Acute pancreatitis: Reflections through the history of the Atlanta Consensus
Pancreatitis aguda: reflexiones a través de la historia del Consenso de Atlanta
Pancreatites aguda: reflexões através da história do Consenso de Atlanta
Ana María Torres López1; Sergio Iván Hoyos Duque2
]]>1 Student, Medical School, Universidad de Antioquia; Gastro-hepatology Group, Universidad de Antioquia, Medellín, Colombia.
2 Surgeon, Titular Professor, Medical School, Universidad de Antioquia. Liver Transplant Group at Hospital Pablo Tobón. Medellin, Colombia. sergiohoyosd@yahoo.es
Received: November 15, 2013
Accepted: March 03, 2014
SUMMARY
]]> Acute pancreatitis is an inflammatory process with systemic and local repercussions. Most cases are mild with a low mortality rate, but 20% of patients have severe pancreatitis, with a mortality rate up to 30%. Throughout the years, the medical community has tried to reach a consensus about this disease to better understand, classify and treat it. The most important consensus is known as the Atlanta Consensus of 1992, which has been in use for many years. However, it has recently been the subject of various proposals for change and updating, which are discussed in this review.KEY WORDS
Acute Pancreatitis, Atlanta Consensus, Multiorganic failure, Necrosis, Pseudocyst
RESUMEN
La pancreatitis aguda es un proceso inflamatorio con repercusiones sistémicas y locales; la mayoría de los casos son leves con baja tasa de mortalidad, pero el 20% de los pacientes sufren pancreatitis grave cuya tasa de mortalidad puede llegar a ser hasta de un 30%. A lo largo de los años se ha intentado llegar a consensos acerca de esta enfermedad con el fin de orientar a la comunidad médica hacia su mejor entendimiento, clasificación y tratamiento. El más importante de estos ha sido conocido como el Consenso de Atlanta de 1992, vigente por muchos años, pero que está siendo objeto de diferentes propuestas de modificación y actualización, que se discuten en este artículo de revisión.
PALABRAS CLAVE
Consenso de Atlanta, Falla Multiorgánica, Pancreatitis Aguda, Necrosis, Seudoquiste
RESUMO
A pancreatites aguda é um processo inflamatório com repercussões sistémicas e locais; a maioria dos casos são leves com baixa taxa de mortalidade, mas 20% dos pacientes sofrem pancreatites grave cuja taxa de mortalidade pode chegar a ser até de um 30%. Ao longo dos anos se tentou chegar a consensos a respeito desta doença com o fim de orientar à comunidade médica para seu melhor entendimento, classificação e tratamento. O mais importante destes foi conhecido como o Consenso de Atlanta de 1992, vigente por muitos anos, mas que está sendo objeto de diferentes propostas de modificação e atualização, que se discutem neste artigo de revisão.
PALAVRAS IMPORTANTES
]]> Consenso de Atlanta, Falha Multiorgânica, Pancreatites Aguda, Necroses, Pseudocisto
INTRODUCTION
Acute pancreatitis is an inflammatory process with systemic and local repercussions. Most cases are mild with a low mortality rate, but 20% of patients with severe pancreatitis have a high mortality rate. The condition is also associated with complications that set the course and treatment of this disease (1,2). Over the years, the medical community has tried to reach a consensus about this disease in order to standardize different aspects of diagnosis and treatment. One of the most broad-reaching of these attempts was the Atlanta symposium in 1992 (3), which improved the previous classification of Marseille (4). However, knowledge about the pathophysiology of the disease, therapeutic strategies and technology has evolved in the last 20 years. Moreover, the 1992 Atlanta classification has been the subject of criticism concerning the severity of acute pancreatitis, the interobserver variability of local complications and the concept of organ failure, among other topics (5). For these reasons it was necessary to reassess those concepts. This review aims to provide a comparative analysis of the classification and the terminology used for acute pancreatitis from the Atlanta Symposium. It will provide concepts from the medical literature supported by evidence and especially emphasize the revision of the Atlanta classification and definitions by the international consensus formulated in 2012. This consensus guides the diagnosis and provides new information about the types of pancreatitis, its severity and local complications, accounting for the implementation of existing knowledge and current diagnostic tools for acute pancreatitis.
