Trabajo realizado nel Curso de Pós-Graduação em Patologia da Fundação Faculdade Federal de Ciências Médicas de Porto Alegre en el Fertilitat Centro de Medicina Reprodutiva. Porto Alegre, Brasil.
* Médica Ginecologista. Preceptora do Serviço de Ginecologia do HSL/PUCRS. Mestre em Patologia Experimental. Membro do Fertilitat Centro de Medicina Reprodutiva. Correo electrónico: adriarent@ig.com.br, fertilitat@fertilitat.com.br. Quintino Bocaiúva, 1617/301, Porto Alegre, RS, Brasil. CEP:90440-051.
]]> ** Médico Urologista. Professor Livre Docente da FFFCMPA. Chefe do departamento de Urologia da Irmandade Santa Casa de Porto Alegre.Membro do Fertilitat Centro de Medicina Reprodutiva.*** Médico Patologista. Professor Livre Docente da FFFCMPA.
**** Médica Ginecologista. Professora Mestre da Faculdade de Medicina PUCRS. Chefe do Serviço de Ginecologia do HSL/PUCRS. Diretora do Fertilitat - Centro de Medicina Reprodutiva.
+ Acadêmica de Medicina da ULBRA./RS.
++ Médico Ginecologista. Professor da Faculdade de Medicina PUCRS. Diretor do Fertilitat - Centro de Medicina Reprodutiva.
RESUMEN
Objetivo: evaluar el resultado de la inyección intracitoplasmática de espermatozoides (ICSI) en parejas cuyos hombres mostraron azoospermia no obstructiva en conformidad con el hallazgo histológico del testículo.
Diseño: estudio retrospectivo con análisis transversal.
Materiales y métodos: han sido estudiados los resultados de laboratorio y clínicos en 59 parejas (79 ciclos) sometidas a la ICSI. Los hombres han sido divididos en 3 grupos de acuerdo con el reporte histológico obtenido en biopsia previa a la fertilización (hipoespermatogénesis, detención de la maduración espermática y aplasia de las células germinativas) y los resultados han sido comparados entre los grupos.
Resultados: el hallazgo principal fue la hipoespermatogénesis (61%), seguido por la detención de la maduración espermática (22%) y la aplasia de las células germinativas (17%). Los espermatozoides estuvieron presentes en 87,7% y la tasa de fertilización (58,8%) en los casos de hipoespematogenesis fue significativamente más grande (p < 0,001) en comparación con los de detención de la maduración (50 y 40,7%) y con la aplasia de células germinativas (21,4 y 36,8%). La primera división celular tuvo una tendencia superior en los pacientes con hipoespermatogenesis (95,9%) seguido de los pacientes con detención de la maduración (87,5%) y luego los con aplasia de las células germinativas (71,4%) (p = 0,001). La tasa total de embarazo clínico por ciclo iniciado y por transferencia fue de 25,3 y 37,7%, respectivamente.
]]> Conclusiones: la biopsia de testículo en hombres con azoospermia previa a la fertilización es una técnica fundamental para una orientación adecuada. Aunque los hombres con hipoespermatogénesis son quienes han obtenido los mejores resultados, es bien posible la obtención de espermatozoides, fertilización y embrazo en los pacientes cuya biopsia no ha evidenciado presencia de espermatozoides.Palabras clave: infertilidad, inyecciones de esperma intracitoplasmáticas (ICSI), azoospermia, histología testicular.
SUMMARY
Objective: evaluating ICSI outcome using testicular spermatozoa in patients having non-obstructive azoospermia according to the histological finding of a previous testicular biopsy.
Design: retrospective and transversal study.
Patients and methods: we evaluated the laboratory outcome and clinical results of 59 couples undergoing 79 ICSI cycles with testicular sperm retrieval. These patients were divided into three groups according to testicular histology (hypospermatogenesis, maturation arrest and germ cell aplasia) revealed in biopsy prior to ICSI. The ICSI was compared to the other groups.
Results : the most frequent testicular histological finding was hypospermatogenesis (61%), followed by maturation arrest (22%) and germ cell aplasia (17%). Sperm recovery and oocyte fertilisation were higher in the hypospermatogenesis group (p < 0,01) than in maturation arrest (50% and 40.7%) and germ cell aplasia (21.4% and 36.8%). Embryo cleavage was higher in patients having hypospermatogenesis (95.9%) followed by maturation arrest (87.5%) and germ cell aplasia (71.4%) (p = 0.001). The groups presented no difference in embryo development. Total clinical pregnancy rate per ICSI cycles and per cycles with embryo transfer were 25.3% and 37.7%, respectively.
Conclusions: testicular biopsy has clinical value when counselling infertile couples. Although patients with hypospermatogenesis returned the best results, sperm recovery and oocyte fertilization are possible, even in cases where no spermatozoa were found in testicular biopsy.
