
Saulo Molina-Giraldo, MD, MSc1; Jesús Bermúdes-Roa, MD2; Edgar Acuña-Osorio, MD3; Alejandro Franco-Hernández, MD4; José Luis Rojas-Arias, MD5
Recibido: febrero 20/12 - Aceptado: noviembre 13/12
1 Especialista en Medicina Materno-Fetal, Hospital de San José - Fundación Universitaria de Ciencias de la Salud (FUCS). Fellow Intervención Fetal, Baylor College of Medicine, Texas Children’s Fetal Center del Texas Children´s Hospital. Especialista en Docencia Universitaria. Magíster en Investigación. Director Programa de Terapia, Cirugía Fetal y Fetoscopia, Clínica Colsubsidio y Clínica de la Mujer. Especialista Unidad de Terapia Fetal, Hospital de San José. Profesor Asociado de Medicina Materno-Fetal, Fundación Universitaria de Ciencias de la Salud. Bogotá, Colombia. Mollina.saulo@ur.edu.co; saulo.molina@colsubsidio.com
2 Médico Ginecoobstetra, Universidad del Cauca. Fellow de Medicina Materno-Fetal, Hospital de San José - Fundación Universitaria de Ciencias de la Salud (FUCS). Bogotá, Colombia.
]]> 3 Médico Ginecoobstetra, Universidad del Rosario. Especialista en Medicina Materno-Fetal, Hospital San José - Fundación Universitaria de Ciencias de la Salud (FUCS). Fellow en Perinatología y Diagnóstico Prenatal, Yale University. Fellow en Intervencionismo Fetal, Saint Josephs Hospital, Tampa Fl. Jefe Servicio de la Unidad de Diagnóstico Prenatal y Medicina Materno-Fetal, Fundación Universitaria de Ciencias de la Salud, Hospital de San José. Coordinador del Posgrado de Medicina Materno-Fetal de la Fundación Universitaria de Ciencias de la Salud (FUCS). Bogotá, Colombia.4 Médico Ginecoobstetra, Universidad del Cauca. Especialista en Medicina Materno-Fetal, Hospital San José - Fundación Universitaria de Ciencias de la Salud (FUCS). Especialista, Unidad de Medicina Materno-Fetal, Hospital de San José. Bogotá, Colombia.
5 Especialista en Medicina Materno-Fetal, Hospital de San José (FUCS). Especialista en Epidemiología Clínica, Universidad del Rosario. Candidato a Magíster en Educación. Jefe Departamento de Obstetricia, Hospital de San José. Especialista Unidad de Terapia Fetal, Hospital de San José. Profesor Asociado de Ginecología y Obstetricia y de Medicina Materno-Fetal, Fundación Universitaria de Ciencias de la Salud (FUCS). Bogotá, Colombia.
RESUMEN
Introducción: el diagnóstico de corioamnionitis se basa en criterios clínicos que no alcanzan una sensibilidad mayor al 60%, y que tienen poca utilidad para predecir el compromiso fetal. El ultrasonido surge como una alternativa útil en el diagnóstico. Al mejorar el diagnóstico con la búsqueda de marcadores ecográficos de infección fetal podemos impactar en la morbimortalidad perinatal al poder intervenir de forma temprana a las gestantes en riesgo de compromiso fetal, especialmente corioamnionitis con curso subclínico. El objetivo de esta revisión es conocer la evidencia que soporta la asociación entre los hallazgos ecográficos del ultrasonido y la presencia de corioamnionitis e infección fetal in utero.
Materiales y métodos: se realizó una revisión de la literatura existente en las bases de datos medline, ovid, ebsco, ProQuest, lilacs, SciELO desde enero de 1985 hasta octubre de 2012. Se incluyeron los artículos de revisión e investigaciones originales.
Resultados: en las gestantes con parto pretérmino y ruptura prematura de membranas ovulares el acortamiento cervical, la presencia de "sludge", el oligohidramnios y la involución del timo son los marcadores que han mostrado mayor asociación con infección amniótica.
Conclusiones: el ultrasonido es una herramienta por considerar en el diagnóstico de infección materna y fetal in utero.
Palabras clave: corioamnionitis, diagnóstico prenatal, ultrasonografía, cuello uterino, timo, oligohidramnios, respiración, perfil biofísico, corazón fetal, ultrasonografía Doppler.
Introduction: A diagnosis of chorioamnionitis is based on clinical criteria which only manage 60% sensitivity and have little usefulness in predicting fetal compromise. Ultrasound emerges as a useful diagnostic alternative. An impact might be made on perinatal morbimortality by improving diagnosis through the search for echographic markers of fetal infection, thereby enabling early intervention in pregnant women at risk of fetal compromise, especially regarding subclinical chorioamnionitis. This review was aimed at providing evidence supporting an association between ultrasound’s echographic findings and the presence of chorioamnionitis in in utero (congenital) fetal infection.
Materials and methods: A review of the existing literature was made in medline, ovid, ebsco, ProQuest, lilacs and scielo databases from January 1985 to October 2012. Original research and review articles were included.
Results: Cervical length shortening, the presence of sludge, oligohydramnios and thymus involution are the markers which have been shown to have the greatest association with intra-amniotic infection.
Conclusions: Ultrasound is a tool to be considered when diagnosing in utero maternal and fetal infection.
