Introduction
The number of people with chronic kidney disease has been increasing gradually in recent years. In the United States, during 2004, about 104,364 patients started renal replacement therapy (RRT), an adjusted incidence rate of 339 per million. The prevalence of dialysis therapy was 335,963 individuals1. It is clear that the disease rates vary substantially according to race and ethnicity. In Colombia, it has a prevalence of 621 patients per million (ppm); there are 22,300 patients on dialysis therapy and, for 2012 the incidence rate was 81.7 ppm2.
Studies have shown that chronic kidney disease (CKD) is associated with increased mortality and morbidity, especially the risk of cardiovascular diseases3. Quality of life is an important indicator of health care, patient experience and measures of efficacy in various chronic diseases. Assessing quality of life is mandatory as a measure of outcome in the evaluation of adverse events and the efficacy of treatment in patients with various diseases, such as CKD4-6. In patients with CKD, quality of life not only provides important information about daily life, but also perceptions of functional status7,8. In this study, it was shown that patients with CKD have a lower quality of life score, compared with the general population9-11.
Subjects and methods
Patients
This comparative study was performed in Dialy-Ser, a renal unit located in Bogotá, Colombia. Data were collected from 154 patients on hemodialysis during the program, between August 2011 and August 2012. 77 patients were defined as incident patients, because their hemodialysis treatment had begun less than three months ago. 77 patients were defined as prevalent patients, because they had been on dialysis therapy for three months or more.
The study included 154 patients (43.5% women and 56.5% men), older than 18 years. The quality of life of the subjects was evaluated using the Medical Outcome Study 36-Item Short-Form Survey (SF-36), version validated in Spanish. Eight areas of health were included: physical functioning (PF), role participation with physical health problems - physical role (RP), corporal pain (BP), general health (GH), vitality (VT), social functioning (SF), role participation with emotional health problems (emotional role) (RE) and mental health (MH).
In addition, to ensure standardized conditions, summary measures of physical and mental component (PCS and MCS) were taken into account. Three scales, PF, RP and BP, are related to the physical component, since they contribute more to the score of the Physical Component measure (PCS). The mental component is most highly related to the scales MH, RE, and SF, which contribute most to the score of the summary measure of mental components (MCS). Finally, three scales have worth mentioning with both components, namely: VT, GH, SF.
Questionnaires were provided, answered by the participants, during the regular hemodialysis sessions, with the help and explanation of the nurse trained in CKD. All patients filled out the questionnaires completely. Through these questionnaires, medical records and interviews with patients, demographic and medical data were obtained, including age, sex, marital status, education, occupation, vascular access, BMI, comorbidities. Likewise, laboratory data, including hemoglobin, albumin, potassium, calcium, phosphorus, glucose and parathyroid hormone PTH, were obtained from fasting blood samples taken during the week of RRT initiation.
Ethical aspects
Informed consent was required for inscription, after patients received verbal and written information about the study. Informed consent was received from all individual participants included in the study. Ethical permission for the study was obtained from the scientific committee of the renal unit. All the procedures performed in studies with human participants were in accordance with the ethical standards of the institutional research committee and with the Declaration of Helsinki of 1964, its subsequent amendments or comparable ethical standards.
Statistical analysis
In our study, the CART model was used to identify the variables that most adequately discriminate between incident and prevalent patients. Classification and regression trees (CART) are widely used in predictive analysis, since they explain non-linear effects, offer quick solutions for the hidden and complex substructure and provide unbiased information, statistically significant, high-dimensional analysis, apparently not related to the data. CART is a non-parametric method, which uses mixtures of categorical (nominal and ordinal) and continuous data in the result, as well as predictors. It has the ability to control the effect of hidden interactions in a better way, compared to alternative methods. In addition, the results provided by tree-based analyzes are interpreted, visually and logically, more easily.
In order to evaluate the possible differences in SF-36 variables between incident and prevalent patients, the MANOVA model was used and the null hypothesis of equality of means between the SF-36 variables was tested. Subsequently, Marginal ANOVA was performed for each variable, with the purpose of detecting the differences observed in detail. In addition, a PCA was performed to identify possible groups of patients associated with certain physical or mental characteristics, which are distinguished by SF-36 variables and which are identified by the contributions of each variable to the main components.
All statistical analyzes were performed in R version 3.0.2.
Results
Through CART, data were obtained from groups of prevalent patients and incidents associated with certain clinical and laboratory variables. It was found that 59 patients (77%) of the group of incident patients had a BMI <31, hemoglobin (Hb) <11 g/dL and catheter use (Figure 1).
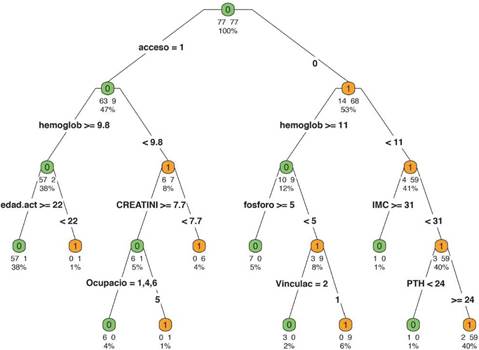
Figure 1 Classification and regression trees (Classification and Regression Tree CART). Incident patients (0) green and prevalent patients (1) orange.