]]> Key words: infertility, ICSI, azoospermia, testicular histology.RESUMO
Objetivo: avaliar o resultado de injeção intacitoplasmática de espermatozóides (ICSI) em homens com azoospermia não obstrutiva de acordo com a histologia testicular prévia.
Desenho: estudo retrospectivo e transversal.
Materiais e métodos: foram estudados os resultados laboratoriais e clínicos em 59 casais (79 ciclos) submetidos a ICSI com uso de espermatozoide testicular. Foram divididos três grupos de acordo com a histologia testicular obtida em biópsia a fertilização (hipoespermatogênese, parada de maturação espermática e aplasia de células germinativas) e os resultados da ICSI foram comparados entre os grupos.
Resultados: o achado histoplatológico mais frequante foi hipoespermatogenese (61%), seguido por parada de maturação (22%) e aplasia de células germinativas (17%). A recuperação espermática e a taxa de fertilização oocitária foram superiores no grupo com hipoespermatogênese (p < 0,01) que na parada de maturação (50% e 40.7%) e aplasia de células germinativas (21.4% e 36.8%). A clivagem embrionária foi superior em pacientes com hipoespermatogênese (95.9%) seguido de parada de maturação (87.5%) e aplasia de células germinativas (71.4%) (p = 0.001). Não houve diferença no desenvolvimento embrionário. A taxa de gestação clínica por ICSI e por ciclos com transferência embrionária foram 25.3% e 37.7%, respectivamente.
Conclusões: a biópsia testicular tem valor clinico no aconselhamento de casais inférteis. A pesar de pacientes com hipoespermatogênese apresentarem os melhores resultados, obtenção de espermatozoides e fertilização oocitária são possíveis, mesmo nos casos onde não foram encontrados em biopsia testicular prévia.
Palavras-chave: infertilidade, injeção intracitoplasmática de espermatozóide (ICSI), azoospermia, histologia testicular.
INTRODUÇÃO
O fator masculino responsável por um terço dos casos de infertilidade, enquanto 20% das causas são imputadas conjuntamente à mulher e ao homem.1 Antes de 1992 a infertilidade masculina era considerada intratável em muitos casos. Com o aparecimento da injeção intracitoplasmática de espermatozóides (ICSI) foi possível solucionar de forma eficaz grande parte destes casos, através da utilização de espermatozoides obtidos do ejaculado.2,3 Inicialmente espermatozoides do ejaculado eram utilizados e após espermatozoides do epidídimo e, finalmente, em 1993 foi demonstrado que com espermatozóides extraídos do parênquima testicular era possível à fertilização de óvulos e obtenção de gestação em pacientes com azoospermia obstrutiva e posteriormente este achado foi confirmado também em pacientes com azoospermia não-obstrutiva.4-9
]]> A azoospermia não-obstrutiva é a ausência de espermatozóides no ejaculado seminal devido à deficiência de produção de espermatozóides, sendo identificada em 12% dos homens inférteis.1,10 Nestes pacientes as principais alterações histológicas detectadasna biópsia testicular são aplasia de células germinativas (11-20%), parada de maturação da espermatogênese (4 a 40%) e hipoespermatogênese (50%), sendo que nos casos de aplasia de células germinativa ou parada de maturação, espermatogênese focal pode estar presente.10
Neste estudo revisamos uma série de pacientes com azoospermia não-obstrutiva nos quais espermatozoides extraídos do parênquima testicular foram obtidos para realização de ICSI. Avaliamos o valor prognóstico da biópsia testicular na obtenção de espermatozóides em ciclos de ICSI de pacientes com azoospermia não-obstrutiva. Também comparamos os resultados laboratoriais (taxa de fertilização, taxa de clivagem embrionária, qualidade embrionária) e clínicos (taxa de gestação, índice de abortamento) obtidos na ICSI de acordo com o diagnóstico histológico da azoospermia.
PACIENTES E MÉTODOS
Desenho do estudo: estudo retrospectivo e transversal.
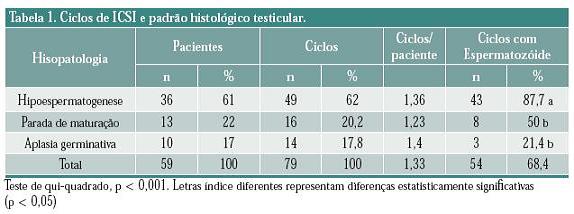
Pacientes: a população foi constituída de casais que buscaram tratamento de infertilidade conjugal por azoospermia não-obstrutiva e que foram submetidos à programa de fertilização in vitro pela técnica de ICSI com micromanipulação de gametas, com transferência de embrião(ões) para o útero, no Fertilitat- Centro de Medicina Reprodutiva. Foram selecionados 59 casais cujos parceiros haviam realizado biópsia testicular previamente ao procedimento de fertilização. Os 59 pacientes foram distribuídos em 3 grupos, de acordo com o padrão histopatológico da azoospermia: onde 36 (61%) apresentaram hipoespermatogênese, 13 (22%) tinham parada de maturação espermática e 10 (17%) tinham aplasia germinativa (tabela 1). Estes casais realizaram 79 ciclos de ICSI sendo que o número de ciclos de fertilização de cada grupo foi 49, 16 e 14, respectivamente (tabela 1).

