Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Colombia Médica
On-line version ISSN 1657-9534
Colomb. Med. vol.46 no.1 Cali Jan./Mar. 2015
Original Article
Dengue in an area of the Colombian Caribbean
El dengue en una región del Caribe colombiano
Nelson Alvis-Guzman1*, Heidi Rodríguez-Barreto2, Salim Mattar-Velilla2
1 Group of Health Economics. Faculty of Economic Sciences. Universidad de Cartagena, Cartagena, Colombia.
2 Institute of Tropical Biological Research, Universidad de Córdoba. Montería, Córdoba, Colombia
Alvis-Guzman N, Rodríguez-Barreto H, Mattar-Velilla S. Dengue in an area of the Colombian Caribbean, 2003-2010. Colomb Med. 2015; 46(1): 3-7.
© 2015. Universidad del Valle. This is an Open Access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Article history: Received: 23 December 2013 Revised: 9 March 2015 Accepted: 25 March 2015
Corresponding author: Nelson Alvis-Guzman. Universidad de Cartagena, Faculty of Economic Sciences, Group of Health Economics. Cartagena. Colombia. Email: nalvis@yahoo.com
Abstract
Background: In Colombia, dengue is an endemic disease and the four serotypes have been reported.
Objective: To describe the frequency and severity of dengue in an area of the Colombian Caribbean (Department of Cordoba)
Methods: A retrospective study was conducted. Two data sources were analyzed: The database from the Direction of Health in Cordoba, and clinical registers of patients diagnosed with hemorrhagic fevers and fevers of unknown origin in reference hospitals.
Results: The mean incidence of dengue between 2003-2010 was 36.5 cases/105 inhabitants (CI95%: 34.3-37.5) and adjusted for sub-reporting, could be between 178.5 and 521.6. The mean incidence of severe dengue was 4.7 cases/105 inhabitants (CI95%: 4.3-5.0). Mean mortality rate due to dengue was 0.3 cases/105 inhabitants. The fatality rate was below 1%. The mean total leukocyte count in patients with dengue was 6,181 mm3 (CI95%: 5,973-6,389) and with severe Dengue was 4,729 mm3 (CI95%: 4,220-5,238). The average platelet count in patients with Dengue was 118,793/mm3 (CI95%: 107,255-130,331) and in patients with Severe Dengue 77,655 (CI95%: 59,640-95,670). Both differences were statistically significant (p <0.05). The frequency of laboratories test per patient in patients with Dengue and severe Dengue were different.
Conclusion: The department of Cordoba is a highly endemic zone of Dengue and severe Dengue in the Colombian Caribbean. Moreover, the results show significant differences between dengue and severe dengue so much in tests as in frequency of use of healthcare services
Keywords: Colombia; dengue fever; classical dengue fever; surveillance
Resumen
Antecedentes: en Colombia el Dengue es una enfermedad endémica en la que se han descrito los cuatro serotipos que la producen.
Objetivo: Describir la frecuencia y severidad del Dengue en el departamento de Córdoba de la región caribe colombiana.
Métodos: Se llevó a cabo un estudio retrospectivo a partir del análisis de dos fuentes de datos: a) la base de datos de los casos reportados a la dirección de salud departamental y b) los registros clínicos de pacientes con diagnóstico de fiebres hemorrágicas y fiebre de origen desconocido., en hospitales de referencia del departamento de Córdoba.
Resultados: La incidencia media de dengue entre 2003-2010 fue de 36.5 casos por cien mil habitantes (IC95%: 34.3-37.5) y ajustando por sub-registro podría estar entre 178.5 y 521.6. La incidencia media de dengue grave fue de 4.7 casos por cien mil habitantes (IC95%: 4.3-5.0). La tasa promedio de mortalidad por el dengue durante el período fue de 0.3 casos por cien mil habitantes. El recuento leucocitario total promedio en los pacientes con dengue fue 6,181 x mm3 (IC95%: 5,973-6,389) y con dengue grave fue 4,729 x mm3 (IC95%: 4,220-5,238). El recuento medio de plaquetas en pacientes con Dengue fue 118,793/mm3(IC95%: 107,255-130,331) y en pacientes con Dengue Grave fue 77,655 (IC95%: 59,640-95,670). Las diferencias fueron estadísticamente significativas (p <0.05). La frecuencia de los laboratorios de pruebas por paciente en los pacientes con dengue y dengue grave fueron diferentes.
