INTRODUCTION
The name Bothriechis schlegelii derives from the Greek word bothros, which means "pit" and echis, "snake", referring to the loreal pit that is located between the nostrils and eyes on each side of the face, and also after the German zoologist Hermann Schlegel 1.
The length of B. schlegelii, also known as eyelash pit viper, varies between 50 and 120 cm, being females larger than males. The variety of its colors (emerald or dark green, yellow, brown and black), helps it mimic its surroundings. It has prehensile tail, and from two to four small superciliar scales, in the way of "eyelashes". It feeds on baby birds, lizards, frogs and rodents, inhabits tropical forests and corn and coffee crops, at altitudes ranging from 0 to 2600 m; the viper reaches the highest altitude in Colombia 2,3.
In the regions in which it inhabits, it is also known as cabeza de candado, granadilla, víbora de tierra fría, víbora de pestañas, yaruma, veinticuatro, guacamaya, víbora rayo, mortiñera, colgadora and grano de oro (these are different names to refer to this snake in diverse regions of Latin America) 2,4.
B. schlegelii extends from southern Mexico, throughout Central America, to the east of Venezuela, and in the Pacific through Costa Rica, Panama, El Salvador and Ecuador 5. In Colombia, it lives in the Pacific and Andean regions, and in the Western, Central and Eastern Ranges. In addition, it can be found from the south to the north of the country, on the border with the Venezuelan Andes, and is endemic in the coffee region 2.
Until epidemiological week 32 in 2016, 2 791 cases of snakebite accidents were reported to Sistema Nacional de Vigilancia en Salud Pública (National System of Public Health Surveillance), of which 65.6% corresponded to Bothrops6. However, the number of cases related to snakebites of Bothriechis genus specimens was not certain.
CLINICAL CASES
Case 1
Reason for consultation
55-year-old patient, from Pensilvania, Caldas, who was bitten on the back of the left hand by a 25 cm, thin, triangular head snake during his work in a coffee crop (Figure 1 and 2). The patient denies hypertension, diabetes, kidney disease, bleeding disorders or previous surgeries.

Source: Own elaboration based on the data obtained in the study.
Fig 1 Specimen of Bothriechis schlegelii which caused this event, in defensive position.
Clinical manifestations and physical examination
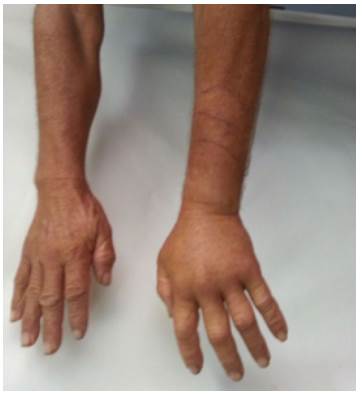
The patient presented with pain when moving the affected hand, paresthesia and 2cm edema in the right hand, which spread to the left forearm. No fang punctures nor local bleeding were observed (Figure 3).
Laboratory tests
Complete blood count, blood urea nitrogen, creatinine and coagulation tests were performed and no alterations were found. Total CPK was not determined.
Treatment
First, the patient was administered intravenous fluids, analgesia with tramadol, and tetanus prophylaxis (after confirming normal coagulation tests). Then, he was referred to a nearby hospital where three vials of polyvalent antiven-om Probiol® were administered intravenously; afterwards, the patient developed fever, which was controlled with acetaminophen. The pain and edema decreased and, finally, he was discharged after two days of observation.
Case 2
Reason for consultation
62-year-old man, from Fresno, Tolima, who was bitten on the third finger of the left hand during agricultural work by a thin snake, known in the area as "cabeza de candado (head lock)"(Figure 4 and 5). He denies hypertension, diabetes, kidney disease, bleeding disorders or previous surgeries.