Key words: Chorioamnionitis, diagnosis prenatal, ultrasonography, cervix, thymus, oligohydramnios, respiration, biophysical profile, fetal heart, Doppler ultrasonography.
INTRODUCCIÓN
La corioamnionitis o infección intraamniótica es una inflamación aguda de las membranas fetales y el corion placentario (1-3). Complica aproximadamente el 40% de los partos pretérmino espontáneos y el 70% de los complicados con ruptura prematura de membranas ovulares (PPROM) (4-6). El parto pretérmino secundario a infección es una forma de protección fetal a la injuria infecciosa (7, 8). El feto desarrolla un síndrome de respuesta inflamatoria (FIRS) que es el estado más avanzado de la inflamación e infección intraamniótica (9),con aumento de la morbilidad neonatal dada por presencia de síndrome de dificultad respiratoria, neumonía neonatal, sepsis neonatal, displasia broncopulmonar, hemorragia intraventricular, enterocolitis necrotizante, leucomalacia periventricular y parálisis cerebral (10-16).
En la actualidad, el diagnóstico de corioamnionitis se fundamenta en los criterios clínicos definidos por Gibbs, que están basados en la respuesta clínica y paraclínica materna y fetal a la injuria infecciosa (17). Estos criterios son de baja prevalencia cuando la infección tiene un curso subclínico y no alcanzan una sensibilidad superior al 60%. El estudio bioquímico y tinción de Gram del líquido amniótico alcanza una sensibilidad del 24 al 57%, y el aislamiento microbiológico específico en el cultivo de líquido amniótico se consigue tan solo en el 60% de los casos, ya que la infección es polimicrobiana en el 65% de los casos; algunos gérmenes implicados, como el Mycoplasma y el Ureaplasma -presentes en el 30 al 47% de las corioamnionitis- son técnicamente difíciles de aislar en los cultivos (3-9).
Debido a esta pobre sensibilidad diagnóstica se han descrito marcadores ultrasonográficos que presentan asociación con corioamnionitis y con el compromiso fetal in utero. El estudio de estos marcadores ecográficos se basa en la respuesta inflamatoria fetal a la noxa infecciosa que se refleja en las manifestaciones a nivel del sistema hematopoyético, glándulas suprarrenales, el timo, el corazón, el encéfalo, los riñones, los pulmones y la piel fetal (9).
]]> El objetivo de esta revisión es evaluar la evidencia que soporta la asociación entre los diferentes marcadores ecográficos estudiados hasta la actualidad y el diagnóstico de corioamnionitis e infección fetal in utero.MATERIALES y MÉTODOS
Se realizó una revisión de la literatura registrada en las bases de datos medline, ebsco, Ovid y Pro-Quest entre enero de 1985 a octubre de 2012. Se consultaron artículos publicados en inglés y español con los términos MeSH "chorioamnionitis", "short cérvix", "sludge", "fetal thymus", "oligohydramnios", "fetal breathing movements", "biophysical profile", "fetal cardiac dysfunction", "Doppler de arteria umbilical". Se incluyeron aquellos artículos de revisión, estudio de cohorte y casos, y controles e investigaciones originales con relación al tema de investigación. También se realizó una búsqueda en la biblioteca virtual en salud lilacs y Scientific Electronic Library Online (SciELO) con el fin de establecer datos de estudios latinoamericanos.
RESULTADOS
Se encontraron 185 artículos referentes a los términos MeSH planteados, de los cuales 54 artículos publicados en inglés y dos publicados en español cumplieron con los criterios de inclusión. Dichos artículos fueron clasificados de acuerdo con el contenido en definición, los métodos diagnósticos y los resultados perinatales del tema estudiado. De estos 56 artículos, 28 fueron estudios observacionales, descriptivos, y de casos y controles que estudiaron la asociación de los diferentes marcadores ecográficos con infección intraamniótica y compromiso fetal in utero. Se incluyeron seis artículos donde se estudió la asociación entre acortamiento del cérvix e infección intraamniótica, dos estudios de "sludge", tres estudios de involución del timo fetal, cinco de oligohidramnios, nueve de movimientos respiratorios fetales y perfil biofísico fetal, dos estudios de disfunción miocárdica fetal y, finalmente, el único estudio que ha investigado la asociación entre índices Doppler de arteria umbilical con infección intraamniótica (figura 1).

Acortamiento cervical (cérvix corto)
La invasión microbiana en el espacio corio-decidual va a desencadenar la síntesis y liberación de sustancias vasoactivas y útero-tónicas como son las prostaglandinas; además de mediadores proinflamatorios como las citocinas IL 1, IL 6, IL 8 y FNT y metaloproteinasas que van a desencadenar en últimas el inicio de la actividad uterina y los cambios en la longitud cervical (18). El acortamiento de la longitud cervical detectado por ultrasonografía transvaginal puede ser un método de diagnóstico no invasivo para determinar la presencia de infección o inflamación intraamniótica (18-20). Un cérvix corto, definido como aquel menor de 25 mm de longitud, predispone al ascenso de bacterias a nivel intrauterino, inflamación intrauterina e infección intraamniótica (21).