Conclusión: El departamento de Córdoba es una zona altamente endémica de dengue y dengue grave en el Caribe colombiano. Los resultados muestran diferencias significativas en algunas pruebas de laboratorio entre el dengue y el dengue severo.
Palabras clave: Colombia, dengue, dengue clasico, vigilancia.
Introduction
Dengue is a Tropical infectious disease caused by four serotypes of the dengue virus (DENV-1, DENV-2, DENV-3, and DENV-4)1. It is transmitted through the bite of the Aedes aegypti mosquito vector1. The incidence of dengue has grown dramatically around the world in recent decades. The actual numbers of dengue cases are under reported and many cases are miss classified. One recent estimate indicates 390 million dengue infections per year (95% credible interval 284-528 million), of which 96 million (67-136 million) manifest clinically (with any severity of disease)2 . The 2009 World Health Organization (WHO) criteria classify dengue according to levels of severity: dengue without warning signs; dengue with warning signs (abdominal pain, persistent vomiting, fluid accumulation, mucosal bleeding, lethargy, liver enlargement, increasing hematocrit with decreasing platelet); and severe dengue (SD) (dengue with severe plasma leakage, severe bleeding, or organ failure)3.
Because of its high epidemiological and economic impact, dengue occupies the fifth place in the list of unattended tropical diseases in the Americas in terms of disability-adjusted life years (DALY)4.
According to the PAHO, between 2001 and 2007, close to 30 countries in the Americas reported 4,332,731 cases of dengue; of which 106,037 (2.4%) corresponded to SD, with 1.2% mortality rate. Argentina, Brazil, Chile, Paraguay, and, Uruguay reported 64.6% of the dengue cases. Bolivia, Colombia, Ecuador, Peru, and, Venezuela reported 19.0% (819,466) of the dengue cases with 58% of the cases of SD and 306 deaths3.
In Colombia, dengue is an endemic disease and the four serotypes have been reported. Between 2004 and 2006, it was the country with the highest number of cases of SD and deaths due to this cause in America5. According to the Dengue Epidemiological Bulletin, to epidemiological week N°53 of 2014 the following have been reported in the National Health Institute’s Public Health Surveillance System (Sistema de Vigilancia en Salud Pública - SIVIGILA): 110,473 total cases of dengue, 107,696 dengue cases (97.5%) and 2,777 (2.5%) SD, and 109 deaths with laboratory confirmation for 3.9% fatality, far above that of 2010 (2.3%)6. However, the situation can worsen given the current high level of sub-reporting7. In Cordoba, department in the tropical region of Colombia’s Caribbean zone, in 2002 some 2,664 cases of dengue (128 x 100,000) were reported, along with 197 cases of SD (9.5 cases x 100,000 inhabitants). This study describes the frequency and severity of dengue in the department of Cordoba in Colombia’s Caribbean (2003-2010) with aim to inform public health policies.
Materials and Methods
A descriptive retrospective study was conducted to analyze the epidemiological characteristics of dengue between 2003 and 2010 in an area of the Colombian Caribbean, the department of Cordoba. The study's reference population was that from the Department of Cordoba, Colombia with a land surface of 23,980 km2, located in Colombia's northwest on the vast plains of the Caribbean (132,000 km2) at 7° 22' and 9° 26' latitude north and 74° 47' and 76° 30' longitude west of Greenwich, which in 2010 had 1,582,784 inhabitants, distributed in 30 municipalities8.