Source: Own elaboration based on the data obtained in the study.
Fig 4 Bothriechis schlegelii. Triangular head.
Clinical manifestations and physical examination
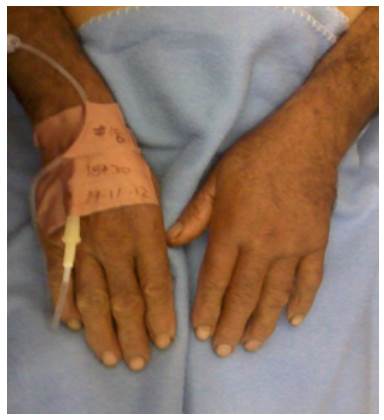
The patient was admitted with pain in the left hand, edema of 1 cm in the right hand, paresthesia in the left shoulder, emesis and diaphoresis (Figure 6).
Laboratory tests
The following tests were performed: unaltered blood count and prolonged prothrom-bin time, and partial thromboplastin time. Total CPK was not determined.
Treatment
The patient received intravenous fluids, analgesia and six vials of polyvalent antivenin produced by Instituto Nacional de Salud intravenously, without adverse reactions. After finding an alteration in clotting, the patient was given two additional vials of polyvalent antivenin, for a total of eight, and was referred to a third level hospital level in Ibagué. In the referral hospital, the patient's condition improved, and coagulation tests were normal 48 hours after the event; finally, he was discharged after 72 hours of observation.
DISCUSSION
The venom of B. schlegelii consists, mostly, of phospholipase A2, followed by metalloproteinases, bradykinin potentiating peptides, Kazal type proteinase inhibitor, serine proteinases, L-amino acid oxidase and cysteinerich secretory proteins (CRISPs), therefore, its properties are hypotensive, edema-forming, procoagulant, myotoxic, necrotizing and hemorrhagic 7.
When dealing with bites by a Bothriechis snake, assessing the severity of the bite through the clinical grading adapted by Otero is important 8, which also serves to determine the amount of antivenin to use.
The grades presented by Otero 8 are: Grade 1, absent, only minimal pain; Grade 2, mild, presence of edema (<4 cm) that compromises one or two segments of the bitten limb, ecchymosis, scarce bleeding with normal coagulation or incoagulable blood; Grade 3, moderate, with edema (> 4 cm) that compromises three segments of the bitten limb, blisters, local incoagulable bleeding or presence of systemic hemorrhage; Grade 4, severe, presence of edema beyond the bitten limb, necrosis, compartment syndrome, local hemorrhage with incoagulable blood, systemic hemorrhage (including brain hemorrhage), hypotension or shock, disseminated intravascular coagulation, renal failure and multiple organ dysfunction. According to this, the two cases were considered as mild.
The symptoms manifested by the patient in the first case -localized pain and progressive edema- correspond to the initial symptoms caused by the bite of this snake, which in some cases may be accompanied by hemorrhagic blisters, itching, bruising and necrosis 9,10. In Colombia, severe poisoning by Bothrops asper, Bothrops punctatus, Porthidium nasutum and Bothriechis schlegelii bite has been characterized and includes local necrosis, systemic and local bleeding, hypotension and renal failure 11.
In the second case, although no marked local symptoms were observed, there was a significant commitment of clotting, which can be explained by two reasons: the direct inoculum of poison inside a blood vessel, and the presence of metalloproteinases in the protein composition of the poison, because their concentration in the venom of B. schlegelii (17.7%) is lower compared to that of B. lateralis (55.1%). This specimen has shown a wide range of biological activities, such as hemorrhagic fibrinogenolytic degradation of components in the extracellular matrix, and activation of prothrombin and factor X, resulting in extensive local tissue damage and systemic bleeding 12,13.
TREATMENT CONSIDERATIONS
Appropriate initial measures for such events include complete medical history; cardiovascular, respiratory and neurological evaluation; intravenous fluids in a limb other than the affected one; bite site antisepsis; gastric protection and oral rest due to the risk of bleeding; prophylaxis for tetanus with tetanus toxoid when coagulation times are normal or normalized after treatment; broad spectrum antibiotic therapy in case of documented infection, and analgesia with opioids. Non-steroidal anti-inflammatory drugs should be avoided 14.
Currently, three types of antivenins are available in Colombia: one manufactured by Instituto Nacional de Salud, one manufactured by Laboratory Probiol® produced in Colombia, and another manufactured by Bioclon Institute of Mexico. The first two act against the venom of B. schlegelii and, according to their availability, should be used taking into account possible adverse reactions such as anaphylaxis, serum sickness, acute renal failure or pyrogenic reactions, which are treated with corticosteroids if they are mild to moderate, or adrenaline if anaphylactic shock occurs 2,8.
The polyvalent antivenin produced by Bioclon Institute of Mexico has also been used to treat this type of envenomation; also, it showed that it can reverse the procoagulant effect of the venom of B. schlegelii, as well as the polyvalent serum antivenin produced by Instituto Clodomiro Picado in Costa Rica 15.
CONCLUSIONS
Due to the correct classification of the severity of envenomation cases, the accurate identification of the causative specimens, the adequate dose and the quality of the antivenin used, a satisfactory outcome was achieved in both patients.
B. schlegelii bite produces poisoning, but this fact is underestimated in Colombia, partly because of the ignorance that health personnel have of this snake and because of the characteristics of their venom. Accurate diagnosis and specific treatment with polyvalent antivenin are crucial to prevent further morbidity in these patients.











 text in
text in