GENERAL CONCEPTS
Acute pancreatitis is an acute inflammatory process of the pancreas triggered by the unregulated activation of pancreatic enzymes, leading to the autodigestion of the gland, tissue injury and a local and systemic inflammatory response with the variable involvement of distant organs and tissues (1) The main causes of this disease are gallstones and alcohol abuse, which account for 80% to 90% of the cases; the remaining 10% to 20% are idiopathic, and a smaller proportion are due to other etiologies, such as metabolic abnormalities (hypertriglyceridemia, hypercalcemia), pancreatic duct obstruction, medications, post-endoscopic retrograde cholangiopancreatography (ERCP) and trauma (2). The overall incidence of acute pancreatitis is 4.9 to 35 cases per 100,000 population (6). Annually, this disease accounts for more than 220,000 cases in the United States (7). Worldwide statistics show that mild acute pancreatitis represents approximately 80% of cases and has a mortality rate of less than 1%, (2), whereas in severe forms, which represent the remaining 20% of the cases, the mortality rate can range from 30% to 50% according to different studies (8,9)
It is noteworthy that the classification of the severity of acute pancreatitis was modified according to the 2012 Atlanta consensus for mild, moderate and severe acute pancreatitis, taking into account the presence of organ failure, its evolution over time and local or systemic complications. The importance of this classification lies in addressing the treatment and the site of care. Furthermore, according to the biphasic mortality model, acute pancreatitis has two peaks: the first, during an early phase (the first two weeks), is associated with a systemic inflammatory response (SIRS) and subsequent organ failure; the other, which occurs later (after two weeks), is related to infection and sepsis (10,11). Others propose using the International Multidisciplinary Classification (IMC), which consists of four severity categories: mild acute, moderate, severe and critical pancreatitis; the latter is also called fulminant in some publications (12-15).
There are few published studies about this subject in Colombia. One was conducted at Pablo Tobón Uribe Hospital, in Medellín. In this descriptive study (case series) 45 patients diagnosed with severe acute pancreatitis were admitted to this institution between 1999 and 2004; 48.9% of the patients were between 31 and 55 years old, and 57.8% were female. The etiology was biliary tract-related in 49% of the cases, idiopathic in 33%, alcohol-related in 11% and due to trauma in the remaining 7% (16).
]]>PATHOPHYSIOLOGY
The pathophysiological process underlying this disease is the unregulated activation of trypsin within the pancreatic acinar cells. The main factors influencing the hyperstimulation of the gland are gallstones and alcohol abuse. Acute pancreatitis is initiated when hyperstimulation exceeds the intrapancreatic protective mechanisms that prevent trypsinogen activation or reduce the activity of trypsin; such mechanisms include enzymes stored as zymogen granules, low intracellular ionized calcium concentrations, a pressure gradient that favors the flow from the pancreas towards the duodenum, secretion of pancreatic enzymes in an inactive form (proenzymes), and enzymes that activate the zymogen outside the pancreas and synthesis of specific trypsin inhibitors by acinar cells (17,18). When these mechanisms are unable to contain the hyperstimulation of the pancreas, activation of enzymes within the gland leads to its autodigestion and triggers an inflammatory response mediated by interleukins and tumor necrosis factor alpha (TNF-α). This process affects the organ through local complications, such as interstitial edematous pancreatitis or necrotizing pancreatitis. This response can be generalized as Systemic Inflammatory Response Syndrome (SIRS) and can lead to multiple organ failure (MOF) (19).
HOW TO REACH A CONSENSUS?
Currently, guidelines and expert consensus have a great influence on clinical practice, but coming to an agreement is a huge challenge in terms of decision making. It should ensure the participation of all members and clarity of concepts, control for factors such as the lack of time and address differing views on a topic. Several strategies have been developed to address these difficulties. One is the GRADE (Grading of Recommendations Assessment, Development and Evaluation) system that classifies the quality of evidence and grades the strength of the recommendations. This system collects information in a structured way to analyze and summarize relevant clinical evidence and uses that evidence to establish a degree for a recommendation. That is, it measures the weight of the items, with emphasis on efficiency, on the grounds that clinical trials are conducted under ideal conditions (RCT or randomized clinical trials).
The GRADE system is characterized by organization of the information analysis in a three-stage process: (1) Formulation of the research question and stratification of the outcomes according to their relative importance. (2) Evaluation of the quality of the evidence and classification into four categories: high, moderate, low and very low. Afterwards, a general idea about the body of evidence is achieved. This system allows for the improvement of the quality of evidence obtained from observational data from the low quality category to the moderate or high quality category; likewise, it could lower the category of a randomized study, taking into consideration details of its design and implementation. However, the decision about the quality of evidence has subjective aspects that can lead to differences of opinion. (3). Lastly, the strength of recommendations (strong or weak) is stratified; that is, the degree of certainty that the desirable effects of an intervention outweigh the undesirable ones is determined (20).
Another strategy is based on formal consensus methods, in which all participants can contribute similarly. This approach measures effectiveness rather than efficiency, because each expert provides realistic scenarios from their experience. The most common types of formal consensus methods are the Delphi method and the nominal group technique. The Delphi method is based on the principle of collective intelligence; it uses a large number of participants, who answer questionnaires in different rounds, and has a coordinator. There is a period for anonymous feedback and finally a statistical group response is achieved. For example, the 2012 Atlanta consensus used this method. In contrast, the nominal group technique obtains reviews from a smaller number of experts, everyone has the opportunity to participate, and there is feedback for each response. It consists of many reviews that are stratified in terms of acceptance. The 1992 Atlanta consensus was based on this technique (21-23).