Two data sources were analyzed for the study: a) Database from the Direction of Health in the Department of Cordoba with 4,874 records of confirmed cases of dengue, reported from 2003 to 2010 (Data A). Of these records, only 1,965 (40.3%) had complete data that permitted estimating demographic and epidemiological parameters. To estimate incidence, population data were taken from population projections from Colombia’s National Statistics Department (DANE), based on the 1993 census8. b) Clinical histories of patients diagnosed with hemorrhagic fevers and fevers of unknown origin in the main reference hospitals in the Department of Cordoba (Monteria, Planeta Rica, Sahagun, Tierralta, Lorica, and Cerete) between 2003-2007. A total of 2,604 clinical histories were identified of patients with presumptive or confirmed diagnosis of dengue (CIE-10, 210, and 220). The 2,604 histories were assumed as universe of observations and from these, a random sample 230 (9%) were selected (Data B), which had complete information, regarding clinical and epidemiological parameters. From analysis of the clinical histories, we studied socio-demographic variables, age, sex, place of residence, and dengue classification (dengue and SD), according to WHO (2009).
To correct the sub-reporting of notification of cases and estimate the actual cases of dengue in the department of Cordoba, we used the adjustment factor proposed by Camacho et al7. The following formula expresses the adjustments of the sub-reporting: Actual number of cases= 9 x cases recorded according to the Cordoba Direction of Health. Information from both sources was entered onto a database by using Microsoft Office Excel® 2007.
Ethical aspects
Access to information from the clinical histories was requested from the directors of hospitals in Montería, Planeta Rica, Sahagún, Tierralta, Lorica, and Cereté. The information provided was used for the benefit of the inhabitants in the region. The study always maintained the anonymity of the patients and adhered to ethical standards, scientific techniques, and administrative norms for health research from Colombia’s Ministry of Social Protection, resolution Nº 008430 of 1993. The study was considered low risk and was approved by the ethics committee in the Institute of Tropical Biological Research at Universidad de Córdoba.
Results
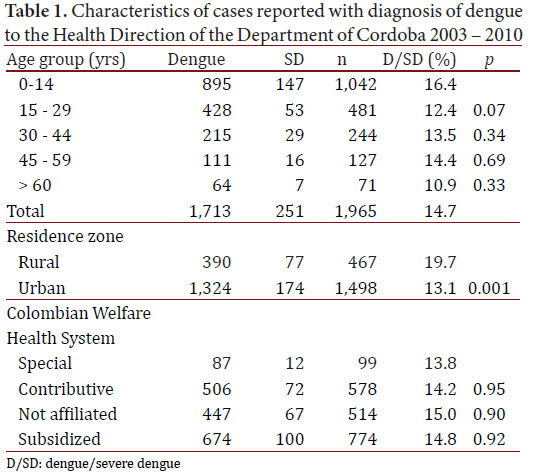
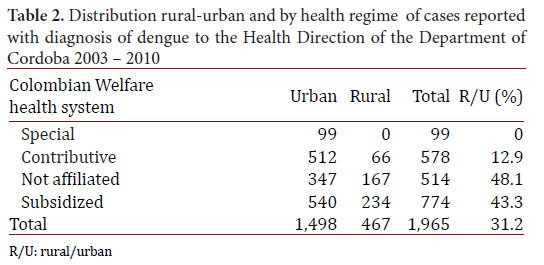
From analysis of the 1,965 cases (Data A), it was estimated that 76.2% were from the urban zone; the dengue: SD ratio was 7:1; 56.8% were men, 53.0% of the patients were younger than 14 years of age. The differences in the ratio dengue/SD by ages and social security health care scheme weren’t significant. However, the differences urban-rural were significant (Table 1). Furthermore, differences urban-rural in the distribution of cases by social security health care scheme were observed. Twenty six, point two per cent of cases were in population no affiliated to health system, especially in rural localities (Table 2).