Hasta en el 50% de las pacientes con cérvix corto se ha documentado infección intraamniótica (2123) antes de las 24 semanas de gestación. También se ha documentado inflamación intraamniótica en el 80% de las pacientes con insuficiencia cervical (24). El acortamiento de la longitud cervical se comporta como un factor de riesgo independiente para parto pretérmino y resultado perinatal adverso, lo cual tiene asociación con la presencia de infección intraamniótica subclínica o inflamación. Holst encontró que un cérvix menor de 15 mm confería un RR de 3,6 (IC 95%: 1,9-10,0) con una sensibilidad del 72%, y una especificidad del 83% (25). Diferentes autores han llevado a cabo estudios para evaluar el desempeño de cérvix en la cervicometría como un marcador predictor de inflamación e infección intraamniótica y, por ende, de parto pretérmino y ruptura prematura de membranas. Los estudios publicados, con un tamaño de muestra pequeño, han demostrado esta asociación en términos de la longitud cervical, tiempo entre la admisión y el parto, y presencia de citoquinas inflamatorias; se sugiere por parte de los diferentes autores su uso como una herramienta para predecir qué gestaciones cursan o no con inflamación e infección intraamniótica, y tomar las medidas pertinentes para disminuir el daño causado por la injuria fetal secundaria a su respuesta inflamatoria (22-29).
]]> Presencia de "sludge" en la cervicometríaEl término "sludge" se define como la presencia de material particulado ecogénico contenido en la bolsa amniótica visualizado al realizar la cervicometría (figuras 2a, 2b, 2c). La importancia de su hallazgo se debe a que se ha asociado con la presencia de infección intraamniótica (30). En el estudio publicado por Espinoza en el 2005, refieren la presencia de "sludge" en el 58,3% de las pacientes con trabajo de parto pretérmino con membranas intactas y con cervicometría menor o igual a 15 mm (31). Además, reportan asociación con infección intraamniótica hasta en el 33,3% de las pacientes, y con corioamnionitis histológica en el 77,8%. Estos hallazgos se correlacionaron con una tasa de partos menores de 35 semanas en el 28,8% de los casos. Al realizar el análisis de regresión logística se encontró que la presencia de "sludge" se comporta como un factor de riesgo independiente para la ocurrencia de infección intraamniótica y corioamnionitis histológica (31). En otro estudio publicado por Kusanovic et al. en el 2007, refieren la presencia de "sludge" en el 23,5% de pacientes asintomáticas con alto riesgo de parto pretérmino; además, reportan una asociación de "sludge" con parto pretérmino menor de 35 semanas del 62,2%; con ruptura prematura de membranas ovulares pretérmino de 39,4%, con corioamnionitis clínica del 15,2%, con corioamnionitis histológica del 61,5%, y con funisitis del 32,3%. Informan que la combinación de cérvix corto menor de 25 mm y la presencia de "sludge" confieren un odds ratio de 9,9 (IC 95%: 3-32,4) para parto pretérmino espontáneo antes de las 32 semanas. Basados en sus resultados, los autores concluyeron que la presencia de "sludge" se comporta como un factor de riesgo independiente para parto pretérmino, ruptura prematura de membranas ovulares pretérmino, corioamnionitis clínica y corioamnionitis histológica en pacientes asintomáticas con alto riesgo para parto pretérmino. Estas observaciones los llevaron a proponer el "sludge" como un signo ultrasonográfico para identificar las pacientes con alto riesgo de infección e inflamación intraamniótica en mujeres con alto riesgo de parto pretérmino (32).
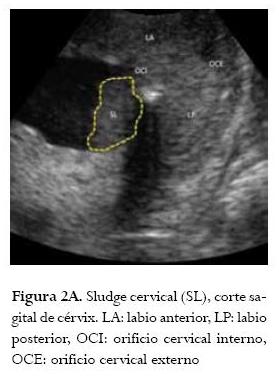
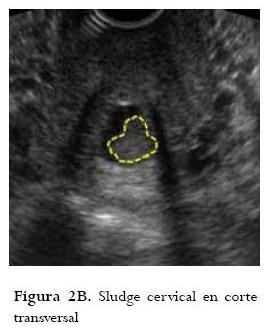
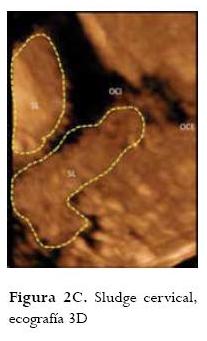
Involución del timo fetal
El timo es una glándula importante para la maduración del sistema inmune fetal. Normalmente esta glándula se involuciona con la edad. Se ha observado que tanto en fetos como en neonatos esta involución puede darse de forma aguda en respuesta a cualquier estrés agudo como la desnutrición y la sepsis. Esta involución es la consecuencia del efecto apoptótico de los corticoides sobre los linfocitos de la médula y la corteza debido a que el estrés conlleva la activación del eje hipotálamo-hipófisis-suprarrenal. Hay evidencia de que la activación de este eje, mediada por el estrés, es la consecuencia de la síntesis y liberación de citocinas proinflamatorias (IL-1, IL-6) ante la presencia de infección intraamniótica y fetal. Por ello, se sugiere que la involución del timo hace parte de la disfunción orgánica observada en fetos comprometidos con infección intraamniótica; este signo se ha documentado en fetos con parto pretérmino, corioamnionitis clínica y ruptura prematura de membranas ovulares pretérmino (33). Por eso se propone la evaluación del tamaño del timo como un marcador ecográfico de infección fetal in utero (figura 3). Di Naro et al. publicaron en el año 2005 un estudio donde demostraron 100% de funisitis en pacientes con un diámetro del timo por debajo del percentil 5 para la edad gestacional (34).