Critérios de inclusão: infertilidade conjugal por azoospermia não-obstrutiva com tratamento pelas técnicas de fertilização assistida com micromanipulação de gametas.
Critérios de exclusão: ausência de biópsia testicular prévia ao procedimento de fertilização assistida, uso de gametas congelados.
]]> Local: Curso De Pós-Graduação em Patologia. Fundação Faculdade Federal de Ciências Médicas de Porto Alegre, Porto Alegre, RS, Brasil. Fertilitat Centro de Medicina Reprodutiva, acreditado pela Red Latinoamericana de Reproducción Asistida, Porto Alegre, RS, Brasil.Procedimento de FIV:
a) Indução da ovulação e aspiração folicular
A estimulação ovariana foi realizada com gonadotropina menopáusica humana (hMG) após dessensibilização hipofisária com acetato de leuprolide. O desenvolvimento folicular foi controlado por ecografia transvaginal e foi administrado gonatotrofina coriônica humana (hCG) quando pelo menos dois folículos apresentavam 18 mm de diâmetro. A aspiração folicular foi realizada 35 horas após o hCG, por via ecográfica transvaginal e o líquido folicular aspirado enviado ao laboratório de reprodução asistida para screening dos oócitos. Foram inseminados os oócitos em estágio de metáfase II (M II).
b) Obtenção de espermatozoides através de biópsia testicular e preparo do material
A biópsia testicular foi realizada através da aspiração testicular percutânea (TESA- testicular sperm aspiration) ou a céu aberto (TESE- testicular sperm extraction). Após anestesia local, através de uma agulha de 18 G acoplada a uma pistola que produz pressão negativa, a coleta era efetuada. Um auxiliar mantinha o testículo firme e a agulha era introduzida diversas vezes no testículo de tal sorte a coletar material de diversos locais.
Quando não eram encontrados espermatozoides no material aspirado, realizava-se biópsia a céu aberto. Através da mesma anestesia e com uma incisão longitudinal. Após a abertura da camada vaginal e da albugínea, o auxiliar comprimia delicadamente o testículo, resultando na herniação parcial de tecido intratesticular, o qual era seccionado com bisturi ou tesoura e imediatamente colocado em meio de cultura. O fechamento da albugínea efetuados por sutura contínua e após se realizava a sutura por camadas. Tanto o material obtido por TESA quanto por TESE foi processado da mesma maneira. O fragmento retirado do testículo era colocado com meio de cultura em uma placa de Petri. Com o auxílio de lâminas ou micropipetas de vidro, o fragmento era macerado, procurando liberar os túbulos seminíferos. O material era transferido a um tubo cônico e agitado vigorosamente, liberando os espermatozóides dos túbulos. Deixava-se o tubo em repouso por 10 minutos, quando então se retirava uma gota do sobrenadante para observação da presença e número de espermatozóides, em microscópio ótico com 200 aumentos. Na presença de espermatozóides em número suficiente, processavase o material em mini-Percoll, centrifugando por 25 minutos a 1.500 rotações por minuto. Quando este procedimento não era possível, retiravam-se os espermatozóides diretamente do material macerado.
c) Procedimentos ICSI, cultivo embrionário e diagnóstico de gestação
A ICSI foi realizada de modo habitual, como descrito na literatura.2,3 O meio de cultivo utilizado para inseminação foi Human Tubal Fluid HTF (Irvine Scientific) acrescido de 20% de soro sintético substituto-SSS (Irvine Scientific). A fertilização foi comprovada pela presença de dois pró-nucleos e corpo polar dividido,18 a 20 horas após a inseminação. Os oócitos fertilizados foram cultivados com meio de cultura HTF® ( human tubal fluid , Irvine Scientific) suplementado com 15% de SSS ( serum substitute solution, Irvine Scientific). A divisão embrionária foi observada 24 e 48 horas após a fertilização. O grau morfológico usado para classificar os embriões foi baseado nos critérios da Red Latinoamericana de Reproducción Asistida (Quadro 1), que utiliza os parâmetros de simetria de blastômeras e percentagem de fragmentação citoplasmática.11 Segundo esta classificação os embriões são graduados em grau I, grau II, grau III e grau IV sendo considerados os melhores embriões aqueles com graus I e II. A transferência foi realizada no terceiro dia de cultivo, sob visão ecográfica via abdominal, sendo utilizado cateter de Frydmann.