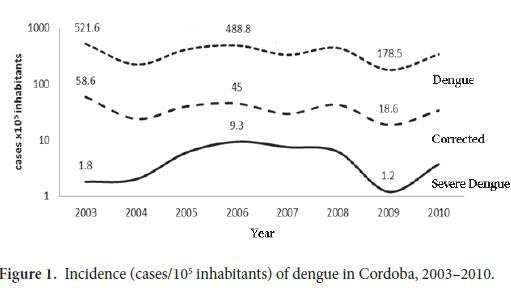
The mean incidence of dengue between 2003 and 2010 was 36.5 cases/105 inhabitants (CI95%: 34.3-37.5) a minimum of 19.8 (2009) and a maximum of 60.4 (2003). With the adjustment for sub-reporting, the incidence could be between 178.5 and 521.6 cases/105 inhabitants. The mean incidence of severe dengue was 4.7 cases/105inhabitants (CI95%: 4.3-5.0) (Fig. 1).
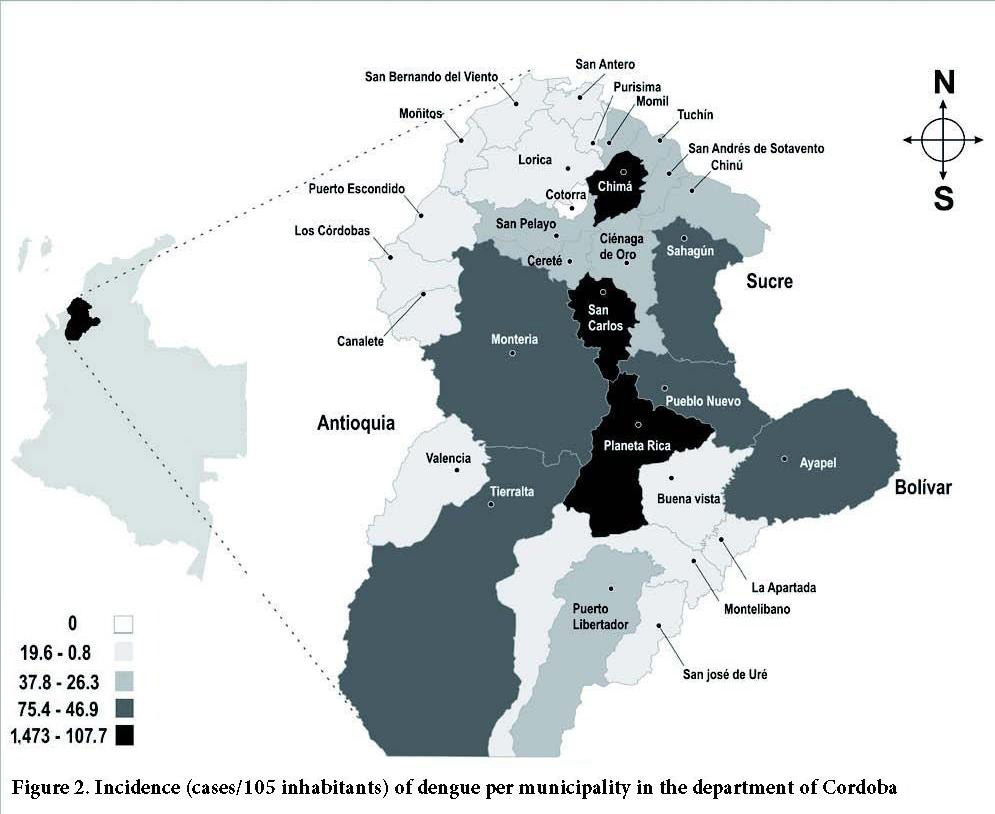
The municipalities in the department of Cordoba with the highest incidence of cases of dengue between 2003 and 2010 were: San Carlos, Chima, and Planeta Rica with a mean incidence of 147.3, 146.7, and 107.7 cases/105 inhabitants, respectively (Fig. 2).