A CLINICALLY BASED CLASSIFICATION SYSTEM FOR ACUTE PANCREATITIS (ATLANTA SYMPOSIUM, 1992)
]]> Positive aspectsOverall, this consensus allows a working diagnosis based on information that can be obtained within the first and second days of hospitalization, using the patient's medical history, laboratory results and some radiological findings (3). It improves upon the previous classification of Marseilles, which was based on morphology and data that could not be obtained during hospitalization (3); and reclassifies acute pancreatitis during its evolution, recognizing it as a dynamic process. The 1992 Atlanta classification system also reached a consensus on the terminology for acute pancreatitis in order to facilitate the communication between institutions and researchers (3).
Why is important to review the 1992 Atlanta classification system?
Knowledge about the pathophysiology of the disease, therapeutic strategies and technology, has changed and evolved over two decades. Furthermore, this classification has been the subject of criticism: (1) The 1992 Atlanta classification does not provide a cutoff level for pancreatic enzymes for the diagnosis of acute pancreatitis (5); (2) It divides the severity of acute pancreatitis into mild and severe according to the organ failure criteria proposed; (3) It determines that a patient has pancreatitis according to a certain Ranson and APACHE II score, which also predicts severity; however, this concept of severity differs from the current one, which is related to organ failure. It is critical to understand these two concepts because not all patients assigned a significant prediction score for severity actually have severe acute pancreatitis (5, 24). Currently, there is better understanding about the pathophysiology and treatment of shock; additionally, organ failure criteria and its classification have changed. (4) Lastly, local complications have large interobserver variability and lack clear radiological criteria (25,26). All of these factors led to a continued failure to use standardized definitions for acute pancreatitis. In addition, heterogeneity of the criteria for inclusion of patients in clinical trials has hindered the progress of evidence-based research.
Classification of acute pancreatitis—2012: revision of the Atlanta classification and definitions by international consensus
The update of the 1992 Atlanta consensus was made using the Delphi method. This process started in 2007 with a web-based consultation to ensure a broad participation of experts. Subsequently, a working group was formed to coordinate the management of the final document, according to the reviewer's annotations. This consultation process was repeated three times and eventually the consensus was published in 2012, retaining only the information with the supporting evidence.
In this new consensus, the interstitial edematous pancreatitis and necrotizing pancreatitis concepts remain. It also proposes diagnostic criteria for acute pancreatitis, which is divided into two phases, early (first two weeks) and late (more than two weeks and only for moderately severe and severe pancreatitis). Severity also incorporates new parameters; by accounting for organ failure, pancreatitis is classified as mild, moderately severe or severe. According to this new classification, complications of the disease can be systemic or local; the latter are described in detail, taking into consideration CT findings, differently from the previous classification, and are classified into peripancreatic fluid collections, pancreatic and peripancreatic necrosis (sterile or infected), pseudocyst and walled-off necrosis.
DIAGNOSIS OF ACUTE PANCREATITIS
The diagnosis of acute pancreatitis requires two of the following three features:
If a patient meets the criteria for abdominal pain and elevated pancreatic enzymes, no images are required to make a diagnosis upon admission to the hospital. Conversely, if symptoms are highly suggestive of pancreatitis, but pancreatic enzyme levels are not diagnostic, an imaging study is recommended (27,28).
It is important to define the onset of acute pancreatitis as the time when the abdominal pain began and not when the patient was admitted to the hospital; the relevance of this distinction lies in the need to know the time course of the symptoms in order to classify the organ failure.
TYPES OF ACUTE PANCREATIITS
Interstitial edematous pancreatitis
Interstitial edematous pancreatitis is the most common type and usually resolves within a few days. Morphologically, it is characterized by diffuse enlargement of the pancreas due to inflammatory edema of the parenchyma and peripancreatic tissues, but without recognizable tissue necrosis. On a CT scan (Contrast Enhanced Computed Tomography), the pancreatic parenchyma shows relatively homogeneous enhancement, and peripancreatic fat usually shows some inflammatory changes such as haziness or mild stranding.
]]> In a CT scan during the first days after onset of acute pancreatitis, pancreatic parenchymal tissue may show a heterogeneous enhancement pattern that is not categorized definitively as either interstitial edematous pancreatitis or necrosis. Thus, the presence or absence of necrosis should be described as undetermined. A CT scan after 5-7 days allows for a better characterization.Necrotizing pancreatitis
Necrotizing pancreatitis is less common and is characterized by the presence of pancreatic or peripancreatic necrosis (29). It is necessary to emphasize that the impairment of pancreatic perfusion and signs of peripancreatic necrosis evolve over the course of several days, which explains why an early CT scan may underestimate the extent of pancreatic and peripancreatic necrosis. In the first week, the pattern of perfusion of pancreatic parenchyma on a CT scan can be patchy, but a non-enhancing area of pancreatic parenchyma could be evident few days afterwards, and it denotes the extent of necrosis (26), which may remain sterile or become infected.