]]>

A gestação foi diagnosticada pela presença de nível sanguíneo detectável de B- hcg acima de 25 mUI/ml, doze dias após a transferência embrionária, com posterior desenvolvimento de saco gestacional ao exame ecográfico.
d) Variáveis analisadas:
Diagnóstico Histopatológico : foi avaliado pelo resultado da biópsia testicular realizada durante a investigação da infertilidade. Os pacientes foram divididos em 3 grupos de acordo com a histologia (hipoespermatogênese, parada de maturação espermática, aplasia germinativa).
Obtenção de gametas masculinos: avaliado tipo de coleta (TESA ou TESE) e resultado da coleta: negativa (ausência de espermatozóides), positiva (presenta de espermatozóides).
Evolução Laboratorial e desfecho clínico: as taxas de fertilização oocitária (é o número de oócitos fertilizados dividido pelo número de oócitos inseminados, multiplicado por 100), clivagem embrionária (é o número de embriões divididos dividido pelo número de oócitos fertilizados, multiplicado por 100) e a qualidade embrionária (classificação embrionária, para a qual foram utilizados os critérios da Red Latinoamericana deReproducción Asistida quadro 1) foi comparada entre os ter grupos de estudo. A gestação foi o desfecho clínico avaliado, também comparada entre os grupos.
Análise estatística
Neste estudo foram avaliados os resultados laboratoriais e clínicos da ICSI em 3 grupos de pacientes, divididos segundo a histologia testicular. As taxas de obtenção espermática, de fertilização oocitária, de clivagem embrionária e de qualidade embrionária foram analisados utilizando teste do qui-quadrado e análise de tendência linear, sendo que um erro a de 5% (p < 0,05) foi considerado significativo.
Ética: o presente estudo está de acordo com a resolução n0 196/96 do Conselho Nacional de Saúde. O projeto foi submetido a aprovação do Comitê de Ética em Pesquisa da Irmandade Santa Casa de Misericórdia de Porto Alegre. Os dados foram coletados dos prontuários médicos da Clínica Fertilitat - Centro de Medicina Reprodutiva sob autorização administrativa e respeitando os critérios éticos para uso dos mesmos. Todos pacientes assinaram termo de consentimento informado antes do tratamento de fertilização, disponibilizando a utilização de seus dados para fins científicos. Nenhum procedimento além dos necessários ao tratamento de fertilização assistida foi realizado.
RESULTADOS
]]> Fizeram parte do estudo 68 pacientes com azoospermia não-obstrutiva. Nove foram excluídos por não terem resultado da histologia testicular prévia ao procedimento de fertilização in vitro . A população estudada compreendeu 59 indivíduos caucasianos, com idade média de 39,2 +/- 7,8 anos, variando de 27 a 63 anos. No grupo com hipoespermatogênese (n = 23, 61%) a média etária foi 38,9 +/- 7,3 anos (27 a 56); nos pacientes com parada de maturação espermática (n = 13, 22%) foi 40,1 anos +/- 8,1 (27 a 55) e naqueles com aplasia germinativa (n = 10, 17%) foi 38,7 anos +/- 9,8 (31 a 63). Não houve diferença significativa entre a média etária dos grupos.Estes pacientes realizaram 79 ciclos de fertilização in vitro: 49 (62%) ciclos em pacientes com hipoespermatogênese, 16 (20,2%) com parada de maturação espermática e 14 (17,8%) com aplasia germinativa (tabela 1).
Nos 79 ciclos de fertilização in vitro em 19 (24%) havia espermatozóides na biópsia aspirativa (TESA), todos estes pacientes com hipoespermatogênese. Em 60 (76%) foi realizada também realizada biopsia aberta (TESE).
Em 54 ciclos (68,3%) foram encontrados espermatozóides. As taxas de obtenção de espermatozoides nos casos de hipoespermatogênese, parada de maturação e aplasia germinativa foram 87,7, 50 e 21,4%, respectivamente (tabela 1). A obtenção de espermatozóides foi significativamente superior nos pacientes com hipoespermatogênese (p < 0,001). Em 14 (17,7%) ciclos sem espermatozóides havia espermátides e em 11 (14%) ciclos nenhuma célula da linhagem germinal foi encontrada.
Em 53 ciclos foram utilizados espermatozoides testiculares para a fertilização oocitária. Foram inseminados 502 oócitos, sendo que 277 (55,2%) apresentaram fertilização normal (formação de 2 pró-núcleos e corpo polar dividido). A taxa de fertilização variou de 36,8% a 58% entre os três grupos estudados (tabela 2), sendo significativamente superior nos pacientes com hipoespermatogênese.