]]> Además, El Haieg et al., reportan un estudio en el año 2008 donde encuentran que la involución del timo tiene una sensibilidad del 93% y una especificidad del 75% para identificar síndrome de respuesta inflamatoria fetal y funisitis (34-36).Presencia de oligohidramnios
El oligohidramnios se define como la presencia de una cantidad de líquido amniótico menor o igual a 5 cm al evaluar el índice de líquido amniótico en la técnica de cuatro cuadrantes, o por debajo del percentil 5 para la edad gestacional. Se considera que hasta en un tercio de las pacientes con ruptura prematura de membranas ovulares el oligohidramnios está asociado a invasión microbiana de la cavidad amniótica (5). El oligohidramnios presente en las pacientes con ruptura prematura de membranas ovulares pretérmino se debe principalmente al escape de líquido amniótico. Pero con la instauración del síndrome de respuesta inflamatoria fetal hay compromiso del flujo sanguíneo renal del feto que lleva a la disminución de la producción de orina fetal y, por consiguiente, a la disminución del índice de líquido amniótico. Por lo anterior, se considera que el oligohidramnios es un marcador de infección fetal y se ha estudiado su relación con infección intraamniótica (9).
La asociación de oligohidramnios e infección intraamniótica aumenta el riesgo de parto pretérmino dentro de las primeras 48 horas, y es un marcador de resultado adverso perinatal y terminación de la gestación (37). En las pacientes con parto pretérmino y oligohidramnios sin ruptura prematura de membrana también se ha documentado una mayor asociación con inflamación intraamniótica, corioamnionitis histológica y corioamnionitis clínica (38).
Los diferentes estudios publicados hasta la fecha muestran que el oligohidramnios presente en las pacientes con ruptura prematura de membranas ovulares pretérmino se asocia fuertemente con inflamación intraamniótica, cultivos positivos y corioamnionitis histológica al compararlos con aquellas pacientes sin oligohidramnios y con ruptura prematura de membranas. Además, se asocia con una mayor tasa de partos a las 48 horas de documentación del oligohidramnios, signo que se cataloga como un mal predictor para manejo expectante en ruptura prematura de membranas ovulares pretérmino. Por ello, se ha utilizado como una herramienta para predecir infección intraamniótica y compromiso fetal (37-41).
Perfil biofísico fetal, movimientos respiratorios fetales e infección intraamniótica
El perfil biofísico fetal (PBF) es un test originalmente desarrollado por Manning en 1980 para detectar compromiso del estado fetal durante la insuficiencia útero-placentaria. El objetivo primario del PBF es detectar tempranamente la hipoxia fetal ante parto para evitar el daño permanente resultante de la asfixia fetal y reducir la muerte fetal in utero (42). El PBF se empezó a usar en el manejo de las pacientes con ruptura prematura de membranas ovulares pretérmino para diagnosticar la infección intraamniótica subclínica y disminuir el riesgo de infección fetal. Se cree que la liberación de mediadores inflamatorios secundarios a infección de la cavidad amniótica puede ser responsable de los cambios del PBF en infección intraamniótica, como son: disminución de movimientos respiratorios fetales, disminución de movimientos fetales y oligohidramnios (42). Hay investigaciones a favor y en contra de la utilidad del PBF en la predicción de infección perinatal. Vintzileos et al. en 1985 encontraron entre 73 mujeres con ruptura prematura de membranas ovulares pretérmino sin trabajo de parto que una puntuación menor de 8 se asoció con una tasa de infección del 93,7% comparada con 2,7% de aquellos con una puntuación normal. Ellos concluyen que el PBF es un buen predictor de infección cuando el intervalo entre la realización del test y el parto es menor de 24 horas (43). En 1986 estos mismos autores encontraron en 130 pacientes con ruptura prematura de membranas ovulares pretérmino que la ausencia de movimientos respiratorios fetales es muy buen predictor de infección fetal. La sensibilidad y especificidad informada por este autor para la ausencia de movimientos fetales para predecir infección fetal fue del 91,6 y 64,8% (44). En 1991, Roberts también encontró que el PBF y los movimientos respiratorios fetales tienen una sensibilidad de 92% y una especificidad del 59% similares a lo informado por Vintzileos (45).
Miller en 1990 y Del Valle en 1992 concluyen en sus estudios que el PBF y el monitoreo fetal son malos predictores de infección fetal in utero (4647). En numerosos estudios de diferentes autores, aunque se encuentra asociación entre la ausencia de movimientos respiratorios fetales e infección e inflamación intraamniótica y fetal, esta asociación no es estadísticamente significativa, lo cual puede deberse al pequeño tamaño de muestra de los estudios, lo que requeriría de investigaciones prospectivas aleatorizadas con buen tamaño muestral para encontrar una asociación estadísticamente significativa (48-51).
Lo que queda claro hasta la fecha es que el PBF permite descartar de manera fiable la ausencia de infección pero solo en las 24 horas posteriores al test y previas al parto, y que la presencia de movimientos respiratorios fetales predice la ausencia de infección en fetos con ruptura prematura de membranas ovulares pretérmino, pero su ausencia no se correlaciona fiablemente con la presencia de infección intraamniótica (42-51).