Mortality
The mean mortality rate due to dengue was estimate with database from the Direction of Health in the Department of Cordoba. In Cordoba between 2003 and 2010 was 0.3 cases/105 inhabitants; the highest rate corresponds to with 0.6 x 105 inhabitants, followed by 2007 and 2009 with 0.4 x 105 inhabitants. Regarding the fatality rate, the department of Cordoba is below 1%, the highest fatality rate was in 2009 a rate of 1.9% was found, followed by the 2006-2007 period with a rate of 1.1%.
With respect to the findings in the 230 histories reviewed (Data B), laboratory results show that the mean total leukocyte count (neutrophils, lymphocytes, eosinophils, basophils, and monocytes) observed during the first test conducted on patients with dengue was 6,181 mm3 (CI95%: 5,973-6,389) and with SD it was 4,729 mm3 (CI95%: 4220-5238). The average platelet count observed during the first test conducted on patients with dengue was 118,793/mm3 (CI95%: 107,255-130,331) and in patients with SD 77,655 (CI95%: 59,640-95,670). Both differences were statistically significant (p <0.05).
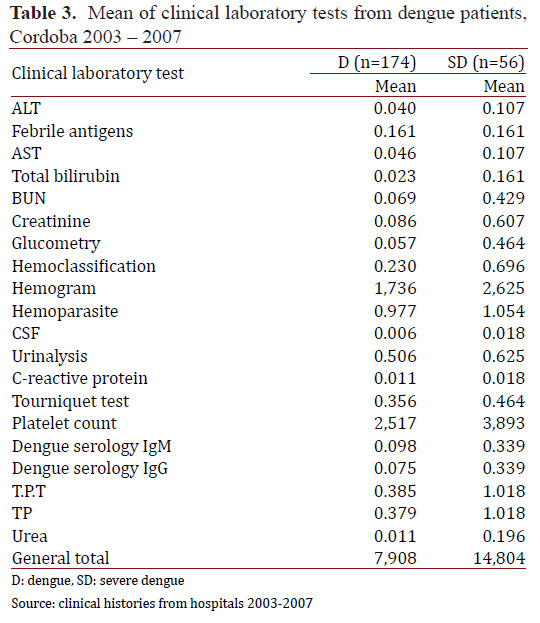
The laboratory tests most often used (frequency of uses: test mean per patient) in patients with dengue and SD were platelet count (Dengue: 2,517; SD: 3,893), hemogram (dengue: 1.736; SD: 2.625), and hemoparasites (dengue: 0.977; SD: 1.054). Only IgM and IgG tests were performed for dengue in 21.3% of the individuals diagnosed with dengue (dengue: 0.98; SD: 0.339) (Table 3).
Discussion
This study summarizes any epidemiological aspects of dengue in the department of Cordoba, in the Colombian Caribbean, showing that the incidence of cases estimated from surveillance records from health authorities is not consistent with the behavior of the diseases transmitted by vectors that describe a significant increase, probably due to climate change and other causes9,10. Correction for sub-reporting shows an incidence probably closer to reality, between 178.5 and 521.6 cases/105 inhabitants. However, the non-adjusted results from the current study were similar to those from Venezuela in 2003, where incidence rate was estimated at 63.4 cases/105inhabitants11; but do not coincide with those reported in Colombia; in Santander, where dengue incidence rates were between 113.4 and 268.7 cases/105 inhabitants, respectively12.
These also do not coincide with international studies like Mexico and Brazil, where incidence was reported at 27.2 cases/105 and 283.8 cases/105, respectively13,14, which shows the probable evidence of sub-reporting and other aspect as lack of diagnostic.