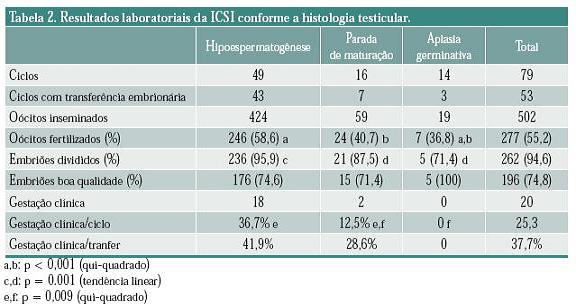
Duzentos e sessenta e dois (94,4%) embriões apresentaram divisão inicial. A análise de tendência linear mostrou diferença significativa na clivagem embrionária (p = 0,001) entre os três grupos, sendo superior nos pacientes com hipoespermatogênes (tabela 2).
Do total de embriões clivados, 180 (68,7%) foram utilizados para transferência uterina no mesmo ciclo, 55 (21%) foram criopreservados e 27 (10,3%) não prosseguiram seu desenvolvimento. Foram transferidos, em média, 3,4 embriões por paciente: 3,6 nos ciclos de hipoespermatogênese, 2,7 nos com parada de maturação e 1,7 nos com aplasia germinativa.
O percentual de embriões grau I, II, III, IV e parados, no terceiro dia de cultivo foi, respectivamente, 13,6, 61,4, 12,2, 2,7 e 10,3%. Não houve diferença na qualidade embrionária entre os grupos estudados. Embriões de boa qualidade (graus I e II) e de má qualidade (graus III, IV e parados) corresponderam a 74,8% e 25,2% do total de embriões clivados, respectivamente (tabela 2).
]]> Em 22 pacientes os níveis de B hcg foram compatíveis com gestação, sendo que em 20 houve desenvolvimento embrionário, caracterizando gestação clínica. A taxa de gestação clínica por ciclo de FIV e por ciclo com transferência de embriões foi, respectivamente, 25,3% e 37,7% (tabela 2). Em 4 (20%) gestações ocorreram abortamentos espontâneos.DISCUSSÃO
No presente estudo o padrão histopatológico testicular mais freqüente na biópsia foi a hipoespermatogênese, seguido de parada de maturação espermática e aplasia de células germinativas. Obteve-se espermatozóides para fertilização asistida em 68,3% dos casos. A taxa de obtenção de espermatozóides foi significativamente maior nos pacientes com hipoespermatogênese (p < 0,001). Estes dados estão em conformidade com os resultados de outros autores e mostram que podem ser encontrados espermatozóides mesmo naqueles pacientes onde a biópsia testicular prévia evidenciou ausência de espermatogênese (parada de maturação, aplasia germinativa)7,12-15 e estão demonstrados na tabela 3.
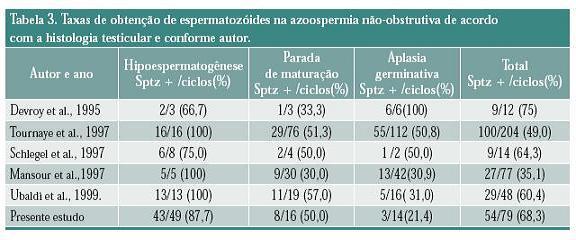
Estes resultados trazem a questão de por que espermatozóides podem ser encontrados em pacientes com azoospermia não-obstrutiva em que previamente uma biópsia testicular havia declarado ausência de espermatozóides (aplasia germinativa, parada de maturação). Na realidade, espermatogênese focal pode ocorrer nestes indivíduos.8,9 Além disso, durante os procedimentos de fertilização in vitro se procura minuciosamente por espermatozóides, usando, algumas vezes, microscópios com campos de aumento superiores aos utilizados na avaliação histopatológica. Também se deve considerar que na biópsia testicular diagnóstica muitas vezes apenas um fragmento de testículo é retirado enquanto nos procedimentos de fertilização se retiram amostras de tecido até que espermatozóides sejam encontrados ou até que toda superfície testicular tenha sido avaliada. Turek et al, 16 introduziram o conceito de mapeamento testicular, sugerindo que a avaliação histopatológica testicular nos pacientes com falência testicular deva ser realizada através da retirada de fragmentos de vários pontos do testículo. Estudos concluíram que a biópsia testicular com aspiração por agulha fina em 4 ou 6 pontos do testículo é um método com maior sensibilidade e especificidade que a biópsia testicular em um único ponto, além de revelar a heterogeneidade da espermatogênese e poder orientar que ponto do testículo deve ser abordado durante a biópsia para obtenção de espermatozoides para fertilização assistida.16,17
No que tange a fertilização oocitária, encontramos uma taxa de fertilização de 55,2% com uso de espermatozóides testiculares de homens com azoospermia não-ostrutiva (tabela 2). Este dado também está de acordo com a literatura, que apresenta taxas de fertilização entre 34 e 69,5% com o uso de espermatozóides testiculares em pacientes com azoospermia nãoobstrutiva.18-23 Os pacientes com hipoespermatogênese apresentaram fertilização superior (58%) quando comparados ao grupo com parada de maturação (40,7%) (p = 0,011). Apesar da taxa de fertilização ter sido menor nos pacientes com aplasia germinativa (36,8%), provavelmente devido ao menor número de casos, esta diferença não se mostrou significativa (tabela 2). Resultado similar foi relatado por Tournaye et al, 24 que encontraram diferença significativa na taxa de fertilização de pacientes com hipoespermatogênese (67,8%) quando comparado a pacientes com parada de maturação (45,7%) e aplasia germinativa (44%). Outro estudo também apresentou resultados semelhantes, onde pacientes com hipoespermatogênenese apresentaram melhor índice de fertilização (79,5%) (p = 0,0001) quando comparados àqueles com aplasia de células germinativas (71,2%) e parada de maturação (47 %).25