Disfunción miocárdica e infección fetal
]]> El corazón fetal es uno de los órganos afectados durante la disfunción orgánica que se presenta con el síndrome de respuesta inflamatoria fetal secundaria a infección intraamniótica (9).En el síndrome de respuesta inflamatoria fetal se observa una redistribución de la circulación arterial como mecanismo secundario para preservar el flujo sanguíneo cerebral ante una disminución del gasto cardiaco. Los fetos incapaces de cambiar la compliance cardiaca no logran mantener un adecuado volumen de latido llevando a hipoperfusión cerebral con hipotensión e isquemia cerebral in utero, favoreciendo el desarrollo de leucomalacia periventricular (52).
Yanowitz reportó que los neonatos nacidos con corioamnionitis histológica presentan anormalidades hemodinámicas que incluyen disminución de la presión arterial diastólica que contribuye a la hipoperfusión cerebral (52). Por tanto, los cambios en la función diastólica fetal observados en fetos con ruptura prematura de membranas ovulares pretérmino pueden evaluarse in utero para corroborar diagnóstico de infección fetal y predecir los que tienen un mayor riesgo de desarrollar leucomalacia periventricular (53-54).
El índice de Tei, o índice de rendimiento miocárdico, es un índice Doppler no invasivo para evaluar la función sistólica y diastólica fetal. Consiste en la relación entre la duración del periodo isovolumétrico (contracción y relajación) y la duración del periodo de eyección en el ventrículo izquierdo fetal. Este índice es usado para evaluar la disfunción ventricular en fetos con restricción de crecimiento e infección (55) (figura 4).
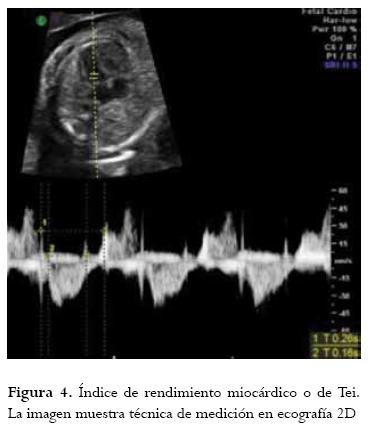
En el año 2004 Romero encontró aumento de la compliance del ventrículo izquierdo en fetos con ruptura prematura de membranas ovulares pretérmino e infección intraamniótica (53). En el año 2010 Letti encontró que el índice Tei es una buena herramienta para evaluar la función cardiaca en fetos afectados con síndrome de respuesta inflamatoria en el contexto de la ruptura prematura de membranas ovulares pretérmino en quienes el Tei índex fue mayor comparado con aquellos sin ruptura prematura de membranas (54).
Índices doppler de la arteria umbilical
Los índices Doppler de la arteria umbilical (AU) son una herramienta diagnóstica no invasiva útil para la clasificación de la restricción del crecimiento fetal de acuerdo con sus alteraciones hemodinámicas, y para predecir las complicaciones perinatales en estos fetos. En la ruptura prematura de membranas ovulares pretérmino no se han logrado relacionar los índices Doppler con invasión microbiana de la cavidad amniótica, corioamnionitis clínica e infección perinatal.
El único estudio hasta la fecha que ha investigado esta relación lo realizó Ovalle et al. en Chile y fue publicado en el año 2005. Ellos evaluaron el Doppler de arteria umbilical en 80 fetos de embarazos con ruptura prematura de membranas ovulares pretérmino entre 24 a 34 semanas de gestación, y encontraron que no había diferencia en la relación sístole/diástole en los grupos con o sin invasión microbiana de la cavidad amniótica. Pero sí encontraron una relación sístole/diástole de la arteria umbilical más alta en aquellos fetos con resultado perinatal adverso. Ellos concluyen en su estudio que en embarazadas con ruptura prematura de membranas ovulares pretérmino y funisitis, el Doppler de la arteria umbilical puede discriminar entre los fetos que tendrán un resultado perinatal adverso y aquellos con buen resultado neonatal. Con el Doppler de la arteria umbilical no es posible detectar invasión microbiana de la cavidad amniótica y funisitis (56).
]]> DISCUSIÓNLa corioamnionitis es una entidad frecuente cuyo diagnóstico prenatal se basa en criterios clínicos y paraclínicos maternos-fetales, y en el aislamiento microbiológico, siendo estos criterios de baja sensibilidad, que dejan un grupo grande de esta población (30 a 40%) sin diagnóstico, con la consiguiente morbilidad que implica. También existen marcadores bioquímicos de inflamación intraamniótica que mejoran la capacidad diagnóstica como la IL 6 en líquido amniótico con una sensibilidad del 81% y una especificidad del 75%, o la metaloproteinasa con una sensibilidad de 90% y una especificidad del 80%, pero son pruebas costosas y no están disponibles en todos nuestros laboratorios (3).