Cases reported of shock due to severe dengue produce mortality between 40 and 50%15,16; but in this study, the mortality rate due to dengue was low. Literature has described that when medical attention is offered by professionals with knowledge of the dengue virus (physicians and nurses who know of its symptoms and know how to treat its effects) the fatality rate can be reduced to less than 1%17. These results on the low mortality rate of dengue in Córdoba do not agree with Salgado et al.18, who reported that Colombia was the country with the most cases of severe dengue and deaths due to this cause in America during 2004 and 2006. This could be because in Cordoba no systematic record is kept and the cases were undervalued or not recorded.
Fatality results coincide with those from the Americas during 2001-2006, where a fatality rate of 1.2% was reported and with that from Mexico19 in 2008 with fatality at 0.7%. This means that the vector control and management program from the Health Direction of the Department of Cordoba needs to improve strategies for vector control and comprehensive management of dengue, according to the entomological risk and the dynamic stratification of probable cases (epidemiological risk) with immediate and comprehensive actions.
According to place of residence, the number of patients from urban areas was higher (76.2%), which is similar to that found in Neiva (Colombia) (69.6%), Panama (86%), Brazil (70%), and Peru (90%)14,20-22. In Colombia, approximately 70% of the population lives in urban zones. Growth of cities is associated to increased rural-urban migration due to multiple socioeconomic causes and forced displacement caused by armed groups, among others. From the epidemiological perspective, these aspects affect the rate of infectious contacts between mosquito vectors and humans and, hence, dengue epidemics and maintenance of the disease in the cities23. Additionally, dengue is a disease mainly transmitted by the A. aegypti mosquito, which inhabits urban sectors24,25, and the A. albopictus mosquito implicated as the second most important vector of dengue virus, unlike A. aegypti, A. albopictus proliferates in urban, rural, and jungle zones. Both mosquitoes evidence close cohabitation with humans and are of great importance at the social level26. Other authors have reported that water tanks and containers to store water in the households were the breeding grounds during different most productive states of the mosquito19,27. Cordoba has been a department with low coverage of drinking water and sanitation facilities in the past decades.
Regarding the most-often used laboratory tests, the results do not coincide with others that found a greater frequency of hemo-concentration associated to a strong plasma capillary leakage (presence of ascites) and upon diagnosis of severe dengue28. Immunoglobulin M and IgG tests were only carried out for dengue in 21.3% of the individuals diagnosed with dengue (dengue: 0.98; SD: 0.339). This shows that perhaps hospitals do not timely diagnosis methods29.
The tourniquet test was carried out on 93 of the 230 patients, 84.9% (79/93) of the cases were positive. According to some authors30-32, it is a useful tool to arrive at the diagnosis and it has also been documented as the main hemorrhagic manifestation in patients with dengue. Although other authors express that the lack of the tourniquet sign should not be considered32 given that it can be negative in up to 60% of the cases, although after the state of shock it becomes positive.
Regarding socioeconomic conditions, only 39.4% of the patients were in the subsidized social security scheme and most came from low socioeconomic levels in impoverished sectors with deficiency of health care services. Villar33 and Kouri et al.34, described that deterioration of health care systems produces substantial increases in the incidence of cases of dengue and gradually increases severe dengue. Although some authors consider that poverty is not related to the disease, however, it has been determined that the magnitude of the risk depends on the materials with which the dwelling is constructed, its sanitation conditions, and its surroundings35.
Conclusions
Study permitted establishing the dengue situation in an endemic zone with high sub-reporting; we managed to observe deficiencies in vector management and that etiological diagnosis is only made in low proportions. Furthermore, the low capability for diagnosis and treatments in hospitals show problems of access and non-quality health services.
Acknowledgements: The authors acknowledge to Direction of Health in Cordoba.
Conflict of interest: The authors declare that there are no conflicts of interest for this study.