Tournaye et al 24 sugerem que esta diferenta na fertilização ocorra porque nos pacientes com parada de maturação e com aplasia germinativa menos espermatozóides móveis são obtidos para a inseminação. No estudo de Nagy et al 26 a taxa de fertilização foi significativamente inferior quando foram utilizados espermatozóides imóveis para inseminação (p = 0,006). No nosso estudo não avaliamos este parâmetro. A literatura levanta a hipótese que a diferença nas taxas de fertilização observada entre os tipos de azoospermia não-obstrutiva seja porque nos casos de defeitos severos na espermatogênese, como nos casos de aplasia de células germinativas e parada de maturação, algumas vezes espermatozóides não completamente maduros são utilizados para a ICSI.25 Além disso, tanto na aplasia germinativa como na parada de maturação espermática, alterações genéticas estão envolvidas com frequência27-29 podendo também explicar a menor fertilização neste casos.
Obtivemos 94,6% de divisão embrionária (tabela 2). Outros autores mostram resultados inferiores, variando de 65 a 75,8%8,9,24 e outros dois autores apresentaram resultados similares, obtendo 95,7 e 97,4 % de clivagem.20,25 Esta diferença talvez seja conseqüente da prevalência de pacientes com hipoespermatogênese na nossa série, enquanto que nos estudos onde a clivagem foi inferior predominavam casos de parada de maturação espermática e aplasia de células germinativas. Na nossa comparação entre os grupos, através da análise de tendência linear, verificamos clivagem superior no grupo com hipoespermatogênese (95,9%), seguido dos pacientes com parada de maturação (87,5%) e aplasia germinativa (71,4%) (p = 0,001) (tabela 2). Estes resultados estão parcialmente de acordo com os apresentados por Tournaye et al 24 que relatam taxa de clivagem inferior em pacientes com parada de maturação (61,4%) do que naqueles com hipoespermatogênese (82,8%) e aplasia germinativa (79,2%), porém sem diferença significativa.
O desenvolvimento embrionário foi similar entre os grupos estudados. Embriões de boa qualidade (graus I e II) totalizaram 74,8% do total de embriões clivados e não observamos diferença entre os grupos analisados (p = 0,403) (tabela 3) e este achado concorda com o apresentado por outros autores.24,25 No nosso estudo obtivemos 20 gestações clínicas.
]]> A taxa de gestação clínica observada no total de ciclos de fertilização iniciados (79 ciclos) e por ciclo onde foram inseminados oócitos (53 ciclos) foi 25,3% e 37,7% respectivamente. Na análise de gestações obtidas entre os grupos, a taxa de gestação por ciclo iniciado foi superior nos pacientes com hipoespermatogênese (36,7%) do que nos pacientes com parada de maturação (12,5%) e com aplasia germinativa (0%), porém diferença significativa foi observada somente com os pacientes com aplasia germinativa (p = 0,009) (tabela 2), probablemente porque nos pacientes com parada de maturação e com aplasia germinativa a taxa de obtenção de espermatozoides foi inferior. Quanto à taxa de gestação clínica por ciclos onde houve inseminação oocitária e tranferência embrionária, esta foi superior nos pacientes com hipoespermatogênese (41,9%) que naqueles com parada de maturação (28,6%) e com aplasia germinativa (0%), porém esta diferença não foi significatica, talvez devido ao pequeno número de ciclos nos pacientes com aplasia germinativa.Resultados semelhantes foram encontrados por outros autores, onde a taxa de gestação clínica por ciclo de transferência embrionária superior nos pacientes com hipoespermatogênese, porém esta diferença também não foi significativa.24,25 Um possível fator de confusão quanto a obtenção de gestação seria a idade da parceira. No nosso estudo a idade média feminina foi 33,7 anos +/- 5,1 anos, não havendo diferença estatística entre os grupos estudados (p = 0,08). Outro aspecto a ser considerado quanto é o número de embriões transferidos por ciclo. A literatura demonstra que as chances de gravidez aumentam numa proporção direta ao número de embriões transferidos, ao mesmo tempo que aumenta a chance de gestações múltiplas.30,31
No presente estudo o número médio de embriões transferidos nos pacientes com hipoespermatogênese, parada de maturação e aplasia germinativa foi, respectivamente, 3,6 , 2,7 e 1,7. A análise pela regressão linear mostrou diferença significativa no número de embriões transferidos em cada grupo (p = 0,025). Quatro gestações (20%) terminaram em abortamento espontâneo (tab), achado semelhante ao descrito pela literatura na população em geral (6,5 a 21%) e aqueles observados em pacientes submetidas à fertilização assistida (20 a 29%)32-35 Também está em conformidade com o resultado apresentado por Mercan et al 22 que observaram 22 (23,2%) abortamentos em 95 gestações obtidas através de fertilização oocitária com espermatozoides obtidos do parênquima testicular.