Quality of Life
Eight SF-36 quality of life variables were evaluated by MANOVA multivariate analysis. Significant differences were found between the two groups (p = 0.028): except for body pain and emotional problems, in all other variables it is observed that the incident patients have less value in the quality of life than the prevalent patients (figure 2). Similarly, the analysis for PCS and MCS found significant differences (p = 0.0027): the incident patients tend to have lower quality of life scores than the prevalent ones. (Figure 3).
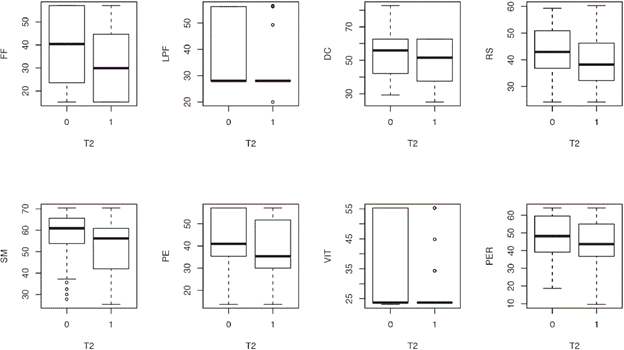
Figure 2 Box plots. Comparison of quality of life between incident patients and prevalent in the SF-36 items.
Principal component analysis
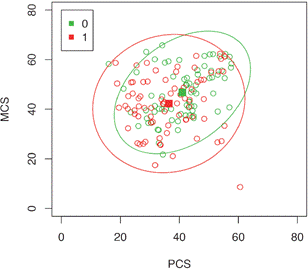
It was found that the first component (with an explanatory power of 46%) is positively associated with all the quality of life variables that indicate that patients tend to have a high or low status in the set of all the variables (figure 4). The second component includes MH and GH. These are moderately associated and negatively associated with RP and VT. They reveal that some patients with low scores on the scale of limitation, caused by physical problems and vitality, are not significantly affected in the scales of mental health and perception of the disease, since a great majority of patients have positive values in the component main 2 (figure 5). On the other hand, we found a significant group of prevalent patients with good scores on the physical component scales.
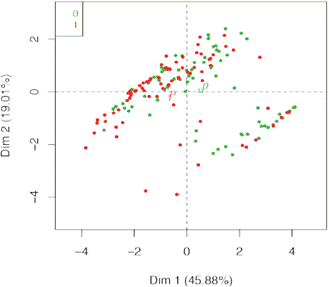
Figure 4 Dispersion plot for the two main components. Incident patients (0) green, prevalent patients (1) red.
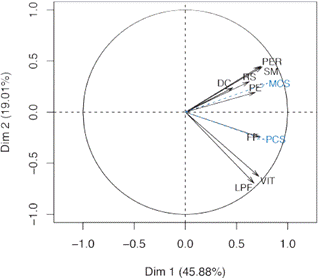
According to the SF-36, in our population there is a high relation between the sum of the mental component and the variables MH, RE, GH and, to a lesser degree, BP and SF, while the sum of the physical component is highly associated with PF, VT. In addition, it is observed that, although the physical pain is involved with the construction of the two indices, it was found more strongly associated with the mental component than with the physical one.
Discussion
Quality of life decreases in incident patients on hemodialysis and in prevalent patients. However, incident patients have even lower quality of life, compared to prevalent patients.
The treatment of anemia in patients with chronic kidney diseases has been described to improve the quality of life of patients on hemodialysis and different levels of hemoglobin have been proposed. A systematic review and meta-analysis suggest treatment at hemoglobin levels greater than 9.0, preferably 12.0 g/dL12.
In this study, it was found that the quality of life was higher in patients with hemoglobin levels higher than 11 g/dL. Similar results have previously been found in such levels of hemoglobin and quality of life13. The nutritional aspects also have an impact on the quality of life. In this study, a lower quality of life was found in patients with a BMI <31 and a better quality of life in obese patients, although it has been previously called inverse epidemiology.
According to clinical guidelines, based on the evidence from the initiative of the Kidney Foundation Kidney Disease Outcomes Quality Initiative (KDO-QI), between 18% and 70% of dialysis patients have some degree of malnutrition and 10% of the population has severe malnutrition14,15. Malnutrition has been attributed, to a large extent, to the mortality and morbidity of dialysis patients, partly explained by protein-calorie malnutrition and the complex syndrome of malnutrition-Inflammation (MICS), or by the presence of both entities concomitantly.
The inverse or paradoxical relationships between the nutritional markers and the results are known as "reverse epidemiology". The MICS seems to be the main contributor to inverse epidemiology and the one with the worst prognosis16-19.
The pre-dialysis program is a great opportunity to improve the quality of life in the incident patients. It should focus on the nutritional status, the early construction of an arteriovenous fistula as vascular access and the maintenance of hemoglobin levels greater than 11 g/dL. This is an important contribution to the physical health of patients who attend dialysis, since it impacts the quality of life of this population, especially of the incident patients.











 text in
text in