The 2012 Atlanta consensus highlights the diagnosis of infected pancreatic necrosis because, if it is present, the patient needs antibiotic therapy and possibly invasive procedures. Infected pancreatic necrosis is associated with increased morbidity and with a reported mortality rate up to 30% (30,31). The presence of infection may be suspected if gas is observed in the pancreatic and/or peripancreatic tissues on the CT scan or when a percutaneous, image-guided, fineneedle aspiration (FNA) is positive for bacteria and/or fungi by Gram stain and culture. (table 1)
LOCAL COMPLICATIONS
The 1992 Atlanta classification system proposed the following terms: acute fluid collection, pseudocyst, pancreatic necrosis and pancreatic abscess, but their descriptions and tomographic criteria were unclear. The new classification system (Atlanta 2012) provided a comprehensive description of the local complications of pancreatitis, including tomographic and morphological criteria that considered the natural course of the disease and management to reach a more accurate diagnosis with decreased interobserver variability. This update proposed the following local complication terms: acute peripancreatic fluid, pancreatic pseudocyst, acute necrotic collections and walled-off necrosis.
The term ''pancreatic abscess'' was proposed by the original Atlanta classification. It was defined as a localized pus collection without significant necrotic material. The new classification of 2012 does not take this term into account, arguing that it is an extremely rare finding, is confusing and has not been widely adopted (32).
The term pancreatic pseudocyst has been used repeatedly and erroneously in the medical literature and in clinical practice. In fact, it is used inappropriately to describe most of the peripancreatic collections in the context of acute pancreatitis. The new classification places more clear and objective limits on pancreatic and peripancreatic collections (33). Consequently, it is important to clarify that a peripancreatic fluid collection that persists for more than 4 weeks can probably become pseudocyst, although during the evolution of acute pancreatitis, it is rare that a true pseudocyst (a persistent fluid collection bound by a well-defined wall whose content is primarily not solid) develops.
]]> Likewise, the 2012 Atlanta classification states that the term pseudocyst should not be used if there is evidence of solid necrotic material within the collection. As a result, it ensures that a pseudocyst cannot be formed from an acute necrotic collection; for this reason, the term ‘pancreatic pseudocyst' in the context of acute pancreatitis may fall into disuse. Bearing in mind that the pathophysiology of a pseudocyst involves an alteration of the ducts, another way that a pseudocyst may develop is the via ‘disconnected duct syndrome'. This term refers to the localized leakage of pancreatic fluid due to the lack of continuity between viable pancreatic tissue and the cavity where a necrosectomy was previously performed (34) in which necrosis was not found because it had been removed by this procedure.To differentiate pancreatic pseudocysts from peripancreatic necrosis in cases where a CT scan does not distinguish solid from liquid content immediately, it may be necessary to use other immunological techniques such as magnetic resonance imaging (MRI) or endoscopic ultrasound to support the diagnosis, by showing the absence of solid material within the collection. Another local complication is walled-off necrosis, the mature phase of an acute necrotic collection. Its content is characterized by varying amounts of solid and liquid material surrounded by an uncoated, fibrous reactive capsule. It usually develops after 4 weeks from the onset of necrotizing pancreatitis (33,35). Imaging studies other than CECT may be required to differentiate that collection from a pancreatic pseudocyst.
ORGANIC FAILURE
The 2012 Atlanta classification proposes a definition of organ failure different from the 1992 Atlanta classification based on the modified Marshall scoring system (36), which is recognized for having universal applicability and the ability to stratify disease severity easily and objectively. Three systems were evaluated: the respiratory system measured based on the PaO2/ FiO2 ratio, the renal system, considering serum creatinine and the cardiovascular system by measuring systolic blood pressure and patient's response to fluid resuscitation. Organ failure is defined as a score of 2 or more for one of these three organ systems. These parameters are relatively similar to those used by the 1992 Atlanta classification, but it only took into account blood pressure to define shock and respiratory failure defined by PaO2. The 2012 Atlanta Consensus also classifies organ failure into transient, if resolved in less than 48 hours, or persistent, if not resolved by then.
SEVERITY OF ACUTE PANCREATITIS
At admission, it is important to define and stratify the severity of acute pancreatitis because patients with severe acute pancreatitis require aggressive early treatment; moreover, it is important in these cases to determine the necessity for a higher level of care and referral to a specialist. Also, for specialists who receive such referrals, it is advantageous to stratify these patients into subgroups based on the presence of persistent or transient organ failure and local or systemic complications (37,38).
Mild acute pancreatitis
Mild acute pancreatitis is characterized by the absence of organ failure and local or systemic complications. It usually resolves during the early phase and no imaging studies are required.
]]> Moderately severe acute pancreatitisModerately severe acute pancreatitis is characterized by transient organ failure and/or local or systemic complications. One example of a symptomatic local complication is a peripancreatic collection associated with prolonged abdominal pain, fever and leukocytosis, or that produces an impairment to tolerate taking anything by mouth.