No presente estudo a biópsia testicular apresentou papel importante não apenas como diagnóstico, mas também como fator prognóstico em pacientes com azoospermia. Acreditamos que a fertilização assistida com TESA/TESE deva ser oferecida a todos os pacientes com azoospermia não obstrutiva, independente do padrão histopatológico do testículo. De um lado, pacientes com hipoespermatogênese devem ser encorajados frente a tratamentos de fertilização assistida, uma vez que a chance de obtenção de espermatozóides se aproxima a 100%. De outro lado pacientes com parada de maturação espermática e com aplasia germinativa devem orientados quanto à possibilidade de não se obter espermatozoides e nestes casos a possibilidade de uso de sêmen de doadores deve ser abordada.Acreditamos que séries maiores e prospectivas devam ser realizadas para confirmar nossos achados retrospectivos.
REFERÊNCIAS
1. Jaffe SB, Jewelewicz R. The basic infertility investigation. Fertil Steril 1991;56:599-613. [ Links ]
2. Palermo G, Joris H, Devroey P, Van Steiterghem A. Pregnancies after intracytoplasmic injection of a single spermatozoon into a oocyte. Lancet 1992;340:17-8. [ Links ]
3. Van Steiterghem A, Nagy Z, Joris H, Liu J, Staessen C, Smitz J, et al. High fertilization and implantation rates after intracytoplasmic sperm injection. Hum Reprod 1993;8:1061-6. [ Links ]
4. Schoysman R, Vanderzwalmen P, Nijs M, Segal-Bertin G, van de Casseye M. Successful fertilization by testicular spermatozoa in an in-vitro fertilization programme. Hum Reprod 1993;8:1339-40. [ Links ]
5. Schoysman R, Vanderzwalmen P, Nijs M, Segal L, Segal-Bertin C, Geerts L, et al. Pregnancy after fertilization with human testicular spermatozoa. Lancet 1993;342:1237. [ Links ]
6. Devroey P, Liu J, Nagy Z, Tournaye H, Silber SJ, Van Sterteghem AC. Normal fertilization of human oocytes after testicular sperm extraction and intracytoplasmic sperm injection. Fertil Steril 1994;62:639-41. [ Links ]
7. Devroey P, Liu J, Nagy Z, Goossens A, Tournaye H, Camus M, et al. Pregnancies after testicular sperm extraction and intracitoplasmic sperm injection in nonobstructive azoospermia. Hum Reprod 1995;10:1457-60. [ Links ]
8. Silber SJ, Nagy Z, Liu J, Tournaye H, Lissens V, Ferec C, et al. The use of epididimal and testicular spermatozoa for intracytoplasmic sperm injection: the genectic implication for male infertility. Hum Reprod 1995;10:2031-43. [ Links ]
9. Silber SJ, Van Steirteghem A, Liu J, Nagy Z, Tournaye H, Devroey P. High fertilization and pregnancy rate after intracitoplasmic sperm injection with spermatozoa obtained from testicle biopsy. Hum Reprod 1995;10:148-52. [ Links ]
10. Hartmann A, Telöken C. Biópsia de testículo. En: Badalotti M, Telöken C, Petracco A. Fertilidade e Infertilidade Humana. Rio de Janeiro : Editora MEDSI; 1997. p. 553-61. [ Links ]
11. Veeck L. The morphological assessment of human oocytes and early concept. En: Keel BA, Webster BW (eds). Handbook of the laboratory diagnosis and treatment of infertility. Boca Raton : CRC Press; 1990. p. 353-69. [ Links ]
12. Tournaye H, Verheyen G, Nagy P, Ubaldi F, Goossens A, Silber S, et al. Are there any predictive factors for successful testicular sperm recovery in azoospermic parients? Hum Reprod 1997;12:80-6. [ Links ]
13. Schlegel PN, Palermo GD, Goldstein M, Menendez S, Zaninovic N, Veeck LL, et al. Testicular sperm extraction with intracytoplasmic sperm injection for non-obstructive azoospermia. Urology 1997;49:435-40. [ Links ]
14. Mansour RT, Kamal A, Fahmy I, Tawab N, Serour GI, Aboulghar MA. Intracytoplasmic sperm injection in obstructive and non-obstructive azoospermia. Hum Reprod 1997;12:1974-9. [ Links ]
15. Ubaldi F, Nagy ZP, Rienzi L, Tessarik J, Annibaldo R, Franco G, et al. Reproductive capacity of spermatozoa from men with testicular failure. Hum Reprod 1999;14:2796-800. [ Links ]