References
1. Potts J, Gibbons R, Rothman A, Srikiatkhachorn A, Thomas S, Supradish P, et al. Prediction of dengue disease severity among pediatric Thai patients using early clinical laboratory indicators. PLoS Negl Trop Dis. 2010; 4(8): e769. [ Links ]
2. WHO . Dengue and severe dengue. WHO media centre; 2014. Accessed: 2011 Jan 15. Available from: http://www.who.int/mediacentre/factsheets/fs117/en/. [ Links ]
3. WHO. Dengue guidelines for diagnosis, treatment, prevention and control. Francia: World Health Organization, TDR; 2009. Accessed; 2011 Jan 15. Available from: http://whqlibdoc.who.int/publications/2009/9789241547871_eng.pdf. [ Links ]
4. Shepard DS, Coudeville L, Halasa YA, Zambrano B, Dayan GH. Economic impact of dengue illness in the Americas. Am J Trop Med Hyg. 2011; 84(2): 200-7. [ Links ]
5. Murillo-Llanes J, Soto-Valenzuela H, Flores-Flores P, Peraza-Garay F. Caracterización clínica y epidemiológica del dengue. Rev Med Inst Mex Seguro Soc. 2007; 45(5): 485-91. [ Links ]
6. Instituto Nacional de Salud,Dirección de Vigilancia y Análisis del Riesgo en Salud Pública Enfermedades Transmitidas por vectores. Boletín Epidemiológico Semanal. 2014; 53:17-22. [ Links ]
7. Camacho T , de la Hoz F, Cárdenas T, Sánchez C, de Calderón L, Pérez L, et al. Incomplete surveillance of a dengue-2 epidemic in Ibague, Colombia, 1995-1997. Biomedica. 2004; 24(2): 174-82. [ Links ]
8. DANE. Demografía y Población. Accessed: 20 August 2010; Available from: http://www.dane.gov.co/index.php/poblacion-y-demografia/proyecciones-de-poblacion. [ Links ]
9. Wilder SA, Gubler D. Geographic expansion of dengue: the impact of international travel. Med Clin North Am. 2008; 92(6): 1377-90. [ Links ]
10. Jansen C, Beebe N. The dengue vector Aedes aegypti: what comes next. Microbes Infect. 2010; 12(4): 272-9. [ Links ]
11. Añez G, Balza R, Valero N, Larreal Y. Economic impact of dengue and dengue hemorrhagic fever in the State of Zulia, Venezuela, 1997-2003. Rev Panam Salud Publica. 2006; 19(5): 314-20. [ Links ]
12. Ocazionez R, Gómez S, Cortés F. Serotipo, patrón de infección y dengue hemorrágico en área endémica colombiana. Rev Salud Pública. 2007; 9(2): 262-74. [ Links ]
13. Escobar MJ, Gómez DH. Determinantes de la transmisión de dengue en Veracruz: un abordaje ecológico para su control. Salud Pública Mex. 2003; 45(1): 43-53. [ Links ]
14. Penna G, Pinto L, Soranz D, Glatt R. High Incidence of diseases endemic to the Amazon region of Brazil, 2001-2006. Emerg Infect Dis. 2009; 15(4): 626-39. [ Links ]
15. Torres E. Dengue. Estudos Avançados. 2008; 22(64): 33-52. [ Links ]
16. Guha SD, Schimmer B. Dengue fever: new paradigms for a changing epidemiology. Emerg Themes Epidemiol. 2005; 2(1): 1-10. [ Links ]
17. Arbo A, Bogado N. Nuevas Guías de Tratamiento del Dengue. Pediatr (Asunción). 2011; 38(1): 7-8. [ Links ]
18. Salgado D, Vega M, Garzón M, Panqueba C, Rodriguez J. Mortalidad por dengue hemorrágico en niños en Colombia: más allá del choque. Infectio. 2008; 12(1): 247-53. [ Links ]