Moderately severe acute pancreatitis may be resolved without intervention (as for a transient organ failure or acute fluid collection) or require specialized longterm care (as for a sterile necrosis without organ failure). This entity may be resolved during the second week or require an extended hospitalization due to local or systemic complications.
This new category has been criticized by some authors, who argue that it includes three different types of patients, namely: those with organ failure, those whose health is impaired by systemic diseases and those with local complications. However, the 1992 Atlanta classification explained the introduction of this new category. It included patients with organ failure, either multiple, simple, transient or persistent, in the definition of severe acute pancreatitis. This is because, at the time, there were no such distinctions. This classification also included patients with local complications. This division was heavily criticized due to its simplicity as prospective. Retrospective analysis suggested a new category called moderately severe acute pancreatitis. Studies demonstrated that mortality and time in the intensive care unit were higher in patients with severe acute pancreatitis with organ failure compared with those who had moderately severe acute pancreatitis, but without organ failure (local complications) according to the Atlanta criteria. Using the arguments mentioned above, it was decided to split the severity into moderately severe and severe acute pancreatitis (39-41).
Severe acute pancreatitis
Severe acute pancreatitis is characterized by the presence of persistent (either single or multiple) organ failure (42). Patients with severe acute pancreatitis that develops within the first phase are at increased risk of death: approximately 36% to 50% of these patients die at that stage of the disease (43-45). The subsequent development of infected necrosis leads to an extremely high mortality rate (31,46). A meta-analysis published in 2010 showed that both pancreatic necrosis and organ failure are independent factors that increase mortality in severe acute pancreatitis up to 30% and 32%, respectively, but when both factors are present, it rises to 43% (31).
One of the most innovative points concerning the new proposed classification (Atlanta 2012) is the distinction between the concept of predicted severity and current severity. The 1992 Atlanta classification system splits severity into mild and severe acute pancreatitis, according to organ failure criteria proposed at the time. It also considered that a patient with a Ranson score ≥ 3 or an APACHE II score > 8 had severe pancreatitis; these scores predicted severity differently from the current severity concept which is associated with organ failure. These tests are also cumbersome, requiring multiple measurements and Ranson's score is not completely accurate until 48 hours after the onset of symptoms.
It is important to differentiate between the two concepts, current and predicted severity, since less than 50% of patients with predicted severity will finally show a current serious illness. This lack of distinction may explain the variation in the incidence of acute pancreatitis. Additionally, treatment may be delayed by the inability to differentiate between the mild and severe forms of the disease (5,24).
Evolution of the severity of acute pancreatitis
During the clinical approach to patients with acute pancreatitis, it is crucial to evaluate the severity over time. From the time of admission to the hospital, the presence or absence of organ failure must be identified and it must be determined, according to its evolution over time, if the organ failure is persistent or not. However, because it is difficult to determine when organ failure is present in the first 24 hours, treatment of the patient for severe acute pancreatitis is recommended. In addition, monitoring should be performed during the early phase, after 24 hours, 48 hours and 7 days after admission.
]]> When the diagnosis of pancreatitis is clear, a CT scan is not recommended during the first 48 to 72 hours because the presence of necrotizing pancreatitis cannot be accurately determined during that period, nor can its extension be defined. Moreover, it is not necessary to identify local complications during the first week since the extent of morphological changes and necrosis are not directly proportional to the severity of organ failure and treatment is not required for complications detected during the early phase (47). A CECT is only recommended during the first days of symptoms when the diagnosis is uncertain or the patient presents a rapid health impairment despite supportive measures (24,26,38).
PHASES OF ACUTE PANCREATITIS
Early acute pancreatitis
Early acute pancreatitis usually lasts one or two weeks. During this phase systemic changes occur as a response to local pancreatic injury, which is mainly due to three factors: activated pancreatic enzymes, microcirculatory impairment and the release of inflammatory mediators (48,49). These elements manifest clinically as a systemic inflammatory response (SIRS). Organ failure risk increases if the SIRS persists; SIRS presence on day one predicts the severity of pancreatitis with a sensitivity of 85% to 100%, while its absence on that day has a negative predictive value (NPV) for severe pancreatitis from 98% to 100% (49). On the whole, it can be concluded that the main cause of death during the early phase is the inflammatory response associated with organ failure (14). At this stage, about half of the deaths from necrotizing pancreatitis are attributable to multiple organ failure (46). The usefulness of surgical intervention during the first phase has been questioned, since it has been shown to be of some benefit only in a very few cases, because the phenomenon has a purely inflammatory systemic nature (50).