Debido a estas dificultades en el diagnóstico de corioamnionitis, diferentes investigadores han llevado a cabos múltiples estudios que, basados en la fisiopatología de la corioamnionitis y en el síndrome de respuesta inflamatoria fetal, han demostrado correlación entre alteraciones ultrasonográficas y esta infección (9). Hay marcadores ecográficos que según la revisión realizada han demostrado asociación estadísticamente significativa con infección o inflamación intraamniótica, inflamación o infección fetal in utero, y corioamnionitis histológica. En la actualidad, el acortamiento de la longitud cervical menor de 25 mm, la presencia de "sludge" en la cervicometría, la involución del timo fetal, y el oligohidramnios son los marcadores ecográficos que mejor relación con infección intraamniotica han mostrado. La presencia de movimientos respiratorios fetales ha demostrado tener muy buena especificidad para descartar la infección intraamniótica, y su ausencia es buen predictor de la misma (44, 48, 51). Los otros marcadores estudiados -el perfil biofísico fetal, el índice de rendimiento miocárdico y los índices Doppler de la arteria umbilical-, aunque han mostrado asociación con infección intraamniótica y compromiso fetal in utero, esta asociación no ha demostrado ser estadísticamente significativa, lo cual puede deberse a los pocos estudios realizados con pequeños tamaños de muestra, por lo que se requerirían nuevos estudios prospectivos aleatorizados para poder demostrar su verdadera utilidad como herramientas diagnósticas para la infección intraamniótica y la infección fetal in utero. Por eso creemos que al combinar la causa del parto pretérmino con los marcadores clínicos y los marcadores ecográficos de corioamnionitis e infección fetal in utero es posible conseguir sensibilidades diagnósticas por encima del 80%, que además serían costo-efectivas, y fácilmente aplicables y reproducibles en todas las unidades de medicina materno-fetal.
Hasta la fecha, todos los signos ultrasonográficos se han evaluado de forma aislada, y desconocemos su utilidad y el mejoramiento de la capacidad diagnóstica de estos aplicados al mismo tiempo en este grupo de pacientes, con el fin de disminuir la morbilidad perinatal. Se requieren revisiones que evalúen la exactitud diagnóstica de los marcadores ultrasonográficos de infección amniótica.
CONCLUSIÓN
En la literatura hay evidencia que soporta el uso del ultrasonido en busca de marcadores de infección intraamniótica y de infección fetal en útero. Marcadores ecográficos como el acortamiento del cérvix, el "sludge", la involución del timo, el oligohidramnios, la ausencia de movimientos fetales y la disfunción miocárdica han demostrado ser útiles para determinar compromiso fetal en infección intraamniótica, y pueden servir a fin de determinar el mejor momento para la terminación de la gestación y prevenir las secuelas perinatales a corto y largo plazo.
Agradecimientos. Al grupo de docentes y residentes de la Unidad de Medicina Materno-Fetal del Hospital San José de Bogotá por su amable e incondicional colaboración para la realización de esta revisión bibliográfica.
REFERENCIAS
1. Newton ER. Chorioamnionitis and intraamniotic infection. Clin Obstet Gynecol 1993;36:795-808. [ Links ]
]]>2. Riggs JW, Blanco JD. Pathophysiology, diagnosis, and management of intraamniotic infection. Semin Perinatol 1998;22:251-9. [ Links ]
3. Tita AT, Andrews WW. Diagnosis and management of clinical chorioamnionitis. Clin Perinatol 2010; 37:339-54. [ Links ]
4. Soper DE, Mayhall CG, Dalton HP. Risk factors for intraamniotic infection: a prospective epidemiologic study. Am J Obstet Gynecol 1989;161:562-6. [ Links ]
5. Shim SS, Romero R, Hong JS, Park CW, Jun JK, Kim BI, et al. Clinical significance of intra-amniotic inflammation in patients with preterm premature rupture of membranes. Am J Obstet Gynecol 2004; 191:1339-45. [ Links ]
6. Yoon BH, Romero R, Moon JB, Shim SS, Kim M, Kim G, et al. Clinical significance of intra-amniotic inflammation in patients with preterm labor and intact membranes. Am J Obstet Gynecol 2001;185:1130-6. [ Links ]
]]>7 . Lee SE, Romero R, Jung H, Park CW, Park JS, Yoon BH. The intensity of the fetal inflammatory response in intraamniotic inflammation with and without microbial invasion of the amniotic cavity. Am J Obstet Gynecol 2007;197:294-6. [ Links ]
8. Edwards RK. Chorioamnionitis and labor. Obstet Gynecol Clin North Am 2005;32:287-96. [ Links ]
9. Gotsch F, Romero R, Kusanovic JP, Mazaki-Tovi S, Pineles BL, Erez O, et al. The fetal inflammatory response syndrome. Clin Obstet Gynecol 2007;50:652-83. [ Links ]
10. Hagberg H, Mallard C, Jacobsson B. Role of cytokines in preterm labour and brain injury. BJOG 2005;112:16-8. [ Links ]
11. Bracci R, Buonocore G. Chorioamnionitis: a risk factor for fetal and neonatal morbidity. Biol Neonate 2003;83:85-96. [ Links ]
