Introduction
Intestinal parasitism is considered an infectious disease of public health importance, affecting one fourth of the global population1 of all ages and both sexes, predominantly in underdeveloped, tropical and subtropical countries2. The prevalence varies greatly according to weather, sanitation, social and economic factors3,4. Mortality rates from intestinal parasites is low, however, the morbidity can be high, thus it implies high healthcare costs5. It is associated to intestinal malabsorption, abdominal pain, diarrhea, lower growth and labor incapacity6.
The location and weather conditions of Colombia, enable the propagation and acquirement of intestinal parasitism7, especially in isolated areas such as Guachene8,9and Urabá, where unfavorable sociodemographic factors contribute to poor sanitary conditions. Furthermore, abdominal pain and diarrhea are among the main complaints in the ambulatory scenarios of these regions.8,9.
Few nationalwide studies have been conducted in Colombia reporting the prevalence of intestinal parasitism, most assays available have reduced samples and are on pediatric or native communities; with a shortage in data of the frequency in adults, whom are an important source of transmission to children. The Colombian Minister of Health reported results of a national survey of parasitism in school population, this report concluded that 62.4% of the 1604 children of 7-10 years old were parasited for geohelmints and protozoa10.
This study intends to find the frequency of intestinal parasites among adults from a determined population with high risk of developing infection, and foresee possible associations with socioeconomic and demographic conditions and symptoms.
Methods
This observational, analytical, cross-sectional study was performed with a non-probabilistic sample, and carried out in the Colombian regions of Quibdó (Chocó), Urabá (Antioquia) and Guachené (Cauca), where continue endemic cases and outbreaks of gastrointestinal disease are reported. We carried out a survey to patients with water-foodborne disease who attended emergency services during 2009 and 2010 period and their household contacts, for a total of 284 volunteers. The sample was chosen for convenience, we included volunteers over 18 years old.
Ethics
This project was approved by the ethical commiittee of the Instituto Colombiano de Medicina Tropical as the minnimal risk according to the Helsinki´s Ethical Principles for Medical Research Involving Human Subjects (https://www.wma.net/policies-post/wma-declaration-of-helsinki-ethical-principles-for-medical-research-involving-human-subjects/). An informed consent was obtained from each participant declaring the procedures, risks, and purposes of the study. Subsequently trained personal directed a specific questionnaire to each volunteer to collect data on clinical and socio demographic information.
Samples
Plastic containers were distributed and guidance on stool sample collection offered. Samples were stored and processed according to international laboratory standardized protocols determined by the World Health Organization1. The samples were processed by stool concentration technique11 and were examined microscopically by experts from the Instituto Colombiano de Medicina Tropical for ova and cysts of parasites.
The data collected was analyzed using IBM SPSS Statistics 21.0 (https://ibm-spss-statistics.softonic.com/). To determinate prevalence ratio (PR) Chi square test or Fishers exact test were used. Variables selected for their relevance and statistical significance in the bivariate analysis were introduced into a logistic regression to determinate which of the variables had the strongest association with the infection. (Adjusted odds ratio [OR] with 95% confidence internal). Statistical significance was considered when p values were less than 0.05. The power of the study was recalculated because of the inaccurate confidence intervals and a power of 66.4% was determined with 95% confidence, hence the results should be interpreted with caution. Besides due to the way the study sample was collected the data from the study cannot be extrapolated to the general population.
Results
Sociodemographic characteristics
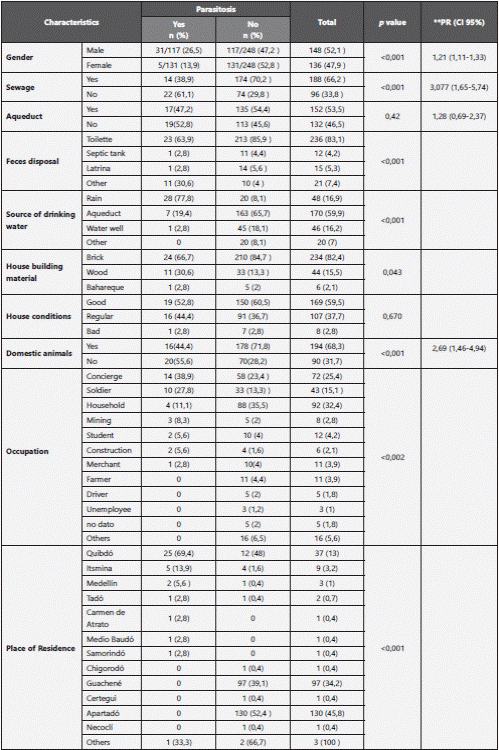
A total of 284 volunteers were enrolled in the study, among them 52.1% were males. The average age of the participants was 34 years (SD: 14.7), and the youngest patient was 19 years old. The 93% of the surveyed patients inhabited in the cities of Apartadó, Guachené and Quibdó. (Table 1)
Clinical manifestations and Laboratory findings
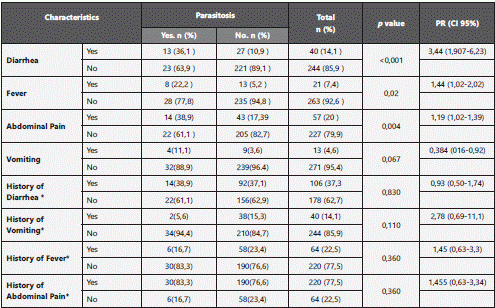
We found that 63.2 % of the infected patients were symptomatic, presenting either one or more of the following: diarrhea, fever, abdominal pain. Significant association was established between intestinal parasites and diarrhea (p=0,001), abdominal pain (p=0,004) and fever (p=0,002) Furthermore, there was no statistical association between parasitism and vomiting, history of diarrhea, fever or antibiotic use during the previous month. (Table 2).