Late acute pancreatitis
Late acute pancreatitis is characterized by persistent signs of systemic inflammation or the presence of local complications. By definition, it only occurs in patients with acute severe or moderately severe pancreatitis, according to Atlanta 2012. Local complications evolve during this phase. It is important to distinguish the morphological characteristics of local complications radiologically owing to the implications for their treatment. Nevertheless, the main determinant of severity is still persistent organ failure. Therefore, the diagnosis of pancreatitis in this phase requires clinical and morphological criteria. The main determinant of mortality during this phase is infection: approximately 30% of patients with necrotizing pancreatitis during this phase die from an infected necrotic zone (31).
CONCLUSIONS
The 2012 Atlanta classification updates the concepts proposed 20 years ago by the 1992 Atlanta Consensus. It contains innovative proposals because it is based on current knowledge about the natural history, pathophysiology, and the diagnosis of acute pancreatitis, as well as the use of clinical and radiological criteria to reach an updated consensus on this topic. The 2012 Atlanta classification system provides more accurate guidelines to diagnose acute pancreatitis; moreover, it provides a reference level for pancreatic enzymes and a diagnostic algorithm. It also incorporates the current concept of organ failure to classify acute pancreatitis as mild, moderately severe and severe, emphasizing differentiation by current and predicted severity scores such as Ranson and APACHE II
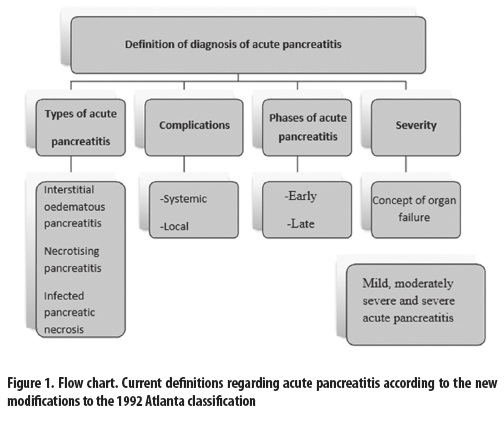
]]> This consensus reaches an agreement about the terminology for local complications, formerly debated because of the large interobserver variability. It divides local complications into acute peripancreatic fluid collection, pancreatic pseudocyst, acute necrotic collection and walled-off necrosis. Additionally, as an innovative factor, it includes tomographic criteria to classify these findings. Moreover, it highlights the importance of infected necrosis because of its association with high morbidity and mortality (figure 1)Arrived at using the Delphi method, the 2012 Atlanta consensus brings strong clinical evidence and common points provided by international experts regarding the current knowledge of acute pancreatitis. Moreover, it is considered a proposal that helps the medical community to make decisions. Although it apparently has no direct effect on the treatment of patients with acute pancreatitis, this consensus will help in the design of clinical studies with standardized parameters, which in turn will have an impact on the recommendations about interventions and specific treatment. In addition, this consensus must be validated by prospective studies that support these guidelines.
ACKNOWLEDGMENTS
Thanks to the sustainability project, Vicerrectoría de Investigaciones, Universidad de Antioquia.
REFERENCES
1. Nieto JA, Rodríguez SJ. Manejo de la pancreatitis aguda: guía de práctica clínica basada en la mejor información disponible. Rev Colomb Cir. 2010;25:76-96. [ Links ]
2. Whitcomb DC. Clinical practice. Acute pancreatitis. N Engl J Med. 2006 May;354(20):2142–50. [ Links ]
3. Bradley EL. A clinically based classification system for acute pancreatitis. Summary of the International Symposium on Acute Pancreatitis, Atlanta, Ga, September 11 through 13, 1992. Arch Surg. 1993 May;128(5):586–90. [ Links ]
4. Singer M V, Gyr K, Sarles H. Revised classification of pancreatitis. Report of the Second International Symposium on the Classification of Pancreatitis in Marseille, France, March 28-30, 1984. Gastroenterology. 1985 Oct;89(3):683–5. [ Links ]
5. Bollen TL, van Santvoort HC, Besselink MG, van Leeuwen MS, Horvath KD, Freeny PC, et al. The Atlanta Classification of acute pancreatitis revisited. Br J Surg. 2008 Jan;95(1):6–21. [ Links ]
6. Talley NJ, Locke III GR, Saito YA, editors. GI Epidemiology. Massachusetts: Wiley-Blackwell; 2008. [ Links ]
7. Fagenholz PJ, Castillo CF, Harris NS, Pelletier AJ, Camargo CA. Increasing United States hospital admissions for acute pancreatitis, 1988-2003. Ann Epidemiol. 2007 Jul;17(7):491–7. [ Links ]
