isolated in 2012 from the sputum of a 43-year-old male with pneumonia in Chongqing City in China, which not only harbored the bla NDM-1 gene, but also other genes conferring resistance, as bla CTX-M-1 group, bla TEM and bla OXA-1 group genes and showed in-vitro resistance to all of the tested drugs. Papagiannitsis et al.5 during a study of hand hygiene among the staff of the Na Homolce Hospital, Prague, Czech Republic, found a strain of L. adecarboxylata, identified by matrix-assisted laser desorption-ionization time of flight mass spectrometry and confirmed through 16s rRNA gene sequence, with a plasmid that contained the bla- VIM-1 gene, with the ability of conjugal transfer to the E. coli A15 strain. Shin et al.14 isolated a strain of L. adecarboxylata from blood cultures of a patient with breast cancer with a peripherally inserted central catheter for chemotherapy administration, identifying through PCR assays the presence of bla TEM-1, bla CTX-M-3 and intl1 with dfrA12 and aadA2 (resistance to trimethoprim-sulfamethoxazole and aminoglycosides, respectively) genes in such strain. Finally, Geffen et al.4 isolated a strain of L. adecarboxylata in Laniado Medical Center, Israel, from rectal surveillance cultures of patients, identified using VITEK-2 system and confirmed by 16s rDNA aequencing, with a plasmid carrying the bla KPC-2 gene.
Conclusion
Although Leclercia adecarboxylata is an uncommon infecting microorganism, it must not be forgotten in the clinical and epidemiological setting, as it is capable of carrying and expressing different mechanisms of resistance, reducing therapeutic options and threatening to alter the antimicrobial susceptibility of the flora in healthcare facilities and the community, as it has been isolated from the skin of healthy human beings, resulting in the spread of the microorganism and, if hand sanitation adherence is not adequate, its acquired resistance genes.
It is possible that infections caused by this microorganism have been under-reported due to its similarities with Escherichia coli, a situation that gains relevance in the setting of urinary tract colonization/infection, as the innate resistance of L. adecarboxylata to fosfomycin, threatens the effectivity of therapeutic/prophylactic regimens with this drug.
To our knowledge, this is the first reported case of the association between trauma with plant material (logs) and infection by Leclercia adecarboxylata in an immunosuppressed patient. It is important to take into account this way of inoculation, being a rather common event in the daily routine of thousands of people around the globe, that added to an underlying condition, immunosuppression or even an immunocompetent state, can result in a soft tissue infection as the case of our patient, a bone infection or even pneumonia or endocarditis.