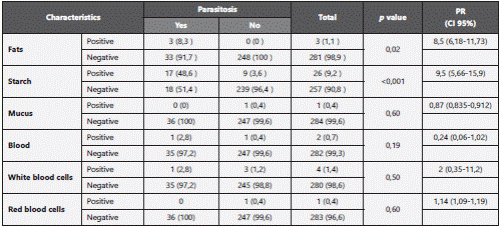
Laboratory findings in fecal samples related to parasitic infections were: presence of fats and starch; but there was not significant association with red blood cells, white blood cells, mucus or blood (Table 3).
Intestinal Parasites
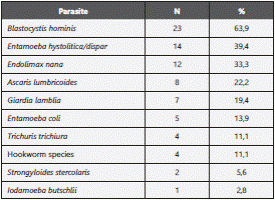
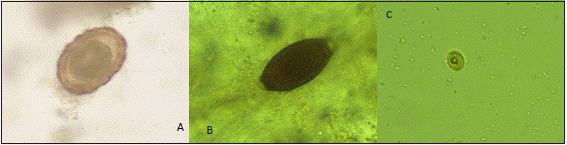
The frequency of intestinal parasitism found in the studied population was of 14.5 % (n=36), from which 39.5% had single parasitic infection and 60.5% had multiple parasites. Blastocystis hominis was the most frequently found parasite in 63.9% of the infected samples, followed by Entamoeba histolytica/dispar 39.4%, Endolimax nana 33.3%. Other parasites were found in much lower figures (Table 4). We did not find the following parasites in the collected samples: Taenia solium, T. saginata, Hymenolepis nana, H. diminuta, Balantidium coli or Enterobius vermicularis (Figure 1).
Associated factors
The bivariate analysis showed significant association of intestinal parasites with: gender, sewage, fecal disposal, source of drinking water, house building material, domestic animals, occupation and place of residence (Table 1)
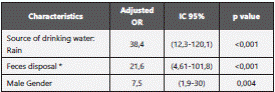
According to the multivariate analysis the variables that forecast the presence of intestinal parasites were: male gender, rainwater as drinking source and fecal disposal different from toilet, latrine or septic tank (Table 5).
Discussion
The present study showed a frequency of intestinal parasitism of 14.5% in an adult population from vulnerable areas of Colombia. The sample selected was a convenience andnon-probabilistic, which restrained the calculation of a prevalence and allowed only to determine the frequency of intestinal parasites in the study group. The findings contrast with previous studies conducted in other regions from the country. For instance, a study conducted during 2004 among population with poor sanitary conditions from all ages, including children from the Atlantic coast showed higher prevalence (92%) of intestinal parasitic infection than in the current study12.
Furthermore, prevalence gathered from school children in different regions of Colombia ranged from 47% to 84%.4,13-15. It must be taken into consideration that over the years the prevalence of intestinal parasitism has been decreasing in the Colombian territory, from 81,1% in 1965-8016, to 54, 6% for the period 2000-0517. Likewise, the actual results could be the illustration of the decline in the prevalence of the infection with time.
Moreover, the contradictory report on the frequency of intestinal parasitic infection could be explained because preceding studies were predominantly conducted among children which are at risk of infection. On the other side, the frequency could be underestimated due to the lack of serial sampling (three fecal samples).
Consistently with evidence from similar studies3,15and medical literature the most frequent microorganism found was Blastocystis hominis (63,9%), whose pathogenicity is still under investigation18. B. hominis infection must be correlated with presence of other parasites, chronicity of the infection and immune status of the patient in order to determine whether the microorganism is the source of the symptoms, and if treatment of the patients is necessary 19,20. The infection with B. hominis has epidemiological importance as reference for hygiene conditions, since other parasites of clinical relevance share the same vehicles of transmission. Other protozoos were frequent causes of parasitosis in this study group, E. histolytica/dispar (39.4%), E. nana (33.3%), and Giardia lamblia (19.4%), in contrast the geohelmints were less frequent. Current results in this adult population contrast with previous data reported in Colombian children, which is more frequent find geohelminths; Ascaris lumbricoides (16-73%), Trichuris (23-72%) were reported in the national study for parasitosis in scholar population10.
The majority of the infected volunteers (63.2%) were symptomatic and significant association was established between diarrhea (p<0,001), abdominal pain (p<0,004) and fever (p<0,02) with parasitic infection. This coincides with different studies that have linked the presence of specific parasites to abdominal pain and diarrhea21,22. On the other side, results from this study diverge from the uncertainty of clinical significance of parasitic infection exposed in previous assays23, which highlighted the low positive predictive value of gastrointestinal symptoms for parasitism24. Therefore, association between symptoms and parasitic infection, warrants further studies. Moreover, the association found may overestimate the clinical significance of parasitic infection, since, most of the studied population, consulted to emergency room because they were symptomatic. Aditionally, no exclusion criteria for the presence of other pathologies such as HIV, celiac disease, salmonellosis, among others were considered, which could act as the direct cause of gastrointestinal symptoms notwithstanding the co-presence of parasitic infection.
The current study does not allow to determine risk factors for intestinal parasitism, however, it is possible to establish an association between certain sociodemographic variables and the frequency of the infection in the studied population such as rain water collected from roofs as drinking source, feces disposal different from latrine, septic tank or toilet, this data correspond to risk factors described in the medical literature25-28. On the other hand, the higher prevalence found in male population in our study was not consistent with other articles and may be due to the occupation of the studied population and their risk for oro-fecal contamination11,25,27,28. Our findings highlight the importance of public health measures as a preventive strategy to mitigate the spread of infection.