8. Díaz C, Garzón S, Morales CH, Montoya M. Pancreatitis aguda grave: curso clínico, manejo y factores asociados con mortalidad. Rev Colomb Cir. 2012;27:281-9. [ Links ]
9. Ueda T, Takeyama Y, Yasuda T, Matsumura N, Sawa H, Nakajima T, et al. Simple scoring system for the prediction of the prognosis of severe acute pancreatitis. Surgery. 2007 Jan;141(1):51–8. [ Links ]
10. Hoyos S, Pelaez M. Soporte nutricional en pacientes con pancreatitis aguda grave. Iatreia. 2007;20(2): 178-185. [ Links ]
11. Beger HG, Rau BM. Severe acute pancreatitis: Clinical course and management. World J Gastroenterol. 2007 Oct 14;13(38):5043–51. [ Links ]
12. Windsor JA, Petrov MS. Acute pancreatitis reclassified. Gut. 2013 Jan;62(1):4–5. [ Links ]
13. Petrov MS, Windsor JA. Classification of the severity of acute pancreatitis: how many categories make sense? Am J Gastroenterol. 2010 Jan;105(1):74–6. [ Links ]
14. Petrov MS, Windsor JA. Conceptual framework for classifying the severity of acute pancreatitis. Clin Res Hepatol Gastroenterol. 2012 Aug;36(4):341–4. [ Links ]
15. Petrov MS, Windsor JA, Lévy P. New international classification of acute pancreatitis: more than just 4 categories of severity. Pancreas. 2013 May;42(3):389–91. [ Links ]
16. Hoyos S, Giraldo N, Donado J, Henao K, Peláez M. Costos, días estancia y complicaciones según tipo de soporte nutricional en pacientes con pancreatitis aguda grave. Rev Colomb Cir. 2007;22(3):157-65. [ Links ]
17. Brunicardi F, Andersen D, Billiar T, Dunn D, Hunter J, Matthews J, et al. Schwartz's Principles of Surgery. 9th ed. New York: McGraw-Hill; 2010. [ Links ]
18. Sabiston DC, Townsend CM. Sabiston Textbook of Surgery: The Biological Basis of Modern Surgical Practice. 18th ed. Philadelphia: Elsevier Saunders; 2008. [ Links ]
19. Frossard J-L, Steer ML, Pastor CM. Acute pancreatitis. Lancet. 2008 Jan;371(9607):143–52. [ Links ]
20. Andrews J, Guyatt G, Oxman AD, Alderson P, Dahm P, Falck-Ytter Y, et al. GRADE guidelines: 14. Going from evidence to recommendations: the significance and presentation of recommendations. J Clin Epidemiol. 2013 Jul;66(7):719–25. [ Links ]
21. Jaeschke R, Guyatt GH, Dellinger P, Schünemann H, Levy MM, Kunz R, et al. Use of GRADE grid to reach decisions on clinical practice guidelines when consensus is elusive. BMJ. 2008 Jan;337:a744. [ Links ]
22. Guyatt G, Oxman AD, Akl EA, Kunz R, Vist G, Brozek J, et al. GRADE guidelines: 1. Introduction-GRADE evidence profiles and summary of findings tables. J Clin Epidemiol. 2011 Apr;64(4):383–94. [ Links ]
23. Alonso-Coello P, Rigau D, Sanabria AJ, Plaza V, Miravitlles M, Martinez L. Calidad y fuerza: el sistema GRADE para la formulación de recomendaciones en las guías de práctica clínica. Arch Bronconeumol 2013 ;49(6):261-7. [ Links ]
24. Tenner S. Initial management of acute pancreatitis: critical issues during the first 72 hours. Am J Gastroenterol. 2004 Dec;99(12):2489–94. [ Links ]
25. Bollen TL. Imaging of acute pancreatitis: update of the revised Atlanta classification. Radiol Clin North Am. 2012 May;50(3):429–45. [ Links ]
26. Thoeni RF. The revised Atlanta classification of acute pancreatitis: its importance for the radiologist and its effect on treatment. Radiology. 2012 Mar;262(3):751– 64. [ Links ]
27. Clavien PA, Robert J, Meyer P, Borst F, Hauser H, Herrmann F, et al. Acute pancreatitis and normoamylasemia. Not an uncommon combination. Ann Surg. 1989 Nov;210(5):614–20. [ Links ]
28. Fallat RW, Vester JW, Glueck CJ. Suppression of amylase activity by hypertriglyceridemia. JAMA. 1973 Sep 10;225(11):1331–4. [ Links ]
29. Bakker OJ, van Santvoort H, Besselink MGH, Boermeester MA, van Eijck C, Dejong K, et al. Extrapancreatic necrosis without pancreatic parenchymal necrosis: a separate entity in necrotising pancreatitis? Gut. 2013 Oct;62(10):1475–80. [ Links ]
30. Banks PA, Freeman ML. Practice guidelines in acute pancreatitis. Am J Gastroenterol. 2006 Oct;101(10):2379–400. [ Links ]
31. Petrov MS, Shanbhag S, Chakraborty M, Phillips ARJ, Windsor JA. Organ failure and infection of pancreatic necrosis as determinants of mortality in patients with acute pancreatitis. Gastroenterology. 2010 Sep;139(3):813–20. [ Links ]