]]>12. Wu YW, Colford JM Jr. Chorioamnionitis as a risk factor for cerebral palsy: A meta-analysis. JAMA 2000;284:1417-24. [ Links ]
13. Wu YW. Systematic review of chorioamnionitis and cerebral palsy. Ment Retard Dev Disabil Res Rev 2002;8:25-9. [ Links ]
14. Speer CP. Chorioamnionitis, postnatal factors and proinflammator y response in the pathogenetic sequence of bronchopulmonary dysplasia. Neonatology 2009;95:61. [ Links ]
15. Been JV, Zimmermann LJ. Histological chorioamnionitis and respiratory outcome in preterm infants. Arch Dis Child Fetal Neonatal Ed 2009;94:F218-25. [ Links ]
16. Shatrov JG, Birch SC, Lam LT, Quinlivan JA, McIntyre S, Mendz GL. Chorioamnionitis and cerebral palsy: a meta-analysis. Obstet Gynecol 2010;116:387-92. [ Links ]
]]>17. Gibbs RS, Duff P. Progress in pathogenesis and management of clinical intraamniotic infection. Am J Obstet Gynecol 1991;164:1317-26. [ Links ]
18. Park JS, Park CW, Lockwood CJ, Norwitz ER. Role of cytokines in preterm labor and birth. Minerva Ginecol 2005;57:349-66. [ Links ]
19. Park CW, Moon KC, Park JS, Jun JK, Romero R, Yoon BH. The involvement of human amnion in histologic chorioamnionitis is an indicator that a fetal and an intra-amniotic inflammatory response is more likely and severe: clinical implications. Placenta 2009;30:56-61. [ Links ]
20. Keeler SM, Kiefer DG, Rust OA, Vintzileos A, Atlas RO, Bornstein E, et al. Comprehensive amniotic fluid cytokine profile evaluation in women with a short cervix: which cytokine(s) correlates best with outcome? Am J Obstet Gynecol 2009;201:276. [ Links ]
21. Mays JK, Figueroa R, Shah J, Khakoo H, Kaminsky S, Tejani N. Amniocentesis for selection before rescue cerclage. Obstet Gynecol 2000;95:652-5. [ Links ]
]]>22. Romero R, Gonzalez R, Sepulveda W, Brandt F, Ramirez M, Sorokin Y, et al. Infection and labor. VIII. Microbial invasion of the amniotic cavity in patients with suspected cervical incompetence: prevalence and clinical significance. Am J Obstet Gynecol 1992; 167:1086-91. [ Links ]
23. Hassan S, Romero R, Hendler I, Gomez R, Khalek N, Espinoza J, et al. A sonographic short cervix as the only clinical manifestation of intra-amniotic infection. J Perinat Med 2006;34:13-9. [ Links ]
24. Lee SE, Romero R, Park CW, Jun JK, Yoon BH. The frequency and significance of intraamniotic inflammation in patients with cervical insufficiency. Am J Obstet Gynecol 2008;198:633-8. [ Links ]
25. Holst RM, Jacobsson B, Hagberg H, Wennerholm UB. Cervical length in women in preterm labor with intact membranes: relationship to intraamniotic inflammation/microbial invasion, cervical inflammation and preterm delivery. Ultrasound Obstet Gynecol 2006;28:768-74. [ Links ]
26. Rizzo G, Capponi A, Vlachopoulou A, Angelini E, Grassi C, Romanini C. Ultrasonographic assessment of the uterine cervix and interleukin-8 concentrations in cervical secretions predict intrauterine infection in patients with preterm labor and intact membranes. Ultrasound Obstet Gynecol 1998;12:86-92. [ Links ]
]]>27. Gire C, Faggianelli P, Nicaise C, Shojai R, Fiori A, Chau C, et al. Ultrasonographic evaluation of cervical length in pregnancies complicated by preterm premature rupture of membranes. Ultrasound Obstet Gynecol 2002;19:565-9. [ Links ]
28. Kiefer DG, Keeler SM, Rust OA, Wayock CP, Vintzileos AM, Hanna N. Is midtrimester short cervix a sign of intraamniotic inflammation? Am J Obstet Gynecol 2009;200:374-5. [ Links ]
29. Vaisbuch E, Hassan SS, Mazaki-Tovi S, Nhan-Chang CL, Kusanovic JP, Chaiworapongsa T, et al. Patients with an asymptomatic short cer vix (<or=15 mm) have a high rate of subclinical intraamniotic inflammation: implications for patient counseling. Am J Obstet Gynecol 2010;202:433-8. [ Links ]
30. Romero R, Kusanovic JP, Espinoza J, Gotsch F, Nhan-Chang CL, Erez O, et al. What is amniotic fluid "sludge"? Ultrasound Obstet Gynecol 2007;30:793-8. [ Links ]
31. Espinoza J, Gonçalves LF, Romero R, Nien JK, Stites S, Kim YM, et al. The prevalence and clinical significance of amniotic fluid "sludge" in patients with preterm labor and intact membranes. Ultrasound Obstet Gynecol 2005;25:346-52. [ Links ]
]]>32. Kusanovic JP, Espinoza J, Romero R, Gonçalves LF, Nien JK, Soto E, et al. Clinical significance of the presence of amniotic fluid "sludge" in asymptomatic patients at high risk for spontaneous preterm delivery. Ultrasound Obstet Gynecol 2007;30:706-14. [ Links ]
33. Toti P, De FC, Stumpo M, Schürfeld K, Di Leo L, Vatti R, et al. Acute thymic involution in fetuses and neonates with chorioamnionitis. Hum Pathol 2000;31:1121-8. [ Links ]
34. Di NE, Cromi A, Ghezzi F, Raio L, Uccella S, D'Addario V, et al. Fetal thymic involution: a sonographic marker of the fetal inflammatory response syndrome. Am J Obstet Gynecol 2006;194:153-9. [ Links ]