16. Turek PJ, Cha I, Ljung BM. Systematic fine-needle aspiration of the testis: correlation to biopsy and results of organ mapping for mature sperm in azoospermic man. Urology 1997;49:743-8. [ Links ]
17. Turek PJ, Ljung BM, Cha I, Conaghan J. Diagnostic findings from testis fine needle aspiration mapping in obstructed and nonobstructed azoospermic men. J Urol 2000;163:1709-16. [ Links ]
18. Daya S. Overview analysis of ICSI outcomes. Recent advances in diagnosis and treatment of infertility. 28 th Annual Post Graduate Program of AFS. 1995 October 7-8; Seattle , United States . [ Links ]
19. Devroey P, Nagy P, Tournaye H, Liu J, Silber S, Van Steirteghem A. Outcome of intracytoplasmic sperm injection with testicular spermatozoa in obstructive and non-obstructive azoospermia. Hum Reprod 1996;11:1015-8. [ Links ]
20. Kahraman S, Ozgur S, Alatas C, Aksoy S, Tasdemir M, Nuhoglu B, et al. Fertility with testicular sperm extraction and intracytoplasmic sperm injection in non-obstructive azoospermic men. Hum Reprod 1996;11:756-60. [ Links ]
21. Witt M, Burt R, Massey J. The results of direct intracitoplasmic sperm injection using testicular sperm. 90th Annual Meeting of the American Urological Association; 1995 April 23-28; Las Vegas, Nevada. Abstract. [ Links ]
22. Mercan R, Urman B, Alatas C, Aksoy S, Nuhoglu A, Isiklar A, et al. Outcome of testicular sperm retrieval procedures in non-obstructive azoospermia: percutaneous aspiration versus open biopsy. Hum Reprod 2000;15:1548-51. [ Links ]
23. Ballesca JL, Balasch J, Calafell J, Alvarez R, Fabregues F, de Osaba M, et al. Serum inhibin B determination is predictive of successful testicular sperm extraction in men with non-obstructive azoospermia. Hum Reprod 2000;15:1734-8. [ Links ]
24. Tournaye H, Camus M, Goossens A, Nagy P, Liu J, Nagy Z, et al. Recent concepts in the management of infertility because of non-obstructive azoospermia. Hum Reprod 1995;10 Suppl 1:115-9. [ Links ]
25. De Croo I, Van Der Elst J, Everaert K, De Sutter P, Dhont M. Fertilization, pregnancy and embryo rates after ICSI in cases of obstructive and non-obstructive azoospermia. Hum Reprod 2000;15:1383-8. [ Links ]
26. Nagy ZP, Joris H, Verheyen G, Tournaye H, Devroey P, Van Steiterghen A. Correlation between motility of testicular spermatozoa, testicular histology and the outcome of intracytoplasmic sperm injection. Hum Reprod 1998;13:890-5. [ Links ]
27. Vogt P, Chandley A, Hargreave TP, Keil R, Ma K, Sharkey A. Microdelections in interval 6 of the Y chromosome of males with idiopathic sterility point to disruption of AZF, a human spermatiogenesis gene. Hum Genet 1992;89:491-6. [ Links ]
28. Martin-du-Pan RC, Campana A. Physiopathology of spermatogenic arrest. Fertil Steril 1993;60:937-46. [ Links ]
29. Reijo R, Lee TY, Salo P, Alagappan R, Brown LG, Rosenberg M, et al. Diverse spermatogenic defects in humans caused by Y chromosome deletions encompassing a novel RNA-binding protein gene. Nat Genet 1995;10:383-93. [ Links ]
30. Franco JG Jr. The risk of multifetal pregnancy. Hum Reprod 1994;9:185-6. [ Links ]
31. Walters DE. The statistical implication of the number of replacements' in embryo transfer. Hum Reprod 1996; 11:10 -2. [ Links ]
32. Jansen RP. Spontaneous abortion incidence in the treatment of infertility. Am J Obstet Gynecol 1982;143:451-73. [ Links ]
33. Warburton D, Fraser FC. Spontaneous abortion risks in man: data from retrospectives histories collected in a medical genetics unit. Am J Hum Genet 1964;16:1-25. [ Links ]
34. Dodson WC, Haney AF. Controlled ovarian hyperstimulation and intrauterine insemination for treatment of infertility. Fertil Steril 1991;55:457-67. [ Links ]
35. Horvath PM, Bohrer M, Sherden RM, Kemmann E. The relationship of sperm parameters to cycle fecundity in superovulated women undergoing intrauterine insemination. Fertil Steril 1989;52:288-91. [ Links ]
Conflicto de intereses: ninguno declarado.
]]>