32. Van Santvoort HC, Bollen TL, Besselink MG, Banks PA, Boermeester MA, van Eijck CH, et al. Describing peripancreatic collections in severe acute pancreatitis using morphologic terms: an international interobserver agreement study. Pancreatology. 2008 Jan;8(6):593–9. [ Links ]
33. Sarr MG. 2012 revision of the Atlanta classification of acute pancreatitis. Pol Arch Med Wewnetrznej. 2013 Jan;123(3):118–24. [ Links ]
34. Pelaez-Luna M, Vege SS, Petersen BT, Chari ST, Clain JE, Levy MJ, et al. Disconnected pancreatic duct syndrome in severe acute pancreatitis: clinical and imaging characteristics and outcomes in a cohort of 31 cases. Gastrointest Endosc. 2008 Jul;68(1):91–7. [ Links ]
35. Stamatakos M, Stefanaki C, Kontzoglou K, Stergiopoulos S, Giannopoulos G, Safioleas M. Walled-off pancreatic necrosis. World J Gastroenterol. 2010 Apr 14;16(14):1707–12. [ Links ]
36. Marshall JC, Cook DJ, Christou N V, Bernard GR, Sprung CL, Sibbald WJ. Multiple organ dysfunction score: a reliable descriptor of a complex clinical outcome. Crit Care Med. 1995 Oct;23(10):1638–52. [ Links ]
37. Besselink MGH, van Santvoort HC, Witteman BJ, Gooszen HG. Management of severe acute pancreatitis: it's all about timing. Curr Opin Crit Care. 2007 Apr;13(2):200–6. [ Links ]
38. Banks PA, Bollen TL, Dervenis C, Gooszen HG, Johnson CD, Sarr MG, et al. Classification of acute pancreatitis-- 2012: revision of the Atlanta classification and definitions by international consensus. Gut. 2013 Jan;62(1):102–11. [ Links ]
39. Talukdar R, Clemens M, Vege SS. Moderately severe acute pancreatitis: prospective validation of this new subgroup of acute pancreatitis. Pancreas. 2012 Mar;41(2):306–9. [ Links ]
40. Vege SS, Gardner TB, Chari ST, Munukuti P, Pearson RK, Clain JE, et al. Low mortality and high morbidity in severe acute pancreatitis without organ failure: a case for revising the Atlanta classification to include ''moderately severe acute pancreatitis''. Am J Gastroenterol. 2009 Mar;104(3):710–5. [ Links ]
41. Vege SS, Chari ST. Organ failure as an indicator of severity of acute pancreatitis: time to revisit the Atlanta classification. Gastroenterology. 2005 Apr;128(4):1133–5. [ Links ]
42. Lytras D, Manes K, Triantopoulou C, Paraskeva C, Delis S, Avgerinos C, et al. Persistent early organ failure: defining the high-risk group of patients with severe acute pancreatitis? Pancreas. 2008 Apr;36(3):249–54. [ Links ]
43. Johnson CD, Abu-Hilal M. Persistent organ failure during the first week as a marker of fatal outcome in acute pancreatitis. Gut. 2004 Sep;53(9):1340–4. [ Links ]
44. Buter A, Imrie CW, Carter CR, Evans S, McKay CJ. Dynamic nature of early organ dysfunction determines outcome in acute pancreatitis. Br J Surg. 2002 Mar;89(3):298–302. [ Links ]
45. Mofidi R, Duff MD, Wigmore SJ, Madhavan KK, Garden OJ, Parks RW. Association between early systemic inflammatory response, severity of multiorgan dysfunction and death in acute pancreatitis. Br J Surg. 2006 Jun;93(6):738–44. [ Links ]
46. Van Santvoort HC, Bakker OJ, Bollen TL, Besselink MG, Ahmed Ali U, Schrijver AM, et al. A conservative and minimally invasive approach to necrotizing pancreatitis improves outcome. Gastroenterology. 2011 Oct;141(4):1254–63. [ Links ]
47. Spanier BWM, Nio Y, van der Hulst RWM, Tuynman HARE, Dijkgraaf MGW, Bruno MJ. Practice and yield of early CT scan in acute pancreatitis: a Dutch Observational Multicenter Study. Pancreatology. 2010 Jan;10(2-3):222–8. [ Links ]
48. Elfar M, Gaber LW, Sabek O, Fischer CP, Gaber AO. The inflammatory cascade in acute pancreatitis: relevance to clinical disease. Surg Clin North Am. 2007 Dec;87(6):1325–40, vii. [ Links ]
49. Singh VK, Wu BU, Bollen TL, Repas K, Maurer R, Mortele KJ, et al. Early systemic inflammatory response syndrome is associated with severe acute pancreatitis. Clin Gastroenterol Hepatol. 2009 Nov;7(11):1247–51. [ Links ]
50. Nathens AB, Curtis JR, Beale RJ, Cook DJ, Moreno RP, Romand J-A, et al. Management of the critically ill patient with severe acute pancreatitis. Crit Care Med. 2004 Dec;32(12):2524–36. [ Links ]
]]>