35. Yinon Y, Zalel Y, Weisz B, Mazaki-Tovi S, Sivan E, Schiff E, et al. Fetal thymus size as a predictor of chorioamnionitis in women with preterm premature rupture of membranes. Ultrasound Obstet Gynecol 2007;29:639-43. [ Links ]
36. El-Haieg DO, Zidan AA, El-Nemr MM. The relationship between sonographic fetal thymus size and the components of the systemic fetal inflammatory response syndrome in women with preterm prelabour rupture of membranes. BJOG 2008;115:836-41. [ Links ]
]]>37. Park JS, Yoon BH, Romero R, Moon JB, Oh SY, Kim JC, et al. The relationship between oligohydramnios and the onset of preterm labor in preterm premature rupture of membranes. Am J Obstet Gynecol 2001; 184:459-62. [ Links ]
38. Kim BJ, Romero R, Mi Lee S, Park CW, Shin Park J, Jun JK, et al. Clinical significance of oligohydramnios in patients with preterm labor and intact membranes. J Perinat Med 2011;39:131-6. [ Links ]
39. Lee SE, Romero R, Lee SM, Yoon BH. Amniotic fluid volume in intra-amniotic inflammation with and without culture-proven amniotic fluid infection in preterm premature rupture of membranes. J Perinat Med 2010;38:39-44. [ Links ]
40. Lao TT, Cheung VY. Expectant management of preterm prelabour rupture of membranes--the significance of oligohydramnios at presentation. Eur J Obstet Gynecol Reprod Biol 1993;48:87-91. [ Links ]
41. Yoon BH, Kim YA, Romero R, Kim JC, Park KH, Kim MH, et al. Association of oligohydramnios in women with preterm premature rupture of membranes with an inflammatory response in fetal, amniotic, and maternal compartments. Am J Obstet Gynecol 1999;181:784-8. [ Links ]
]]>42. Oyelese Y, Vintzileos AM. The uses and limitations of the fetal biophysical profile. Clin Perinatol 2011; 38:47-vi. [ Links ]
43. Vintzileos AM, Campbell WA, Nochimson DJ, Connolly ME, Fuenfer MM, Hoehn GJ. The fetal biophysical profile in patients with premature rupture of the membranes-an early predictor of fetal infection. Am J Obstet Gynecol 1985;152:510-6. [ Links ]
44. Vintzileos AM, Campbell WA, Nochimson DJ, Weinbaum PJ. Fetal breathing as a predictor of infection in premature rupture of the membranes. Obstet Gynecol 1986;67:813-7. [ Links ]
45. Roberts AB, Goldstein I, Romero R, Hobbins JC. Comparison of total fetal activity measurement with the biophysical profile in predicting intra-amniotic infection in preterm premature rupture of membranes. Ultrasound Obstet Gynecol 1991;1:36-9. [ Links ]
46. Miller JM, Jr, Kho MS, Brown HL, Gabert HA. Clinical chorioamnionitis is not predicted by an ultrasonic biophysical profile in patients with premature rupture of membranes. Obstet Gynecol 1990;76:1051-4. [ Links ]
]]>47. Del Valle GO, Joffe GM, Izquierdo LA, Smith JF, Gilson GJ, Curet LB. The biophysical profile and the nonstress test: poor predictors of chorioamnionitis and fetal infection in prolonged preterm premature rupture of membranes. Obstet Gynecol 1992;80:106-10. [ Links ]
48. Agustsson P, Patel NB. The predictive value of fetal breathing movements in the diagnosis of preterm labour. Br J Obstet Gynaecol 1987;94:860-3. [ Links ]
49. Ohlsson A, Fong K, Hannah M, Heyman Z, Gonen R, Rose T, et al. Prediction of lethal pulmonary hypoplasia and chorioamnionitis by assessment of fetal breathing. Br J Obstet Gynaecol 1991;98:692-7. [ Links ]
50. Vintzileos AM, Campbell WA. Clinical chorioamnionitis is not predicted by an ultrasonic biophysical profile in patients with premature rupture of membranes. Obstet Gynecol 1991;77:649-51. [ Links ]
51. Sherer DM, Spong CY, Salafia CM. Fetal breathing movements within 24 hours of delivery in prematurity are related to histologic and clinical evidence of amnionitis. Am J Perinatol 1997;14:337-40. [ Links ]
]]>52. Yanowitz TD, Jordan JA, Gilmour CH, Towbin R, Bowen A, Roberts JM, et al. Hemodynamic disturbances in premature infants born after chorioamnionitis: association with cord blood cytokine concentrations. Pediatr Res 2002;51:310-6. [ Links ]
53. Romero R, Espinoza J, Goncalves LF, Gomez R, Medina L, Silva M, et al. Fetal cardiac dysfunction in preterm premature rupture of membranes. J Matern Fetal Neonatal Med 2004;16:146-57. [ Links ]
54. Letti Muller AL, Barrios PM, Kliemann LM, Valerio EG, Gasnier R, Magalhaes JA. Tei index to assess fetal cardiac performance in fetuses at risk for fetal inflammatory response syndrome. Ultrasound Obstet Gynecol 2010;36:26-31. [ Links ]
55. Arreaza M, Rojas JD, Molina S. Síndrome de Respuesta Inflamatoria Fetal (FIRS): adaptación cardiovascular. Rev Colomb Obstet Ginecol 2011;62:71-81. [ Links ]
56. Ovalle A, Figueroa J, Gomez R. Relacion entre Doppler de la Arteria Umbilical, invasión microbiana de la cavidad amniótica, funisitis y resultado adverso neonatal en la rotura prematura de membranas pretérmino. Revista Chilena de Obstetricia y Ginecología 2005;70: 375-85. [ Links ]
]]> Conflicto de intereses: ninguno declarado. ]]>