19. Villegas-Trejo A, Che-Mendoza A, González-Fernández M, Guillermo-May G, González-Bejarano H, Dzul-Manzanilla F, et al. Control enfocado deAedes aegypti en localidades de alto riesgo de transmisión de dengue en Morelos, México. Salud Pública Mex. 2011; 53(2): 141-51. [ Links ]
20. Salgado D, Rodríguez J, Garzón M, Cifuentes G, Ibarra M, Vega M, et al. Caracterización clínica y epidemiológica de dengue hemorrágico en Neiva, Colombia, 2004. Rev Salud Pública (Bogota). 2007; 9(1): 53-63. [ Links ]
21. Armien B, Suaya J, Quiroz E, Sah B, Bayard V, Marchena L, et al. Clinical characteristics and national economic cost of the 2005 dengue epidemic in Panama. Am J Trop Med Hyg. 2008; 79(3): 364-71. [ Links ]
22. Mamani E, Figueroa D, García M, Garaycochea MdelC, Pozo E. Infecciones concurrentes por dos serotipos del Virus dengue durante un brote en el noroeste de Perú, 2008. Rev Perú Med Exp Salud Publica. 2010; 27(1): 16-21. [ Links ]
23. Rey JR, Lounibos LP, Padmanabha H, Mosquera M. Resurgencia del dengue en América: pautas, procesos y prospectos. Interciencia. 2010; 35(11): 800-6. [ Links ]
24. Sánchez CR, Torres ZR, Segovia SF, Reyes VF, Alvarado MM, Fernández SI. Localización de criaderos no residenciales de Aedes aegypti y su asociación con casos de dengue en la zona Metropolitana de Monterrey, Nuevo León, Mexico. Rev Salud Pública Nutrición. 2010; 11(1): 1-6. [ Links ]
25. Ospina MC. Vigilancia epidemiológica del dengue en Antioquia. IATREIA. 2004; 17(3): 283-4. [ Links ]
26. Rivera A, Rodríguez A. Actualización en aspectos epidemiológicos y clínicos del dengue. Rev Cub Salud Pública. 2010; 36(1): 149-64. [ Links ]
27. Romero-Vivas C, Arango-Padilla P, Falconar A. Pupal-productivity surveys to identify the key container habitats of Aedes aegypti (L.)) in Barranquilla, the principal seaport of Colombia. Ann Trop Med Parasitol. 2006; 100(1): 87-95. [ Links ]
28. Ramírez ZM, Velasco MH, Ramos C, Peñuelas J, Maradiaga CM, Murillo LJ, et al. Caracterización clínica y epidemiológica de los casos de dengue: experiencia del Hospital General de Culiacán, Sinaloa, México. Rev Panam Salud Publica. 2009; 25(1): 16-23. [ Links ]
29. Acosta CB, Gómez IC. Biología y métodos diagnósticos del dengue. Rev Biomed. 2005; 16(2): 113-37. [ Links ]
30. Castrillón M, Iturrieta N, Cativelli S, Padilla F. Hallazgos ultrasonográficos en pacientes con Dengue. Revisión de la literatura. RAR. 2010; 74(1): 70-6. [ Links ]
31. Ramírez J, Aguirre A, Velandia R, Rosero H, García R, Ospina J, et al. Fiebre por dengue: guías de manejo. Rev Med Risaralda. 2010; 16(1): 41-51. [ Links ]
32. Pizarro D. Dengue, Dengue hemorrágico. Acta Pediátr Costarric. 2009; 21(1): 8-17. [ Links ]
33. Villar CL. El dengue: la epidemia se extiende y urgen intervenciones efectivas y herramientas clínicas para su atención. Infectio. 2008; 12(1): 9-10. [ Links ]
34. Kourí G, Pelegrino J, Munster B, Guzmán M. Sociedad, economia, inequidades y dengue. Rev Cubana Med Trop. 2007; 59(3): 177-85. [ Links ]
35. Gomez-Dantés H, Willoquet J. Dengue in the Americas: challenges for prevention and control. Cad Saude Publica. 2009; 25(1): 19-31. [ Links ]